Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“ I want to answer questions from one of my clients Laura as part of my 1:1 consulting and advocacy service! Laura’s mother is in the ICU for Septic Shock and Laura is asking if the futile treatment or management by the ICU doctors is considered ethically appropriate.
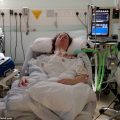
My Mom is in the ICU for Septic Shock. Why Does the ICU Team Aim for “End-of-Life” Treatment For Her?

“You can also check out previous 1:1 consulting and advocacy sessions with me and Laura here.”
Patrik: Okay. How many days has she been on Precedex for?
Laura: They had her on Propofol, and then Precedex for, let’s see how long… well, if the breathing tube was put in. Let’s see. The breathing tube was put in like… was it the 13th? The morning of the 13th. And that was the 21st. So that’s… the dates.
Patrik: Yeah, okay. Okay. And how is she responding? When you talk to her, is she opening eyes?
Laura: Yes. She’s waking up gradually. She opened her eyes and my brother is up there talking to her. But she is very tired and sleepy, but she is having the eye open now and then enhanced moving a little bit.
Patrik: Okay. If you asked her to squeeze your hand, would she do that?
Laura: She might. Right now, she has the mitts on, you know, those little gloves.
Patrik: Oh, that’s terrible.
Laura: Maybe we could take them off and I’ll try.
Recommended:
Patrik: I think so.
Laura: Yeah.
Patrik: If you asked her to open her eyes, would she do that because you asked her to?
Laura: Yes. I saw her doing it earlier with one of the nurses.
Patrik: Okay, that’s great. That’s something. That’s good.
Laura: Yes.
Patrik: So, because I am trying to find out what else is going on. With the Levophed do you know how much she’s on? Do you know how long she’s been on it for?
Laura: Yes. She’s been on it for quite a while. When did she go on it… after the respiratory event?
Patrik: Okay. Okay. Do you know how much she’s on?
Laura: At first, she was on Vasopressin and Levophed but now it’s just Levophed and it’s a moderate amount. Now, as they were trying to wean it down, on the Levophed her blood pressure was a little lower, so we kind of tweaked a lot.
Patrik: Yeah, yeah. No, that’s fine. That’s fine. What is important to understand with Levophed as well as… so your mom, at the moment, is on two forms of life support. Number one, ventilation, that’s life support. And the Levophed is also considered life support.
Laura: Okay.
Patrik: So, because… so ventilation, obviously, is life support because it’s sustaining breathing. Okay. And the Levophed is life support because your mama has the low blood pressure.
Laura: Yes.
Patrik: Okay, and without the Levophed your mom’s blood pressure would drop to a level that would be non-compatible with life.
Laura: Yes.
Patrik: Okay. So, she’s on two forms of life support. If she was to go on dialysis, that would be a third form of life support. Okay. But that just… you know, why that doesn’t sound appealing? That’s normal in Intensive Care. It’s perfectly normal. A lot of patients are on multiple forms of life support.
Laura: Yeah.
Recommended:
Patrik: Okay. So, this is, you know, people might hear, oh my goodness, your mom is on life support, and they might panic. Yeah, it’s not good to be on life support, but at the end of the day, that’s why patients are in Intensive Care. They need life support. Again, temporary life support.
Laura: Yes.
Patrik: Right? So, I tell you where the issues could be. And I’m glad that you’ve spoken to the Urologist. What did he say? What was his stand on all of this?
Laura: Well, he said that… I wanted to know if the… because I was alarmed about the low urine input that I saw today, whereas the past two days, the urine was more plentiful, it was more yellow. Today was less urine and rusty in colour. So, I wanted to talk to him. I haven’t seen him for a while. And I said well, is there anything that we can do? You, as a Urologist, is that stone prohibiting anything? I just wanted to find out. He says no, the stone is not blocking anything. It has the drainage for the colostomy bag. He said there’s nothing that we can do as a Urologist to treat any more. He said that this low urine output is, I guess, the kidney issue failing, I guess.
Patrik: Okay. And who do you think is calling the shots at the moment? Is it the Intensive Care thing, or it is, for example, the Urologist, or, there would also probably a gastric surgeon involved because of the bile issues and whatnot. Who do you think is calling the shots?
Laura: I know who’s calling the shots, it’s the doctor that’s in charge of the CICU here.
