Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of the INTENSIVECAREHOTLINE.COM PODCAST and in the last podcast I interviewed Shirley who shared her sister’s stiry in ICU and LTAC!
You can check out the last podcast here.
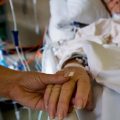
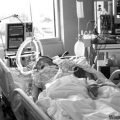
In this week’s episode of the intensivecarehotline.com “PODCAST” I want to share another story of a family who’s going through a tremendous ordeal with their husband and father in ICU! In this interview from one of our clients Arabella is sharing her and her Mum’s ordeal of having their father and husband in ICU for over 11 months. Arabella’s Dad is currently in ICU on a ventilator with tracheostomy and Arabella and her Mum are fighting a battle with the ICU team about what is in the “best interest” for her father.
Listen to Arabella’s story here or read the transcript of the podcast below.
INTENSIVE CARE HOTLINE PODCAST: My Dad has been in ICU with tracheostomy and ventilation for 11 months! The ICU team wants to tell us what’s in the best interest for our Dad and it’s wrong!
Patrik: Hello, and welcome to the intensivecarehotline.com podcast. Intensive Care Hotline helps families of critically ill patients to improve their lives by making informed decisions, get peace of mind, control, power, and influence. Thank you and welcome for listening to another episode of the intensivecarehotline.com podcast. I’m your host Patrik Hutzel, from intensivecarehotline.com.
Patrik: And today, I have a very special guest with me. Today, I’ve got Arabella with me. Hi, Arabella, how are you?
Arabella: Hi. I’m all right, thank you, amidst this absolutely horrific situation that we’re in. But thank you for speaking with me today.
Recommended:
Patrik: Yeah, and thank you for coming on to this podcast, because I know your situation. And I know what you’ve been dealing with for it, the last 11 months. We’ve been in contact on and off for the last 11 months. And I understand your dad has been in ICU for 11 months.
Patrik: Can you tell our listeners more about what you’re going through, why your dad has been in ICU for such a long time? And do you think your dad will come out of this?
Arabella: Yes, thank you, Patrik. Dad was taken into A&E with respiratory arrest 11 months ago now, and was then taken into the ICU, where he still is. He was first in a different ICU for two weeks and because of lack of beds, he was then changed to the Sister Trust, because he was supposed to be the most well person.
Arabella: So he was transferred in the middle of the night, which is one of the first things that just highlighted us to the kind of situation that we were in. And never thought that 11 months down the line, that we would still be in an absolute horrific situation here in the UK, and within the NHS too.
Arabella: I must say, the NHS on personal experiences prior to this, are absolutely fantastic. And sadly, I would never ever have thought that this would happen in this country and with the NHS, where they have such a grasp on you, and they basically cover up a lot. And that’s the situation we’re in. And we have fought and fought and fought for my dad and also, what is in his best interests.
Arabella: My dad has been through so much. He is on a ventilator and has a tracheotomy. So he’s now fully ventilated. And he was doing extremely well, and then a situation happened in November. He was destined to go to a specialist unit in London, a respiratory unit. And he was doing so well until a consultant came on, because here in the UK, the consultants change all the time.
Arabella: And a consultant came on and even though he knew, I must point it out, that dad had at that time a potential diagnosis of motor neurone disease. Which for people that don’t know, motor neurone disease is a terminal illness. We only found out that he would potentially have this by looking at his medical notes with a psychiatrist on an off chance. We were never informed.
Arabella: But basically, the consultant that night decided to take my dad off of the ventilator, even though he knew that he had suspected motor neuron disease, which affects the lungs. And that’s where people obviously pass away, because of lung failure. And he knew this and he decided to take my father off of the ventilator that night.
Arabella: And since then, it has been an absolute fight, because we have been up and down. They were prescribing my dad Risperidone and then hence why I got in touch with you, Patrik, because we could see all the things that they were doing to let my dad slip away, because of what had happened. So obviously, we fought from that moment to keep my dad alive.
