Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Can Mom’s Quality of Life Improve After Leaving the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients, Angie, as part of my 1:1 consulting and advocacy service! Angie’s mom is in ICU and she is trying to maintain a friendly relationship with the ICU Team to stay consistently informed of her mom’s care. She is asking how to get in control of the narratives so the ICU team will listen and provide the best care for her mom.
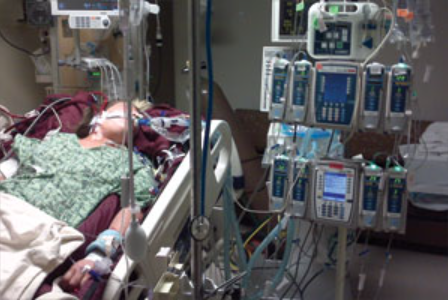
How Can I Ensure the ICU Team Listens to My Requests and Provides the Best Care for my Mom?
Patrik: Oh, yes. Hello.
Hi Angie, it’s Patrik here from Intensive Care Hotline. How are you?
Angie: Hi, Patrik. I’m okay.
Patrik: Are you-
Angie: I’m in the hospital with my mother.
Patrik: I’m a little bit earlier, is that okay with you?
Angie: Oh, no problem. No problem. I have some questions.
Patrik: Please?
Angie: So how much… I don’t know, just it’s quite one hour, do you want to talk for half an hour? Or-
Patrik: Whatever you need. We can do 20 minutes, we can do 30 minutes, we can do an hour. You are guided by you.
Angie: Good.
Patrik: I’m guided by you.
RECOMMENDED:
Angie: Thank you. Thank you, a lot. So let me pull up my questions, quickly.
Patrik: Yep.
Angie: Sorry. So, Patrik, I’ve read some of the free stuff you have, the guidelines?
Patrik: Yeah. Yeah. Yeah. Yeah.
Angie: So, I think my behavior has been very similar to what you recommended, since we’ve been at this hospital.
Patrik: Yeah.
Angie: The instant impact report.
Patrik: Yeah.
Angie: So, I’ve been following your guidelines, asking questions.
Patrik: Yeah.
Angie: And I’ve been able to get past that crisis, that they were requesting end of care. I was able to get… She had two extubations.
Patrik: Yeah.
Angie: So, she had the initial one, and then she had two chances, and so I was able to get her one extra try.
Patrik: Mm-hmm.
Angie: So I’ve been trying to engage with them, as friends or equals.
Patrik: Yeah.
Angie: I’ve had some success, it kind of varies, depending on who’s the boss that day.
Patrik: Right.
Angie: So, it’s someone that’s flexible. And I thought maybe I should give you a very brief summary, expand on what I told you yesterday. It should take about a minute.
Patrik: Please.
Angie: So today, right now, she has no daily blood labs, no ABGs (arterial blood gases).
Patrik: Right.
Angie: But only the ICU protocol, for glucose monitoring.
Patrik: Mm-hmm.
Angie: She has PT/OT (physical therapy/occupation therapy) twice per week. And being pushed towards the LTAC discharge.
Patrik: Mm-hmm.
Angie: And there’s no try for a trach collar or changing the pressure support variables she’s on.
Patrik: Do you know the-
Angie: We also don’t have any CAT scans. There’s been only one, during… Today’s the 30th day of her hospital stay.
Patrik: Mm-hmm.
Angie: But there’s daily chest X-rays, and her big issues are various forms of fluids in her lungs, and anemia.
Patrik: Right.
Angie: So that’s how far my knowledge allows.
Patrik: Mm-hmm. Yep. Yep. Yeah. Yeah.
Angie: If you have any questions?
Patrik: Yes, I do. I do.
Angie: There you go.
Suggested links:
- Not knowing what to do & how to get the ICU team understand my mom would improve if she’s extubated!
Patrik: No. I do. One of the things you mentioned is, did you say she’s got PCO-2, twice a week? Is that what you said?
Angie: Physiotherapy.
Patrik: Oh, physio? Physio?
Angie: Physio. Yeah.
Patrik: Okay. Physio? Yeah. Okay.
Angie: Yeah. Yeah.
Patrik: Got that. I misunderstood that.
Angie: She’s able to sit. One time she was standing using the device called a Steady so she could stand one time.
Patrik: Mm-hmm.
Angie: And then today, she sat for 2 hours.
Patrik: Oh, good.
Angie: Yeah.
Patrik: When you say she sat for two hours, in a chair?
Angie: Yes. In a chair, the brand is called Broda, I believe.
Patrik: Okay. Okay.
Angie: It’s a medical chair.
Patrik: Right. Yeah.
Angie: And she communicates here, she communicates by writing, and lip-reading, with me and other family members.
Patrik: Yep. Okay. A couple of questions there. So, she was sitting up for two hours. Was she tolerating that well?
Angie: Yes. She’s on 35% FiO2. Her pressure support, she’s on a Dr?ger.
Patrik: Yeah.
Angie: … it’s five and eight, so I believe that’s 35% FiO2 (fraction of inspired oxygen).
Patrik: Oh, that’s low. Five and eight? That’s low. That’s low.
Angie: Yeah.
