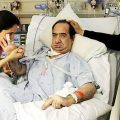
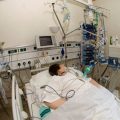
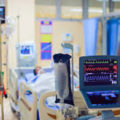
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Where Do We Start in Weaning my Sister Off the Tracheostomy & Ventilator in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Joyce, as part of my 1:1 consulting and advocacy service! Joyce’s sister is still with a tracheostomy, on a ventilator, and has developed grade 4 pressure sores. Joyce asks how the ICU team can improve the arterial blood gas (ABG) of her sister so she can possibly come off the ventilator.
How Can the ICU Team Improve the Arterial Blood Gas (ABG) of My Sister so She Can Possibly Come off the Ventilator?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Joyce here.”
Brent: Listen she’s exhausted, she’s never been this tired like I’ve seen her today.
Joyce: Well she went to the CT, she had like, you know.
Patrik: Okay.
Joyce: I don’t want her back on the-
Patrik: I know you don’t, but it’s a bit like if you’re training for a marathon, if you don’t rest a day, you can’t get your strength back.
Joyce: I feel like shouldn’t they advocate … I just don’t want to advocate … I don’t know, it’s like I just … I’m scared she’s going to get stuck there again.
Patrik: Oh for sure, but you don’t want to go to sub-acute, for sure, you definitely don’t.
Joyce: But Patrik that’s the problem, the problem is I don’t want to, but from what it seems like, I don’t know what the options are. If the sub-acute tells me, “Oh yeah, we could take care of the wound,” should I not trust them that they can take care of the wound?
Patrik: I wouldn’t … the wound would probably be not so much my concern, my concern is even though they’re advertising to be the specialist on trach and ventilation, they’re not.
Joyce: That’s why I wanted to get her off the ventilator, and that was one step closer. You know what I’m saying? You bought myself time.
Patrik: Yeah. No for sure. Look I hear you loud and clearly, but get her back … if she goes back on a ventilator for a night to give her a rest, and then she could do another five days, another week, that’s a win.
Joyce: You’re saying do that instead of a setback coming in?
Patrik: Oh definitely.
RECOMMENDED:
Joyce: Like you’re saying there’s … the other scenario would be I’m going to not … let’s just say I’m going to let this ride, she’s going to get so tired that she can get to the point that..
Patrik: Crash.
Joyce: She’ll crash?
Patrik: Crash.
Joyce: Okay.
Patrik: But ask them for the-
Joyce: I’m not going to … but listen I’m also entrusting that the doctors are looking at everything and making-
Patrik: I would hope so. I’m not telling you that everything that I’m saying is 100% the right approach, but I’m just telling you what I’ve seen over the years.
Joyce: Okay, and then as far as this … I told them about the patch for … somebody told me about the patch for drying secretion, they absolutely said no way.
Patrik: Patch?
Joyce: Somebody said there’s a patch, there’s a sticker that goes behind your ear that can dry secretions, and they were like, “No.”
Patrik: Probably there is.
Joyce: And they’re saying there’s medicine that can dry your secretion but she doesn’t want to do that because she doesn’t want the secretion to like trap in the lungs.
Patrik: No definitely not. There is medication, glycopyrrolate.
Joyce: She doesn’t like it. The doctor said she doesn’t like it.
Patrik: Yeah, no I don’t like it either. For certain situations yes, but not in your sister’s situation. Definitely not.
Recommended:
Joyce: So am I far away from getting off the tracheostomy?
Patrik: I’d say at the moment yes, but I mean you’ve got to look at how far you’ve come.
Joyce: Right.
Patrik: You can’t look at how far away are you from removing the trach, you’ve got to look at how far has she come and what are the next steps.
Joyce: I just want to hear her voice, I want to give her the voice, but you’re saying that’s not coming near?
Patrik: So when they tried the speaking valve, who was trying? Was that a speech therapist?
Joyce: Respiratory was next to her and so was my brother, an hour ago.
Patrik: Okay I would argue that a speech therapist needs to-
Joyce: No but she desaturated so fast and the respiratory therapist was like freaking out and then she like desaturated so it didn’t happen more than two minutes.
Patrik: Okay. Okay.
Joyce: so where am I now? Like I feel..
Patrik: Yeah I’ll tell you … got to wait, find out what’s happening with that CO2, and ask them what the reasons are for that.
Joyce: For the 54?
Patrik: That’s right.
Joyce: And you’re going to send me that … that other machine you mentioned, what does it do?
Patrik: Yeah so let’s just say she’s going back on a ventilator overnight, okay? So that’ll give her some steady pressure overnight, a low pressure overnight. If she has the cough assist machine during the day, she will have a high onset of pressure for short periods.