Arabella: And this is the most ridiculous thing. You’re in an ICU unit and the family outside of the unit are trying to keep their loved one alive. And that’s what I’m saying, I never thought I’d be in this situation here in the UK and with the NHS.
Patrik: What was your response? It sounds to me like when the intensivists wanted to take your dad off the ventilator, you didn’t see that coming. What was your immediate response?
Arabella: I mean, it was absolute disgust and shock. I mean, basically we were told, I mean, there’s so much to go into, Patrik, absolutely so much as you know of our conversations. But at that particular point, when he was taken off the ventilator, he, in the morning, he had no airway entry. And he had to have emergency intervention.
Arabella: And when we asked for the medical records, there was nothing that was recorded about that. And apparently, the consultant said, well, it wasn’t an issue. But the man had, for brain damage, at 17.6. But obviously, talking to you, more than three minutes at 17.6 on your CO2 is going to cause some damage to the brain.
Arabella: And what happened is that a couple of days after, the consultant took us to the side, he said, all your dad needs now is a few good days in a hospice with some dogs and cats and children. Now, this is 11 months on and my dad is still here.
Related:
Arabella: So I think what I want to say to the listeners is don’t listen to what the consultant says, because they could be completely wrong. Yes, consultants are completely right, but in this particular case and with our particular situation, this consultant was covering his own back. I mean, my mum said I want to take him to a private hospital. And he said, well, why would you want to spend his, not my mum’s, his good earned money on care? He’d want you to live a good life.
Arabella: So when we talk about best interests, they think that they know that the person lying in that bed that is wearing a hospital gown is just a patient. They do not know the ins and outs and the best wishes that that person would want for themselves or for their family.
Arabella: And my dad through this all has wanted to live and he has wanted to fight for his life. And obviously, we’re helping him. So when that comment was made, it was a decision, because ultimately after that, the respiratory unit, the specialist respiratory unit in London said we’re not going to take him. Because obviously, with this aggressive weaning, he didn’t do well.
Arabella: So this consultant blocks that from happening. So my dad then was faced with a choice. And this is what I said in this meeting, I said so he doesn’t get to go to a respiratory unit. But you’ve just now commented, because one of the nurses in that meeting said, well, we can take him off the ventilator here, and we’ll put a Swedish valve on, which is a valve for moisture, to take him off the ventilator for him to die at home.
Arabella: And I said…
Patrik: To humidify, to humidify.
Arabella: Sorry?
Patrik: To humidify the air.
Arabella: So, yes, the Swedish valve, to humidify air. So basically, because he was not breathing through his mouth, it’s a humidifier through his tracheostomy. So she said, we can take him off the ventilator here, and he can die at home. And my response is, he can’t go to a respiratory unit, so the other option is death?
Arabella: So obviously, from that particular moment, it highlighted to us what was being planned, and what they thought was in the best interest for my dad, not his best interest, our best interest. Sorry, not our best, their best interests. And we’ve had so many conversations about cost, how much it costs for somebody to stay in an ICU bed.
Arabella: And the point is, is that my dad is still there. And he has fought, I mean, we then had to have best interest meeting about what was going to happen. Because we fought for him, we got him, after your advice, we got all the Risperidone removed, because that’s what they were doing. They were increasing the sedation, so that my dad would just be in… And I hate to use that word, but that’s how to describe it, a vegetative state, where you just lie. So he was in that and they were saying this because he wouldn’t sleep.
Arabella: Now, the consultant, the one consultant who actually does have, who is very clear, said, you’re more than welcome to come and stay to help your dad get some sleep. And by doing that, so this is mid-November. By Christmas Day of me going and staying there with him overnight and helping him sleep, so that they wouldn’t put him back on the Risperidone, my dad on Christmas Day started walking without a ventilator. I sent you the footage…
Patrik: With the diagnosis then of motor neurone disease, it’s a degenerative disease that stops people from using their muscles. They’ve diagnosed him with MND and then he starts to walk, which is not happening in MND normally.
