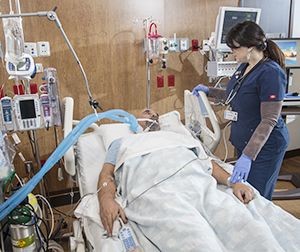
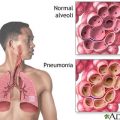
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
If My Dad Will End Up with a Tracheostomy, Why is it Alarming if He Goes Out to LTAC?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Irene, as part of my 1:1 consulting and advocacy service! Irene’s dad is with a breathing tube on a ventilator in ICU and Irene is asking when is the best time to extubate her critically ill dad.
When is The Best Time to Remove the Breathing Tube of My Critically Ill Dad in ICU?
Patrik: Hello.
Irene: Hello doctor.
Patrik: I am not a doctor, I’m a critical care nurse.
Irene: Critical care nurse, nice to meet you sir.
Patrik: Nice to meet you. Is it Irene is it?
Irene: Yes sir.
Patrik: Irene, are you in hospital at the moment or?
Irene: No I’m at home. I’m not allowed in the hospital right now because they locked it down. Normally I’m in the hospital with him.
Patrik: Right, but you are not in a position to be in the hospital at the moment?
RECOMMENDED:
Irene: No. I just got off the phone with the neurologist so either zoom or phone.
Patrik: Right, I see. And are you the medical power of attorney for your dad?
Irene: Yes I am.
Patrik: Great. And what’s your biggest challenge at the moment?
Irene: Can you hear me okay?
Patrik: I can, I can.
Irene: Okay. The biggest challenge right now is we’re doing some trials to wean him off of the endotracheal tube. The tracheal… Not tracheal, but the endoscopic tube that’s in his intubation.
Patrik: Yep, the breathing tube.
Irene: Yep, he’s not been able to come off it yet. They tried this morning but his blood pressure went up to 200 and the heart rate shoot up to 140.
Recommended links:
Patrik: Right.
Irene: So they discontinued and just turned the machine back on. But the doctor today asked me if I had permission to do a trial extubation where they’ll try to put him maybe on a high-flow. Let’s see how he tolerates it. So what happened is, dad had to… What?
Patrik: How many days is he in the ICU now?
Irene: He’s been in there for three weeks now.
Patrik: So two weeks. Was he on the ventilator from day one in ICU?
Irene: On Day 2.
Patrik: Okay. So it’s 13 days ventilation now.
Irene: Yeah.
Patrik: Okay.
Irene: And in a nutshell what happened, he’s been in the ICU a couple of months ago. He was hospitalized for aspiration events and pancreatitis. Both of them built up fluid into the lung’s sepsis. And I was in the ICU with him, he was on BiPAP at nighttime and hypo during the day. And within a week got him out of the ICU, they put him in a hospital room and then he went home within two weeks of the whole time.
Patrik: Okay.
Irene: He had a sinus infection that was operated on, it was a long-term fungal ball, so it was removed. He has a lot of post-nasal drip and we were treating it, there was still residual infection in there in the following months. End of last year, I overfed him. He vomited a little bit and that’s what got him in the hospital. And then after a month, I think they sent him home a little bit too soon, he developed pancreatitis and again edema and sepsis, in the lung pneumonia. And then went home after that stay in the ICU and then this time around, I started hearing a little bit of wheezing at home and his temperature dropped down to 94 and that’s when I talked to his pulmonologist. He said, “Bring him to the emergency room. He’s not going to stay in the hospital he’ll go home. I’ll X-ray his lung, maybe give him a strong antibiotic, I doubt he’ll stay in the hospital.”
Irene: But after I took him to the ER they didn’t allow me to go upstairs with him. They took him by himself. And what happens with dad because of the sinus, if they lay him flat, he immediately aspirates the secretions from his nose and it will run into his lung and that’s what happened. It was a mistake in the hospital. Every time I’m with him for the first 24 hours to kind of get the RT and everybody on board, how we take care of him. But they laid him flat, his face went blue, he was drowning in his secretions and he had three heart attacks.
Recommended:
Patrik: Plus the COVID?
Irene: No COVID.
Patrik: Oh, there’s no COVID?
Irene: Yeah.
Patrik: Okay. So COVID, negative.
Irene: No COVID.
Patrik: Okay.
Irene: Yeah, we are all COVID negative.
Patrik: Okay good, good. So the main reason that led to this is basically the heart attacks and probably lungs are decompensating because of it?
Irene: A little bit, yes. But they recovered the lung, they put him on antibiotics. He’s been on an antibiotic now for a week and I think they’re going to stop it today. There’s some improvement, they took the arterial line out. His new doctor this week called me, he is breathing, initiating breathes on his own but they’re very faint. And he may have a trial to remove the breathing tube and get him on the other one. But he also discussed tracheostomy and I pushed back on that. I read all your sites, all your info over the weekend a couple of times to learn it. He had started pushing back on the trach and told them, you know my dad recovers. He’s in a sleep right now but he is responsive to brainstem. He’s responsive to pain.
