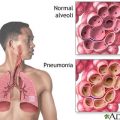
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Dad’s Condition in ICU Improves But Why is the ICU Team Pessimistic About His Prognosis?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Irene, as part of my 1:1 consulting and advocacy service! Irene’s dad is with a breathing tube and on a ventilator in the ICU. Irene is asking what are the important questions to ask during family meetings in ICU.
My Dad is in ICU on a Ventilator. What Are the Important Questions To Ask During Family Meetings in ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Irene here.”
Irene: It’ll take a month for them to mail it to me and the hospital still hasn’t, I still don’t know what the records… Matter of fact, the cardiac doctor who is making rounds, he had questions about the heart attacks. It’s unclear to him what happened when and how it happened. He knows it happened when he was first on that floor, but it’s not clear how much did he vomit and aspirate, or was this the purely an oxygen starvation problem at the beginning. And then there was another one when he was in the ICU. And apparently there was another one when they intubated him as well. So it’s unclear, there’s like three of them. It’s not clear, it’s unclear. And then there’s also another story. Something happened when they were trying to take him down to the MRI room.
Irene: Something happened with the heart. So I know there’s at least three, but I haven’t seen the record. But when I complained to the insurance company… So one nice thing about me complaining to them about a hospital trying to push for a relative, a loved one out too soon, early discharge, you don’t think they’re ready to be discharged, you can complain. And it’s a real quick process. Within 24, 48 hours, you get the response. And what happens during that 24, 48 hours is they get a doctor. The government does, to get all the medical records electronically over to the government. And the government has a doctor that reviews the whole record and then contacts the hospital and asks them, why are you trying to send a patient out? He’s still on life support.
RECOMMENDED:
Irene: And basically they decided, no, we’re still going to cover this patient that the insurance is. But in the meantime, the whole record was shared with the government doctor. So we know for a fact that there is a record, they shared it with the government electronically, through email. And I need to get that record. You need to get that record and be able to review it and see what happened. And the other doctors that are on his case need to get the record. They don’t seem to have it or know it. So it’s a real situation that we really don’t know what happened on what day and what. So that’s a problem.
Patrik: Right, right. And who will be in the meeting tomorrow? So the neurologists, the ICU specialist, who else will be there?
Irene: There’ll be a case manager. There will be a social worker, most likely. Some administrative people. It might be a palliative doctor. They wanted me to meet this palliative doctor two weeks ago. And it may be his primary doctor and internist as well. And there may be one or two outside doctors, his ENT that did the surgery on the sinuses was invited. There might be a handful of people, but internally, the doctor will be the new intensivist. There will be his neurologist too. There might be that the cardiac doctor as well, whoever that is. The palliative doctor and the various staff from the hospital.
Irene: And then I’m trying to get… My father has a doctor who works on his mouth. Does his endodontic work and he’s become like a friend. He’s an older guy. I called him over the weekend to tell him what’s going on with my dad, and I just found out that his doctor is my dad’s new intensivist. It’s the same doctor. So he’s going to write a memo.. he’s going to send a message to him explaining how my father is normally when he’s healthy. How he sits in the dental chair and really doesn’t say much. He’s a quiet person, he doesn’t communicate.
Irene: So he’s going to explain that to him, that do not expect my dad to respond to people talking to him in the hospital. He just doesn’t do it even when he’s healthy and able to get around. So he’s a professor, he’s a teaching professor also at another university. So he has some reputation behind him and he’s friendly with the intensivist. And he says a lot of nice things about this new intensivist, so we’ll see.
Patrik: Okay. And what about the case manager? Is this a clinical person, do you know?
Irene: No, they’re all civilians. They’re all administrative-type people.
Patrik: Administrative. Okay. Right, right, right. Okay.
Irene: There’ll be a social worker.
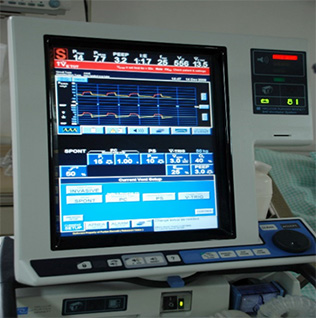
Patrik: Yep. Okay. All right. No, that’s good. That’s good. Let’s see how we go. Is there anything else that you think might be important? It would be good if you can find out before the meeting, what ventilation settings he’s on today, yesterday. So we can see a trend.