Arabella: And without a ventilator.
Patrik: And without a ventilator.
Arabella: And he was just on the Swedish nose. So my dad turned himself completely around. And obviously, because we got all of those medications removed, also they put a DNAR (do not attempt resuscitation) on my dad without our knowledge. And we managed to get that obviously removed with your help. Subsequently now, a month ago, they put that back on my dad, because I’m that’s something else to come back to.
Arabella: But my dad obviously started really fighting to live, because his body was getting more food and obviously, he’s putting on weight and he was doing really well. So what happened is that we had a best interest meeting to say what would happen, where my dad would go, and they decided that he could go to a long-term care. My dad was awarded full funding in January to go to a long-term care placement.
Arabella: And the issue is that this placement, for whatever reason, and he told us that it could be very quick, still has no bed. I mean, I phoned last week, they still have no bed. We do not know why, because whether the unit has got involved, we are stumped.
Arabella: And speaking to other people, we’ve been waiting for this bed, because there are obviously very few places with my dad’s diagnosis, clinical diagnosis. Because he’s never had the major tests. Otherwise, I’d have to go to Kings in London for that. There are other places that could take my dad and this is what we’re doing now. Because he is stabilised, again, obviously I will have to come back to that. But he’s just been existing in a corner. In 11 months, he has had one shower.
Patrik: It’s shocking. Can I just ask Arabella, you mentioned the best and I always put it in quotes, quote-unquote, “best interests”. Because we’ve been talking on and off, I know how often it has been mentioned. How do you feel about the hospital calling a quote, unquote best interest meeting and how do you feel about that?
Arabella: The thing is, they’re not best interest meetings at all, Patrik, and feel really strongly about this. If you don’t have power of attorney and basically, this is the issue, that sadly, mum and dad never sorted that out. Any listeners out there, please do it, please get power of attorney straight away.
Arabella: Because if your partner is there, or loved one, father, mother, sister, please do it. And even if they’re not in hospital, please do it anyway, because we never know what’s going to happen. My parents never thought that they would have their power taken away from each other. They’ve been married for 53 years, and it comes down to nothing.
Arabella: Because once people say this is in their best interest, they have the control. So in all our best interests meetings, and taking your advice, you don’t have to go. I mean, there have been many that we have not attended because ultimately, they ask you to sign things. And when we’ve been there, we’ve not signed things, there have been best interest meetings that we have not attended. Because we have not been given an agenda, or the people’s names that are going to be there.
Related:
Arabella: So we’ve taken it is that, you’re just creating a meeting to make decisions about my father, that we don’t agree with. And if we don’t agree with it, then we’re not going to come to the meeting. And we will take the notes and then ultimately, we will decide to do with them, or seek legal advice after.
Arabella: So I do say to your listeners out there, don’t feel that you have to attend any meeting. If they want to take you into a room, don’t go in on your own. Please take notes of everything.
Arabella: And one of the things that I wish that we had done throughout this whole… And I say it’s a journey, because my goodness, it has been one, ups and downs, a roller coaster of emotions, how it has affected us all. Please take notes of everything, and write your own diary.
Arabella: Because one of the things is that to be able to refer back to those things is very important when you’re in a case like this, and say, you know what? This is not in his best interests, because of the conversation that we’ve had two months ago. And it’s very important.
Arabella: And they have to say, again, repeatedly, you know what is in your loved one’s best interest, they don’t. They see a patient that’s lying there, they’ve seen hundreds of times, thousands of times before, that is lying there in a hospital gown. They don’t know the history of that person. They don’t know what they used to look like.
Patrik: Just a number-
Arabella: They’re going on a statistic, a patient without… Yes, you call them a name, but there are many other patients they see all across different hospitals. And they do not know that the best interest of your loved one, you do. It’s you, it’s the relatives and the family and the friends, all those people that are close to that person that know what is right and what they would want.