Irene: They even have him on a bike but he’s not participating actively on it twice a day to get in some physiotherapy like you suggested, that started yesterday but he still… He opens his eyes and closes them throughout the day. He’s got good color, pretty much he’s recovering. I had them transfuse him yesterday with my RBCs because he has low hemoglobin, below seven. Second time he was below seven on that. His liver got injured, chest compressions and his liver enzymes went really high but they’re starting to recover. He was breathing. The doctor says or else initiates but he’s very faint. But the big worry of everybody is neurologically. They are saying he has some kind of hypoxic, some kind of oxygen deprivation injury to the brain and he’s not waking up to their satisfactory. Neurologically he is not waking up.
Recommended:
- The 10 answers to the 10 most frequently asked questions when your loved one isn’t “waking up “ after an induced coma!
- My Dad is in ICU after a subdural haematoma, he’s had multiple surgeries and he’s not waking up! Help!”
Patrik: Okay. Is he still on sedation?
Irene: No. He really has been off sedation for some time. He tolerates the breathing tube pretty well. That’s why another reason why I was thinking that with the tracheostomy.
Patrik: Yeah. Let me ask you a few questions. So when you say he’s been off sedation for some time, can you quantify that? Can you quantify how long? How many days, tell me how many days has he been off sedation?
Irene: What do you mean when a heart stopped?
Patrik: No. How many days has your father been off sedation?
Irene: Oh, I think almost immediately. They were trying to wean him off a sedation.
Patrik: Okay.
Irene: They were giving him a blood pressure steroid to bring up his blood pressure, that’s been taken off now. And now there’s I think norepinephrine but it’s intermittently given to him because he tends to maintain blood pressure but it’s kind of weaning off now.
Patrik: Okay, good. And when they’re saying he has a neurological event, has that been confirmed with a CT scan of the brain, with an MRI scan of the brain?
Irene: We did all the studies. This is a little background back mid last year..
Patrik: Acute, acute, acute this is now, he’s not waking up.
Irene: No, nothing new.
Patrik: Nothing new.
Irene: They haven’t found anything. An EEG test as well was done, his burst padding there’s some slowness on the EEG. However, we compared them back to the last one done when he was in the ICU, and there’s no changes to the imaging.
Patrik: Okay. Have they done a CT scan or an MRI scan of the brain since this admission?
Irene: Yes, that’s why I’m saying. They compared it..
Patrik: They have?
Irene: Yes, and they compared them to the other ones and there’s no change.
Patrik: All right.
Irene: Same thing with the EEG, no change.
Patrik: Okay. Do you know her Glasgow Coma Scale? Do you know what I mean by that?
Irene: No, I do not.
Patrik: That’s okay, I’ll send that to you when we come off this call. I’ll send you like an assessment score. Glasgow Coma Scale is a neurological assessment tool, it goes from a three to a 15. You and I talking, we are both at Glasgow Coma Scale of 15. The lowest Glasgow Coma Scale is three, it’s basically a vegetative state, your dad will be somewhere in between. But it is a very good assessment tool that can guide the nursing staff, the doctors but also you as a family member. I’ll send that to you.
Recommended:
Patrik: Okay. So tracheostomy… Look you need to find out the Glasgow Coma Scale. You really do, because if he’s alert and oriented, if he can obey commands then he has a chance of coming off the ventilator. If he’s not alert and not obeying commands, it’s not impossible but it will be more difficult for him to come off the ventilator. Right, with the heart attack or with the heart attacks what have they done? Have they sent him to cath lab? Do you know what I mean?
Irene: No, not during this admission. He’s been through a cath lab in 2016, and I know he was like 80, 90%. But since then he’s been through ECP treatments. It’s the enhanced external counter pulsation, where they squeezed the… Assist the diastolic blood uphill 35 sessions a year. He’s done three years ago and he’s been asymptomatic on his heart since then. He was exposed though, to toxic waste up here. We had the worst gas blow out disaster and we were evacuated from that in 2016. And then recently we had a big fire where we were evacuated from it. So there is some of that toxic substances that he was exposed to for a while there, but I’m not contributing that but there’s some background there.
Patrik: Right. What are his kidneys doing? Are the kidneys okay?
Irene: His kidneys are okay. Most of his numbers are looking better. His liver was… His enzymes were very high. There was liver damage, pretty extensive when they did the chest compressions. They did several rounds of chest compressions on him, he’s a small little thing.
Patrik: How long ago did they do the chest compressions?
Irene: On a weekend.
Patrik: And for how long?
Irene: I know his heart stopped they said one time for 30 minutes.
Patrik: My goodness. Right. And the CT scan of the brain was that before the CPR or after the CPR do you know?
Irene: All the scans on the brain were after. He was too unstable to do MRI for a few days. They got the CT done right away. And they were actually getting him ready for MR and he was in code again. So they didn’t do the MR until just last week when he was stable enough.
Patrik: Okay. So when you say the CPR was during the weekend, was that Saturday a week ago?
