Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Tracheostomized Husband is in the ICU. Is a Skilled Nursing Facility Better for Him?
You can check out last week’s question by clicking on the link here.
In this week’s episode of ““YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Kaye as part of my 1:1 consulting and advocacy service! Kaye’s husband had a cardiac bypass surgery and tracheostomized on ICU and is now on LTACH for recovery.
My Tracheostomized Husband was in ICU, now in LTACH. What are the Priorities for His Recovery?
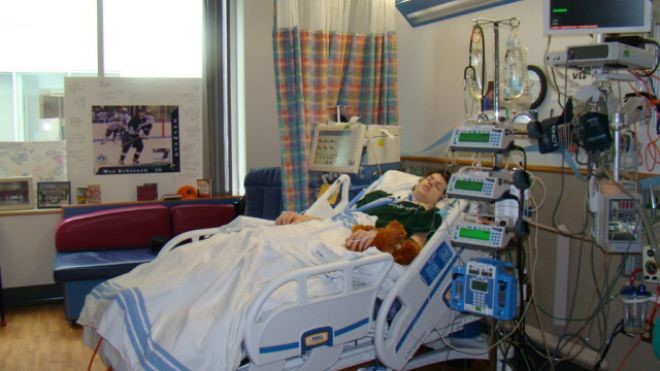
“You can also check out previous 1:1 consulting and advocacy sessions with me and Kaye here.”
Kaye: Hello Patrik.
Patrik: Hello Kaye, how are you?
Kaye: I’m good, it’s actually evening there right?
Patrik: Yeah that’s right that’s okay.
Kaye: Good evening, how are you? It’s early morning.
Recommended:
Patrik: That’s right I know. It must be just after 8 o’clock where you are.
Kaye: Yeah. I’m on my way driving to see my husband.
Patrik: Right.
Kaye: Everything is well with you, everything okay?
Patrik: I’m very well, thank you. I’m really well, thank you.
Kaye: Good to know. Good to know.
So, I’m afraid I’m going to tell you what’s happening-
Patrik: Right.
Kaye: It’s really, really, really busy here, My life has been so busy.
Patrik: Mm-hmm (affirmative).
Kaye: So last time I spoke to you they were planning to move my husband to the healthcare.
Patrik: Yes. Yes.
Kaye: And we are in LTACH which is really very… very good facility and people.. what is this facility called, people know and stuff, so it’s really, really good, but the good news is, today, they’re removing my husband’s trach.
Patrik: Oh fantastic.
Kaye: They’re taking it out.
Patrik: That’s fantastic. That is really good.
Kaye: Yes. Yeah. So I’m so happy about it, so even out of the oxygen and he’s trach is checked for the past three days now.
Patrik: That’s really good. How long have-
Kaye: He’s … Yeah go ahead.
Patrik: How long ago did you go into LTACH when was that?
Kaye: September 1st.
Patrik: Right, so nine, ten days. Okay that’s pretty good.
Kaye: Yes September 1st when we got admitted to the LTACH they wanted to put him at night on a ventilator and I begged them, I said listen if he was doing good for two days and ICU without ventilator.
Patrik: Right.
Recommended:
Kaye: So he picked his way.
Patrik: Mm-hmm (affirmative).
Kaye: And they agreed with one condition, if you do go into the distress they will put him back I said fine let’s do that.
Patrik: Right.
Kaye: So he was saying he never used them while he was there, so they downsized the trach and they said let’s see how he’s going to do this way. So he learned how to set the respirations to his flow.
Patrik: That’s great.
Kaye: And he’s doing it very, very well, no problems with his throat and they said what do you think if it will stop this I said let’s do that.
They kept his oxygen level…his level, I know this thing, it’s from 93 to 99, in this range.
Patrik: Yup, yup, that’s good.
Kaye: I said okay-
Patrik: Oh anything about 92 is usually fine.
Kaye: Okay. Where he goes 93 usually it’s steady I would say 95, 96.
Patrik: Right. Right. That’s good. But even a little bit lower might actually be fine. But 95, 96 is great. That’s great.
Kaye: So, he was more than went to the 11.8.
Patrik: 11.8?
Kaye: Are you with me?
Recommended:
Patrik: Yeah, yeah I’m with you. What do you mean 11.8?
Kaye: Haemoglobin.
Patrik: Sorry I didn’t get that. What do you mean when you say 11.8? What do you mean by that?
Kaye: Haemoglobin, haemoglobin.
