Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Can Doctors Push You to Take Family Member Off Life Support?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Camille, as part of my 1:1 consulting and advocacy service! Camille’s brother is in ICU and the ICU team wants to perform brain death testing without any hospital rules. Camille is asking what should she do?
My Brother is in ICU and the ICU Team Wants to Perform Brain Death Testing Without Any Hospital Rules. What Should I do?
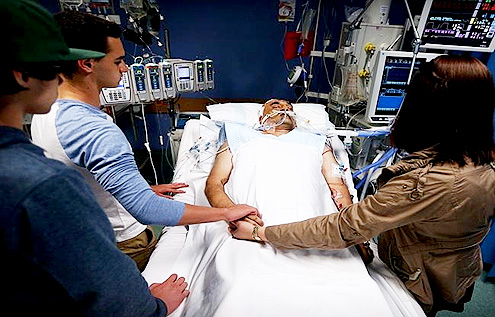
“You can also check out previous 1:1 consulting and advocacy sessions with me and Camille here.”
Patrik: Right? And if somebody comes in with something minor, of course, they want to help people. I’m not disputing. But in a situation like that where it’s life or death, the dynamics change completely.
Camille: Yes, yes. I understand.
Patrik: Right?
Camille: So, I’m so grateful.
Patrik: That’s great. That’s great. So my advice is, can you please send me that stuff? And then I’ll have a read and then I’ll tell you what to do next.
Camille: Okay. I will do that right now.
Patrik: Okay. Thank you.
Camille: I’ll go ahead and take a picture.
Patrik: Thanks.
Camille: Thank you so much, I appreciate it. I’ll just try and take the picture.
Patrik: Okay.
RECOMMENDED:
Camille: Hello?
Patrik: Hi, Camille, I’m sorry. Look, it sort of reminded me because I’m making, I’ve got unlimited international because I’m talking to people all over the world every day. But sorry about that.
Patrik: So, where was I going with this? Yes. So let’s just say-
Camille: Given the event, it’s been taken off.
Patrik: Correct, correct.
Camille: They told me they did the testing and it lasted 8-10 minutes.
Patrik: Okay. I tell you what I’m really wondering about, you know. I’ve seen the document, where it says your brother is brain dead, obviously. My experience shows with any brain dead people, right? The testing needs to be done by two independent parties. Sometimes again, dependent on the hospital policy or on the state’s policy one by an independent outside physician.
Patrik: That’s why you might’ve, you might’ve heard me- and that’s why I think this policy is so critical. Right? I have been in situations in the past as a bedside nurse and that only came over the years with experience. You know, it doesn’t, you don’t see that sort of stuff when you’re new in the environment. I only saw it sort of, in the latter years of my bedside nursing, right. Where I realized, hang on a sec, they’re doing brain testing, brain death testing here, but they’re not really following the rules.
RECOMMENDED:
Patrik: And families don’t, right, and families don’t know that. Right. You only see the fine, once you know enough about how an ICU operates and what needs to be. That’s when you find those things out. But, and here and here, here’s the other thing that’s important to know for you. Is this a big ICU? How many beds?
Camille: Let me see.
Patrik: Roughly? 20?
Camille: 38.
Patrik: 38? Okay, okay. That’s big. That’s big. Okay. So, I’ll give you an example. Okay. If this is a 38 bed ICU, there is a very, very, very high chance that within those 38 beds that there is one patient, at least, was waiting for an organ donation. At least.
Camille: Yes. Yeah, yeah.
Patrik: Right. So, and I’m not putting any judgement on it, right. I’m just saying that’s the reality. That’s the reality of a big ICU, right?
Camille: Yeah. Yeah.
Patrik: And you know, it’s just what it is. People are sick and they go to ICU and they’re waiting for organs. So that’s the dynamics. If this was a five-bed ICU or a 10 bed ICU, I would say, okay, well unlikely, but 38 beds, big ICU, there would be somebody within their most likely waiting for an organ, so, it’s all part of the dynamics, I believe.
