Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Can I Ensure the ICU Team Listens to My Requests and Provides the Best Care for my Mom?
You can check out last week’s question by clicking on the link here.
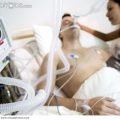
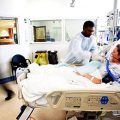
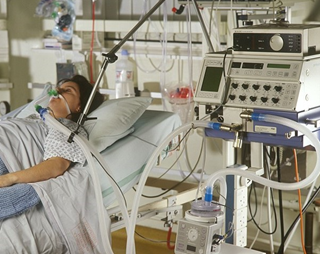
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients, Angie, as part of my 1:1 consulting and advocacy service! Angie’s mom is in the ICU with a tracheostomy and with low hemoglobin. She is asking if the low hemoglobin level impacts her mom’s ability to get off the ventilator.
Does Low Hemoglobin Affect my Mom’s Ability to Wean Off the Ventilator While She is in the ICU?
Patrik: And you generally speaking, can get them to open up. The advocacy, if you tell them, “Look, I’ve hired a professional advocate,” can be very threatening for them. And they might retreat, or they might not. I haven’t met these people, but I would suggest trying the friendly approach, because that seems to work better. We can still advocate. The most important thing is, that they start talking.
Angie: Correct.
Patrik: That is the most important thing, that they start talking. And often, you don’t get them to start talking when you say, “I’ve hired a professional advocate.” That, they shut down.
Angie: Got it. Got it. Yes. Yes. It’s a fairly big size of residents, the rounds, they’re attending.
Patrik: Mm-hmm.
Angie: So hopefully there’s a different opinion, it’s not just a reflection of what the attending wants that everybody else is going to push for. Okay.
Patrik: Who’s on those rounds? Who’s on those rounds?
Angie: It’s a teaching hospital.
Patrik: Yeah.
Angie: So most of them are critical care residents.
Patrik: Yep. Yep. Yep. Yep.
Angie: They’re surgery, doing critical care.
Patrik: Yep.
Angie: Learning critical care. I believe.
Patrik: Yeah. Yeah. Yeah. Yeah. And who’s calling the shots, though? Who’s the one, that’s making decisions?
RECOMMENDED:
Angie: He’s actually, believe it or not, he’s a… Usually, they’re surgeons, but this week it’s a pulmonologist. So previously, I’ve had better luck with the… I think one of them… Yeah, they were both surgeons.
Patrik: Right.
Angie: That had done critical care. But the actual pulmonologist, who you kind of hoped would be more open to helping, he just had his mind made up, the second he heard about my mom’s case.
Patrik: Yeah. Yeah. Yeah.
Angie: So I don’t see any flexibility in his stance.
Patrik: Okay, fair enough. Fair enough.
Angie: Yeah.
Patrik: That’s okay. That’s okay. So just remind me please again, Angie, when did she have the tracheostomy, and how long ago?
Angie: She had it on the previous Tuesday.
Patrik: Tuesday.
Angie: I believe it’s July 21st.
Patrik: Okay. Yeah. Yeah. It would have been a Tuesday. Okay. Okay. So those ventilation settings, assuming ABGs (Arterial Blood Gas) are okay, should allow your mom to have a trach collar, absolutely. Do you know how often she gets suctioned; do you know what I mean by that?
Angie: Yes. Today zero since I’ve been here.
Patrik: Wow. Wow.
Angie: And I’ve been here for, I’d say five hours. But yesterday was quite a lot.
Patrik: Okay.
Angie: Every hour to two.
Patrik: Okay.
Angie: So I don’t know if they’re neglecting, or they’re just decreasing.
Patrik: No. No. No. I wouldn’t say they’re neglecting, because especially if you are there if she needs suction, you will hear her tracheostomy rattling, and you would see her oxygen levels go down. You would see her becoming very, very uncomfortable.
Angie: I see. No. She’s standing at 99%, right now.
Patrik: Great. No, so that’s good. Do you know?
Angie: Yeah?
Suggested Links:
Patrik: Do you know whether she’s got an inner cannula, do you know what I mean by that?
Angie: No. I don’t know what you mean by that.
Patrik: That’s okay.
Angie: Is that the small tube, inside the trach?
Patrik: Yes. Correct. Correct. Yep. Correct.
Angie: Yep.
Patrik: She does have that?
Angie: I think she does have that. I remember one of the nurses-
Patrik: Cleaning it?
Angie: … replacing it.
Patrik: Yeah. Yeah. Yeah. Okay, that’s good. Because that’s important information, because if she does have an inner cannula, and they’re changing it regularly, and they’re not… It’s almost like a safety device. It’s almost like a safety valve, as long as they keep changing it, that’s good.
Coming back to, what you mentioned earlier she’s got fluids in the lungs (Pleural Effusion). Do you know more about that, can you tell me more about that?
Angie: Yes. Yes. Yes. I can pull up his radiology report. And what I read there, that’s what the attending would tell you. Let’s say the two of you have a conversation.
Patrik: Yeah.
Angie: That’s what she’s going to emphasize. Let me just get the latest. Luckily we see 99% of her medical record, in real-time. So that’s very helpful.
Patrik: Do you see her medical records online?
Angie: Yes.
Patrik: Oh, great.
Angie: Yes. We are very lucky.
Patrik: Great.
Angie: Very lucky. So today there are no chest X-ray results yet.
Patrik: Mm-hmm.
Angie: But this is from yesterday. So it says no significant variable change.
Patrik: Mm-hmm.
Angie: “Persistent pleural effusions, and vascular opacities.”
Patrik: Mm-hmm.
Angie: “Which can represent opacities or is pneumonia.”