Patrik: Absolutely. So the best interest really is a euphemism and nothing else. It’s just a nice word to achieve the agenda of an ICU.
Arabella: Yeah. And it really has. When I hear that wording, it makes me feel sick to my stomach. Absolutely sick to my stomach, because I know what it is. I know what it is, it’s saying you actually don’t have any right. It’s a, you don’t have any right in the meeting. That’s what it is.
Patrik: It’s a…
Arabella: We’re the ones in control, we’re the carers, so therefore, it’s a what’s right for us, not what’s right for you and what’s right for the patient and what’s right for the family. It’s what’s right for us.
Patrik: Yeah, they’re managing, what I always say, they’re managing their worst case scenario by framing it as a quote, unquote best interest meeting. Their worst case scenario is exactly what’s happening with your dad. Somebody stuck in an ICU bed for a long time with an uncertain outcome. That is their worst case scenario and that is why they are doing what they are doing.
Arabella: Yeah.
Patrik: Trying to cut your dad’s life short.
Arabella: And that’s what we’ve seen. I mean, that’s what we’ve seen. From that moment, I mean, up until November, so from September to November, we were like the rest of those families that we’ve seen coming in, and subsequently the families that we’ve seen. And we were them, we were the ones that were smiling at the doctors, we were the ones that were saying thank you. We were the ones that were just very pleasant of taking what the perceived authority was, from the consultants or from the doctors.
Arabella: And obviously, the nurses and the registrars, because they’re the ones on the ground and they know. But it’s the hierarchy of the matrons and the consultants and the medical directors and all the ones up there that have got all the purse strings, and they’re the ones that are in control.
Arabella: And ultimately, what we’re facing is a situation of, there is one man and his family against us as a whole hospital, against us as a unit, and this is all of our lives, and all of our jobs, and this is what we’re facing. Because ultimately, we’re easy to sacrifice in the big scheme of things.
Arabella: And I urge families just to keep… It’s very difficult. It’s so difficult to do. And you have to, I don’t know, you have to keep digging deeper and deeper. And you will lose your mind many times and you will not know how to carry on. But I just urge people that if they’re in this situation, please find it, dig deeper and dig deeper.
Related:
- THE 10 THINGS YOU DIDN’T KNOW ARE HAPPENINGBEHIND THE SCENES IN INTENSIVE CARE THAT HOLD YOU BACK FROM HAVING PEACE OF MIND, CONTROL, POWER AND INFLUENCE, WHILST YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE!
Arabella: Because if you don’t say anything, if you feel like you are lacking confidence, and you don’t mention anything or you don’t send an email and make it wider known, then… I know that we’ve done everything that we can do by my dad. And I would hate for somebody else to be in that position, and go, I wish I would have said something, I wish.
Arabella: Because in actual fact, that night that this happened to my dad back in November when it all started, we did, we did say, we said but he has sleep apnea, and you’re him putting on Zopiclone and you’re taking him off the ventilator. Please would you put him back on? And they assured us that would they would put him back on and they didn’t.
Arabella: And ultimately, I think what I’m trying to say is that, yes, even though we did say something, things can happen out of your control. So it’s very important to… Sorry, I’ve got myself into a muddle there. But I was just trying to say it’s very important, regardless of what happened, for your own sake and your own self and your own mental health that you do say something, regardless of…
Patrik: And that you do the right thing for your family member. Doing the right thing for your family member.
Arabella: It is. Yes.
Patrik: And Arabella, can you elaborate a little bit on your goals? Once you knew sort of that your dad will have a very hard time of coming off the ventilator, given that he’s been ventilated now for 11 months, can you elaborate for our listeners what your goals were from that point forward? Obviously, you mentioned the facility. But I think you also wanted to elaborate or look into home care. What are your goals at the moment?