Recommended:
Irene: It’s the same setting that they set the last couple of days, they haven’t changed it.
Patrik: Haven’t changed it. Do you remember, I would have to look through my notes? What are the last, what were they…
Irene: Yeah, I do have it. The PEEP is 5. The tidal volume is 300 milliliters a second. The FIO2 is 25. It goes between 25 and 30, back and forth. Then they’re on 12 ACBC. I’m not sure what that means.
Patrik: Right, okay. Carry on. 12 ACBC, is it?
Irene: And its pressure support. It’s not CPAP.
Recommended:
Patrik: Yep. Yep. Okay. Do you know how much pressure support? Do you know the number?
Irene: No, I don’t.
Patrik: Right. So did you say 12 AC / BC? Is that what you said?
Irene: Yeah.
Patrik: I think the 12, I do believe the 12 stands for the number of breaths he’s getting per minute. And that would have to be a zero, you know, ideally it has to be a zero so he can trigger every single breath himself. I would argue that what you’ve shared there with me, he’s getting 12 breaths per minute from the machine. If he’s breathing on top of that, that’s great. But it wouldn’t be enough to take him off the ventilator. They would have to turn the rate, the machine delivered rate, they would have to turn that down to zero to see that he’s breathing. But even if that’s achieved, he would also have to show that he’s neurologically intact.
Patrik: Oxygen 25 percent is fine. A PEEP of 5 is fine. Tidal volumes of 300. I think we said last time, it’s a little bit too low. He would need at least 400. Do you have a blood gas?
Irene: Yeah, they’re kind of in a normal range. I didn’t check it, I might have to see. We have that page here. And it’s… They’re doing venous blood gas. They took you out the arterial line about a week ago.
Patrik: Right. Venous gas is not as good as arterial blood gas, but it still gives us some idea.
Irene: Right. I’ll get on there in a second. The other thing is, he has this anemia or chronic inflammation issue that we don’t know what the chronic inflammation is. So there’s something to do with the body’s response to some kind of chronic disease or inflammation. We’re not sure, they’re guessing it might be the sinuses. It might be something else. We never figured out what that underlying disease was, or inflammation.
Recommended:
Patrik: Right, yeah. You talked about this. Yeah. I see. Okay.
Irene: Bringing up the test result. Pulling up the test here, and see what it is. Let me see. Oh, they didn’t measure it today. It was days when they last measured it. Yeah, they’re not measuring it lately. That’s odd.
Patrik: That’s odd, hmm. Do you know his hemoglobin? Can you see his hemoglobin?
Irene: Yeah. Let me just tell you the next meeting with the venous, you wanted to know what the CO2 was.
Patrik: Yep.
Irene: Okay. It was 51.
Patrik: Okay. And have you got the pH?
Irene: 7.45.
Patrik: Okay. That’s all right. And what about, do you have a hemoglobin?
Irene: A hemoglobin will be under the CBCs. Let me get that. All right. His CBC is improving now, slightly. They had to transfuse my red blood cells into him by next week.
Patrik: Right.
Irene: So his hemoglobin was really low then. Now, it’s 8.4.
Patrik: Okay. That could be a little bit of an obstacle to get off the ventilator as well. A low hemoglobin. 8.4 isn’t too bad, should be all right. But if it drops, it could be an obstacle to get him off the ventilator. He might need a higher FIO2, the lower the hemoglobin. But 8.4 is fine. And 25 to 30 percent of FIO2 is fine. Okay, Irene, I think we got to get to this call tomorrow and I guess see what they say, but I also believe respecting what you want, which is extubate him.
Recommended:
Irene: Right, yeah. The CO2 on the blood is 31.
Patrik: 31, okay.
Irene: That’s the blood. That’s the metabolic panel. It’s fairly out of range, it’s supposed to be between 20 and 30, so it’s fairly…
Patrik: Which means… I can tell you something what that means, straight away. If he’s getting a rate of 12 from the ventilator, with the CO2 of 31, he will be breathing above, which means he’s triggering some breaths himself. I’m almost certain there. Because otherwise, the CO2 might be higher.
Irene: Oh yes. I saw him. What he normally, how he breathes at home, and he’ll lay down on the bed, then occasionally he takes these sighs and takes this big breath and his lungs fill up. I see that, he does that for bed. It’s like a natural… He normally is a shallow breather, you know? Like a half a cup. So am I. Shallow breathing, shallow breathing, and shallow breathing. And then once in a while, he turns to the provider and takes this big breath and then goes out, you know?
