Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” in last week’s episode I answered another question from our readers and the question was
Will Mom Get the Best Quality of Life by Having 24/7 ICU Nurses at Home?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients, Emma, as part of my 1:1 consulting and advocacy service! Emma’s mom is with ongoing dialysis in ICU and Emma is asking why is it crucial to have access to their mom’s medical records while she’s in ICU on dialysis.
Why is it Crucial to Have Access to Our Mom’s Medical Records While She’s in ICU on Dialysis?
Emma: Hi Patrik!
Patrik: Hi Emma! How are you?
Julius: Hi Patrik!
Patrik: Hi Julius!
Emma: Okay. My name is Emma. I found your website, by the way. I found it really excellent. Excellent! I thought it was just very unique. Haven’t seen anything like that. One of a kind, kind of things. I’m not really sure what to say. We wanted to make sure that we were doing everything and we weren’t really getting communicated with, and we just wanted to make sure everything was being done that could be done. And we don’t know medications or what else can be done, or if there is anything else that can be done. We were just feeling out of the loop basically.
RECOMMENDED:
Patrik: Julius, since we spoke yesterday, have there been any changes?
Julius: Yes. She was on the kidney dialysis, just trying to do the two-hour dialysis. Let’s see, yesterday after we left, so it was probably after her three o’clock flip from her stomach to her back, her lung collapsed. So, there was a tube that they had to put in and then also they tried-
Patrik: A tube? What kind of-
Emma: Yeah. I think it reinflate; I believe.
Julius: Yeah. I think they reinflated; I think.
Ron: To get air in her lungs.
Patrik: Air in her lung?
Julius: Air in lung. Mm-hmm.
Patrik: So, they put a tube. Oh, like a pneumothorax?
Julius: Yes. Yes.
Patrik: Right. Okay. Right. Okay, so they put a chest tube in?
Julius: Yep.
Patrik: Okay.
Julius: Then at that point, I think, I don’t know when they tried to do the kidney dialysis part, that two hours, it was all supposed to happen during that time, and they just couldn’t get anywhere because her blood pressure drops when they try to do that. So, this morning I had a call at 6:30 that they had to go with the full dialysis, the CRRT (continuous renal replacement therapy) I think it is.
Patrik: CRRT. Yep. Yeah.
Julius: And she’s actually responding. They had her on her stomach, just flipped her to her back again, or side, however that is, that posturing that they’re doing at about 2 … What about 12 o’clock today?
Ron: Yeah, was about then.
Julius: About 12 o’clock today. And they said that that actually went better. I don’t think they expected good results with that, but it actually worked better than they thought. And she’s stable now, but it’s literally hour by hour, kind of.
Patrik: Okay.
Julius: Yeah.
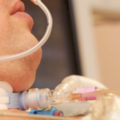
Patrik: Yesterday, Julius, she was on a hundred percent of oxygen?
Julius: Yes.
Patrik: Is she still on a hundred percent oxygen?
Julius: As of just about a half hour ago they were saying yes. They got to manage everything. Fortunately, I said, “Can you kind of give me a little bit more?” Basically, they’re doing everything at a hundred percent at this exact moment.
Emma: What was that 80 number though? Was it-
Julius: They gave me an 80 number. And this is-
Emma: We’re not sure what it is. We thought it may have been a little better for the oxygen, but it could be something different.
Julius: I think they wanted it at 90, but 80 is acceptable, I think she said. And I’m-
Patrik: Could be from an arterial blood gas. Have you heard of that?
Julius: Yes, that’s it.
Emma: Thing about gas.
Julius: Thank do.
Emma: Yeah. Okay. All right.
Patrik: Right. Okay.
Emma: We just don’t know.
Patrik: Yeah. That’s okay.
Julius: What did you call it? blood gas?
Patrik: Yeah.
Recommended:
- Quick tip for families in ICU: Should I get access to my critically ill loved one’s medical records?
Julius: So that’s what they’re really monitoring, it sounded like, this afternoon. Well, they’re monitoring everything, but …
Patrik: Okay. So, with the arterial blood gas, they’re saying there’s a number 80, is that right?
Julius: Mm-hmm.
Patrik: Okay. Well, if that’s her oxygen level in the blood, which I hope it is, that’s not too bad. That’s not too bad at all. However, room air, the air that you and I are breathing, is 21% oxygen. She’s on a hundred percent oxygen.
Emma: Oh, yeah.
Julius: Okay.
Patrik: Right. So, if you or I had a blood gas, our oxygen level in the blood would probably be 80 as well.
Emma: But without a ventilator.
Patrik: Without a ventilator and on 21% oxygen room air and she’s got a hundred percent of oxygen via a ventilator. So that’s just to put it in perspective. I can’t see any other number that they would be talking about.
Julius: You are spot on. Spot on. Because I just heard her, so that makes sense to me.
Patrik: Right.