Irene: Yeah.
Patrik: Okay. I see. Okay. Right. And at the moment your biggest question… Your most important question from what I understand now is, should you consent to a tracheostomy or not? Is that where you’re at?
Irene: It’s that and then this trial extubation that’s been proposed as well tomorrow. At 5:00 am is when the respiratory therapists are in the room, maybe said that I’m allowed now on zoom 5:00 a.m. So I want to be there and observe what goes on. And I’m not sure if it’s safe to extubate him right now based on this morning’s findings that his heart rate shoot up to 140 and he became hypertensive a few hundred and he didn’t tolerate it for very long before they came back on.
Recommended:
Patrik: I’ve written about this extensively on my blog, when to extubate. If you go onto our website and you type in, when should a patient be extubated? I’m sure you will get an article about that. There are certain boxes that need to be ticked before you extubate a patient and one important one is following commands. That’s an important one, which is where the Glasgow Coma Scale comes in. He needs to be able to breathe on pressure support or CPAP for at least 24 hours, for at least.
Patrik: He needs to have adequate arterial blood gases. He needs to be able to cough. He almost needs to be in a position where he can cough out his own tube. And you’re saying he’s still on norepinephrine or levophed, I can’t remember what you said. That shouldn’t stop him from being extubated, but those are the main points that I just mentioned. If those boxes aren’t ticked there’s no point in extubating. When you extubate, you have a limited time window. You got to choose the right time window because otherwise it could backfire. How old is your dad?
Irene: This year 86.
Patrik: That’s a very good age. I’ve seen people being successfully extubated at that age. So there shouldn’t be something stopping from that. It would help if you and I can get on a call to the doctors before they extubate, it would help. We could ask those questions. You’ve got some questions. If you and I were to talk to the doctors I could ask questions back straight away. I can definitely see an advantage there if we could do that. It sounds like you’ve done some research already. You have some things to run with.
Irene: Right, right. No, I would welcome you on a call and actually I would welcome you if… What I observe of the respiratory therapist do every morning at five.
Patrik: Right. Yeah, look we can definitely set that up if you would like that.
Irene: Okay. Yeah I would.
Patrik: Go on.
Irene: There’s this whole neurologic question and I wanted to tell you. Dad has been in the ICU last year, and it takes him about five days to wake up in those situations. Now that he has had this heart issue, it seems like the wake up period is going to be much longer.
Patrik: Right.
Irene: I heard some promising things from the doctor, the pulmonologist, the intensivist. But then at the same time I heard some negative things from the nurse that takes care of him and said, your dad has been in stupor for a long time. He’s in dire straits, there’s no wide avenue for improvement. He’s got some kind of different type of brain injury, hasn’t really improved neurologically. And I know he does not do commands right now and take command. He’s still sleepy, he opens his eyes when they move him and talk to him, he’ll open his eyes and take note of them.
Recommended links:
Irene: But he’s just so exhausted that he does not respond yet to, hey squeeze my hand or, pick your foot up or something like that he won’t do. He does cough quite a bit into the tube, his face will turn beetroot red. He has secretions up here that drip down. And I noticed when I’m on zoom for the hour or so, I’ll see my dad’s face get really red and he whoops up a cough and then they’ll have to suction him a little bit extra in his mouth. He has a cough and gag reflex, it’s pretty strong. And there’re other times I’ll see him yawning and moving his body and taking a deep breath. So maybe we could avoid cutting into his throat. I don’t really think he would like that anyway. He’s the type of person when he’s well, he’s going to pull things out.
Patrik: Yeah.
Irene: He’ll pull the feeding tube out of his nose. He’s very hyperactive. He’s a dance teacher. So he’s a very very… A physical guy. Even though he’s small, he’s lost five inches of height in his back, so leaving him in the bed is not good either. Traditionally we’re having our cardiac chair to sit him up. The mid lobe has, was like a mid-lobe area that gets collapsed with all the institutions. So we need to get him out of the bed.
RECOMMENDED:
Patrik: Absolutely, absolutely. He needs to get out of bed. There’s no doubt about this. Look, mobilization is inevitable for anyone that wants to get off the ventilator, it’s inevitable. And the challenge is if a trach needs to be done down the line… I always see in my practice that patients don’t get mobilized. And that’s one of the reasons, not the only reason but it’s one of the reasons why they can’t come off the ventilator in a good timeframe. And they often end up on ventilators for the rest of their lives because they don’t get mobilized. It’s terrible.
Irene: Right.
Patrik: So mobilization is inevitable. I know the first couple of weeks in ICU people don’t necessarily get mobilized because they’re too critically unwell. But as soon as you can mobilize, you need to mobilize. Now the Levophed that you mentioned earlier, or the norepinephrine depending on the dose might stop him from being mobilized. That could be a contraindication depending on the dose. But as soon as that’s off there shouldn’t be anything stopping him from mobilizing. And it will help him with expanding his lungs, it will help him with cognition, it will help him with everything.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!