Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Eva as part of my 1:1 consulting and advocacy service! Eva’s husband had a cardiac bypass surgery and stroke in ICU, he is delirious with a MAP of 78 is he deteriorating?
My Critically Ill Husband is on Dialysis and in ICU due to Septic Shock. He is not sleeping, is this another sign of deterioration?
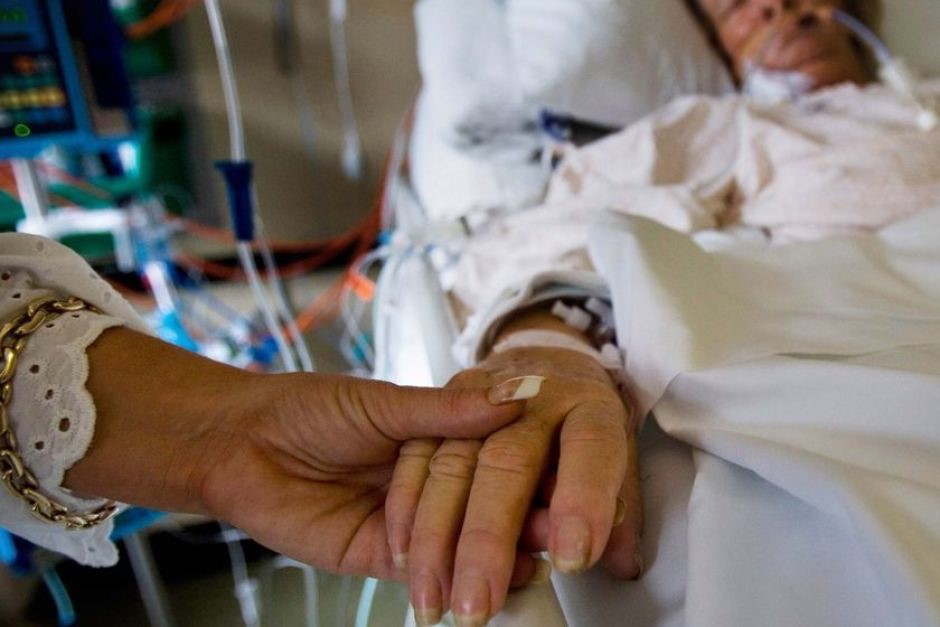
Eva: Hi, Patrik. It’s Eva Peters calling from Perth, Australia. How are you?
Patrik: I’m very well, thank you. How are you?
Eva: I’m not so great today. We had a not bad day medically yesterday, but I don’t know whether you remember everything that we chatted about in terms of Frank’s mental health and the push about making decisions.
Patrik: Yes.
Eva: Well, unfortunately it now has meant that he has not slept for almost three days and slid back into a delirium.
Patrik: Oh, my goodness. That is so bad.
Recommended:
Eva: Which is exactly what I predicted.
Patrik: Yeah. What you predicted and what you see.
Eva: Yeah. So, I’m just beside Frank so I’m going to watch what I say because he is still not speaking. We will have rounds coming up.
Again, we talked a little bit about the change in settings yesterday, and so I wanna run that by you. Yesterday, he was on Norepinephrine at about 4.9 all day, which meant that his MAP was quite a bit higher … it was in the mid-60s for most of the day, what I saw … and today they’ve got it at 3.8, which is up in the mid … it’s running at 62-61 right now. The arterial line on his blood pressure cuff is actually showing about 78, is showing quite a bit higher. The setting here is not correct.
Patrik: Well, the MAP on the blood pressure cuff is 78.
Eva: Yes.
Patrik: How often do they check the non-invasive blood pressure reading?
Eva: Yesterday it was set for every half hour. Right now it’s every fifteen minutes.
Patrik: Right. If they’re doing that, that means they’re not really trusting the arterial line.
Eva: They did wake him up in the middle of the night, or he wasn’t sleeping, to put a new one in because the other one they said was not working. So, part of the reason is, from what I understand, from where he’s sitting he slipped down in the bed so the leveller is not at the right height to actually be reading properly on that. So, I’m guessing the blood pressure cuff is probably more accurate. I’m wondering why they would have it set much higher within the MAP of 55. When they talk about a MAP of 55, is that over a 24-hour period?
