Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Francia, as part of my 1:1 consulting and advocacy service! Francia’s dad is with a tracheostomy and is on a ventilator in ICU. Francia is asking how she can dominate over the doctor’s decision to transfer her dad to LTAC.
How Can I Have Power Over the Doctor’s Decision to Transfer My Dad from ICU to LTAC?
Patrik: Hi, how can I help you?
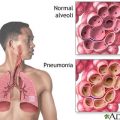
Francia: Yeah. Hello. My dad has been admitted in the hospital since end of last year. He has multiple sclerosis. He’s been bedridden. What happened was he developed pneumonia at home, so he got admitted to the hospital. He was on the ventilator overnight. They extubated him, and he got discharged to the second floor, and they had to give him morphine because he had nerve pain. And since then, they re-intubated him three times, then he ended up with a tracheostomy and PEG now. And he’s currently not in the ICU. He’s on the 2nd floor of this hospital but they want to discharge him to an LTAC or an SNF, a skilled nursing facility.
Patrik: Yeah.
Francia: Yeah.
Patrik: Okay. So when was the trach done?
Francia: It was done last year, around end of 2020.
RECOMMENDED:
Patrik: Okay. So around two and a half months. What stopped them from going to LTAC so far or from sending him to LTAC so far?
Francia: His insurer got him covered in the hospital, and we haven’t agreed to transfer him to an LTAC because we believe that at the current hospital, it’s better care than if he were to go to an LTAC.
Patrik: Yeah, I agree.
Francia: Okay.
Recommended:
Patrik: And so far, you basically asked them to keep him where he is, and that was successful so far.
Francia: Yes. The insurance said they’ll cover his stay at the hospital indefinitely for as long as it need to be, but the hospital wants to transfer him over.
Patrik: Right. They want the bed. Okay. What’s the progress for your dad? Is he having time off the ventilator?
Francia: He’s doing weaning on CPAP. He’s been doing eight hours a day, but he’s not doing great. He was doing 24-hour weaning trials a month ago.
Patrik: Yeah.
Francia: He got a procedure where they take mucus out of your chest and lungs. And after that procedure and a round of IV antibiotics, he hasn’t been doing great on CPAP, but he has been doing better the past week for more than eight hours, but he said it’s hard to breathe right now.
Suggested links:
Patrik: Right. I see. Excuse me. Your dad doesn’t have COVID, does he?
Francia: No.
Patrik: Okay, good.
Francia: No. He had rhinovirus. Originally, he had rhinovirus. That’s what he came in with. He just couldn’t cough up the mucus, I guess, because of the multiple sclerosis. He was just weakened too a little bit from, he was dieting for, I don’t know, it was a stupid decision, but he was weakened. Yeah.
Patrik: I see. And is he still breathing on CPAP or is he in a different ventilation mode at the moment?
Francia: He was on CPAP today. I believe they take him off of CPAP during the night because I think he hyperventilates after too long on it, but they’ve been trying to wean him on it every day on CPAP.
Patrik: Okay.
Francia: And also, an important point to make, he has intense sciatica nerve pain, so this whole time, he’s been on opiates that he’s been in the hospital.
Patrik: What is he getting? Do you know what opiates he’s getting?
Francia: Well, right now, he’s getting oxycodone, but in ICU, throughout the whole time, he was on fentanyl 200 micrograms, IV in ICU, on the ventilator. He was on oxycodone. He was on methadone.
Patrik: Oh my, goodness.
Recommended links:
Francia: He’s a little man. He’s 120 pounds, but he has intense sciatica pain. It doesn’t seem to help, even though they’re giving him the opiates. It doesn’t really help.
Patrik: No. When you’re saying he was on CPAP today, how many hours?
Francia: Today was about, I think, nine hours they had him on, and they put him back on the regular setting.
Patrik: Right. And what are the regular settings? Do you know?
Recommended:
Francia: It’s 40% concentration of oxygen.
Patrik: Yeah.
Francia: It was at 30 a few days ago. They put it up to 40. I don’t know why. I guess maybe to see if he could breathe better. And I don’t really know other than that, specific-
Patrik: It would be important to find out what settings he is on besides when he’s not on CPAP. When he’s on CPAP, have they ever managed to get him off the CPAP even? Was he breathing without the CPAP, without the ventilator at all?
Francia: Not since he got the trach, no.
Patrik: Okay.
Francia: When he was in ICU, when they extubated him the second time, he was on oxygen again, but then they had to re-intubate him.
Patrik: Right. Is your dad getting mobilized? Is he getting out of bed?
Francia: He was bedridden at home. He’s been bedridden for two years.
Patrik: I see.
Francia: That’s partly to do because of the sciatica pain because he didn’t want to get in the scooter because it hurts a lot, but-
Patrik: Yeah. I see. He couldn’t even sit in a recliner chair. That’s too uncomfortable, is it?
Francia: He could. He could at home. I believe they did try to get him in a chair while he was in ICU just to sit him up, but it’s very difficult.
Patrik: Difficult, okay.
Francia: And also, they’re not really moving him too much. I got to go in and do physical therapy with him. They’re not moving him too much at the hospital.
Patrik: Why do they not want to do physical therapy? Why not? Do you know?
Francia: They’re saying that since it’s an acute hospital, they want to transfer him over to the SNF to do that kind of stuff. I’ve been saying, “Why don’t you do physical therapy more often?
Patrik: Absolutely.
Francia: It’s a no-brainer.
Patrik: It is a no-brainer. Okay. How old is your dad?
Francia: He’s 70.
Patrik: That’s not very old.
Francia: No.
Patrik: That’s not very old.
Francia: And he’s in good spirits. He’s fully mentally aware. It’s just the physicality of it right now.
Patrik: That would have been my next question. How is he mentally? Is he not depressed?
Francia: No. Well, no though. I Face Time with his friends when I’m there. He’s smiling. He’s fully aware of what’s going on, but he can’t talk because of the trach. He’s a little hard of hearing. He has some wax buildup, but a little hard of hearing.
Recommended:
Patrik: Sure. Okay. Any other medical issues? Does he have heart issues, kidney issues, or liver issues?
Francia: No. He has thalassemia. He received about a dozen blood transfusions in the hospital.
Patrik: Right.
Francia: That’s been going … Now, I don’t know. At home, his blood tests were good. No other medications besides morphine. He was on 30 milligrams. He was going on 15 at home. No medications though. And yeah, he’s on, Jevity at the hospital too regarding her nutrition, the PEG. So I don’t know if that’s contributing to what’s going on with his hemoglobin and everything else, but he does have thalassemia. He was diagnosed with the minor.
RECOMMENDED:
Patrik: Can you say that again? What was he diagnosed with?
Francia: Thalassemia.
Patrik: Thalassemia. Oh, got it. Yeah, it is a blood disorder involving lower than normal amounts of an oxygen carrying protein. So he’s been getting red blood cells.
Francia: He’s been getting blood transfusions in the hospital. Before that, he never got one. His sister has it. His sister’s daughter has it. So it’s a genetic trait.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!