Julius: It’s just they throw all this, and I just have a hard time-
Patrik: Piecing the puzzle together. I get it.
Julius: Yeah. Yes.
Patrik: Okay. Do you remember yesterday I was suggesting to you, you may want to ask them about other therapy options, such as nitric oxide or epoprostenol? Have you-
Julius: Yeah. I have not been able to do that because we got there and they were doing the whole flipping and it was kind of freaking me out a little bit. I think I wanted to-
Patrik: I would see that as a kind of urgent intervention.
Julius: Okay. I did pull up an article on that a little bit too.
Patrik: Some people in the ICU community might say that nitric oxide is outdated and I neither agree nor disagree. What I do know is that in ARDS (acute respiratory distress syndrome), it’s been used in some ICUs … since I’ve worked in the environment, which is over 20 years, it’s been a little bit out of fashion probably just before COVID, mainly because of the cost. It’s ridiculously expensive. But I’ve seen it said-
Julius: That’s okay.
Patrik: That’s okay. Exactly. I’ve seen it-
Julius: Have good insurance. My mom’s got good-
Emma: Yeah, we got good insurance. We don’t care about the price.
Patrik: It really isn’t. No, no, I agree with you. That it’s outdated just because of a perception, I believe, rather than actual results. There would be some patients that their lives have been saved by the use of nitric oxide. Others, it didn’t work. But it sounds to me like they’re, to a degree, clutching at straws. And they should use whatever is at their disposal, really.
Emma: Absolutely.
Julius: Exactly. The only attention I had today was with the nurse and they were all in the middle of … they basically wanted us gone from there.
Emma: Yes. Yes. They made it very, very clear that they wanted us up.
Julius: So, I had no real … But now though, I would be able to, because we’re going to head over there right after this call, head back to the hospital.
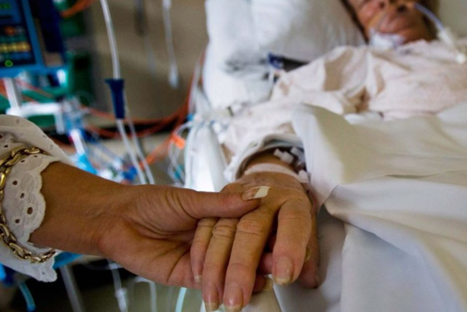
Patrik: Right, right. Okay. Look, and then also what would be helpful I think, just take a couple of pictures if you can, of the ventilator, the monitor, if you can. There would be some infusion pumps, if you can take a couple of pictures there.
Julius: No. Yeah, we understand. Right? I wanted to do that today.
Emma: Well, she’s been doing it.
Julius: I’ve been doing this. Yes.
Julius: Yeah. I always take a picture of my mother and under the bed. I’m sure that that’s not a Snapchat thing, that they kind of get the idea.
Patrik: Have you got access to the medical records already?
Julius: Oh, my God. That’s a whole another-
Emma: Oh, boy.
Julius: That’s the first thing we started with this morning, actually. That was our main goal. I think I might have said that to you. Now, there is a form, they … it’s like the only way they’ll do it is if we have a medical professional fill out the form for what they’re needing, the medical. Because, while it’s open, while it’s like open and she’s not home or out of the hospital-
Patrik: Let me ask you this. Is one of you the power of attorney for your mom?
Julius: All three of us.
Patrik: All three of-
Emma: All three of us.
Patrik: In all my time doing this, we’ve never had a client that could not get access to medical records, assuming they are power of attorney.
Julius: Yup. And that’s what I gave them, the medical records.
Patrik: Right. But they’re doing what every other hospital is doing. Hospitals are amazing at pretending they’re operating in a vacuum. They’re amazing at pretending that. Right? I mean, they can’t just withhold medical records from you, especially since you’ve got paperwork about power of attorney. So, they’re just trying-
Emma: Can I tell you what they told us about the medical records? She said, “Well, her chart isn’t done yet, so we can’t release those records.”
Patrik: Well, it’s 2022. You know what medical records should be like? They should send you a link to a URL with a username and a password. That’s what it is.
RECOMMENDED:
Emma: Okay.
Ron: She said, “You have to wait until she’s out of the hospital to get it.”
Emma: Yeah.
Patrik: What I’ll do is … I don’t have it right in front of me now, but I’ll send you the … I mean, there’s rules, laws in any state all around the world really, that it’s a right. It’s not a privilege, it’s a right to have access to the medical records. I will send you some stuff there that you can more or less present it to them. What I would do next if I was you, I would just tell them that it’s your right and that you want access to the medical records tomorrow by three o’clock. Just work with a deadline, so they’re aware of your rights. And the other thing-
Julius: And that’s okay, because you know what I’ll call right now? I will call the patient right area, that I’ve been … That’s the only way I have ever gotten any results. And even to get the doctors to talk to us.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!