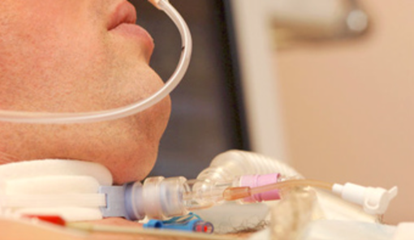
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Do We Know If Our Dad is Ready to Come off the Ventilator in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Joy, as part of my 1:1 consulting and advocacy. Joy’s dad is with tracheostomy and is getting worse in the pulmonary ward, and she is asking why they don’t want to bring him back to ICU.
My Dad is with Tracheostomy and is Getting Worse in the Pulmonary Ward. Why Don’t They Want to Bring Him Back to ICU? Help!
“You can also check out previous 1:1 consulting and advocacy sessions with me and Joy here.”
Patrik: Hi Joy! How are you?
Joy: Hi Patrik!
Patrik: There has been a fair bit happening with your dad?
Joy: Yeah, they took him off the ventilator, but now he really needs, we don’t know.
RECOMMENDED:
Patrik: Yeah.
Joy: His CO2 (carbon dioxide) levels are going back up and previously it was that they said that the ventilator would help with the CO2 levels and so we were looking to put him back on the ventilator. But I don’t know. I know you had mentioned that there may be some other things they could do in between a BiPAP and a ventilator.
Patrik: Very much so.
Joy: Without having to go that extreme. And so, I think we’re just sort of in a loss. We don’t know what the options are because they’re of course limiting our options so that they can limit what we do.
Patrik: Right.
Joy: Yeah.
Patrik: I’m just looking through your records from last time. So, he was off the ventilator at times and then back on the ventilator at times.
Joy: So, they took him, right. They started weaning him in the ICU and then they put the trach collar on him, and he was able to breathe on his own shortly, I think, after you and I and Rey talked.
Patrik: Yes, yes.
Joy: And so, we told them that we were not going to move him until he was off the ventilator. So, we kind of feel like that they hurry him off the ventilator just so we can move him.
Patrik: I see, I see.
Joy: And so now they’re acting like, oh, he can now go to the LTAC (long-term acute care) because he’s off the ventilator. And we’re not going to put him back on the ventilator. And the only place they can put him on that ventilator is in the ICU and they’re acting like they don’t want to put him back down in the ICU. They have moved him to a regular floor.
Patrik: Oh, I see. He’s now on a regular floor.
Joy: Yeah. And they have the ventilator in the room right there next to him. But they’re saying they can’t put him on it, that they have to take him back down to the ICU. And the same with the BiPAP. They can’t do that on the regular floor. Only in ICU.
Patrik: In ICU, which makes sense. How long has he been on the regular floor for?
Joy: Maybe five days.
Patrik: So the last time he’s been on the ventilator is about a week ago?
Joy: Yeah. It’s been about five days.
Patrik: Been about five days. Okay.
Joy: Five days. And he was on, right? Well, he was on the ventilator, but they put him on the trach collar, and they felt like he was okay. They did the trach collar for a couple of days, and they felt like he was fine. So, we were excited, and they were able to move him.
Patrik: Fair enough. And now they are talking about high CO2 (carbon dioxide)?
Joy: Right. He’s up to 72.
Patrik: Okay. When you visit him, is he drowsy, or confused?
Joy: He’s completely confused. It’s everything he was right before we put him on the ventilator the first time. And so that’s why I insisted that they check his CO2 levels again.
Patrik: Yes. You’re on the right track there.
Joy: Thank you. Okay. I’m sorry.
Patrik: That’s okay. Because the minute he goes back on the ventilator or on the BiPAP, doesn’t matter. BiPAP or ventilator, it’s almost the same. It’s just a different setting. That CO2 will come down in no time. Right? And his baseline should be reestablished, and the baseline is he’s not confused, I would imagine.
Joy: Right.
Patrik: Can he talk? Does he have a speaking valve?
Joy: Yeah, he can talk. Yeah, he was back to talking and everything when they put him back on. Sorry, it’s like hot as blazes here.
Patrik: Right.
Joy: To have the air conditioner in here. But yeah, I don’t know if he can’t get in.
Patrik: I can’t see him. He’s not here.
Joy: Oh. He said the respiratory team is coming to reconnect the ventilator.
Patrik: Good.
Joy: So, he is there.
Patrik: Good. I like what I’m hearing there straight away.
Joy: Yeah.
Patrik: So, with all of that said, so they’ve checked the CO2. Do you know if they’ve checked an arterial CO2 or a venous CO2? Do you know?
Joy: You know what? I don’t know.
Patrik: That’s okay. That’s okay. Does he still have an intravenous line?
Joy: He does. He just got the feeding tube and the IV. He got the IV, he’s been on the feeding tube. And then he got an IV, I think a PICC line keep going there yesterday, the day before.
Patrik: Right. Why did they put that in?
Joy: I think for like to take blood. They’ve been trying to draw blood. They’re having a really hard, he’s a very hard stick.
Suggested Links:
Patrik: Yeah. Okay. That makes sense. So, would you then say that the CO2 has been climbing gradually day by day?
Joy: It has, yes. Yesterday it was like 62. The day before it was 55. And then today was just an alarming 72, which is about, it was actually, that’s actually higher than I think it was when we initially put him on the ventilator the first time.
Patrik: And just, yes. And just remind me, he doesn’t have an underlying condition of COPD or asthma?
Joy: No, but his cancer is, that tumor on his head is, actually, it seems to be a little bit more contained. It seems to have stopped growing. We’ve had them put flax seed oil in his feeding tube.
Patrik: Right.
