Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
WHAT IS VENTILATOR ASSOCIATED PNEUMONIA (VAP)?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Francis as part of my 1:1 consulting and advocacy service! Francis’ wife had a brain death test in ICU without consent and is asking if it’s legally right for the ICU team to push towards killing her by doing another brain death test which she has not consented to?
My Wife Had a Brain Death Test in the ICU. Why Are They in a Hurry to Kill Her?
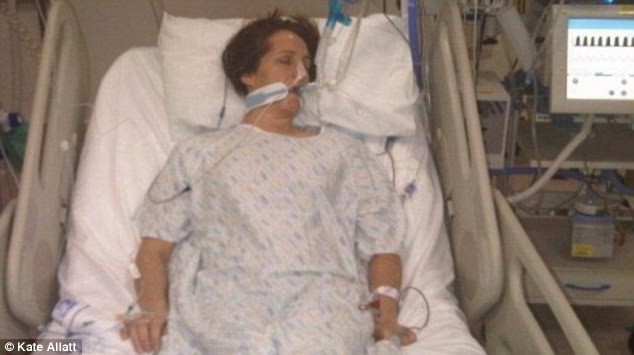
“You can also check out previous 1:1 consulting and advocacy sessions with me and Francis here.”
Francis: Hello?
Patrik: Hi Francis. It’s Patrik again from Intensive Care Hotline. Now, I had a bit of a look, and I found the End-of-Life Care policy in New York. And I’ll send that to you that in an email just a minute ago.
But, I’ll read it out to you, so that you know what we can do with that. I’ll read that out to you. There’s a section that we need to use.
“If the patient or the patient’s representative,” which is you, you are the patient’s representative, “disagree with the position to withdraw intervention, the family representative should be given the opportunity to secure the services of another physician, and supported in their efforts to do so, if that is their wish.”
Francis: Okay.
Recommended:
Patrik: Okay? I sent that policy to you. In fact, it’s not a policy. This is actually law. This is New York law. I sent that to you in an email. When you’re going to hospital, it’s probably best to take that with you.
Or, if you have it on your phone, you can show them on your phone, in an email or whatever. But, you know, the evidence that you are bringing to the table is mounting. So you’ve got this that I sent to you.
I had a look, and I haven’t got what I need about brain death testing yet. I had a quick look about brain-death testing in New York. Basically, what its saying is, it’s referring back to local policies, which is, again, why you need to ask for the hospital policy.
Francis: Okay.
Patrik: Right? So the law about brain-death testing, in the U.S. and in New York, is pointing back towards local policies, which is why it’s so important you need to ask for that policy.
But in the interim, that document, that I just sent you a moment ago, the End-of-Life Care Guidelines in New York, clearly support you, as the spouse of somebody who can’t make their own decisions.
Francis: Well, that’s kind of like what happened earlier. I wanted to secure another physician, and they said they couldn’t. We called in this hospital, the other hospital wouldn’t take them.
Patrik: Right. But, that’s okay. You’ve only asked one …
Who asked that other hospital? You or the physicians there? Who made that contact?
Francis: They wouldn’t talk to neither physician. They only talk to the physician.
Recommended:
Patrik: So, they initiated the contact. You didn’t initiate the contact. Is that what you’re saying?
Francis: Yeah, I actually called the hospital, and they asked to speak to the physician. Yes.
Patrik: Okay. That’s all right. That’s all right, but you could go to another hospital.
Francis: Okay.
Patrik: Right? You need … Forget about everything that happened, really. Just keep bringing stronger evidence. You are not agreeing to what’s happening, and the law is clearly supporting you with that.
Francis: Okay.
Patrik: Have they used the term “futility,” or “futile treatment?” Have they used that term?
Francis: No.
Patrik: Okay. That’s all right, then. Don’t worry about it. If they happen to use the term, that’s fine. That’s fine.
Recommended:
So, check your email. I sent that to you. Take that with you when you’re going to the hospital tonight. And just because one hospital wouldn’t take it, doesn’t mean another might not.
Francis: Okay.
Patrik: Right? You see, it’s very easy in those situations, to give up, Francis. It’s a very difficult situation, I understand that. It’s incredibly tough. It’s a life-or-death situation, and giving up is easy in those situations, because they present this situation as a very one-sided situation.
You know? They just say, “Oh, we make the decisions, and you don’t have a say.” You have a lot of say, you just need to exercise your rights.
Francis: Okay.
Patrik: Your wife doesn’t have an advanced-care directive.
Francis: No.
Patrik: Okay. But, if you and your wife would have sat down three months ago, and you would’ve…
Let me ask you this. Have you and your wife ever discussed what she would want in a situation like that?
Francis: Yes.
