Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
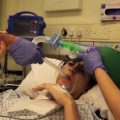
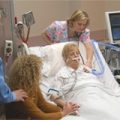
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Laura as part of my 1:1 consulting and advocacy service! Laura’s mother is in the ICU for Septic Shock and she is asking if a DNR status is an ICU Team decision or the family’s decision.
My Mother Has Sepsis and Had a Code in the ICU. Will This Be Her First Stage to Withdrawal of Treatment?

“You can also check out previous 1:1 consulting and advocacy sessions with me and Laura here.”
Patrik: Yes. It sounds like they have suggested that, even, if that’s what you want.
Laura: Well, I was trying to find my options, and I said well, we’d like to go to back to Sierra Hospital and she said but you would have to find a doctor, a specific name and his phone number. And so, I started some preliminary work on that, just on the phone, and I’m having a little difficulty at first try. They said but you can’t do it, Laura, for your mother. You must have the case manager here at this hospital, Victoria Hospital, contact the other case manager at the new hospital, and have them coordinate. And then when I looked back to keep with the case manager here after some time, she said oh, they said no. They said no.
Patrik: Okay. I wouldn’t worry… okay. I contend that if you find a hospital that will take your mom, they wouldn’t be in your way. They wouldn’t be in your way. I tell you again, what they are probably worried about is let’s just say you’re starting the process of getting your mom out to another hospital, they would just be worried in terms of you know, how long does it take, you know. It could take another week. In their minds, your mom shouldn’t be here in another week. You know, all of that. So, what I do believe that if you can get the process started, to me it sounds like you will find another hospital. Are you in L.A.?
Laura: I am in what they call Sub-urban neighbourhood, which is a little bit south of Los Angeles, about 50, 60 miles south.
Patrik: Yep. Yep. So, you know…
Laura: Challenge. I get the challenge of trying to find a doctor and somebody who will take her case because they’re saying it’s futile or whatever.
Patrik: Yeah, yeah, yeah. And that’s probably why you will need, besides talking to the ICU, I do believe you will need to talk to the Gastroenterologist because they will have a view. You know, ICU… one of the reasons why ICU is so doom and gloom is you know, they only see the bad things, normally. They see people at their worst, right? Whereas the Gastroenterologist sees both sides. They see people at their worst, but they also see people leaving ICU. Right? And that Gastroenterologist could be your advocate, almost, to leave Intensive Care and go to another hospital. Because he will also know other Gastroenterologists in other hospitals. Because it sounds to me like the primary issue is the pancreas or the gallbladder. That is the primary issue leading to all of those, you know… leading to the critical illness.
But the primary issue clearly is the gallbladder or the pancreas or whatever might be affected. So that still needs the input of a specialist.
Recommended:
Laura: The gastro… the GI…
Patrik: Yeah, the GI doctor, you know? And that could be your advocate to get her somewhere else. However, what you could also do as a next step, and if you could go back to the ICU and you could say hey, I really want her somewhere else. Please give me the time and help me to get her somewhere else. And you can frame it in a way like look, I don’t agree with the Catholic values. I don’t believe this is futile, you know? And you could also start changing your language in terms of they’re saying it’s futile, and you could say something along the lines of well, its perceived futility. Right? So, choosing your language is going to be very important going forward.
I would also… with the discussion around end of life, I would also start using stronger language. I would start using language such as you are killing my mother or potentially murdering her. I would start using stronger language so that they know… I mean, they probably know by now that you are serious, but in order to buy time and in order to get all of that organised, you will need to start using stronger language so that they know hang on, I’m dead serious here. I am not going to follow your… whatever they are instructing you. And they probably know that already that you’re not a pushover, but I would recommend that at this point in time, you will need to start using stronger language.