Patrik: So that would have been my next question. What are the ventilator settings, so you’re saying five over eight, on a 35% FiO2. Do you know any arterial blood gas results? Do you know what I mean by that?
Angie: Yes. Yes. They do ABGs, but they stopped. So, the whole… I know basically they have a duty of care.
Patrik: Yes.
Angie: To do what’s right for the patient.
Patrik: Yes, correct.
Angie: But I think we are dealing with the business side.
Patrik: Yep.
Angie: Where they want to push her out, to free the bed.
Patrik: Yeah. Yeah.
Angie: So, they stopped doing that, on the seventh.
Patrik: Right.
Angie: So, three days ago, was the last one. I can find you those numbers.
Patrik: That would be good.
Angie: But she was compensated.
Patrik: Okay. Okay. That would be great. An ABG would be great. But irrespective of the ABG, Angie, your mom is on very low ventilator settings. I would argue they need…
Angie: Okay.
Patrik: Unless the ABGs are really, really poor, which I doubt, they need to start the trach collar. Even if it’s only for five minutes to begin with.
Angie: Got it. Got it.
Patrik: Right?
Angie: Got it. Got it.
Patrik: And they’re saying they’re not a weaning facility, and I disagree with that. Because what if she manages to stay off the ventilator, even for five, 10 minutes? Maybe the next day she can do an hour, and maybe the next day she can do two hours, and so on.
Angie: Correct. Correct.
Patrik: That’s how you start, you start by getting started with five minutes. And if a patient tolerates five minutes, you increase that to 10 minutes. And if they tolerate 10 minutes, you do 20. You know?
Angie: Got it. Got it.
Patrik: It’s simple.
Angie: Got it. We asked for that-
Patrik: Yeah. Yeah.
Suggested links:
Angie: … last Saturday. So about six days ago we asked for that, and our respiratory technician was favorable, he took it to the team, he got vetoed, or he got shot down.
Patrik: Yeah. Knocked back?
Angie: Yeah. He got knocked back. I’ve been asking for that every day. So, I think it’s more of a political thing. And the current attending, because I’ve stood up to him, he’s not-
Patrik: Right.
Angie: Basically, whatever I request, he tries to block. So that brings me to the other point, where you mentioned you can negotiate on our behalf?
Patrik: Yeah.
Angie: I wonder, how can I get them to listen to you, perhaps get them to talk?
Patrik: Okay. So… Okay, there’s… Yeah. So, a couple of things there Angie, a couple of things there. How do you get updates?
Angie: I attend the rounds, in the mornings.
Patrik: Mm-hmm. Okay. Great. Great.
Angie: And I listen in to their evaluations and medical jargon.
Patrik: Yeah.
Angie: And usually I can follow.
Patrik: Great.
Angie: But the point… I mean, depending on an attending, sometimes I can jump in. But this one says, “No, you’re not allowed to…” He said, “Oh, we don’t have time.” So, he’s basically a little bit, what I just told you, already.
Patrik: Yeah. Yeah. Okay. Okay.
Angie: Yeah. So, there’s no open discussions, because there’s probably varying opinions, within the team too.
Patrik: Oh, probably. Probably.
Angie: One of the fellows was more favorable to our case.
Patrik: Yeah.
Angie: And more supportive. But sometimes when I asked a question, he would back me up. And said, “Yeah, you’re right. That’s a good question. Why don’t we do that?” But dealing with a personality, that they basically for whatever reason, doesn’t want the family to ask the proper questions, or change whatever their idea of treatment is.
Patrik: Okay. I tell you, there’s two approaches in how they will listen. There are two approaches to that. One approach is when you’re there, get me on the phone. And you can do two things. And that is up to you. You can introduce me as a family friend. And you can say, “Oh, I’ve got Patrik here. He’s a family friend, he’s got a critical care nursing background. He’s just trying to help me make decisions for Mom.” That’s one way to approach it. That’s the friendly approach, sort of nonthreatening for them.
Angie: Got it.
Patrik: Or the more sort of… I wouldn’t say hostile, but the more forceful approach might be to say, “Hey. Look, I’ve engaged a professional advocate that’s helping me to advocate for Mom.” You could do that too. I’ll tell you what I’ve found with both approaches. The one where you say, “Oh, I’ve got a family friend on the phone,” is a nonthreatening approach for them.
Angie: Right.
RECOMMENDED:
Patrik: And you generally speaking, can get them to open up. The advocacy, if you tell them, “Look, I’ve hired a professional advocate,” can be very threatening for them. And they might retreat, or they might not. I haven’t met these people, but I would suggest trying the friendly approach, because that seems to work better. We can still advocate. The most important thing is, that they start talking.
Angie: Correct.
Patrik: That is the most important thing, that they start talking. And often, you don’t get them to start talking when you say, “I’ve hired a professional advocate.” That, they shut down.
Angie: Got it. Got it. Yes. Yes. It’s a fairly big size of residents, the rounds, they’re attending.
Patrik: Mm-hmm.
Angie: So hopefully there’s a different opinion, it’s not just a reflection of what the attending wants that everybody else is going to push for. Okay.
Patrik: Who’s on those rounds? Who’s on those rounds?
Angie: It’s a teaching hospital.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!