Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
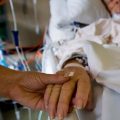
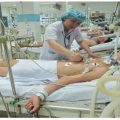
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Camille, as part of my 1:1 consulting and advocacy service! Camille’s brother is considered brain dead in the ICU and the doctor wants to pull the plug. Camille is asking what is the best thing for her to do.
My Brother is Brain Dead in the ICU and the Doctor Wants to Pull the Plug Now. What Will I Do? Help!

Camille: Hello.
Patrik: Hi, it’s Patrik here from intensive care hotline sorry, I’m-
Camille: Big doctor just called me and told me off, “You need to be here right now.” I said, “I’m at work right now.” “I don’t care. You need to leave work and get here right now.”
Patrik: You need help. You need help because what … You know, as I said, we’re very experienced in managing these situations. You need to change your total approach in all of this. You know, if somebody speaks to you like that, I would … you know, there’s one saying that I always say, sort of some games in life you don’t play in order to win.
RECOMMENDED:
Camille: Yes.
Patrik: Right?
Camille: Could you try to be the doctor on the other side?
Patrik: Yeah, I can tell you I am not a doctor. I’m an intensive care nurse with 20 years of experience, but I am very happy. I can speak to the doctors on a similar level. I’m not a doctor and they know that and I’m not … you know, I am happy to come in as your cousin, as your friend, or I can come in as a consultant, you know, it doesn’t matter to me, but I’m not intimidated. Right?
Patrik: And it sounds to me like you’re not intimidated either.
Camille: No.
Patrik: But they need to know that-
Camille: They want me to pull the plug now.
Patrik: That’s okay. That’s okay. Just, just ignore it. Which you have done.
Camille: Do I need to go and show up right now?
Patrik: Again, some games in life you don’t play in order to win. Does that answer your question of whether you should go there or not?
RECOMMENDED:
Camille: No, I guess I didn’t understand it.
Patrik: Right. No.
Camille: Yeah.
Patrik: Could be. I would not go there and that’s why I’m saying some games in life … they’re trying you to play their game right? But you don’t play.
Camille: Yeah.
Patrik: Right and I know it’s not a game. Don’t get me wrong. I know this is serious. This is very serious, but I’m trying to illustrate sort of, you know, a way forward. So I would be very happy talking to the doctor, right? Or to the doctors I don’t know how many people are involved.
Camille: Yeah.
Patrik: You know, and are they pressuring you with family meetings? You would have had some family meetings?
RECOMMENDED:
Camille: Yeah, we’ve recorded all of their conversations-
Patrik: How-
Camille: And they said, “Well, I’m going to have to go and pull the plugs because that’s what your brother wanted,” and they said, “No.” He says, “Well, he signed the durable,” which is a power of attorney and durable. Okay? Which is a medical durable.
Patrik: Yeah.
Camille: And I said, “Yes, but I have verifiable information that he has the mentality of a seventh-grader,” I said, “And he can’t read.” He says, “Yeah, but somebody would read it to him.” I said, “Yeah, but he did not want to sign it,” I said, “The only reason why he signed it is so that I could take him out of the state of Nebraska to bring him to my home.”
Camille: I said, “Plus,” I said, “He chose to live and that’s exactly what I’m doing. Abiding by his rules.”
Patrik: Yeah. How old is your brother?
Camille: He’s 58.
Patrik: Right. That’s very young. I mean that’s not … you know, I mean-
Camille: That why they want his organs, because he’s very young, you know?
Patrik: Yeah, absolutely. Absolutely. So how does that-
Camille: I just … I’m so glad I talked to you because I’m like … they push you all the way to your side. I mean, eight doctors, you know? And now this one was yelling at me, “You need to be here right now. She said “you need to leave your job.” I’m like, “Okay, all right, I’ll be there. Just wait.”
RECOMMENDED:
Patrik: Yeah.