Arabella: At the moment, we’re going through a situation of court protection for my father, because it was decided that it wasn’t appropriate. Obviously, because this placement was taking so long to come about, off of my dad and my dad’s just in an ICU ward, the continuing healthcare team approached us and said why don’t we… So it came from them. Why don’t we actually get your dad home?
Related:
Arabella: We were over the moon, because obviously we were told that that could never happen. That he had to go to a placement first for rehabilitation, and then it was up to the placement to see about whether he could come home. Obviously, that was our goal, always has been, because those are my father’s wishes. He’s written notes, he’s told us from day one being in there, I want to go home, take me home. Even to the point where he’s bribing people, get me the ambulance and trying to get out of bed.
Arabella: And those are his wishes. And I think this is the important thing, is that whatever situation it is, thinking about what your loved ones’ wishes are. For us, it is that he wants to come home. Yes, it’s lovely for us, of course it is. But it’s very important to think about that person that’s in that bed, it’s their wishes.
Arabella: Now, if it’s a person’s wishes that they think, you know what, I don’t actually want to be like this. Then, you’re taking in their wishes. And I think this is very important, you have to remember what it is that your loved one would want. My father wants to come home.
Arabella: So we’re doing everything that we can to enable that to happen. And that means fighting the hospital and the decision. Because as I said, we don’t have power of attorney. Now, it’s gone to court protection. And basically, what they’ve said is that it takes a long time to put into place. And that because of my dad’s situation and his disease, it would be very difficult to have the care at home.
Arabella: But our argument is, is that he’s on a portable ventilator, he’s fed by a peg. And he doesn’t need 24 hour… He does, of course he does, but when we’re in the hospital, my mum and I are sitting with him and the nurse is either over at the desk or sitting on a desk writing notes about… They’re having to write notes and instant reports about us now, and that’s not a whole other situation, because we’ve made complaints.
Arabella: So, yeah, so the point is, is that that’s what we’re trying to do to get him home, because those are his wishes.
Patrik: Arabella, I just want to ask you one thing that I think is very important for our listeners in the UK, in particular. I mentioned to when we spoke before the recording, Alfie Evans case last year in Liverpool had all the… worldwide publicised case, that the NHS at the time managed to basically remove guardianship from the family there too. And it sounds to me like you’re in a similar situation.
Patrik: It sounds horrible to me that the NHS has that power to take guardianship away either from a parent or from a child by themselves or from your mother in this situation. And then basically, puts their agenda onto a patient, that’s quote, unquote, in their best interest. That’s a huge concern for me. I have not seen that outside of the UK. It must be concerning for anybody who’s got a loved one in ICU or in the health system in the UK, because now this is the second time that I’m coming across this.
Patrik: That when there’s dispute, the NHS basically has the power to go back to a court and remove guardianship and then can do basically whatever they want. That’s a huge concern. What are your thoughts around that?
Arabella: Well, I mean, I did not know. And that’s why I go back to what I said, that you could be in this country and with the NHS and to be a victim of it, in terms of their control and their power. When someone is so sick and poorly, it is unbelievable.
Arabella: So basically, what they’ve done is they’ve suddenly put a deprivation of liberty on my father, saying it isn’t safe for him to leave the hospital. So they basically, ultimately said, he’s ours. That’s what it is. And because we have pointed out and made complaints and asked questions, my mother and I and the family have now been accused… I mean, it’s absolutely disgusting. We have these false allegations against us.
Arabella: So I don’t know what they are trying to achieve, but they’ve ultimately stopped. Now, this is a man that they have diagnosed with a terminal illness. And they know that he gets anxious, they know that he loves spending time with us, this is 11 months down the line, where we haven’t had any restricted access to my dad. I’ve stayed overnight by his bedside for probably 80% of the time that he has been in there.