Another recommendation would be, especially if they keep pushing towards end of life, if I was you, I would ask for the end of life care policy. And I would-
Laura: I did. I did. I asked for… I did because I saw that on your tips. Now, they had a sheet in front of them, a single sheet covered in a plastic sleeve, and then they had this packet that I have here, called Ethical and Religious Directives for Catholic Healthcare Services. And so, I remember you saying that, so I said well, you’re saying that you’re going to terminate treatment and blah blah blah, then may I see a copy of this policy that you’re showing me? And they hem-hawed around well, it’s just in this packet, you know, they gave me this packet.
Patrik: So-
Laura: But they had another single sheet. I said, what’s that single sheet? And she acted like it was just one page out of this packet, I guess.
Patrik: And did you have a look? Is there something in there that you think is relevant?
Laura: Yes. Well, yes, I’m looking here. It says we affirm the ethical standards of behaviour in healthcare that flow from the church’s teaching about the dignity of the patient, provide authoritative guidance on certain moral issues. Now, they were saying to me verbally that like continuing to treat my mother would be almost like cruelty and all that kind of thing. I’m kind of just skipping through here. Some spiritual stuff in all that.
Recommended:
Patrik: Right. But you see, this is where it gets important, like even though they might base their decision-making on their moral or ethical sort of Catholic values, that, for example, can’t overrule a state law.
Laura: Aha.
Patrik: Right? Imagine they are saying from a Catholic point of view we think it’s futile and we think on Monday at 12 o’clock we stop life support. And if the state law in Los Angeles says something along the lines of well, end of life care decisions can’t be made without consent of a patient or a medical power of attorney .
Laura: Aha.
Patrik: Right? I mean, that’s why… yes, surely people are entitled to their beliefs, but they’re not entitled to overrule a law because of their beliefs.
Laura: I see.
Patrik: Right?
Laura: I need to get my laws in front of me.
Patrik: While we’re talking, I’m just Googling some things. I haven’t found what I’m looking for yet, but I’m just Googling, and I know I will find something for you. But you see where I’m going with this. So, people… it’s easy to lose sight. It’s very easy to lose sight, and it’s very easy to panic in situations like that, you know. People… all they present you with is doom and gloom. And all they present you with is on Monday, 12 o’clock, we have to stop life support, blah blah blah. That’s overwhelming. That’s very overwhelming, it’s very confronting. Right? And people can’t see the wood for the trees because of that. So, it’s really important to go one step back and say, hang on a sec, what are we doing? What are the options? You know?
As I said, I’m just looking… I’m just actually on a website here where it says end of life option act in California. So just give me a minute and I will find something. I have not found a state in the US where a hospital can just willy-nilly withdraw life support without consent of a family.
Laura: Okay.
Patrik: That’s not happening.
Recommended:
Laura: Aha. Good point.
Patrik: Right. And that’s what I mean. It’s very overwhelming and it’s very easy to lose sight. And it’s very easy to think like people thought like 100 years ago where they say oh wow, if the doctor says we’ve got to do this, then it must be right.
Laura: Yeah. Yeah.
Patrik: Right, it’s very easy to lose sight of that and as I said, it’s very important to go one step back and really look at okay, what are we actually dealing with?
Laura: Yes.
Patrik: Right? So, know that you have rights. Okay, it’s very important for you to understand that you have rights. And it’s just a matter of exercising them. Okay? And as I said, I’m just looking it up, and I’m sure I’ll find it for you, that the law in Los Angeles and in any other state-
Laura: May I say something? May I say-
Patrik: Please.
Laura: May I say something as a side note? My mother has Medicare where they pay 80% and we pay 20%, okay?
Patrik: Yeah.
Laura: And Medicare here, a lady showed up toward the beginning of my mom’s hospital admission, and she said here’s the paper. And I read it. It said that if you’re being discharged and you don’t agree and you think it’s too soon or whatever, here’s like a number where someone can come and hear your appeal and stuff. So that’s an interesting thing too. The Medicare.
Patrik: Very much so. Very much so. There are lots of options. There are really lots of options. And you know, look, I’ll give you another example. If your mom was on more than two forms of life support, if she was on five, six forms of life support, I’d say okay, well, maybe your mom is really dying. But I can’t see that. I can’t see that.