Joyce: Okay, and that’s not a ventilator, it’s a different machine?
Patrik: No it is a ventilator, but it’s designed specifically for those short bursts.
Joyce: Because she was on a pressure mode, it’s called P Spontaneous, where she took a breath and they gave her extra breath or gave … is that what you’re talking about?
Patrik: No it’s … yes overnight, yes, that’s what I would be talking about for overnight. During the daytime, the cough assist, is short onset of high pressure, then a negative pressure, that makes her cough, which would clear out her secretions. Are they doing chest x-rays?
Joyce: Yes.
Patrik: Daily?
Joyce: And they’re saying it’s gotten a little better.
Patrik: Okay daily?
Joyce: Often. I don’t know if it’s daily, but it’s often. Like I think-
Patrik: Three times a week?
Joyce: For sure, probably. Most likely.
Patrik: Okay.
Joyce: Because she had a chest tube that they took out, they did it a lot and then-
Patrik: Oh yeah. Have you … do you have a recent chest x-ray report?
Joyce: Yes. Yes I do. I’ll give that to you right now. Hold on. It says liver … protein. Okay. I don’t know where it is. X-ray, we’ll see. I think there is. It said on the x-ray that she has … oh here it is. Here, I have one from the … oh so it happens every couple of days. Here it is.
Patrik: Yeah.
Joyce: Here I just sent it to you. Hold on, I’m going to text this to you right now. What’s App, Patrik. Okay just sent it to you.
Suggested links:
Patrik: Okay, just quickly, the BUN levels were high.
Joyce: Yeah I don’t know what that means either.
Patrik: Well are the kidneys working?
Joyce: Yeah.
Patrik: Okay, she’s not on dialysis?
Joyce: Nope.
Patrik: Okay. Just give me a second. Mild right infiltrate improved, interval removal of right chest tube. No appreciable pneumothorax.
Joyce: This was on the 3 days ago.
Patrik: Oh so last Saturday. Moderate left upper-
Joyce: I sent you one from the 13th too. I sent you like the previous one.
Patrik: Yeah. Aortic … okay that looks … so hand one, just let me go back to the previous one.
Joyce: Yeah they do it every couple of days, like I said..
Patrik: Yeah no that’s good. Okay there’s nothing in there that would hint why she would have a high CO2.
Joyce: So maybe … but then again, hold on, I’m going to look at blood gas. Give me a second, I’m going to look at blood gas, and then what I’m going to do is I’m going to look … okay here it is, there is a blood gas, one second, I’m going to look at your … okay, the PCO2 was 53.
Patrik: Yeah.
Joyce: Okay hold on, I’m just going to give you the … okay hold on, blood, so that was 53 on the four days ago. Okay. Why is it stuck? Blood gas. Okay hold on. Test results. So I have to monitor where that number went, right?
Patrik: Yes.
Joyce: Okay so I don’t … I think it was generally always high, I don’t think it’s ever been low. So can that be? I mean because remember we were looking at that number.
Patrik: Yeah look the CO2 is the significant number, maybe ask them, I would ask them. I would not be happy with that number, unless your sister had COPD or asthma.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Joyce: Which she doesn’t.
Patrik: Yeah exactly.
Joyce: And what does that actually mean? Can you explain to me what it actually means?
Patrik: Oh yeah, so when we exhale … when we breathe in, we breathe in oxygen, and when we exhale, when we breathe out, we exhale carbon dioxide, CO2, if we don’t exhale enough carbon dioxide, we get drowsy.
Joyce: Okay. Yeah Patrik her numbers have always been high, 58.
Patrik: Yeah but I wouldn’t be happy with that, because I’ll tell you something, you’re saying your sister is awake, or you know, I would argue that once her CO2 is within a normal level she’ll probably be even more awake.
Joyce: If it was at a normal level?
Patrik: Very much so.
Joyce: But like how do you explain … I mean okay, but even with the ventilator it was high, so it’s not … so what my argument is, is to put her on a ventilator, I don’t see the solution in that because..
Patrik: Depends on what she was on before, depends on what settings she was on before, and what settings she will be going back to. I would also … if I was you I would want to find out how much pain relief is she getting, is she getting any tranquilizers, because if she does, and if she’s been getting it for a period of time, she might have to be weaned off any tranquilizers and pain relief, because that might get her CO2 back to a normal level too.
Joyce: But you’re saying painkillers can be part of why the CO2 is high?
Patrik: Very much so. Opiates in particular.
Joyce: Because I’ll tell you, I just researched, from the day she came in, she came in at 58, and the lowest she’s ever been in 53, and that was full-on ventilation.