Arabella: And what they’ve done now is they’ve limited our access to him, because they say we are in breach of the policy. So they incited a management of aggression and violence policy to say that we have threatened… My mum is 72. And that we have intimidated staff.
Arabella: So this is what I’m saying to your listeners. They will try whatever they can to ultimately cover their own tracks. And it is very important for you to write down everything. I mean, they’ve said that we have tampered with medical records. How can we tamper with medical records when we can’t access them?
Arabella: They accused me in a best interest meeting, obviously that you attended Patrik, of loosening my father’s…
Patrik: Yes.
Arabella: And that we have had bad relationships with the nurses, which we completely contested, because that is absolutely appalling. I have been in education for 20 years, and run a boarding house, and I know about safeguarding and this is my own father. And so they used that as a reason of why they decided that my dad could not come home. Obviously, that was a best interests meeting. So they said that we would be unsafe.
Arabella: So ultimately, because I think they think this could go legal, they have created a kind of, quickly, a picture about us. And they’ve done it, obviously, trying to do it publicly as well, in front of other people, so that they have a backing. And it is absolutely appalling, that they are now… It’s almost like my dad is a pawn, it’s disgusting. This is a person and we are fighting over this person and if they had any empathy in their heart, they’d think, you know what, we’ve just put this family through absolute hell. Why don’t we help them? And we have not had any of this, this whole way along. Because it seems like they’re making it up as they go along, this unit.
Arabella: It’s because we took your advice, and it’s horrible to say, but we’ve caught them out.
Related:
Patrik: But now, here is a massive issue. By them removing guardianship, you don’t even have to right to look at the medical records, because you don’t have guardianship. I mean, one thing that we advise constantly to clients is get access to the medical records. And that’s no issue as long as they have medical power of attorney or have guardianship.
Patrik: But in your case, they’ve basically removed every right that you had with losing guardianship. You can’t even look-
Arabella: We can’t speak, we can’t ask the nurses questions anymore. If there is anything, we have to have a weekly update with the lead consultant. Now, that’s a weekly update on how my dad is doing. We can’t ask them anything. We can’t ask them if he had a sleep. We can’t ask him if he passed a motion. We can’t ask them…
Arabella: When I tried to ring the other day, at night, because obviously we have to leave at six o’clock now, I rang to see how he was, about 11 o’clock at night. And I was made to feel like I was disturbing the unit, because I made a phone call.
Patrik: Yeah, it’s a horrible, it’s a nightmare situation for you, for your dad and for your mum. As we all know, your dad needs the family support and they’ve basically completely removed it and it’s just absolutely appalling. It’s beyond imagination really.
Arabella: Sorry, Patrik, and they’ve said if we don’t abide by their rules, then they will remove our access completely and we are banned from the hospital. So basically, they are saying you have to play our game, otherwise we are not letting you see your father.
Arabella: And there’s no evidence. I mean, obviously, there’s no evidence against us, because it’s false. So they have created this situation, as I said to you before, it’s like this horrific chess game, where they’re making a move, because they think that we’re going to go a legal with it. And everything that we wanted to do from the outset, is just to have my dad have quality of life in his situation. It is unfair for him.
Arabella: And now they’re punishing us as a family, for what? For questioning, for standing up for our rights, for my father’s rights? The point of this is the person that is key here is my dad, and it shouldn’t be what’s good for them, or what’s best for the NHS or that particular unit or the name of the hospital. It shouldn’t be that, you should be thinking, this is this man, we have diagnosed him with a terminal illness. We don’t know how long he has. We shouldn’t be depriving him of loved time with his family.
Arabella: This, I don’t get. Obviously, they felt that we’ve done something where somebody has, because we’ve made a complaint about a senior nurse, who put my dad’s CO2 valve on the wrong way, the whole day. And then ultimately, he was breathing in his own CO2. We made a complaint about that.
Arabella: Since that particular point, it has become horrendous. Even more horrendous. This is because we highlighted, again, a negligent case, which ultimately resulted in my dad having an ischemic attack and becoming responsive.