Patrik: So, and their push is towards organ donation. And even if they don’t use it in their own unit, they would, there are people waiting for organs. Again, that’s just reality. So, and that’s all part of it. And then I realized at some point the brain death testing is not really, it’s not really following all the rules. Right. While I do believe that most people that are tested for brain death, are brain dead.
RECOMMENDED:
Patrik: I believe that it doesn’t and that that is on a legal level, they’re legally dead. What Professor Pope said. They’re legally dead. But that doesn’t mean that for a family with certain beliefs, cultural backgrounds, whatever, religion and so forth, it does not mean that illegal deaths make a family believe that their loved one should be taken off the ventilator.
Camille: Yes.
Patrik: Right. That’s what it, that’s what you’re dealing with. That’s what we’re dealing with. Yeah.
Camille: Yes, that’s right.
Patrik: Right. That’s why I believe this, the policy. The policy is going to be really important, because you know, if they can’t show you a policy, they’re potentially performing illegal tests. If they can’t back up what they are doing with a piece of paper or with an email or whatever with a document. In this day and age, it’s mainly online. But if they can’t back that up to me, that could potentially be illegal.
Camille: Do I cut off the tag that says DNR? I sent you a picture of that too.
Patrik: Do you talk to, what did you say?
Camille: I sent you a picture of the DNR on his own tag on his hand.
Patrik: Yes, yes, I’ve seen that. I’ve seen that. Yeah, I’ve seen that.
Patrik: I’ve seen that. Another thing when they talk to you, are they talking to you in front of your brother?
Camille: Oh yes. Today there were eight doctors in this room. All ready to bombard me.
Patrik: Right, right. Because you know, I would also tell them, please stop talking in front of my brother so negatively. I would do that if I was you.
RECOMMENDED:
Camille: I do.
Patrik: Oh, you have done that already? Okay.
Camille: With the doctors. Big arguments.
Patrik: Great. Okay, good. No, no, that’s good. So your brother has been started at 20 ml an hour of feed, which is not a lot, but it’s a start. And they, they would probably gradually increase that. So I have to look-
Camille: His oxygen. He had his oxygen, well, a percentage was 21. Yeah. And his total, VM?
Patrik: Volume, yeah.
Camille: Yeah, his total that used to be at 15, and it went to 14, then it went down to 10.
Patrik: Right, right, right.
Camille: They upped his oxygen for one week. They had him at 25% I mean 21% now he’s up at 35%.
Patrik: Right. Okay. I do believe that they are trying to optimize his condition for organ donation. At the same time, they also know that they can’t harvest any organs without your consent. I mean that’s not going to happen.
Camille: Yeah, exactly.
Patrik: Right. So but, change your approach and also with, with the lawyer or with the attorney what you might, what you might have to do tomorrow, that would be, you could always contact, there must be a court you can contact on a weekend. Right. There must be somebody you can contact on the weekend. Or as a last resort. You could potentially call the police as a last resort.
Camille: Okay.
Patrik: Right. So I mean, certainly a lawyer or an attorney would get back to you over the weekend. There must be people who are dealing with those situations. I mean, not that they happen every day, but they do certainly happen regularly.
Camille: So what would the police do? You mean when they’re going to pull the plug?
Patrik: Yes. That you could inform them and you could say to them, “Look, I need an injunction here, but I can’t get hold of a lawyer.” Maybe they have some advice for you about where to go next. Right. But you know, I mean you’ve contacted the lawyer later today. I believe so. Maybe tomorrow. You know, somebody will get in touch with you. Look, I don’t know. I know that here or even, again, this is not the first time I’m dealing with a situation like that. I do know that people over the weekend have been able to get hold of emergency lawyers or they have been able to go to court over the weekend. It’s, again, I’m not the expert on that, but it’s definitely possible.
Camille: Yeah. I did send a letter on my email to the gentleman, the attorney that you gave to me, I did send him an email.
RECOMMENDED:
Patrik: Good, good.
Camille: And I asked him if he could represent me in any way, in this urgent situation.