Patrik: Oh Haemoglobin. Okay so that’s gone up.
Kaye: Yup.
Patrik: That’s gone up, that’s good. Has he had more blood transfusions?
Kaye: He has right before we were at … Before we were transferred to the LTACH, they gave him 2 units.
Patrik: Great.
Kaye: Once he got immediately to LTACH there’s no problem, no antibiotics, he is sitting on diuretic-
Patrik: Right.
Kaye: He’s swelling, edema went down we don’t have that anymore.
Patrik: Okay.
Kaye: He’s got moving much better, his legs.
Patrik: Right.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Kaye: He was moving little but not much, but his muscle was so weak.
Patrik: Yeah. Yeah. And are there-
Kaye: This is my concern.
Patrik: Are they sitting him out of bed?
Kaye: Are they what?
Patrik: Are they mobilising him? Are they getting him out of bed?
Kaye: Okay. We’re good, we’re doing very awesome he’s sitting on the cardiac chair twice a day right now.
Patrik: Okay.
Kaye: Approximately every time, an hour and a half, two hours-
Patrik: Right.
Kaye: So, total approximately three, four hours a day, and plus myself I hired a helper right now.
Patrik: Right.
Kaye: So, we have already sitting out three times a day and massages came really, really, really awesome.
Patrik: Okay.
Kaye: Probably four, five times a day.
Patrik: Right. Right.
Kaye: He’s doing excellent with the difficult therapy with his chance to get back he’s capable of catching ball and throwing ball back to you. And his hands are very, very mobile I would say.
Patrik: Right.
Recommended:
Kaye: And all of the things he does, where there are about his trach.
Patrik: Right.
Kaye: So today, they have been thinking to take it out.
Patrik: That’s great. That is really good. But you are saying, the mobilisation is mainly what you have organised, if you hadn’t organised it, they wouldn’t be doing it? Is that what you’re saying?
Kaye: I don’t think so, because they’re saying, the typical therapy they’re offering three, five times, but to be honest with you Patrik it’s not even three times. When I’m there, when I’m there, when I’m saying, “Okay guys we are ready for physical therapy,” 30 March I put pressure on all of them. I’ll be honest with you-
Patrik: Who-
Kaye: And I am actually organised this special routine to turn him around every two hours. I created those sign in sheets for the times, and they all have to sign up for the time.
Patrik: Good.
Kaye: And I come and I check, and I check because otherwise he was laying all day long and no one is coming because they think oh well they have a family there they can turn him around. They have a helper there, she can turn him around. And I said it’s not okay.
Patrik: No.
Kaye: You’re going to turn him around, and they actually, once I did this sign in sheet, they are doing it.
Patrik: Good.
Recommended:
Kaye: They are coming and they are doing it. Yeah.
Patrik: I’m very pleased to hear that. Very pleased to hear that.
Kaye: I met with the doctors and they said that he will have to go through the rehab for the extensive physical therapy because he is so weak.
Patrik: Mm-hmm (affirmative). Can I-
Kaye: And I’m worried about that. Yeah go ahead.
Patrik: Yeah, no… no. Of course, and you should be worried about that. I have one question and that’s mainly my curiosity at the moment. Do you think he’s off the ventilator and gets the trach removed, because he’s improved? Or do you think it’s because the LTACH is particularly good?
Kaye: Yeah. No. I ruled it out. I thought about this too. Because insurance in my understanding gave us 25 days okay?
Patrik: Yeah.
Kaye: And the insurance is also asking about it before every seven days.
Patrik: Okay.
Kaye: So, what they do son of a gun, they give you his progress every seven days and they okay another seven days. I met with the case manager and his doctor and I told him, “Doctor, if he’s not ready to be on his own, I don’t wanna rush this time because guess what, guess what, I’m not leaving.”
Patrik: Yeah, yeah, yeah.
Kaye: They said, the doctors, I’ll be honest with you, she said, he is not using antibiotics, he’s not using any drugs, we’re not giving him any of the blood transfusions because his haemoglobin has significantly improved. We don’t see any infection, we see his lungs are improving, there’s no water staying in his lungs, and no water into pleura underneath of his lung. And I think he’s really ready to get up.
Patrik: Yeah, good.
Kaye: Looking at my husband, looking at my husband, I will be honest with you, he improved significantly given spiritually, mentally, he’s much optimistic, and he is, every time I’m telling him, “Honey if you have any problem in breathing, you will have to let me know, because legal wanna rush the doctors.” He said, “No I’m doing good.” I ask him, “Do you feel you will be confident.” He said, “Yes I will be confident.”