Camille: I’m not in a rush. I’m not leaving so-
Patrik: Yeah, no, and, and again, you know, I mean that just sounds terrible. We’ve just worked with a client in Oregon the last couple of weeks where they were in a religious hospital too, and even though it wasn’t what I refer to as a perceived end of life situation, they were the worst people to deal with because they were real bullies.
Patrik: Look, I’m a Christian myself. Right?
Camille: Well that’s good. That’s so good.
Patrik: But I’m, you know … what I’m seeing … you know, and I work with all sorts of people, but what I’m seeing with some religious organizations, it’s just … I’m just horrified.
Camille: Horrible. I’m horrified too. I’m really scared.
Patrik: Let me ask you another-
Camille: They try to bully you, but the fact of it is, is that they’re taking my brother’s life while they think they can and they’re trying to manipulate it, but with the power of attorney, they can’t do anything. That’s my assumption, and that’s why they keep bringing all different kinds of doctors, you know?
Patrik: Yeah. So let me ask you this. Have you tried to get him to another hospital? Have you tried that or?
Camille: I have tried that, they’ve denied it. They painted a grim situation from day one.
RECOMMENDED:
Patrik: Yeah sure. What should I say to that? That’s their default position. So that’s nothing new. It might be new to you, but because we’re providing … you know, we’re talking to people every day, that’s nothing new. Okay? From my perspective, we know that the doom and gloom and it is their default position. So then moving forward there’s … so as I mentioned to you, I believe that the clinical level is very important. A policy level could be very important. I would not rule out getting him to another hospital at all. You know, again, we’ve certainly-
Camille: They’ve denied them to hospitals and yeah they did a scan, it’s a-
Patrik: You’re referring back to them as they are making the decision you need to stop doing that. You need to keep stopping… your language going forward is very important. The language that you are using from this point forward.
Camille: Okay.
Patrik: It’s very important. If you keep saying they are doing this and they are doing that, it puts them in a power position.
Camille: Yeah okay.
Patrik: You need to stop doing that. You need to stop doing that.
RECOMMENDED:
Camille: Okay. In their comments, what they were trying to tell me was that there’s a thing called nuclear medicine brain limited with the vascular flow and it says here the conclusion is positive for brain death, but the findings they say dynamic head and neck, vascular flowing images. There was a normal flow to the carotid arteries. There was no evidence of intracranial flow.
Patrik: Has there been testing for brain death? Has that been done?
Camille: That what this piece of paper says, it’s called the final result.
Patrik: But it doesn’t imply brain dead. It doesn’t imply that but-
Camille: It says a conclusion is positive for brain dead. There was no evidence of intracranial flow or uptake within the brain.
Patrik: Oh I see. Okay, so has that been done by two independent parties?
Camille: That was done by … yeah, and another doctor and imaging were done.
Patrik: Right. Okay. So that is new information then for me. So you are suggesting your brother is brain dead, is that what the papers are saying?
Camille: Yes.
Patrik: Right. I see. That is new information. Okay. I didn’t know that. Then I can see why they wouldn’t do a tracheostomy. I can see that. Where then … okay, so with the knowledge that your brother is brain dead, I can see why an attorney wouldn’t take it on. What … and I probably now would have to say if your brother has been declared brain dead, then it becomes an issue of, you know, what does the law in North Dakota say? You are in North Dakota, your brother is in North Dakota, is that right?
Camille: Yes.
Patrik: Yeah. So, what will happen is the law might allow the doctors to withdraw treatment. It might allow them, I’m not privy of the law in North Dakota. Right?
RECOMMENDED:
Camille: That’s right.
Patrik: I’ll give you a very quick rundown, and if your brother is brain dead, I don’t think I can help you. Right?
Camille: Okay.
Patrik: Because that puts a different spin on it. I’ll give you a very quick example. Have you heard of the case Nadine M.C.? Does that ring a bell?
Camille: No.
Patrik: No. I’ll give you a very very brief story. A 15-year-old girl in Oklahoma actually had, a tonsillectomy late … had a cardiac arrest.