Patrik: That would have been my next question. I think it’d be interesting to hear from your perspective and for our listeners as well, how has the whole situation impacted your dad? I mean, we talked about this before, your dad is very strong. And he has managed to pull it through all of that.
Patrik: But how does the situation at the moment, how do you think it is impacting on your dad?
Arabella: He’s basically suffering clearly from ICU psychosis. He is completely, it’s almost like a locked in syndrome. As we just said, it’s almost like a Twilight Zone for him. He’s not really engaging, responding. A little bit. He’s not using any facial muscles anymore. And it’s almost like he feels, why isn’t he leaving? Because each time we’ve said soon, you’ll be leaving soon, you’ll be leaving soon.
Arabella: And I think he thinks that he can’t believe anything anyone says anymore. So he’s just existing, and I don’t know where he is in his head, bless him. And it’s horrible. I mean, I’m using that word lightly.
Patrik: Yes, yes. I think it’s the best way to describe your dad’s situation. How do you think his situation could have changed if he had left by now? Obviously, it was all lined up, then didn’t happen. How do you think his whole recovery could have changed if he had gone to this long-term weaning facility? What do you think-
Arabella: Oh, my gosh, they’ve got a multidisciplinary team there who actively… So they would have observed him for a few weeks, they said. Then, put a physio programme in place, he would have had holistic therapies. Obviously at that time, he was very mobile, so he was getting out of bed, using the commode. He was very active and moving and responsive and listening to music.
Arabella: He could have had, even, because they stopped using the speaking valve on him for whatever reason. Once he had the flu, they didn’t put it back on him. So he would have had access to speech and language therapy, to various different things that would have enriched his life.
Arabella: And this is the whole point. My dad’s a very spiritual man in the factors of things about nature and a tactile person. And when you’re in a clinical environment for so long, I mean, he’s been there for nearly 11 months. And this has affected him, his mental health, obviously, massively. To the point I think he doesn’t know what is reality and what is not. And also, thinking, looking at my mum and I and thinking why are you not getting me out of here?
Patrik: Yeah, yeah. And it’s fair to say that, and I’ve seen it over the years working in ICU, it’s probably fair to say that even if your dad didn’t have ICU psychosis or delirium, it’s fair to say he’s depressed by now, with everything that he’s been through.
Arabella: Yeah, severely depressed, because he’s thinking I have been in here for such a long time. Why isn’t anyone doing anything? I’ve got everything that I need to go home. Yes, he’s accepted, obviously, that he’s ultimately got a tracheostomy and we fully ventilated, and he is fed by a peg. But all of this time until, obviously, we’re going back now to when he just suffered the ischemic attack a few weeks ago.
Arabella: He’s been able to communicate, he’s been able to play his music. I mean, obviously, he’s in an ICU ward. So he’s not getting any freedom of his own personal expression. But what he has been able to do, he has done that.
Arabella: And now, because he is bed bound, because even after the ischemic attack, he wanted to get out bed to use the commode. And they said, it’s not safe. We understand that, but it’s since that point they haven’t done anything more. The physios have been completely discharged him, we’ve asked for exercises, so they’ve given exercises for us to do with him, because we asked. Nothing was provided and so we need to keep this man mobile.
Arabella: And what they’re seeing now, is that they’re just deciding that this is a futile situation with my dad, because they’re not actively… we were the ones pushing. Please, can you give him a hand wash? I mean, the man’s had, as I said before, one shower in 11 months, and he’s had probably five hair washes and three of those have only been in the last month.
Patrik: Right. It sounds to me like they’re almost trying to break his will to live, and they’re trying to break your will to fight for him. I mean, that’s the best way I can describe the situation, knowing your situation. Is that how you feel too?