Patrik: Okay. Okay. But as part of the abdominal sepsis, do you know what I mean by that?
Recommended:
Laura: Yes, the biliary-
Patrik: Yes, the biliary, that’s right. As part of the abdominal sepsis, there needs to be another specialist involved like a gastric surgeon or a general surgeon because somebody would have had to perform all those procedures and surgery. Who was going that?
Laura: Yeah, that’s another piece of this puzzle that has not been seen is the GI. There was a GI that came down, his name was Dr. Vanessa, and he says well, my partner Dr. Charles will perform the endoscopy and the stent, and then do a biopsy of those nodes down in there. And you know, then they just kind of dropped off. The Dr. Vanessa was the one coming to the room, and it was just kind of like just a little bit of a doom and gloom and that’s it, they’re gone. So, I’d like to bring them back to speak about-
Patrik: I think so. I think that is really going to be important, to bring them back. The other thing that’s important to know is, for example, the gastric surgeon… or let me ask this. Do you know who admitted your mom into ICU? Is it like, because if she went in with respiratory issues or with gastric issues, it’s often not the ICUs admission, it’s the specialist that’s admitting.
Laura: Okay, I know who admitted her and I’m pretty sure not a… there’s a hospitalist. The hospitalist that came around, his name was Dr. Peter, and he’s on a break right now, I guess for the holiday, and he has another hospitalist lady that’s taking his place.
Patrik: Okay. Because again, they often have a different point of view, compared to the ICU. And it would be very important for you to get their point of view.
Laura: Well, as far as I can tell, the one who admitted has the same point of view… I believe it was Dr. Peter that admitted her, and he was just very negative from the start. He just said well, you know… and my mother was combative, which with them poking her, she was very edematous, both her legs and… were very edematous. Her whole body is oozing out that yellow liquid, yeah, so she’s oozing out. And so, he said from the beginning, which I did not appreciate his bedside manner, he was rude to me, I feel like. He said you weren’t going to touch your mother and do these things against her will. I said, look, she has delirium at this point with two infections. She is combative because she’s not feeling good, okay? And she has dementia and it makes it worse if you have infection, you go into delirious. And she was combative. He says, I feel like just keep charging you with oral antibiotics and take her home because I don’t want my nurses being bothered by her like that. And stuff. So, he was negative with me from the start. I didn’t like his manner at all.
Patrik: Sure. Sure. Any talk… as part of the discussion today, any talk about DNR. Do you know what I mean by DNR?
Recommended:
Laura: Oh, I know what you mean by that because that was pressed from the very beginning. All the time, every day, almost on an hourly basis.
Patrik: Right. And any talk about that?
Laura: Well, they just encourage it. Pressure it, pressure it, pressure it. And when they pressure it, I said I don’t want it.
Patrik: Okay. So, you can rule out a DNR.
Laura: Yeah. I mean, they pressured me to do it so many times, and they said that oh, we will keep these measures and protocol, but we just don’t, you know… but you know, here’s the thing. If I had the DNR in place when she had the respiratory failure after her little procedure, she would have been gone.
Patrik: Absolutely.
Laura: Because she was code blue.
Patrik: Yeah. No, absolutely. Okay. So, you’ve covered your bases, which is you haven’t agreed to a DNR. Which means… that also brings me back to the choices they’ve given you, which is ridiculous at the end of the day, you know. I mean, you don’t put patients or a family in a situation like they put you in terms of saying look, by Monday, you need to make a decision about this, that, and the other. That’s just ridiculous. You know, it’s very important that whatever you respond to, just always remember you’re just responding to an external event and it’s your choice in how you respond to that. Whether you respond to it at all, even. You know?
So, let’s just take the worst-case scenario for a moment. Let’s just take that, okay? Let’s just say on Monday they would stop treating her and they would take out the breathing tube and she potentially may not survive that, right? They can’t do that without you approving that. That’s number one. And again, that’s not what they’re telling you; they’re just telling you at the moment, “Yeah, we just do whatever we think is right.” Okay? They can’t do that. And I’ll tell you why.
Recommended:
Whenever it comes to potentially removing life support, and therefore also potentially ending somebody’s life, and I would even go as far that if they take out the breathing tube against your will and without your consent that all goes as far as murder, right? In my mind that is murder. And that also comes down to they must follow hospital policy, and they also have to follow state law in California. Okay? Both hospital policies as well as state laws in California say that you can’t withdraw life support against the wishes of a medical power of attorney or, if your mom was awake and could make her own decision, they would have to. It’s as simple as that.