Patrik: No. It’s really a live reading. It’s a live reading because if, for whatever reason, the MAP goes below 65, the kidneys are not perfused, right?
Eva: What I was told yesterday, I asked specifically about that, and the doctor said that a MAP of 55 for him would be appropriate to perfuse him.
Patrik: But why? If you look at literature, and it’s been drummed into pretty much everyone in ICU that a MAP of 65 is needed to achieve, sustain, the kidney perfused … I would really like to know from this person, why all of a sudden for your husband the rules are changing.
Eva: It does appear that the MAP is running higher than what he has said, so again I’m not quite clear on why that would be. If they were reaching a target one of 55, why do they actually have the Norepinephrine turned up high enough to make it higher than that?
Patrik: And you know what? From what we’ve discussed it almost comes down to … You know, you remember they are really negative, and on the other hand you have the respiratory therapist coming in this week and saying, “Oh, yeah, his breathing is really good.” It almost sounds to me like it’s all about lowering expectations; but at the same time, doing whatever is necessary to keep your husband alive and well. Because they know that they can’t stop this treatment, right? From my perspective, it all comes down to having low expectations and telling you, “Oh, yeah, a MAP of 55 is fine,” but in the meantime they do treat him properly anyway.
Recommended:
Eva: Okay.
Patrik: Which is what we talked about yesterday. It’s all about looking for actions and not so much for words. The words are designed to keep your expectations low, and you’ll keep your husband’s expectations low; but at the same time they keep treating him properly, which I think is way more important than what they say. Again, it all comes down to watching the actions versus watching the words and making sense out of it. I would argue that if the MAP is 78 on average, they should reduce the Noradrenaline.
Eva: Right. Yeah. So, I’m wondering why that’s changed. A couple of days ago that’s what they were doing, they were reducing it in response to what the blood pressure was reading; and yesterday and today, that’s not happening; it’s just stayed at the same level.
Patrik: Have you asked?
Eva: No, and our rounds are coming up, so that’s why I was asking. That’s why I called, about why there’s been that change.
Patrik: Yeah. Look, I tell you why … If you have an arterial line and a non-invasive blood pressure cuff, the non-invasive blood pressure cuff usually always supersedes the arterial line; it’s more accurate most of the time, right?
Eva: Right.
Patrik: So, if I was handling a patient and I had the arterial line and the blood pressure cuff, I would always go with the blood pressure cuff because the arterial line is too temperamental.
Eva: Then should they be reducing it in response to a 78 blood pressure or MAP?
Patrik: I would strong argue that, very strongly argue that. Now, there’s a number of reasons why you shouldn’t overshoot your target, especially not with Noradrenaline or Norepinephrine. The Norepinephrine is a great drug; but it also, like with any other drugs, it has side effects. Your husband would have been on Norepinephrine for probably now a number of days, but he would have also been on Norepinephrine while he was on ECMO.
Recommended:
Eva: Oh, right. Yeah.
Patrik: Right? So, one of the main side effects of Norepinephrine, especially when it’s given for prolonged periods, is really vasoconstriction. I don’t want to get dramatic here, but basically what it does is it reduces blood flow in the skin, and therefore … So, your husband is bed-bound: imagine, you reduce blood flow in the skin that increases the risk for pressure sores.
Eva: Yeah.
Patrik: Do you know whether he’s got any pressure sores?
Eva: No, he doesn’t.
Patrik: Okay. Good. Good. But the Norepinephrine, that’s one of the main side effects; it reduces peripheral perfusion. Because what the Norepinephrine does is it’s concentrating blood towards the heart, which means it’s drawing the blood out of the peripheries and it reduces skin perfusion, and that increases the risk for pressure sores. So, if the MAP is higher than what we’re aiming for, reduce Norepinephrine.
Eva: Yeah. So, I just don’t understand why they would have left it running so high all day yesterday. Are they checking, are they using the arterial line, which is not measuring correctly, as far as what I have been taught? So, if the leveller is too high, does the blood pressure read lower or the opposite?
Patrik: If the level is too high, blood pressure is reading lower. Yes, absolutely.
Eva: Okay. What I was told is it should be just at about the level of his armpit.
Patrik: Yes.
Eva: And I would say it’s about five inches above that because he slid down in the bed.