Patrik: Mm-hmm.
Suggested Links:
Angie: That’s the top-line findings. Then in the lower section, it talks about perihilar vascular prominence, likely reflecting mild pulmonary edema.
Patrik: Yep.
Angie: “And left colorectal cardiac pulmonary opacity is unchanged.”
Patrik: Yep.
Angie: “Similar binocular and perihilar pulmonary opacities.”
Patrik: Mm-hmm.
Angie: “Unchanged moderate bilateral pleural effusions.”
Patrik: Yeah.
Angie: “No pneumothorax,” that’s it.
Patrik: The last one, you said no pneumothorax?
Angie: No pneumothorax. No pneumothorax.
Patrik: Yeah. Okay. Okay. Okay, then you mentioned earlier anemia, have you got a hemoglobin level?
Angie: Again, most of our tests, recede about a week ago, to try to push her out. So the data I have, I asked for it once, on the seventh. So that was three days ago.
Patrik: Mm-hmm.
Angie: There’s a CBC (Complete Blood Count). So her hemoglobin is 7.7. Her RBC (Red Blood Cells) is two point-
Patrik: One week ago?
Angie: It was three days ago.
Patrik: Three days ago?
Angie: Three days ago. Her RBC is 2.34. This is half, what you know what she has to have.
Patrik: Mm-hmm. Yeah. Yeah.
Angie: HPLC (High-Performance Liquid Chromatography) is 25.6.
Patrik: Yeah. Do you have a white cell count?
Angie: The white cells were 8.6.
Patrik: Okay. That’s good. That means there’s no sign of infection, really, is there?
Angie: Correct. Correct.
Patrik: That’s good.
Angie: Yeah.
Patrik: Okay.
Angie: But she does fluctuate. Like today she’s-
Patrik: Of course.
Angie: Yesterday she was more energetic, but today she seems tired.
Patrik: Yeah.
Angie: Maybe the physical therapy, took it out of her.
Patrik: Yep.
Angie: But she’s more drowsy. And her temperature is a little bit higher than her base. But still 37.4, I believe.
Patrik: Right. Right. Any idea why she’s anemic?
Angie: On admission, she was not. I don’t want to take time looking for it, but I believe her hemoglobin was 11, a month ago, so-
Patrik: Yep. Why-
Angie: So that was normal.
Patrik: Yep.
Angie: Why does it go down? Her RBC count was low.
Patrik: Yeah.
Angie: Lower in that range.
Patrik: Yeah. Yeah.
Angie: It was low. So I’m suspecting, based on her age, her bone marrow probably has something to do, with the production of red cells.
Patrik: Yeah.
Angie: But I’m not 100% positive-
Patrik: And they haven’t-
Angie: … there’s no diagnosis for that.
Patrik: There’s no diagnosis there?
Angie: Yeah.
Patrik: Okay. So here is… And with that low hemoglobin, in her hospital stay, has she had any blood transfusions?
Angie: When she was critically ill, on one night she went below seven. But she got one unit.
Patrik: Okay. Okay.
Angie: But that was approximately two weeks ago.
Suggested Links:
Patrik: Okay. So when someone has low hemoglobin, there are fewer red blood cells in the body, making it difficult for oxygen to go around the body. So I would argue that low hemoglobin is potentially a hindrance, to getting your mom off the ventilator.
Angie: Sure.
Patrik: I also argue that if she goes to LTAC (Long Term Acute Care), and her hemoglobin stays low and they’re not fixing it, it’s going to be a big issue going forward.
Angie: Sure.
Patrik: And in a hospital, in an ICU setting, it’s easy for them to give blood transfusion, when needed. In an LTAC setting, I’d argue it’s more difficult, they just don’t have that expertise.
Angie: Got it.
Patrik: Right.
Angie: Could it be because of the anticoagulation? She gets I think, Lovenox, 40 units, I believe. I don’t know if it’s that.
Patrik: Unlikely. The only way the Lovenox might impact that, is if the Lovenox for whatever reason would cause a bleed. But you haven’t mentioned anything about a bleed.
Angie: No. They have not looked for it. But I feel that maybe there’s a… Yeah, you’re right. Maybe there is a slow GI (Gastrointestinal) bleed, that they’re not looking for. But it’s just a guess.
Patrik: She’s getting nutrition, through the PEG (Percutaneous Endoscopic Gastrostomy)? Does she have a PEG?
Angie: Yes. Yes. Yes. She’s getting nutrition through the PEG.
Patrik: She’s absorbing feeds, she’s opening bowels?
Angie: Yes. Yes. I believe so.
Patrik: Mm-hmm. Okay. You should definitely think about GI (Gastrointestinal) bleeding. But I would hope that in the ICU, they’re checking that quite frequently, they’re aspirating every four hours from the PEG tube, to check that she is absorbing and that there are no bleeds. So I would have trust in them, that they’re doing that. Do you know?
Suggested Links:
Angie: Sure.
Patrik: There is often in ICU, in the critically ill, there is often a reduction in hemoglobin levels, for no reason that you can explain. Right?
Angie: Got it.
Patrik: It certainly is part of a critical illness. And it’s also often, if that is the case, if the anemia is an issue, it’s also often an obstacle to getting people off the ventilator, for the reasons that I mentioned before. Do you know?
Angie: Got it.
Patrik: There’s not enough red blood cells, which oxygen can attach to.
RECOMMENDED:
Angie: Sure. Sure.
Patrik: Right?
Angie: Sure.
Patrik: But nevertheless, that should not stop them from trying the trach collar.
Angie: You’re right.
Patrik: You know?
Angie: Right.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!