Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
I Want To Request For My Dad’s Medical Records In ICU But Do I Have A Right As His Daughter?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Anna as part of my 1:1 consulting and advocacy service! Anna’s dad is in the ICU and she is asking for help for her dad to have the right kind of ICU care whilst ICU nurses are busy.
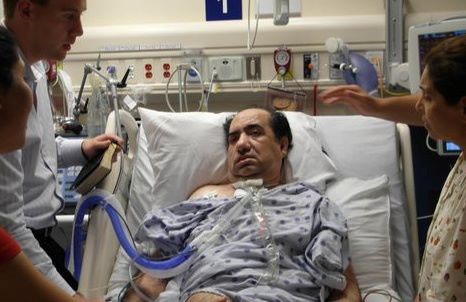
My Dad Still Needs the Right Kind of ICU Care Whilst ICU Nurses Are Busy. Help!
Hi Anna,
Thank you for your email.
Please see response and comments below.
Please let me know if you have any questions.
Kind Regards
Patrik
RECOMMENDED:
Hi Patrik,
Thanks so much for your email, which was extremely helpful to me yesterday. I had asked to see the respiratory consultant for a meeting which they arranged for yesterday afternoon. He took over dad’s care on Monday.
Patrik: That’s great that you have somebody on your side by the sounds of things
Yes, dad is still on the respiratory ward. I saw him yesterday and he looked well. He is still off all oxygen and says he is breathing fine.
Patrik: That’s fantastic and very good news
The respiratory consultant asked dad’s lead physio to give us an update; he said dad is improving and he is aiming to do physio 3 x a day.
Patrik: That’ll be very important, make sure that it’s not just lip service and that it does actually happen!
The respiratory consultant is a leading specialist in lung disease. I was impressed; he had reviewed dad’s chest history going back years, including scans and x rays etc. I liked him and felt I could trust him.
He told us dad’s lungs have recovered! We were floored. He said dad has interstitial lung disease, and that the most appropriate, evidenced treatment for dad is careful use of steroids. He said there is fibrosis/scarring – but that it is minimal. That dad has gone from 40% oxygen support to none.
Patrik: Getting different people on your dad’s care team was way overdue. It sounds like he’s positive and more optimistic, which is great!
We said ICU showed us the CT scan and subsequent x rays and said his lungs were in terminal failure and at best chronically damaged?
He said, “ok so my approach and interpretation as a respiratory physician is very different from ICU. I see lungs every day and every possible presentation. Some ICUs call in respiratory consultants to give a view, some don’t. Had I been involved in your dad’s care his presentation would have said to me interstitial lung disease. Craig made the turnaround after he was given steroids. The critical care team were right to treat for an infection and to focus on the microbiology; but my focus would have been what is the lung inflammatory response telling us. Why are his markers not doing what is expected? Is it still infection or is it inflammation? What else is going on?”
Patrik: Yes, that’s why I kept saying, get the specialists in. ICU is often having a different approach and has a different focus! The respiratory physician’s perspective and input seems to come at the right time.
RECOMMENDED:
He told us he wants to screen dad for a rare auto immune condition called ante synthetase syndrome. The presentation is interstitial lung disease and chronic muscle atrophy, along with other symptoms.
Patrik: Including micro aspiration potentially causing chest infection/Pneumonia as per fluoroscopy. It also says, “delayed cough”, which again is nothing unusual after tracheostomy removal but also concerning. What are the respiratory physicians’ thoughts about the fluoroscopy?
On Monday he sent off blood samples to a specialist laboratory in the UK to test for it. We should know the results next week.
He is involving neurology and wants to work with them. (I told him we had to insist on neurology getting involved in ICU). They are looking to do a head MRI scan. Neurology feel his swallow issue might be sensory axonal neuropathy?
Patrik: Ask them why they think that? Where is the evidence? It would be hard for anyone to learn swallowing again after such a long time of being nil orally and the tracheostomy. The MRI might give clarity about this diagnosis.
My stepmom asked if it meant dad will have to have a PEG feed? He said “I don’t think we should jump to that.”
Patrik: Your dad is not having a PEG or does he? He has an NG tube and that should be sufficient for now. PEG is too complicated and he doesn’t need another procedure
SALT did a video fluoroscopy (not a barium swallow) which showed dad doesn’t have a safe swallow. I attach screenshots of the report below for you.
Patrik: Safe swallow with micro-aspirations the report says. This is what they often find during those fluoroscopies especially after tracheostomy and neuropathy etc.. after such a long stay in ICU.
Patrik, should we find out what swallow assessments were done on dad historically, both in ICU and post ICU? My instincts say we need to find out. What we do we ask for?
Patrik: Get the reports from SALT, that’s the easiest way to find out what they have done or haven’t done. But also, if you have a meeting with the doctor, you can also request for SALT to be there and ask more questions such as what their plan is going forward. With micro aspirations still present, the risk for another chest infection is present as long as he has oral intake. It sounds like he can swallow to a degree but he’s probably not quite there yet.