Patrik: You know what they can do? There is the transfuser, or what they refer to as the leveller, right?
Eva: Yeah.
Recommended:
Patrik: You can use the term interchangeably. If they fix it with a tape on his arm, then it should always be in the right position no matter what. Right? So, they could just use a tape and should fix the transfuser on his left or on his right arm. Then, he can move up and down, whichever way, and it would always be-
Eva: They’ve got it fixed into the actual line that’s going in, from what I see.
Patrik: Right. Okay.
Eva: It’s where the actual line runs down. They’ve got it fixed onto a little thing that holds a number of different probes, I guess. So, it’s just sitting on the IV stand.
Patrik: Okay. I see. It’s external almost. It’s outside of the bed.
Eva: Yeah. It is outside of the bed.
Patrik: And that’s why it would be dependent on your husband moving up and down. Yeah, okay. I see.
Eva: There you go.
Patrik: How long has this arterial line been in? Do you know?
Eva: They just replaced it last night, and that one had only been in a couple of days before that. They had a brachial line before that, and so they removed that one and put in an arterial line about three days ago, and then removed it last night and put another new one in.
Patrik: In his wrist?
Eva: In his wrist. Yeah.
Patrik: Why did they change it after only three days? Do you know?
Recommended:
Eva: They said it wasn’t working anymore.
Patrik: Okay. All right. In terms of what really concerns me is obviously your husband’s not sleeping and slipping back into a delirium because of that. Has there been anymore …
Eva: We’re waiting for the psychiatrist to come in to consult, but no indication that they will stop by or check on him. Nothing.
Patrik: Have there been any more discussions, as far as you’re aware, between the doctors and your husband while you were not present?
Eva: Because I trusted them last night and went home, I don’t know. So, I came back to his NG tube taped to his face, he was awake all night, they had to bandage up the new arterial line because he was picking at that. They had taken his teeth out and no one can put them back in again because they don’t know how to do it, and he has not slept, and I am with no indication of getting someone here to … Well, they’ve just said they don’t want him to get any medication during the day because they want him to sleep at night, which is because they all go off on two hour breaks.
Patrik: Yesterday, for example, you were present during the round?
Eva: Yes. Everything was looking good. The … darn, I can’t remember the name. It starts with A, that you measure indication of organ failure. Do you know what I’m meaning?
Patrik: No, I don’t. Indication or organ failure. Which organ failure?
Eva: Lactate. Sorry.
Patrik: Oh, lactate. Yeah, lactate.
Eva: It doesn’t start with A. It’s lactate. So, that was normal, which was great. White blood count is still elevated. He’s off his antibiotics, off of the hydrocortisone. They did one of the leg-levelling tests to decide whether he needed more fluid or less fluid, decided that he needed less fluid, and so drew off additional fluid last night.
Patrik: Do you know what they’ve giving him? Just some saline, some normal saline, or did they give him some albumin?
Recommended:
Eva: No, they actually are pulling off more fluid.
Patrik: Oh, they were pulling off.
Eva: They decided he needed more … Yeah. They upped the rate last night.
Patrik: So, fluid removal?
Eva: Yes.
Patrik: Okay. I understood they were giving fluid.
Eva: No. They decided he actually didn’t need …
Patrik: Okay.
Eva: They thought that might help with his blood pressure and decided it was the opposite, and basically they needed to have more removed.
Patrik: Okay. What is their long-term outlook with dialysis? Do you know?
Eva: They’re guessing it’s long-term, that the kidneys won’t come back.
Patrik: Right. Okay. When your husband was on ECMO, was he on dialysis as well?
Eva: No.
Patrik: So, this is new.
Eva: No. This occurred after a huge Lasix, or a couple of boluses, they shut down, and then they got going after a few days of CRT. When they stopped it, then they started again. The creatinine had gone up, so they could intermittent just one session, and then they were working on their own. But what happened was when he went up to the ward, they dehydrated him four out of the seven days that he was there by not giving him fluids. So, coming down this time, they’re predicting more impact, but I don’t know whether the long period on CRT that most likely they’re not gonna start up again. The last time they did say it could take months for him to recover. Do tell me a MAP of 55 should be sufficient to perfuse him, if that’s going to help. I don’t know how you tell without a try.