Patrik: Okay, find out why. I’m not … you know, if it’s …
Joyce: So I’m going to say to her I see the PCO2 … or see whatever it is, I see it’s high, what’s your plans of bringing it down?
Patrik: Very much so. Very much, and see what they say. I wouldn’t … you can see the normal range in the blood gas.
Joyce: Yeah it’s 43, 45, so my question is when she breathes on … this is an important component to get her off the trach and breathing normally, this is one number that is playing an important role of her breathing naturally, because I’m closer to get there, but if that number doesn’t go down, then … right? Like we’ve got to make sure that number goes down or the rest is not going to work.
Patrik: Because-
Joyce: If there’s no oil in the car it’s not going to work.
Patrik: Correct, and especially if the trach is being removed, you have limited ability to manage that. I would argue the cough assist or a bit of ventilation overnight will correct those numbers. Now, once the trach has been removed, you could do some CPAP with a mask, but now is the time to correct it.
Recommended:
Joyce: But my question is even on ventilator mode and full pressures and up and down she was always high.
Patrik: Yeah I hear you, that doesn’t make it right though. That doesn’t make it right.
Joyce: Right, but what I’m saying is I’m feeling even putting on the ventilator, I don’t know if it’s going to get better.
Patrik: I would argue it does, if they change some of the settings.
Joyce: So I’m just … okay, so I’m not … I’m going to basically address this issue and let them see what they say about it, and they have to address it because it’s a very important component in the pot?
Patrik: From my experience.
Joyce: So right now, what I’m going to focus on, because we can’t do everything, so what I’m taking from this conversation is I’m going to attack this particular issue from the blood gas and say, “How are we addressing it? How are we going to fix this? Because in order for her to breathe on her own and really be trach- dependent and take it out we need this number down, what is your solution for it?”
Patrik: Yeah.
Joyce: You gave me some, but I’m going to have them speak on it.
Patrik: Of course, absolutely, and they might say … they might have another reason for it, but I kind of doubt it, you know?
Joyce: I will keep you updated, and so that’s kind of where we are, and then we basically … the reason right now she’s with a humidifier still connected to the trach is because of the secretion.
Patrik: Very much so.
Joyce: I’m going to monitor the secretion, and obviously if that goes down then we’ll be able to cap her and hopefully hear her voice, right? That’s kind of what I’m monitoring and why the humidifier is there, so that’s fine, and then as far as the bed sores are concerned, the argument is really that’s the only thing that’s really keeping her in the hospital at the moment because that’s the only high level of care she really is getting, and I will argue the fact that she needs high level of care.
Joyce: And let me ask you a question, bringing her home, this high level of care, can it be monitored if somebody comes once every three days?
Patrik: Yes, if she has an ICU nurse 24 hours a day they can definitely communicate with a wound care specialist, yes. I would argue yes.
Joyce: But the only way it’s really going to happen is if there’s an ICU nurse for 24 hours. Question is, there’s no … you’re saying there’s no doubt about it that no matter what, there needs to be an ICU nurse with my sister 24/7?
Patrik: If she has a trach.
Joyce: If she has a trach.
Patrik: Yeah.
Joyce: And if she doesn’t have a trach then we could just get a nurse and that’s fine?
Patrik: There’s all sorts of opportunities for you if she doesn’t have a trach, it’ll be so much easier.
Joyce: And I’m going to buy time to try to get her off the trach at the hospital?
Patrik: Very much so. Very much so. Joyce I’ve only got a couple of more minutes left.
Joyce: Okay. Finish it up and tell me what else I need to advocate for.
Patrik: CO2, get the CO2 down, keep mobilizing, right? Does she do-
Joyce: And then are you happy with the two hour arrest chair for two hours a day?
Patrik: I would say longer. I would say longer.
Joyce: But the pressure sores are an issue, so they don’t want her there-
Patrik: Get them to sit your sister on a cushion, on a gel cushion.
Joyce: They are.
Patrik: They are?
Joyce: They are.
Patrik: So there’s no limitations.
Joyce: Push it more?
Patrik: Push it more.
Recommended:
Joyce: Push it more than two hours?
Patrik: Push it more that … two hours in the morning, two hours in the afternoon.
Joyce: They’re only doing it once a day.
Patrik: Not good enough. Morning, two hours, lunch break, get her to have a snooze, afternoon-
RECOMMENDED:
Joyce: I’m going to ask the doctor to put another order throughout the … for two times a day.
Patrik: Yeah definitely.
Joyce: Okay I got it. Oh I got a lot … okay Patrik I got a lot from this. We’re going to do this again. Thanks Patrik.
Patrik: Please. Thank you. Bye.
Joyce: Thanks, bye.
Patrik: All the best. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!