Arabella: Absolutely. I mean, you’ve just hit the nail on the head, Patrik, it is that. It is that they are thinking, they decided, going back to the best interest, they have decided it is in my dad’s best interest that he doesn’t live. They’ve decided that, because they think, because they put themselves into that position, I think. They’re thinking, how could you possibly want to, if you’re lying in a bed, and you’ve a tube out of your neck and out of your stomach, how could you…
Arabella: But they are thinking about it from their point of view, in their particular moment of life. My dad said, back a few months ago when they did put the speaking valve on, the psychiatrist said what do you want? My dad actually said sustained life. So he said that he wants to live and that has been recorded. He said sustained life.
Arabella: So they have decided that actually he doesn’t. So they are trying to, I can see it, they’re trying to break him. They’re not helping him get out of bed, and they’ve done suddenly a ceiling pair plan of treating with dignity, don’t do anything that he doesn’t want to do. Don’t take blood, unless clinically, a clinical side. Don’t take…
Arabella: The man in an ICU unit had an ischemic attack, had a heart attack, which is unheard of. Because what they decided to do is they decided that they weren’t going to monitor him. Even though that week, he was very clammy, I repeatedly said he’s very clammy. He may be dehydrated, because it’s very hot in here. He may have low potassium, because that’s something that my dad suffers with, low potassium all the time. And my dad started to wet the bed and they didn’t do any of those blood tests and they didn’t do any blood pressure.
Arabella: And what happened at 2:30 in the morning, he suffered an ischemic attack and then bizarrely, the next day when the cardiologist came round, they said his heart has gone back to normal, there isn’t any sign of any damage. But subsequently, because of that, what has happened, they then decided to reput a DNAR back on my dad, without obviously, so they put it back on him. Because they said it would not be in your best interest.
Recommended:
Arabella: And then the week later, Patrik, not the week later, but I’m just sort of… I’m thinking of when things were. Sorry, my head’s a little messy at the moment this morning.
Patrik: You’re breaking up there a little bit, Arabella.
Arabella: Oh, am I?
Patrik: You’re breaking up there a little bit. Can you hear me?
Arabella: Yeah, I can hear you. Yeah.
Patrik: Now it’s better. Carry on.
Arabella: Then, he had a small intestine obstruction, which we were informed would be a hernia and then inoperable. And palliative care were then brought in and literally, the next day, so four days, they took him off the feed. He was just on water, fluids and Hartmann’s. And we had palliative care come in, because obviously it was…
Patrik: Right. Right. You’re breaking up. I think we might have to… I can only hear you at times at the moment. We might have to wrap it up here, even though our listeners would like to continue the conversation, I know. Because I know you haven’t finished any we haven’t shared everything that’s important. But I can’t hear you at the moment. So maybe we’ll stop the recording here for now and record a second session at some point.
Patrik: But thank you, Arabella, so much for sharing this with our listeners. Because I’m sure our listeners can emphasise with your mum and your dad, it’s horrific. I know your situation. And from my perspective, it can only get better, really. It can’t get much worse from everything that you’ve shared.
Arabella: I know, thank you, Patrik. And I do hope that, if you can still hear me, that even anything that I’ve said in here that might help anybody else. Because I think this is the thing that I’m very aware of. It’s about all of us, actually, that we’re in this situation with a loved one in an ICU. That we’re all part of this actual bigger team and supporting each other for the people that we love, and that are very important to us, and actually being a voice. So for them, it’s very important that we are their voice.
Patrik: Absolutely. Okay, thank you so much, Arabella for taking the time and sharing this with our audience. I know this is really important for anyone listening. So thanks again, Arabella, and we’ll talk to you soon. You’ve listened to the intensivecarehotline.com podcast. And thanks for listening and I’ll talk to you soon. Take care.
Arabella: Thank you, Patrik. Thank you.
Patrik: Thank you, thank you. Bye-bye. Bye.
Arabella: Bye-bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s podcast episode and I’ll see you again in another update next week!
Make sure you also check out our “your questions answered” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!