Recommended:
Patrik: Yeah, that’s right, and you can tell by, “Are the kidneys recovering?” How do you check that, number one, urea and creatinine when you’re checking blood? And number two, simply-
Eva: Yeah. So, it is continuing to come down. I think the creatinine was 127 yesterday. I’ll ask that again.
Patrik: You’re also looking for, “Is he producing any urine?”
Eva: He doesn’t have a catheter in.
Patrik: Do they use the bladder scanner, like an ultrasound for the bladder, kind of thing?
Eva: Every now and then. The last time I think was on Monday, and he was actually complaining about pain on his right side.
Patrik: That could also be from just being bed-bound for such a long time.
Eva: For sure. Yes.
Patrik: But in order to check whether he’s producing any urine, it’s really a matter of using the bladder scanner and see whether the bladder is filling up.
Recommended:
Eva: They kinda shrugged and said, “Well, it’s not,” when the resident asked about it yesterday, again not holding out much hope.
Patrik: When you had the rounds yesterday, was there any more discussions from the doctors with your husband in terms of “decision-making” and what not?
Eva: We had discussions, and then the doctor came at the end of the day, and I actually sent everyone away. I said, “There will be no more.” But we did have a brief discussion with the doctor who apologised and said that they just really wanted Frank to be a part of the team, Frank and myself to be a part of the team, that’s what this discussion was about, and he again went to long-term goals after this. The spiritual counsellor who was there stopped him and said, “Long-term goals right now, that’s not a thing to be …”
Patrik: They’re far away.
Eva: Yeah. So, we talked about the fact that for Frank, it’s regaining the ability to shave himself, and being able to sit up on the side of the bed, that those were things that to him measure progress.
Patrik: Absolutely.
Eva: And so I think perhaps the doctor understood that, or indicated that a little bit, but it’s certainly one of the issues that we do have here is physician-assisted suicide, and that actually was what he was offering the other day; I didn’t even know such a thing existed.
Patrik: Oh, you’re talking about voluntary euthanasia, basically.
Eva: That’s exactly.
Patrik: Is that legal in Perth, Australia?
Eva: It is. I had no idea until a lawyer said that it is.
Patrik: Right. In any state where voluntary euthanasia is legal, I have always been concerned that this could be misused in ICU. I have always been concerned about that. Always.
Eva: Well, here we go, and this is a Catholic hospital.
Recommended:
Patrik: Oh, my goodness.
Eva: Who said that they would not use that?
Patrik: Yeah, but the doctor might not be Catholic. I don’t know.
Eva: Well, it should be…
Patrik: You’d think that they would be selecting their staff potentially according to their faith, but I don’t know.
Eva: Well, or if you have a policy about it or not that’s … I mean the hospital policy needs to be followed whether you personally agree with it or not agree with it.
Patrik: Correct.
Eva: Generally, it’s something that people ask for, not that it’s put out there and people are forced to choose between one option and that option. So, in terms of mental health, I’m pretty sure that that is why he is now in delirium because he’s afraid to go to sleep, which is what the doctor said.
Patrik: Yeah. I think you mentioned in one of your emails that he is on Seroquel?
Eva: Yes.
Patrik: How much is he getting? Do you know?
Eva: I think … Yeah.
Patrik: 25?
Eva: It was 12.5, and so they popped it to 25 at night, but that was not … He’d slept for about an hour and a half and then woke up again, and then I think they maybe gave him a second dose and that didn’t work.
Patrik: Anything else he’s getting to “sedate” him?
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Eva: Paroxetine. That’s not to sedate. That’s again a minimum dose.
Patrik: When you were saying yesterday the counsellor was here, is that from the Ethics Department or is that from other department?
Eva: No, that’s their spiritual counsellor. But I did meet with the Ethics Department, and her as well, to talk about again my concerns about how we was being badgered about this.
Patrik: Yeah. And it sounds to me like if they apologised, the Ethics Department must have spoken to them because …
Eva: Yes.
Patrik: That’s good. I’m glad.
Eva: But it hasn’t fixed the problem.
Patrik: No, no. It hasn’t fixed the problem, but at least it’s good to stop, to them putting pressure on, for now.