As you know it was a concern, we expressed to ICU re his discharge to a ward environment. The ICU matron told me she thought it would be weeks for his swallow to return and that it would be a slow process before he was ready to eat food. And yet from the first day on the ward he was given custard and yoghurt.
Patrik: The progression or built up after tracheostomy removal usually is to go from yoghurt or custard to more solid foods but only after speech therapy has given approval. That’s why talking to SALT directly would be helpful to find out what their instructions were to the nursing staff and also to the dietician.
We are quite prepared to go to the senior executive level if we need to in order to get the care dad needs! We want to retain good relations of course, but we also want them to be aware we are watching! I told Dr. Cavalera yesterday we had to be robust advocates for dad and that he wouldn’t be alive otherwise.
Patrik: Yes of course you want good relations whenever possible and you have certainly shown that your family can’t be pushed around
After the steroid therapy dad went from 40% oxygen to nothing. Literally nothing!
Patrik: That’s fantastic and he’s found the right treatment!
My stepmom asked do you think Craig could come home eventually. He said “yes, yes I do”.
Patrik: You need optimistic people on his care team, keep working with him.
He said “look I think there has been a lot of negativity around Craig and his prognosis, particularly re his lungs. I think we need to change the focus to the positives: he has made a remarkable recovery in a week using the steroid therapy appropriately. His lungs have recovered. I will be looking to keep the steroids to a level that provides the lung support but at the safest lowest dose. I am conscious of his diabetes. It all needs to be balanced.”
RECOMMENDED:
His junior, a respiratory doctor, told me they want to write a paper on dad. He is a fascinating case, she told me.
Patrik: Your Dad is a fascinating case. He survived 7 cardiac arrests, that is unheard of!
Apparently, they did an x-ray today to see if dad’s NG tube (inserted in ICU as you know) is in the right place, which it is. Presumably this was to check the passage of liquid feed going through the line?
Patrik: The chest x-ray after NG tube insertion is purely to check the correct position. It needs to be ruled out that it’s stuck in the lungs because getting food into the lungs would be a disaster. The passage of liquid feed going through the line can’t be checked in an x-ray.
Dad still has extremely loose bowel movements requiring frequent changes. He is often aware after it happens and requests help. He does get sore and my stepmom Ginnie worries about whether they are really on top of his tissue viability. What should we be saying about this? Do we go to the ward matron to flag this up? Should we be saying things verbally or in writing?
Patrik: Ask them if his skin remains intact with the loose bowels. They should be checking his skin at least three to four times per day. They could also potentially try a flex seal or simply a “bum bag” to try and contain the loose stools and therefore protect his skin. Ask if they have either flex seal rectal tube or a simple “bum bag”. Try and bring it up verbally to begin with, given the complexity of the situation, I would also be asking if you can see his nursing care plan. Those issues and action plan should be documented there. If you can’t get anywhere verbally put things in writing for sure. If you need help in writing a letter please let me know, I can assist.
Patrik, I asked one of the nurses whether a continence nurse could come to see dad and do training? He said he didn’t see how they would be able to help while dad is still having liquid feeds???
Patrik: A continence nurse is specialised in doing sphincter and bladder training to maintain and/or relearn patient’s continence.
Also, my stepmom Ginnie told me that dad had said to her he was suddenly feeling the sensation of needing to urinate; she looked and saw the catheter bag was full. She went to tell the charge nurse, who said he would come to change it. It was a busy time, but the nurse didn’t come after a decent time, so she went back again to ask and he said he would do it. The auxiliary later admitted to Ginnie it wasn’t done for many hours after that and that dad was very uncomfortable. Surely this is not acceptable and really quite serious?
Patrik: It is serious if the bag was so full that your dad wasn’t able to pass urine due to overflow. That could cause urinary retention.
RECOMMENDED:
I told Ginnie to report it to the senior matron of the ward. Should we check what was recorded too Patrik? His notes are at the end of his bed. Of course, this would never have happened in critical care where it is 1-1; things like this demonstrate to me the drop down in care – the nurses are busy and looking after more patients aren’t they. But dad is vulnerable, and he needs the right level of personal care.
Patrik: Your Dad remains vulnerable no doubt. Getting the right level of care is very important and it sounds like some people, mainly the respiratory physician is taking more ownership now. The drop down in care form ICU is significant but it also sounds like he’s in a better environment now then he was, when he first went to the Rehabilitation Ward. Nothing will replace ICU care. That’s why I would look at his nursing care plan. That’ll give you an idea if the staff have a good grasp of your dad’s real care needs. I would be very happy to look at this. Keep talking to the senior matron and to more senior staff in general and keep voicing your concerns. Keep talking about the goals for your dad!
Many thanks Patrik for your help as ever.
Best wishes
Anna
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!