Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Eva as part of my 1:1 consulting and advocacy service! Eva’s husband had a cardiac bypass surgery and stroke in the ICU but he is conscious and coherent and Eva is asking if the doctors are really giving up on him.
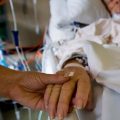
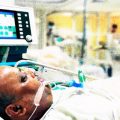
My Critically Ill Husband is On Dialysis and in the ICU Due to Septic Shock. Are They Really Letting Him Go Without my Consent to Withdrawal of Treatment?

“You can also check out previous 1:1 consulting and advocacy sessions with me and Eva here.”
Patrik: What? No. You see, that is very disappointing. Because, clearly, of course ICU at the moment has the overall decision making authority. However, this is clearly a cardiac problem. Right?
Eva: Yes. Okay. That’s a good question as well. We’ve moved out of short term emergency. Now we need to have someone come on board here, until such time as he can be discharged to cardiology.
Patrik: Very much so.
Eva: Which actually wasn’t the problem before? It should have been like the things that were taken care of last time. His heart was fine.
Patrik: Right.
Eva: Manageable.
Patrik: There needs to be a cardiologist. And if they’re not bringing in a cardiologist, and if they’re referring back to then making the decisions, well, maybe, I guess he’s an ICU patient at the moment. So let them make decisions. But still. Basically what they’re saying is they know it all.
Eva: Yes.
Patrik: Keep asking. Keep asking for a cardiologist. And see what they say.
Recommended:
Eva: It’s managing his heart is the issue to moving forward with the kidneys.
Patrik: Exactly. Exactly.
Eva: Okay. So as far as what I understand, is they are trying to do the pre load and after load, and get that balance upright.
Patrik: Of course. Of course they’re trying to manage that. Yeah, go on.
Eva: Yeah. And trying to sort out whether it’s distributive, the blood pressure issue, that it’s distributive or cardiogenic. Would that make sense?
Patrik: It does, it does. And most likely, it’s cardiogenic. Most likely with an ejection fraction of 20-30%. Most likely.
Eva: Yeah. How do they measure that?
Patrik: I can tell you how they measure it. They measure the ejection fraction in the ultrasound. Have you heard of a TOE? Have you heard of that?
Eva: No, no.
Patrik: Your husband, at one point or another, would have had a TOE, and a TOE stands for transesophageal echocardiogram. Basically, he would have had an ultrasound through his oesophagus at one point or another.
Eva: Oh. So while he was still intubated?
Patrik: Yeah, most likely. Most likely.
Eva: Okay.
Patrik: And that’s one way to measure ejection fraction, but another way is to measure it through an ultrasound, which is why I asked last night, are they doing ultrasounds? And as long as they do that, that’s a positive.
Eva: Yeah, and that’s where it kind of went from 20-24%. For the next number, I could say 20-30%.
Patrik: Mm-hmm (affirmative). When was the last?
Eva: One done? Probably Monday. Monday.
Patrik: Right. Right. Right. Okay. Okay. And when was the last time your husband was mobilised?
Eva: Actually mobilised?
Patrik: Mm-hmm (affirmative).
Recommended:
Eva: He hasn’t.
Patrik: At all?
Eva: He’s actually lying in bed. Yesterday was the first day that they actually had him sitting upright.
Patrik: Okay. Okay. On the dialysis?
Eva: Well, that’s the nurse last night. He spent a lot of the night sitting upright because he couldn’t sleep. So she was hoping that would tire him out enough to go to sleep. And she said well, if his blood pressure wasn’t low, I’d pick him up and put him in a wheelchair, because that would really work.
Patrik: Okay. Okay. Because I think if they can, just sitting him up on the edge of the bed would be really good. The more mobile the better.
Eva: Yeah. Yeah. Well, he would love that. He’s asking for it.
Patrik: Yeah.
Eva: So I will try and see if they have a cardio chair that they’d make into a cardio chair, so that’s what they’ve been using.
Patrik: Yeah, no, that’s great. That’s great.
Eva: Well, except, yesterday’s nurse did all that, and today’s has not.
Patrik: Right. Okay. Okay.
Eva: That’s where it’s so inconsistent. It really seems to be at the whim of the person who’s on that day.
Patrik: But it’s also important to keep looking for those positive messages like you had from-
Eva: Absolutely. Yeah.
Recommended:
Patrik: From our team. The other thing that’s important to understand, I mean, you know how sick your husband was, especially with ECMO, and the heart attack, and whatnot. At the same time, most patients in ICU, and you would have seen that one way or another. Especially if they are in a coma, and they’re ventilated or whatnot. Your husband is talking. That again is such a good sign.
Eva: Yeah. Yeah. Yeah. Not only coping, he told me his computer password.
Patrik: Right. Right. I don’t remember them.
Eva: So, that is such a positive. I can’t believe it. And because this team is new, they didn’t see him two weeks ago. Yes, he’s maybe weak, but he’s actually stronger than he was.
Patrik: What are they doing? How are they feeding him? Your husband has a nasal gastric tube?
Eva: He does, yeah.
Patrik: And they’re feeding him there?
Eva: Yeah.
Patrik: Okay.
Eva: So, if we had someone come in and sit him up, he’s on nectar fluids, which he has been for a while, because they haven’t made any progress towards moving towards anything else. Nothing seems to be moving.
Patrik: Okay.
Eva: If I wasn’t here, then I don’t know how this would get done at all.
Patrik: And that’s one of their main things, like in terms of them. And don’t misunderstand me, please. From their perspective, they can’t empty that bed quick enough.