Irene: So I think he’s capable of breathing. It’s just a matter of are they capable of monitoring him on a trial extubation safely, including suctioning him and maybe watching everything’s right. Because when I had him on high flow, I remember last month we had him on high flow and the first two days it was pretty precarious. Because I would hear the alarm go off and I would be in the bed, I would be in his room the whole time. And the nurses loved it because they were able to go do other things. I heard it and I would put it in his nose better, and I would straighten him up in the chair, open up his lungs.
Patrik: Yes, yes.
Irene: Dad just got a bunch over, and the nurse goes, what do you want? I was doing that last month, I was there the whole time. He was on the high flow, we had to adjust it. You know, it was kind of scary the first few days because you the alarm kept going off and they were kind of threatening, “Oh, we might have to intubate him, this or that.” So I was always there watching and listening and I didn’t get any sleep for the first two days in there. But we got him through that period where, and then he tolerated the high flow and then got onto BiPAP.
Patrik: That’s good. And how did that go, with talking him through all of that, with the language barrier? You were there all the time, you kept him…
Irene: I was there the whole time, but they don’t know where to touch him. And I have certain areas where I agitate him and kind of steer him out of him slumber and say, “Dad, dad, it’s Irene here.” And I grab his arm, I’ll massage the whole arm and say, “Hey dad, here, it’s Irene.” I’ll take the fingers apart one by one, do that with his feet along the leg and grab the calf muscle on his and stuff. And then I’ll shake him up here. You know, the pectorals and the shoulder, maybe the back of the neck. “Dad, dad, dad here, listen.” You know, but I do it my way that he understands because he doesn’t communicate with anybody in English besides me, and I always speak like that with him, I say other things too. But I’m the one that kind of arouses him out of his sleep.
Irene: Or if he’s not, you know, doing the right breathing I’ll straighten him up and physically… I just physically place his shoulders here, get him secure, and wedge him in with the pillows again, whatever it is. And then I’ll even put my hands on his face, you know, say, “Dad, look, look, wake up, wake up, start breathing, start breathing.” You know? So I do that pretty much when he’s on the ICU and in the hospital room. If I hear him gargling and suctioning, they already… They just leave the suction equipment for me. And they know that if I hear it while I’m sleeping in the room, because I’m a very light sleeper. There’s like a couch there on the hospital floor. I sleep on the couch with a pillow, they give you a seat.
Suggested links:
Irene: I just take these little naps and if I hear the gargling, I’m up and I suction him in the mouth. Suction, suction, you know, put it down. And sometimes the nurse will come in and a new nurse is like, “Wow, how often do you do that?” I say, “I do it as often as I hear it. Sometimes it’s every five minutes. Sometimes it’s not for an hour,” but sometimes he wakes up in a way and he gets a lot of secretions and suction here, suction here. Because I’ll control, I’ll push the button, ask for a nurse to bring respiratory therapist. And then we’ll suction him through the nose. And I hold the head. I hold the head for the RT and he gets up there nice and smooth, suction, pulls it out. The RT, they always want me in the hospital because I’m the one that takes, you know, I steady my dad and she lifts up his hands like this, I’ll put an elbow on it. You know…
Patrik: I understand that. Yeah. I hear you. Irene, do you want to have some time left for tomorrow? What do you want to do? Do you want to continue the conversation? Do you want to have some time left for tomorrow? What would you like to do?
Irene: I don’t know. It’s up to you.
Patrik: No, I think we should leave some time for tomorrow. I’ve got a good understanding now what needs to happen. And I think we should leave the time for tomorrow.
Irene: Okay. What time?
RECOMMENDED:
Patrik: Two o’clock did you say, isn’t it?
Irene: Yeah, unless they change it. They didn’t give me the Zoom number yet. I’ll find out.
Patrik: That’s fine, you let me know, and you let me know. But let’s call it for now. And let’s talk tomorrow morning. Two o’clock. Tomorrow afternoon, your time, two o’clock.
Irene: That’s when the meeting’s going to start.
Patrik: Yeah. Okay. Well, we can talk 10 minutes before, just so you could give me an update.
Irene: Okay.
Patrik: All right. You have a good night, Irene, and we’ll talk tomorrow at two. Thank you. Thank you so much. Bye bye. Bye.
Irene: Bye. –
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!