Recommended:
Laura: That’s what I tried to say. Look, her heart hasn’t given out and some people have a respiratory issue after going under general anaesthesia, plus she had the sepsis in the lungs, you know, she needed the respirator. But her brain, they scanned it, no stroke. Heart seems to be doing okay. You know?
Patrik: Exactly, exactly. So, and you know, I hope that I really sort of number one, explained to you your mom is just in a “normal” Intensive Care situation. That’s number one. Number two, your mom, more than 90% of Intensive Care patients survive, right, that’s number two. And number three, you have options. You just didn’t know about them. Right? You just didn’t know about them, and also from experience, they know you’re not a pushover. They know that by now. But in order to go from A to B and in order to get what you really want, you probably have to push harder, right, because they’re often not giving in at the first sign of resistance. Most people give in, but you’re probably just at the beginning and it’s just a matter of being very clear about what you want.
And what’s going to be important, I think, in order to move the needle is, number one, use stronger language. And number two, if they keep talking about futility, just make sure you’re saying look, this is perceived futility. It’s not real. This is just their perception. And you need to be very clear that you want time to find another hospital, and you would argue on the basis of hang on a sec, I just ended up in this Catholic hospital randomly, I did not choose to go here, and I don’t agree with those Catholic values.
Laura: Yes. That’s right.
Patrik: Right? There would be other hospitals out there that are non-religious, and they would just go with what you want.
Laura: Yes. That’s right. I don’t remember this ever happening at the other hospital. Albeit, it was a different scenario, but she was in mxedema coma and her heart rate dropped down to 27 and her temperature was 72, and they brought her back with a Levothyroxine and with the interventions in the ICU, you know? I don’t remember anybody pressuring me about all this.
Patrik: Exactly. Exactly. So, it is really a matter of changing your language, changing your approach. I would definitely recommend tracking down the GI doctor. Right? The doctor who’s pressuring you in ICU, he’s the medical director, you think?
Laura: Yes, yes, at the ICU, yes.
Patrik: Okay. You could also go down the track of-
Recommended:
Laura: I’m sorry, I guess they call it interventionist, something like that, I guess.
Patrik: Okay. I would also go as far as potentially saying that if you feel… I mean, do you feel bullied, do you feel intimidated? Is that the right way?
Laura: Absolutely, yes.
Patrik: Okay.
Laura: Absolutely.
Patrik: Right. If that’s how you feel, then I would… again, probably use those words, bully and intimidate, and potentially go to a hospital executive level. All you want, probably, at the moment, Laura, is you probably want to buy time. You want to buy time to get your mom in a better environment. You want to buy time that somebody can do whatever needs to be done in terms of sorting out the kidney issues. Right? And if you feel like you’re bullied and if you feel like all they want to talk about is end of life and they don’t want to treat your mom because of their values, because of their… let’s just call it again Catholic values for argument’s sake, then you need to go on to probably an executive level and say hey, wait a second, I’m feeling bullied, I want my mom out, I don’t agree that it’s futility, and I need the time to find another hospital. And in the meantime, while you’re looking for another hospital, I want my mom to get full treatment. And that includes treating the kidneys. Because by the sounds of this, it was denying treating the kidneys.
Laura: Yeah, they did try to say she can’t handle dialysis in her condition now.
Patrik: That’s rubbish. I really want to know why. That’s rubbish. You know, if she is on Levophed they should be able to manage dialysis I tell you why. I tell you why they might refer to that she can’t handle it. When somebody goes on dialysis who’s already in sort of a critical condition, their blood pressure drops. That blood pressure drops significantly, okay? But the good news is, if that happens, many patients end up on the Levophed okay. So, given that she’s on Levophed already, they probably just have to increase Levophed for a period of time. You know, to manage…
Laura: Right. Well, you know, they’ve got me in here, they’re making me feel like a trapped animal and they intimidate, and they bully, and the negativity so much, you know?