And so, he is the one who actually can give me characteristic of his feelings. And so far I see him, and my husband, bless his heart, my husband is trying so hard, so hard to work out his lungs and everything.
I would say 99% I’m very confident. Of course one would think of me about that the stuff he went through.
Recommended:
Patrik: Yeah yeah.
But I mean you said I do remember last time, I do remember when we spoke last time, your husband was struggling with breathing, but even then you said you do believe he will come out of it. You said that, I do remember that.
Kaye: Yes. I’m telling you if I have a go, I have a very good intuition of feelings always. I always can … And I just listen to myself, and even after the surgery, once he was intubated and he wasn’t moving for a couple of weeks, I knew he will come out, but some reason, I don’t know what it is Patrik-
Patrik: Yeah you do, well-
Kaye: I cannot explain it.. what.. I knew he gonna come out.
Patrik: Well it’s something that I always recommend, I mean I always recommend listen to your feelings, and listen to your intuition. You know, I think it’s very important.
Kaye: Yes.
Patrik: You know-
Recommended:
Kaye: And I believe my husband will get up and walk maybe not seven miles, not seven miles, but I know he will be able to walk fine. My intuition’s telling me it’s gonna have to go for several months-
Patrik: Yeah, yeah…yeah.
Well, but the good news is, if they can decannulate him, then they can focus on the muscle rehab and not the ventilation part, you know, that part is taken care of.
Kaye: One thing I’m really afraid is swallow, and doctor told me my husband failed but the thing is, also by removing the trach and exercising which we’ll do this exercising, four exercises, listening songs, we’re using loud noises, quiet noises, breathing and … My husband just now, who was kidding, he recently learned how to pass the secretions off from his throat. It was struggle for him before, but now he’s regaining all the things back. He’s kind of re-learning.
Patrik: Right.
Kaye: Also using old things come on before.
Patrik: If he’s swallowing have they tried that? They must have. They must have tried it.
Kaye: Yes. We’re going to … He was able to swallow, to suck on an ice chip, but I’m afraid he has the silent, what you call it, silent-
Patrik: Silent aspiration?
Kaye: Yeah. I’m afraid that. But he did really good with ice chips, but, they are going to do barium swallowing within this couple of days, they’re going to do the steps and see how he would be able to pass the food that way.
Patrik: Yeah, no no-
Kaye: But I know from previous swallows that he did okay on applesauce, he was okay.
Patrik: Okay that’s good. That’s really good-
Kaye: And they said, it’s what he thought ought to do.. yeah.
Patrik: But I would imagine, if they are planning to take the trach out, he doesn’t need much suctioning anymore.
Kaye: No. We did not suction him for the whole week.
Recommended:
Patrik: Good good good. That’s really good.
Kaye: Because he was able to pass through, he does it, not after … I would not say every minute he make it a couple of times now. But, he’s capable of doing it like you and I, we can get it out.
Patrik: Yeah that’s really…that’s really encouraging.
Just remind me, your husband never had a stroke, he never had a stroke through all of this?
Kaye: No, no.
Patrik: Yeah yeah yeah.
Kaye: No. He never had a stroke.
Patrik: Yeah, no no, I’m so pleased. I’m so pleased to hear that. What are they saying is a next step, once he’s got the trach removed, what’s the next step?
Kaye: They would be watching him, his wound to heal. And very much just that one day take the trach out very much insurance confident for. And they pretty much will be, what are they going to do, they … After it heals, he will get sent to the rehab.
Patrik: Yeah that’s great.
Kaye: This is what they plan to do.
Patrik: That’s so good. I mean that’s really encouraging news. Very encouraging.
Kaye: Yeah. I’m really happy, even afraid of the rehab, to be honest with you, I’m just like … And don’t be that happy, don’t be that happy, we’ll have another steps, swallow that, another step, we have another step, lungs, I hope it will be okay, I hope he will start walking. There’s so much things to go-
Patrik: Oh yeah.
Kaye: We have so much complications, you know.
Recommended:
Patrik: Yeah.
Kaye: I’m telling you, my husband took me for a ride, I’ll be honest with you.
Patrik: He did? He completely sure did.
What happened, I know when we last spoke and there was still the talk about getting him to a nursing facility. Why did he go to LTACH and not nursing? What happened there?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!