Patrik: Right. And she’s very pro-life, I would imagine.
Francis: Yes.
Patrik: Have you mentioned that to them?
Francis: Yes, they asked me what… We had discussed.
Patrik: Okay. And that’s in this document that I sent you as well. That you are advocating for your wife, in terms of what she would want.
Francis: Yes.
Patrik: Right? And that’s in the document, too. So far, you know, there’s two issues. You are talking to a nurse practitioner, who’s not the decision maker, that’s one issue.
And the other issue is, you haven’t presented any evidence, beyond your wishes. Now, you need to back up your wishes with documentation, which is what I sent to you.
But, the other evidence will be in the brain-death testing policy, as well as in the hospital withdrawal of treatment policy, and in the medical records.
I also sent you, in the first email that I sent you, there’s a link to the Department of Health in the US, very clearly says you have every right to access medical records.
They’re just making life difficult for you. That’s all. You have every right to access medical records. Every right.
Francis: Mm-hmm (affirmative)-
Okay.
Recommended:
Patrik: And you probably have to point that…
And if that, also, if you think it’s not going anywhere, you need to threaten with legal action. You need to threaten them, to bring in a lawyer or an attorney, tomorrow.
Whether you do that or not doesn’t really matter, but they need to know that you are thinking about this. You have to stop them doing what they’re doing.
Francis: Then…
Patrik: All you need, you need to buy time, to determine the next steps.
Francis: Okay.
Patrik: Did you get the emails that I sent you?
Francis: Okay, let me check.
Patrik: Have a look. Make sure you got them, because they’re very important.
Francis: Okay.
Okay, let’s see. Yes, I see the End-of-Life Care policy. Is that it?
Patrik: That’s it. And I also sent you another quick summary, End-of-Life Care Policy, and I also sent you-
Francis: I see both.
Patrik: -quick summary about what to do next, in the hospital itself. And I also send you a recording of the call.
Francis: I see. I see it. Thank you.
Patrik: Okay? So, take action. Don’t be afraid. Don’t be intimidated by them. Don’t be afraid, and don’t be intimidated.
Recommended:
Francis: Okay.
Patrik: Okay? Let me know when you’re in hospital, and let me know what you want me to do next. Okay?
Francis: Thank you.
Patrik: You’re very welcome. All the best, for now. Take care.
Francis: Okay.
Patrik: Bye. Bye.

Patrik: Hello. Hi Francis, it’s Patrik here from Intensive Care Hotline. Sorry, I just missed your call. Great, great.
Okay, sorry, I’m not following. I’m not following. You’ve got the medical records and what did you say about EEG and ECG?
Okay. Can you … okay a transplant. Okay yep, yep, Uh-huh (affirmative).
Okay great. Do you have those results? Okay. That, and also ask them to sit down with you to evaluate those results. I can’t believe they have done those tests without sitting down with you and elaborating on that. That to me is very unprofessional, and it’s highly inappropriate. You know what I mean, don’t …
Okay. Okay what does he say?
Okay. That doesn’t concern brain death. What’s the correlation between the tests they’ve done and saying that your husband is brain dead, that’s what I want to know?
Recommended:
Okay, is that still the case as of now? Are they saying there is no blood flow to the brain as of now, that’s what they’re saying?
Yeah. Okay. Okay, that may well be the case but, that still doesn’t … You see, somebody has no blood flow to the brain for more than three minutes, they sustain what’s called a hypoxic brain injury, right. What does that mean? It means the brain can be irreversibly damaged, but I think I mentioned that to you when you contacted me for the very first time. There is no, or little correlation between brain dead and brain damage, there’s a big difference. Right, your wife might be brain damaged, but that doesn’t necessarily mean she’s brain dead. There is a big difference between being brain dead and being brain damaged.
Right. What have you … You’ve got the medical records, that’s good. What’s happened with any more talk about the brain death testing today and the withdrawal of treatment, any more talk about that? No, no, no, no. No, no, have you shown them the law? Have you shown them the New York legislation, have you shown that to them?
Yes, yes.
(silence)
Recommended:
The brain death testing policies. Say that again, say that loud. They don’t have that for you? Sorry, you’re dropping out. If you can say that last part, you’re dropping out. Okay. Okay, they don’t have that available, that means they’re not transparent with you. Okay look, I really need to be very clear here Francis, you need to be very forceful here if you wanna stop them. But you have to also use evidence to be forceful. If you’re babbling around with that, your wife could be dead this afternoon. You can’t be babbling around with that. I don’t think you understand the gravity of the situation.
You have all the evidence in your hand to stop them. Now, yesterday they were telling you, you can’t have access to the medical records, now you have access to the medical records, right. Yesterday they were telling you they were doing certain things, to in essence kill your wife. You have all the evidence to stop them from doing that, but you need to act on it.