Camille: Oh yes.
Patrik: Right? You’ve heard of her?
Camille: Yeah.
Patrik: Yeah, so she was declared brain dead by the hospital, and my understanding was that the state in Oklahoma would have allowed for the hospital to stop treatment. Right? That would have been within the law, however, the family managed to get her to New Mexico where it’s allowed to continue treatment even for people with brain death.
Camille: Yeah.
Patrik: Right? So I have no … I don’t know the law in North Dakota when it relates to brain dead, I do believe to a degree that they might be able to stop treatment without your input. However, I … look, again, that is outside of my expertise. If your brother wasn’t brain dead, I’d say, “Yeah, we can argue on a clinical level.” Given that he is brain dead, we can’t argue on a clinical level.
RECOMMENDED:
Patrik: However, what you can argue on, is potentially on a level that is … you know, they’ve mentioned religion, right? You could argue on a level that says, “Look, my brother may be brain dead on a clinical level, but that’s not, to me, on a belief level.”
Patrik: Right? So you could argue on that level, right?
Camille: Yeah.
Patrik: Which sounds to me like you might’ve done already, but on a clinical level, you know … in a hospital environment somebody is considered dead if they are brain dead. However, that does not often gel with the belief system of a family. Right?
RECOMMENDED:
Camille: Yeah.
Patrik: And that could be … and it sounds to me like you’ve been holding that argument there already.
Camille: Yes.
Patrik: I tell you what, I’ll give you another quick example of what you could do. This is outside of my area of expertise, right? Because I can argue on a clinical level but if somebody is brain dead, there is no clinical level to argue on. I tell you what you could do as a next step. You could contact-
Camille: Okay.
Patrik: You could contact a gentleman called Professor Thaddeus Pope in Minnesota. He is a medical futility lawyer. He may not be able to help you, but he may be able to set you up with somebody in North Dakota who can help you.
Camille: Okay.
Patrik: He’s a well known attorney in the US-
Camille: How do you spell his first name?
Patrik: Yeah Thaddeus, if you-
Camille: Oh Thaddeus.
Patrik: T-H-A-D-D-E-U-S.
Camille: Okay.
Patrik: Pope, P-O-P-E, like the Pope.
Camille: Okay.
Patrik: And he’s a professor and if you type into Google, Thaddeus … or Professor Thaddeus Pope medical futility lawyer, you will find him.
RECOMMENDED:
Camille: Yes. Okay.
Patrik: He will probably not take on your case. I know he has taken on cases in the past. He will probably not take on your case, however, he will know … he has a network. He has a network.
Camille: Okay. We’ll do that. Yes.
Patrik: Right. I’m so sorry that I can’t help you.
Camille: Thank you so much. Yes, but you’ve been very, very helpful.
Patrik: Okay.
Camille: I just, I hate the fact when they start yelling. They try to …that is not professional at all.-
RECOMMENDED:
Patrik: No, it’s not professional, it’s ignorant, and you know, no matter where people stand on the issue of brain dead, their point of view is yes, if somebody is brain dead, they’re considered dead. Right?
Camille: Yeah.
Patrik: And that may well be within their legal right, you know? Again, it depends on the law in North Dakota, right?
Camille: Yeah.
Patrik: But, that doesn’t neglect the fact that people have very different beliefs around what they think about this whole issue of brain dead beyond the medical fraternity.
Camille: Yes.
Patrik: Right?
Camille: I’m hoping that I can get to see him, or even getting a … I don’t know what to do, it’s just … it’s so scary. You know? It’s just like … because I think I definitely … if I need to call you back, is it possible? Could you talk to them on behalf?
Patrik: It is. No, I would talk to them. I would talk to them. I would be very happy to talk to them. Bear in mind, you know, if you do want me to talk to them, there’s a couple of things. Number one, I do charge a fee for that.
Camille: Okay.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!
Related Articles:
- 5 Ways to have control, power and influence while your loved one is critically ill in Intensive Care