So those are the things they’re not telling you. They’re just basically telling you, “Well on Monday, we’re going to do this, this, this, and this.” So why are they doing this? Here is what’s also important then: they are managing their worst-case scenario. What’s their worst-case scenario? Their worst-case scenario is to look after a patient indefinitely with an uncertain outcome. That’s their worst-case scenario.
And your mom, at this point in time, fits that worst-case scenario in their mind.
Laura: Yes.
Patrik: Right? Because if they continue treating your mom, and for example, she can’t come off the ventilator, she would most likely end up with a tracheostomy. Do you know what I mean by that?
Laura: Yes, I do.
Patrik: Right. Right. So, when somebody has a tracheostomy, they could be in ICU for weeks or for months, even. Right? So, they are trying to prevent their worst-case scenario by pushing you towards end of life or pushing your mom towards end of life. You know, because they know that if your mom was to pass away, that bed will be occupied in no time. Right? And they know that if your mom is in ICU for a long time to come, you know, that would be very detrimental to their ICU.
Laura: Yes.
Patrik: So that’s… it’s important to understand the bigger picture there.
Laura: Yeah. May I say something?
Patrik: Please. Please.
Laura: They gave me a packet here. This is a Catholic hospital called Victoria hospital. There was a religious person along with the CITU doctor and the hospitalist, those three people they gave me a packet, ethical and religious directives for Catholic healthcare services. They’re trying to say it was unethical for them to continue futile treatment and that it was subjecting their nursing staff to lowered morale.
Patrik: I wouldn’t…
Recommended:
Laura: By treating the dying and there’s no hope and it’s futile. So that’s what they’re saying, it goes against their belief in the hospital to continue to treat my mom when it’s futile.
Patrik: Sure. Are you… if I may ask, have you chosen this Catholic hospital because you or your mom is Catholic? Or is it just-
Laura: No. No. It just happened… actually, we requested this other hospital that my mother was in three years ago, but apparently that hospital, for some reason, was turning down patients and sending them over here to the emergency.
Patrik: Right. So, it wasn’t really your choice to go there in the first place.
Laura: No.
Patrik: Okay. So that’s even better. Because then you could argue on your own cultural beliefs and your own religious beliefs because it sounds like it’s probably not aligned with the Catholic point of view. Right? You could argue that. I tell you, I’ll give you a quick example. We worked with a client in New York not too long ago, and they were in the Catholic hospital too. And they got out of the Catholic system too, very quickly, because of the way they treated their family member. Now, that was a different story because it was a young person, it was a 21-year-old girl who was in ICU at the time, but we advised the family to run, and they did. And they went to another hospital in New York but away from the Catholic system, very much because of similar issues in terms of you know, their beliefs were contrary to what the family believed.
Laura: Yes, I see.
Patrik: Right. And that person, I do believe that person would be dead now if she hadn’t left the Catholic system quickly. And the good news there was it’s probably similar with what you have shared with me now. It sounds to me like they won’t oppose if you go somewhere else. It sounds like that could be an option for you, wouldn’t it?
Recommended:
Laura: You mean to transfer to another hospital?
Patrik: Yes. It sounds like they have suggested that, even, if that’s what you want.
Laura: Well, I was trying to find my options, and I said well, we’d like to go to back to Sierra Hospital and she said but you would have to find a doctor, a specific name and his phone number. And so, I started some preliminary work on that, just on the phone, and I’m having a little difficulty at first try. They said but you can’t do it, Laura, for your mother. You must have the case manager here at this hospital, Victoria Hospital, contact the other case manager at the new hospital, and have them coordinate. And then when I looked back to keep with the case manager here after some time, she said oh, they said no. They said no.
Patrik: Okay. I wouldn’t worry… okay. I contend that if you find a hospital that will take your mom, they wouldn’t be in your way. They wouldn’t be in your way. I tell you again, what they are probably worried about is let’s just say you’re starting the process of getting your mom out to another hospital, they would just be worried in terms of you know, how long does it take, you know. It could take another week. In their minds, your mom shouldn’t be here in another week. You know, all of that. So, what I do believe that if you can get the process started, to me it sounds like you will find another hospital. Are you in L.A.?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!