Recommended:
Patrik: Yeah, yeah. And you could also, especially with the intimidation and bullying, I would try and turn this on its head, and I would say hang on a sec, you are promoting Catholic values. Surely, bullying and intimidation would not be part of the Catholic values.
Laura: Yeah, yeah.
Patrik: Right. It’s really important that you almost turn this on its head, and you know, and use whatever you have in your arsenal, you know, to push back.
Laura: Yeah, yeah, yeah. Okay, well…
Patrik: Is that helpful?
Laura: Yes, it’s helpful. And it’s helpful when you’re mentioning about the state laws, too, to look up.
Patrik: Absolutely. Absolutely. I am still looking it up and I know I’ve got it somewhere because we’ve had clients before in Los Angeles. I’ll find it for you, and I will email it to you, you know, and you would also have to remind them that more than 90% of patients survive Intensive Care. You have to remind them of all of that because now you have more information than before.
Laura: Yes.
Patrik: Right, and you’ve got to remind them that you are doing your research.
Laura: Yes.
Patrik: Right? And you know, what argument do they have? In terms of when you say to them, when you remind them more than 90% of patients survive Intensive Care, why should your mother not survive Intensive Care? Because they don’t want to her to give the time that she needs.
Laura: Yeah.
Patrik: That’s all it is.
Laura: I did go to the head nurse at the CICU, the director, and she has a master’s degree. And I talked to her, I said what’s going on here? I said, I want my mom to have time. I feel pressured, like we must run out of here. She says, no, you don’t have to run out of here. I said, well, can we have time for my mother, to give her the chance to recover? She said, yes, you do. But then here we have this other doctor who’s an interventionist here at the CICU, and his team that want to pressure me to say we already did give her a chance, get out, you know?
Recommended:
Patrik: Does your mother have an advance care directive?
Laura: She has… I don’t know what you would call it, but she has a living trust, and it’s not really advanced care directive. It’s more like living trust for her assets and her… something like for me or my daughter Laura will take over. But I know her house call doctor, when she was home, handed me a pink sheet to fill out. I didn’t even fill it out yet, but here in this hospital, I’ve just been giving verbal… you know, they want to know verbally, full code versus DNR and all that.
Patrik: Right, right. But okay, there is nothing documented, for example, on your mom’s… where she says something along the lines of, I do want to have everything done if a situation like this ever came up. There’s nothing-
Laura: No, I don’t think she does. I have to check the living trust again to see, but it was originally made for my father, who passed 25 plus years ago, and then it went into my mother as well, saying that if she passed, then you know, like the inheritance and whatever, whatnot, you know. Assets. But I don’t think that there’s anything there.
Patrik: Okay.
Laura: It would have helped if we did have something that was proactive that way, probably, right?
Patrik: Right, yeah. It would. If she had a will that said look, in a situation like that, if I was ever in Intensive Care, I want all life support to continue. Something like that. It would be non-ambiguous, and it would also tell the Catholic hospital, well, I’m not interested in whatever the Catholics say, I’m interested in what I’m saying.
Laura: Right, that’s right. More armour there, or more ammunition, as they say.
Patrik: That’s right. But you have enough ammunition because you could also say something along the lines of, you know… it sounds to me like… I mean, did you ever have the discussion with your mom, like if a situation like this comes up, what she would want? Have you ever had a discussion with your mom about that?
Recommended:
Laura: I don’t know. Not so much, but you know, when she was sick with the myxedema coma, we felt that we gave it our best shot. That’s the kind of people that we are. She was that way with my dad, and that’s how we roll. We fight until it’s over.
Patrik: Yeah. Yeah. Exactly. But again, those are probably the things they need to hear because you know, that’s very contrary to what their Catholic principles are.
Laura: Yeah, that’s right. I see your point, yeah.
Patrik: You know.
Laura: Yeah, those things could have helped. Helped to solidify and all that.
Patrik: Yes. And really, don’t feel like… the hospitals often do that. Intensive care units often do that as sort of a real threat, sort of saying out by Monday, 12 o’clock or whatever the case may be, we stop life support. They can’t do that. They can’t do it.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!