Eva: Not really. No, that didn’t stop that at all. I had to send people away. They were all gathered around the foot of his bed again because he was still aware yesterday and there was this feeling of urgency for him to make a decision while he was aware; because when he’s not, then he cannot make a decision.
Patrik: Sure. But for now, in order to take the pressure away, it’s almost like … I mean what’s your feeling? I mean your husband has a strong will to live? Do you think he would even-
Eva: Absolutely.
Patrik: Right. We wouldn’t consider giving up?
Eva: Not that way. No. I didn’t even know that was what was being suggested. No, I don’t think so. I did say to them, because his speech is … now they’re taken his teeth out, so it’s even harder … I said his actions speak louder than words. He is cooperating and participating until last night when now he’s picking at things; they may use that as a sign; I’m worried about that.
Recommended:
Patrik: A lot of patients in ICU can become delirious especially after sleep deprivation and especially after not being in natural daylight for weeks.
Eva: Yeah.
Patrik: So, it’s nothing unusual, unfortunately. At the same time, the delirium is often not being used to stop treatment. It’s other signs usually that would be … You know, it’s more like the organ failure side of things when people might say yes.
Eva: Right.
Patrik: So, the delirium is definitely a concern because it’s torturous being in ICU without being delirious.
Eva: Anyway, yes. Yeah. I’m so sad because we only had two days where he was able to talk with his family and friends, and all he had was people stopping by not for positive things. I said, “Unless you’re coming by to just chat and have a positive interaction, go away.”
Patrik: Right. Good.
Eva: But I don’t know what they did last night and that’s … you know.
Patrik: Concerning.
Eva: Concerning.
Patrik: Yes.
Eva: I had a request on his file that I’d be present at any kind of procedures because he is very anxious, and so previous to this I’ve been there. So, they told me that he agreed to it and that it wasn’t a problem, but internally it is.
Patrik: Absolutely.
Eva: He doesn’t show it outwardly.
Recommended:
Patrik: Any more talk about having a cardiologist involved in all of this? Or have you asked again?
Eva: No, but I will ask today.
Patrik: So you’ve got to keep asking for what we believe is appropriate, right?
Eva: Yeah.
Patrik: And this particular consultant that’s on this week, he won’t be finished for a while. Is that right?
Eva: I think he’s actually on for one week.
Patrik: That means he would finish when? By Sunday?
Eva: That’s what I heard. I can ask again. The other doctors were on for two-week rotations.
Patrik: Right. It depends.
Eva: Am I talking too much?
Patrik: It depends, but most of the time it’s one week.
Eva: Here it has been two weeks.
Patrik: Okay. Sure.
Eva: But I don’t know for sure. I can check that out.
Patrik: Your husband would have a catheter for the dialysis, right?
Recommended:
Eva: Yeah.
Patrik: Where is that catheter? Is it in his shoulder or is it in his groin?
Eva: No. It’s in his neck.
Patrik: In his neck. Okay. The reason I’m asking is we were talking about getting your husband mobilised and potentially keeping him on the edge of the bed, and they should be able to do that as long as he’s got what’s called the vascular catheter in his shoulder. If it was in his groin, mobilisation would be very difficult.
Eva: Right. He did have one to start, and then they moved it to the … The catheter wasn’t there; it’s always been up there.
Patrik: Okay. Good.
Eva: He has nothing in his groin.
Patrik: Okay. Have they tried to mobilise him this week at all?
Eva: No. Well, just the cardio chair.
Patrik: Okay, that’s good.
Eva: And today he’s too sleepy.
Recommended:
- What if you could reverse the Intensive Care team wanting to “pull the plug” or “withdraw treatment”
Patrik: Is he tolerating that? Is he tolerating the cardio chair?
Eva: Yeah. Up all day yesterday. It was their plan to tire him up.
Patrik: Good.
Eva: Physically it tired him out, but…
Patrik: Right. And again, Eva, that is important information because if they were completely giving up they would not do that. That’s why I-
Eva: Well, I had to push, but yes-
Patrik: Yes you have to push for it and keep pushing.
Eva: Yeah.
Patrik: Definitely keep pushing, but I’m glad to hear that those things are happening. Is your husband on oxygen, a little bit of nasal oxygen?
Eva: No.