Yeah. Yeah. I sent you the Withdrawal of Treatment Policy for the state of New York. Okay and I highlighted this in yellow for you on page five. Right, that’s what you’ve got to take and pretty much rub into their face. You’ve got to rub it into their face. This is a life or death situation. You didn’t hire my services to babble around with this. I can only get results for you if you follow what I’ve given you. If you are going half-hearted about this, your wife might be dead this afternoon. You can’t be half hearted around this.
Francis, your wife … I would never say that I can save a life. I would be foolish to claim that because I can’t, but what I can do with my advice is buy time. Buy time until they’re following due process. They’re not following due process. They’re making up their own rules and they are going against what’s the law.
What do you think changed, so you got access to the medical records, what do you think changed? Why all of a sudden have they changed from not giving you access to the medical records, and within hours you had access to the medical records, what do you think changed?
Correct. Correct. Correct. You’ve shown them something and they know that you are doing your research and they know that if they’re not following you, they could be in big trouble. Imagine they’re doing what they set out to do and you don’t question them. Right. They might do the brain death testing and they might stop treatment this afternoon. By you showing them the law, they won’t be doing that because they know they could be in big trouble. They also know that 99% of the families don’t question, which is why they get away with that sort of behaviour. Right, they know that 99% are not questioning, but you are not the 99%, you are the 1%.
Recommended:
I cannot save a life, but I can guide you to buy time. That’s all you want for now, you want to buy … What’s the rush from their end to stop your wife’s life? What’s the rush, where’s the urgency?
Yeah. You want to stop them from doing the brain death testing, that’s number one. Now, you are telling me they don’t have the policy? Now, I can assure you that they must have a policy. They must have a policy about brain death testing and they must have a hospital policy for withdrawal of treatment, they must have that. They’re lying to you. I’ve never worked anywhere, where they don’t have those policies. They’re lying to you.
Right. I’m very happy to talk to them now. All you need to say is, you can say that I’m your cousin and I’m an Intensive Care Nurse, that’s all you need to say. You don’t need to disclose who I am, I’m very happy to talk to them.
Do you want me to talk to them now or do you want me to talk to them later? What do you want me to do?
Who am I talk … Right? Who would I be talking to, who would that be?
Okay great. What’s his name? That’s all right.
Okay.
Yeah. You can call me back when they enter the room, that’s absolutely fine. Before you go, I’ll tell you what I’m going to tell them. I’m going to tell them that you want access or, number one, I’m going to ask them to stop the brain death testing this afternoon. Right. Number two, I’m going to ask them for the policies and I’m also going the make them aware of the End of Life Care Law in New York. Right. I will ask them, “What’s the rush in killing your wife, where’s the hurry?”
Please, please. Thank you. Thank you, bye, bye.
Patrik: speaking.
Francis: Hi, Patrik. The doctor is about to walk in, but the EEG tech is here to do the EEG and I’m refusing it, too, because they wanted to do another EEG.
Patrik: Okay, so they want to do the EEG?
Francis: Mm-hmm (affirmative).
Patrik: You are refusing it. That’s good. Keep refusing for now. They need to understand that they can’t just do whatever they want. You need to challenge them with the policies, you really do. If they … I can tell you-
Francis: The EEG is set up.
Patrik: Yes.
Francis: The EEG is … that’s the test that I … So, yesterday I had asked them if they could do a EEG before they did the-
Patrik: Alright.
Francis: the brain dead test.
Patrik: I see. So, you asked them yesterday, but now did you say that now you are refusing it? Is that what you said?
Francis: No, no.
Patrik: No.
Francis: I’m asking, is it okay to go ahead with?
Recommended:
Patrik: Yeah, I think so. I think an EEG is fine. I think an EEG is fine. An EEG is very different compared to brain testing. I think you’re very safe with an EEG. It’s a very safe test, but you really need to go back … I sent you this email yesterday in regards to ask for those hospital policies about brain dead testing as well as the end-of-life care policy within the hospital. You need to keep asking for that, and you need to tell them that unless you have seen those policies, you will not agree to anything, and if they don’t give you those policies, you need to say that you will get legal advice on it. Whether you do that or you don’t doesn’t matter, but you need at this point in time … because it’s such a difficult situation, and you don’t have much time. You need to say those things.
Right, don’t worry about if you don’t get an attorney, but you need to use stronger language, and you need to make them aware that you feel if they are doing the brain dead testing and potentially withdraw treatment, that they’re going to kill or murder your wife. You need to use that language. You need to start using … right. You will need … Refer back to the law in New York. That law is crystal clear, and it’s black and white.
Okay, okay.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!