Patrik: Are you talking, are you talking about Professor Pope or are you talking about?
Camille: Yeah. Yeah. Pope.
Patrik: Yeah. Look, he will most likely respond to you. He’s very, I’ve contacted him numerous times on weekends, and I, and I just tend to send him an email because he’s in your time zone. I have sent him a lot of clients contact.
Camille: You’re so wonderful. Thank you so much. Yeah, I’m so glad you’re able to get in touch with him. Everything. I mean, now you just need lawyers on your side.
Patrik: I do. I look, I do work with lawyers. I do work with lawyers and he’s, he’s certainly you certainly one of them. And you know, I have, I have a podcast and I have interviewed Professor Pope on my podcast number of times because there is, we have a lot, a lot of similar interests. He comes from a legal perspective. He’s not a clinical person but, but he has a lot of perspectives, that perspective that I need and I have a lot of perspectives that he needs. And he is, he is really a wonderful person. I’ve contacted him numerous times on weekends and he always responds. Even on a weekend.
Camille: Is it true… Or is it true or possible with the situation like they’re saying, right now his brain dead? If in fact that when I rubbed his toes or his feet, he jerks his leg?
Patrik: That is a possibility. I guess what I would want to know, is he still on any medication? That’s what I would want to know. Right.
Camille: I showed you all those little bottles-
Patrik: Yeah. But it’s not, no, you did. But it’s too small. It’s too small. I can’t see what it is. What you could do as well as I would, I would ask for the medical records if I was you. I really would because, and the lawyer, if you get a lawyer involved, there’s a very high chance yeah.
Camille: Hum? Or something like that. H-U-M.
Patrik: Pardon?
Camille: It says hum, H-U-M, the container.
Patrik: Oh, I see what you’re saying. Like the container of drugs.
Camille: Yeah. But yeah, that’s what it says. It’s just, cause it was covered up with tape. H-U-M, hemolog?
Patrik: Humalog. Humalog is insulin. It’s insulin.
Camille: Oh, okay. Okay. So that’s, that’s what these are then.
Patrik: Right it’s insulin.
Camille: The other one that’s here. Yeah, that’s Humalog.
Patrik: It would be good to keep the pressure on them. I just request the medical records as well. And the lawyer, it’s a very good chance that if you get a lawyer involved, that he will ask for the medical records too. I don’t know what the lawyer does. Again, that’s not within my scope or sort of practice. Have they, since you’ve been there, have they approached you differently since last time?
RECOMMENDED:
Camille: Yeah, they’re all staying away. They’re definitely staying out of the room the whole time.
Patrik: What’s your interpretation of that?
Camille: And, and it doesn’t say anything anymore on the board to turn him every two hours.
Patrik: So that? They’ve stopped that?
Camille: Yeah.
Patrik: Okay. So, here is one thought there. That’s not a good sign. That’s definitely not a good sign. I tell you, we were dealing with a withdrawal of treatment situation potentially. Right? That’s what we’re dealing with. Withdrawal of life support potentially end of life. Okay. Sometimes people might use the term “withdrawal of care” instead of “withdrawal of treatment.”
RECOMMENDED:
Patrik: Okay. If they stop turning him, that to me it’s a sign that they’re withdrawing care. Now people can withdraw treatment but they must never withdraw care. In care, I mean also the care for you or for your family or for your brother, and that is a typical situation for me. They’re not only withdrawing life support, but they’re also withdrawing care towards you. You know, like what they did today, where they called you basically and told you their executive decision about next Wednesday. That to me is guerrilla tactics.
Patrik: Right? I mean like, it’s like bullying, there is no compassion towards- you potentially lose your brother, at such a young age. And they’re just walking all over you and saying, “Well this is what we’re doing next Wednesday. Bad luck.”
Patrik: And that is not a good sign. Of course, but it fits right in with their culture probably that they now stop turning him.
Camille: They’re going to do it right now. I’m just looking.