Eva: Yeah. Sure. Yeah. Absolutely. Yeah. Our problem was last.
Patrik: That’s right. That’s right.
Eva: They intubated far too fast.
Recommended:
Patrik: That’s right. That’s right. And you need to keep looking for the positive signs. You will need to be repetitive in your demands to the point where they think you sound like a broken record, right?
Eva: Okay. I think they already do, but I can continue that.
Patrik: You will need to continue that, because they may sound like a broken record at some point, you know? But doesn’t matter. You have rights, and you would have seen from the email that there is evidence that you have rights. And you have every right to question everything that they’re doing.
Eva: So we now have a MAP of 73.
Patrik: Oh. That’s good.
Eva: Yeah, and I’m the only one here. He’s not being monitored at all. Yeah, so that is good. Certainly it’s having some effect at this level. Can I call you back later, after my meeting, and their rounds?
Patrik: Sure. Absolutely.
Eva: That would be great.
Patrik: Call me back.
Eva: Okay. Thank you. Can I just have you say one more thing to Frank?
Patrik: Yes.
Eva: Tell him to hang in there.
Patrik: Absolutely. Hi Frank, it’s Patrik again. Can you hear me?
Frank: Yes, I can.
Patrik: Okay, great. Great. So, Frank, you’ve been through a lot, from what I understand from your wife. And as I said, I have looked after, maybe, hundreds of patients in a similar situation than you are. You have pulled through against the odds, and that’s very positive. That’s very positive. Keep going. The other positive thing is, you’re not on a ventilator, you’re not in a coma, that’s all very positive. Especially with what you’ve been through, with ECMO and heart surgery and all of that. So at the moment, the main issue is your kidneys, from what I understand. Also, bit of an infection. But from what I understand that’s all sort of on the mend, and the next step, really, is to get you off that dialysis machine. And then slowly start to get you out of bed again.
Recommended:
But overall you are unwell at the moment, but there is no reason why you can’t get out of ICU alive. There’s absolutely no reason why not. Okay? So keep fighting and keep getting well.
Okay? Stay positive. Very important. It sounds like you are. You’re a fighter. If you managed to get rid of that tracheostomy within that short period of time, that’s a very good sign. That’s a very good sign. And setbacks like this, they do happen. It’s just a setback. You’ll just keep pulling through. That’s it. Don’t let their negativity bog you down. As long as you can hear me and as long as you can make your wishes known, that’s one of the most important things. Tell them what you want, tell them that you want to get out of ICU alive, and that’s all that matters for now. You can then take the next steps once you’re out of ICU. Take one day at the time, which I’m sure you have done. Take one day at the time, and keep improving.
Frank: I will.
Patrik: Okay? Eva, can you hear me?
Frank: Yeah.
Patrik: Right. That’s good, that’s good. Okay. Keep doing what you’re doing. You’re here with us, and keep fighting. The overwhelming majority of Intensive Care patients do survive. There’s no reason why you can’t. There’s no reason why you can’t either. And they do everything that they can at the moment, I have no concerns there. They’re just not telling you. They’re just being negative, that’s all. But I can assure you from what your wife has shared with me, they’re doing everything they can. Which is important to know. Okay? All right. I’ve got to go for now, but all the best for now. I’m sure we’ll talk again in the next couple of days.
Frank: Ok.
Patrik: Take care for now. Bye.
Eva: Patrik, how are you?
Patrik: And how are you?
Eva: Hi. I’m fine. I’m sorry about that.
Patrik: That’s okay.
Eva: Yeah, you get on the phone, and some comes in all the time.
Patrik: Right. That’s okay. Look, I had a look at your email, and so you’re wondering why this conflicting information. And I’ll tell you what it is. So it’s so important in a situation like that to read between the lines. What do I mean by that? They’re trying to plant a seed in terms of positioning. This consultant is basically, again, giving you the doom and gloom, and it’s all negative, and your husband has two options. And then respiratory therapy is coming in and saying, “Well, he’s breathing is actually pretty good,” and so forth.
So in ICU, generally speaking, nobody is telling patients or families, “Look, we can definitely help you. We can definitely get you out of Intensive Care alive.” It’s very rare. It’s very rarely what they tell you. Okay?
Eva: Right. Because they don’t want to make any kind of prediction, guarantees.
Patrik: Correct. And if they do make any predictions, it’s usually on the negative side to keep your hopes low. Right?
Eva: Yes.
Patrik: And also when it then comes to end of life potentially, it’s easier for them to tell you about end of life if they kept your hopes low from the beginning.
Eva: True. Yeah.
Patrik: Right?
Recommended:
Eva: And if all goes well, then they’re the heroes.
Patrik: Very much so. For them, it’s all about managing probably and reducing the risk of litigation.
Eva: Right. But we don’t really have that here the same way.
Patrik: Sure, the same way they have it in the US or in other countries. But still you could-
Eva: No, we don’t.
Patrik: Right. But still you could, if they told you, “Oh, look, Eva, we’re definitely going to get Frank out of ICU alive,” and then they don’t, you could argue a case. And they put themselves in a position where they don’t, they would never want you to argue that case in the first place.
Eva: Right.
Patrik: Right? With your husband’s chest, from the email what I had, they’re removing 120 ml an hour from the dialysis, right?
Eva: Right.
Recommended:
Patrik: If you calculate that over 24 hours-
Eva: Oh. Okay. Excuse me. Can I just give you a call back? They’re just about to do rounds.
Patrik: Of course. Okay. Thank you.
Eva: Thank you so much.
Patrik: Bye.
Eva: Okay. Bye-bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!