Joy: But I think the biggest thing we wanted to ask you was, is there anything else between ventilator and the BiPAP? But it sounds like they’re getting ready to hook him up.
Patrick:Right. There probably is. There probably is, Joy. So, there is a device called Cough Assist and I can send that to you.
Joy: Oh, can you? Thank you.
Patrik: Yes. There’s a device called Cough Assist that might help.
Joy: Okay.
Patrik: It might help. The BiPAP in and of itself might be sufficient. But let me ask you this. When he was off, well, when he was off the ventilator, how close would you say was he from having the trach removed? Do you know?
Joy: Very close.
Patrik: Very close.
Joy: Yeah, that’s why, I guess, I want to ask you. Why are they not just doing the BiPAP?
Patrik: It doesn’t make any sense to me. I don’t actually think there is any need for, the Cough Assist might help. It’s mainly for coughing, not so much for CO2 reduction, but it might still help. I don’t understand why they were hesitating. Probably because they wanted him out. So, they’ve been in your ear to send him to LTAC, is that right?
Joy: Exactly. That’s all they’ve been, yeah.
Patrik: So, I would say the BiPAP should help, and it could be just couple of hours here, a couple of hours there. With the CO2 going up and with him getting confused, that’s probably impacting not only on his quality of life, but also was he getting mobilized?
Joy: Right. He was starting to get mobilized. And so, I guess that’s why I’m asking. I don’t know. Rey said that they are putting him back on the ventilator right now.
Patrik: Good. But basically, with the CO2 climbing, that’s been a big step backwards because he couldn’t get mobilized. I guess he was probably getting better because he was getting mobilized.
Joy: Right. He actually sat up yesterday. I took a picture of him, but I was sitting on the edge of the bed.
Patrik: Great.
Joy: Yeah, they were moving his legs and asking him to bend his toes and stuff and he couldn’t. They were doing it for him, but they did have him sit on the bed.
Patrik: That’s great.
Joy: And that was when he said, yeah. So, I was glad to see that. But now I’m like, his CO2 levels are going back up. So, are you saying, Patrik, that if he gets on the vent now and they bring his CO2 levels down, they can take him back off of it and put him on the BiPAP the next time instead of another vent?
Patrik: Look, if they put him on the ventilator now, they might use BiPAP. So the BiPAP is just a setting. So basically, depending on what ventilator they’re using, as I said, I’ve just looked through your notes. The last picture that you sent me, there’s no reason why they can’t use a BiPAP setting on that particular ventilator. So, the BiPAP is just the ventilation mode. That’s all it is, right? Yes, there are designated BiPAP machines that only can do BiPAP, but on the ventilator that he was last time, they just need to change the settings. That’s all. Right? And his CO2 levels, I argue, if they use the right settings should come down within hours.
Joy: Right. Okay. All right.
Recommended:
Patrik: So if he needs BiPAP in the long term, which I hope he doesn’t, they may use a BiPAP machine, but for now all they need to do is hook him up to the ventilator, probably choose BiPAP as a ventilation mode to begin with, and then see how he goes. Now are you saying, or are you suggesting that the high CO2 is related to the tumor?
Joy: They’re saying no. They’re saying that, let me think. How did they say it? So, his pH levels are still I guess okay.
Patrik: Right. Okay.
Joy: I think they just went up a little bit or something, whatever the wrong direction is. But it’s been very slow. So that’s why they did not feel like it was necessary to do anything regarding his CO2.
Patrik: I see.
Joy: They said that his kidneys were compensating and that it was okay.
Patrik:Yes and no. The kidneys were compensating for his pH going up. So the kidneys stopped the pH from going up. But the kidneys won’t stop him from having a high CO2. So, what happens is, when someone is having a high CO2, they’re going into what’s called a respiratory acidosis. Right? pH is going up and that could put the blood in imbalance. So, the kidneys then excrete alkalotic substances and that brings the pH back in balance. But it won’t stop him from the CO2 going down. It just keeps the blood in balance. That’s all, right? So, I don’t want to get too medical here, but the bottom line is this. Yes, the pH might be okay, but the CO2 is still high, and therefore he needs that CO2 down. And the only way to get the CO2 down is with BiPAP most likely.
Joy: Okay. And it’s okay that he’s back on the vent?
Patrik: Well, it’s definitely a step back, but the only way to manage it at the moment is with the ventilator slash BiPAP. That’s the only way to manage it at the moment. The question is, what’s the long-term plan? That’s the question.
Joy: Right.
Patrik: Right? Is this a one off? Why did it happen? How do they think they can prevent it going forward without using the BiPAP?
Joy: Yeah. So, they’re saying that they feel like he needs to be on the ventilator longer and that he would be able to do that in a LTAC.
Patrik: Okay.
Joy: That’s what it shows.
Patrik: Right. Do you feel that up to this point with the CO2 rising, you would say that he’s made progress since we last spoke?
RECOMMENDED:
Joy: Yeah, I think up until, you know, it’s hard to say, but definitely we feel like the nutrition was, we feel like he was looking better. He was more alert. I mean, because he was completely delirious right before they had put him on the ventilator the first time. So, he seemed, he was able to have a conversation. They were mobilizing him. And I think if we felt like if we could mobilize him, we felt like he was getting better and that we were right. We wanted to make sure that that tumor stopped growing also.
Patrik: Would you say that between last time and now, besides the, I mean, it sounds to me like he’s made progress. I mean, it’s not unusual that in a situation like this that it’s two steps forward, one step back. It’s not unusual. So, no recovery. I’ve seen very few recoveries in ICU that are just up, up, up all the time. It’s usually two steps forward, one step back. So, my concern is, from what you’re sharing with me, how will they get the CO2 down in the long run? He might need a sleep study. Do you know whether he had a sleep study?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!