Patrik: Oh, good.
Eva: He only needed a little bit of that last week, and so that’s been off.
Patrik: Oh, good. That’s a good sign.
Eva: He’s back to being NPO again today just because he’s not staying very awake, which made me very sad. He ate way more yesterday than he ever had. Jessica came in, ripped the old one off and put NPO up. That’s a little heartbreaking, especially since they took his teeth out and can’t get them back in.
Patrik: You know, it’s those little things that really make a difference.
Eva: Well, sure.
Patrik: It’s not being to talk. Not being able to talk is just like …
Eva: And it’s only this nurse who can’t do it, and he refuses to ask anybody else to do it.
Patrik: I see.
Eva: Whereas other nurses just went and got someone else when they had difficulties with it.
Patrik: You think there’s a realistic chance he might get them back in with the right nurse?
Recommended:
Eva: Yeah. It’s just a little difficult. Because he slipped right back there.
Patrik: Okay. How many days has it been now on this admission, on this ICU admission, two weeks did you say?
Eva: 10 days.
Patrik: Okay. This communication from there needs to stop and it really needs to go from end-of-life talk to, “How can we take one day at a time?” It’s all about one day at a time, and really getting him through this day, and getting his through tomorrow, and look for the little signs. You are there pretty much 24-hours a day. You said you went home last night, which I think it’s good that you did that.
Eva: Well, not really.
Patrik: No, no, no… It was alright
Eva: No, no, no. Yeah, but it’s …
Patrik: Yeah, but you need to look after yourself as well.
Eva: Yeah, but it comes down to a … I have had people come and be here while I was not there; I’ve used them all up. With that being said, I have talked about hiring someone to come in just to provide that little bit of support while I’m not here, and especially them being here during the night when he is just left pretty much alone and is not sleeping. So, that makes it a very, very long time to be sitting, which does not help with delirium.
Patrik: No, not at all.
Eva: If you’re not being reoriented and talked to it’s a long time.
Recommended:
Patrik: Absolutely. At the same time, your well-being is just as important.
Eva: Well, I can sleep during the day.
Patrik: Right. Having been a shift worker for many years, and done night shifts for many years, I know how tiring it is.
Eva: Can you hold just a minute? I just want to check with Graham here.
Patrik: Sure.
Eva: (silence)
I’m sorry.
Patrik: That’s okay. So, where to from here? I guess now that you also mentioned the euthanasia part, that is a real concern, and you really do need to watch them.
Eva: Yeah. Can I have you hold one more time?
Patrik: Sure.
Eva: (silence)
Hi. Thank you for staying.
Patrik: That’s okay. I think, from what you’ve shared so far today, it’s really a matter of, on the one hand, the clinical things seemed to stabilise, if not improve.
Eva: Yes.
Patrik: It’s really all about the communication.
Recommended:
Eva: Yeah. I think perhaps what I need to do is to actually write something up and have it on his chart.
Patrik: Yes.
Eva: About what wishes we have discussed, and we can put that health care directive on there.
Patrik: Very good idea.
Eva: Yeah.
Patrik: Very good idea. And as I mentioned to you, you need to be repetitive.
Eva: Okay.
Patrik: You almost need to sound like a broken record until they get it, until they really understand you and your husband don’t want that talk about end of life while he’s here.
Eva: Yeah.
Patrik: Again, I can’t stress this enough, Eva. When you go into this place, into this unit, if you look around you would most likely see that most other patients are on a ventilator?
Eva: No, actually. No.
Patrik: Okay.
Eva: They’re pretty good at getting that off pretty quick.
Patrik: Okay. That’s good. But where I’m going with this is really a lot of patients in ICU would be on a ventilator, right?
Eva: Yeah.
Patrik: And your husband is not, and that’s good.
Eva: Absolutely.
Patrik: If he was on a ventilator and he was on the Norepinephrine and he was on the dialysis machine and everything was failing, maybe the discussions need to be had, but that’s not the case.
Recommended:
Eva: Yeah. Okay. That makes total sense. Can I let you go and give you a call back later?
Patrik: Absolutely.
Eva: Okay. Thank you so much.
Patrik: You’re very welcome. All the best.
Eva: Talk later. Bye-bye.
Patrik: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!