Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Loved ones in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Why Should I Not Trust the Intensive Care Team Blindly Whilst My Dad is Critically Ill in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions that we get quite frequently as part of my 1:1 consulting and advocacy service!
Why is My Loved One Prone to Develop Depression after a Long Stay in the ICU?
Patients who are treated in an intensive care unit (ICU) and survive are at increased risk of depression, a new study suggests. And depression in ICU survivors was linked with a higher risk of death in the next two years, researchers found.
What is Depression?
Depression is a medical and psychological illness that is characterized by prolonged feelings of sadness and disinterest as well as an array of physical symptoms including fatigue and problems with sleep.
Depression has many manifestations – in some cases individuals suffer from “Major Depression” which is severe and debilitating. In other cases, symptoms of depression are minor and brief in duration.
Critical illness is often a life-changing experience and depression may be understood as a natural development in response to the turmoil and upheaval that ICU survivors encounter.
Depression is one of the important causes of illness and disability in adolescents and adults. In the past few years, an increasing number of survivors have been discharged from intensive care units (ICUs). Patients recovering from critical illness, physical dysfunction, and organ failure may experience psychological and cognitive dysfunction after discharge, which is called post-intensive care syndrome. A previous study showed that depressive symptoms are common in patients discharged from the ICU and have a negative impact on quality of life.
What is the environment in the ICU that leads my loved one to have depression?
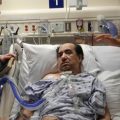
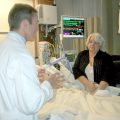
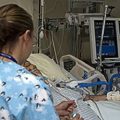
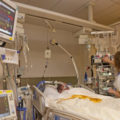
ICUs are psychologically challenging environments; patients in the ICU may be frightened by high-pitched alarms that beep sporadically; if patients have endotracheal tubes, then they cannot communicate with people, and many patients have intravascular lines in their arm or leg, Foley catheters in their urethra and physical restraints. These experiences make patients suffer a loss of dignity; they may feel helpless, sad, powerless, punished, embarrassed, and violated, and these feelings could trigger depression after their discharge from the ICU.
Recommended:
Who is at most risk to develop depression after ICU stay?
In some cases, resilient individuals rebound from critical illness and experience few if any persistent mental health problems. Individuals exposed to similar traumatic stressors often have very different reactions and, in most cases, do not go on to develop depression. However, some people are more susceptible than others to developing depression after critical illness. Individuals at greatest risk may include those who:
- Have pre-existing mental health problems
- Have a history of exposure to previous traumas of different kinds
- Are young in age
- Are female
- Experience prolonged delirium
- Have vivid memories of delusions and hallucinations during critical illness
Psychological symptoms occurring before an ICU stay and psychological distress experienced during the ICU stay or hospitalization were risk factors most associated with depressive symptoms after hospital discharge, the review found.
Psychological symptoms that existed before ICU stay were strongly associated with depressive symptoms after ICU discharge, as was the presence of psychological distress symptoms experienced in the ICU or hospital, including anger, nervousness and acute stress symptoms, such as emotional detachment or flashbacks.
What are the diagnoses related to depression after ICU discharge?
One study found that the common diagnoses among patients with depression were cerebrovascular disease, included intracerebral hemorrhage, subarachnoid, subdural, and extradural hemorrhage, occlusion of cerebral arteries, and chronic ischemic heart disease.
It has also been found in study that the most important diagnoses related to depression after ICU discharge were intracerebral, subarachnoid, subdural, and extradural hemorrhage. Brain damage has a substantial impact on depression after patient discharge. This is consistent with the findings of previous studies. Brain injury may result in long-term disability of physical, cognitive, and psychosocial functioning. Patients also experience difficulty remaining employed in the same occupation, having and maintaining social relationships, and fulfilling their true social function. In addition to cognitive sequelae and psychiatric problems, anxiety disorders combined with alcohol use disorders may contribute to depression.
Suggested links:
Can anything be done for Depression?
Depression may respond to a variety of treatments, while sometime improving on its own. Popular treatments for depression may include:
- Medication management – done either by a primary care physician or a psychiatric specialist
- Cognitive therapy or cognitive-behavioral therapy, which helps people recognize distorted and maladaptive thinking patterns
- A combination of medication and psychotherapy, which many experts recognize as the best and most effective course of action.
- While some forms of depression are resistant to treatment and may require very specialized interventions like Electroconvulsive Therapy (ECT), the treatment outlook for individuals with mild forms of depression (most common after critical illness) is hopeful and promising.
It is important to detect and recognize depression because it may lead to poor quality of life following ICU discharge; furthermore, depression is potentially treatable and preventable. Depression is related to a poor quality of life after a critical illness, and a previous study also showed that depression increases mortality.
Recommended:
With our service at Intensive Care at Home, it is a genuine alternative to a long-term stay in intensive care. We’re basically setting up a mini ICU at home with all the equipment, with all the monitoring but more importantly, with all the staff that you or your loved one needs and we’re bringing the intensive care and the intensive care expertise into someone’s home where we provide quality of life/quality of end-of-life at home for mainly long-term ventilated patients with a tracheostomy.
Your loved one may develop depression in the ICU because simply they are not having any quality of life. They’re stuck in an ICU room or ICU bed space, often with no natural daylight and with no natural day and night rhythm because often the lights are on and off all day and all night in ICU. And also because there’s people everywhere. It’s loud and it’s noisy. It’s very difficult to get in a normal day and night rhythm. Unlike at Intensive Care at Home where your loved one can have a routine that is conducive to your loved one’s wishes and situation and not dependent on the ICU schedules and potentially prevent the risk of your loved one going into depression.
You can visit our website at intensivecareathome.com for more information.
REFERENCES:
- Depression
https://www.icudelirium.org/patients-and-families/depression
- ICU Stay Can Lead to Depression
https://www.psychcongress.com/news/icu-stay-can-lead-depression
- The association between depression and length of stay in the intensive care unit
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7306368/
- Study Finds 1 in 3 Former ICU Patients Shows Symptoms of Depression
- Antidepressant Use and Depressive Symptoms in Intensive Care Unit (ICU) Survivors
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6448143/
- Depression Common After Time Spent in ICU
https://www.webmd.com/depression/news/20160817/depression-common-after-time-spent-in-icu
- Image credit to:
https://www.icudelirium.org/patients-and-families/depression
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!