Patrik: Right, right. So, that is not a good sign, but so they did you say they are turning him now? Is that what you’re saying?
Camille: They are turning him right now.
Patrik: Okay, good, good. Keep an eye on that. Keep an eye on that.
RECOMMENDED:
Camille: Okay. There’s a sore on his back, he just can not-
Camille: You can help her. Now they’re putting him on his back right now. Can we check and see that sore on the back? To see how he?
Nurse Mary: We’re aren’t going to turn him again.
Camille: Oh. Oh, okay. All right. Yeah. Okay. That’s it.
Patrik: So right.
Camille: She put a pillow on a shoulder. That wasn’t a turn.
Patrik: Right. I’m just so you know, and hopefully Professor Pope gets back to you with something, but I’m just quickly typing in which city are you in? Are you in North Dakota?
RECOMMENDED:
Camille: Bismarck.
Patrik: How do you spell that?
Camille: B-I-S-M-A-R-C-K.
Patrik: Oh! Bismarck. Just give me one sec. Just give me one sec.
Patrik: Okay. I’ve just typed into Google court injunction, Bismarck, North Dakota. I’m just looking whether there’s something coming up where you can contact there, someone.
Camille: I’ve tried visiting there.
Patrik: Right, right. Look, look, I think, I think you have a little bit of time. You can tomorrow wait, whether the lawyer will contact you, if the lawyer doesn’t contact you, I would have a look whether you can go to the court directly on the weekend and there must be a way to do that.
Patrik: There must be a way you can approach a court on a weekend. And that would be the next step. And then even if that, even if you can’t get anything over the weekend, you probably would need to go to the police as a next step. And then you would still have Tuesday and Wednesday. You would still have almost like two business days to get, well-
Camille: Monday is a holiday.
Patrik: Yeah, I know. I know. But you would still have the whole Tuesday and you would still have Wednesday until five o’clock to get an injunction. Right. It’s not that you’ve got 24 hours and that’s it.
Camille: Okay. Okay. Yeah. So I think I’ll just- I feel blessed, you just walk me through everything as it’s like, it’s holding you by your hand. I mean it’s not only medical but also, giving me wisdom as far as like law’s concerned. I’m really grateful. You don’t know how grateful I am and just to be able to put my recommendations on what you have done in, so far. Just, I mean it’s like everything. No taking off my shoulder and then being there in the midst of the world. I mean, just to know that, I’m so glad you said “don’t go” because I would’ve walked into eight doctors yelling at me about my brother. That was a bad scene in itself.
Patrik: Yeah, absolutely. Absolutely. It’s a nightmare, and it’s bad enough that you’re dealing-
Camille: All the patients are hearing it cause-
Patrik: That’s terrible that means that the culture there must be really bad. I mean you wouldn’t, if you if you have those discussions you would have them behind closed doors.
RECOMMENDED:
Camille: Do you happen to know a doctor. Who would allow me to transfer him?
Patrik: I don’t know a doctor who would allow you to transfer him, but I’ll tell you what I think. You need to get an injunction to stop them from doing what they’re doing. Right. That’s number one. Once you’ve got the injunction and you have time, cause all you need for now is you need time. Okay. Once you’ve gotten an injunction, you will need to look at those options that I mentioned to you before. Potentially New Mexico, where somebody, because again, in some states, a person whose brain dead is legally dead. Right. In other states and especially in New Mexico, if people are brain dead, they are not legally dead.
Camille: Okay. Do you know of any other states?
RECOMMENDED:
Patrik: No. No. I don’t. However, however, if you will. I think again, probably ask Google saying something, like “legally dead brain dead.” I don’t, I don’t know. I’ll tell you what you could do as well. You could, I’ll tell you what I’ll do. I’ll tell you what I’ll do when we come off this call. I emailed you, what’s the name of the policies? No, and I will email you a link to Professor Pope’s blog. He has a blog and he’s blogging all about that and he must have a search box on there and he would have, I don’t know, type in “brain dead New Mexico” or something like that. Something will come up. Something will come up.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!