Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Your loved one in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions that we get quite frequently as part of my 1:1 consulting and advocacy service!
Can Doctors Push You to Take Family Member Off Life Support?
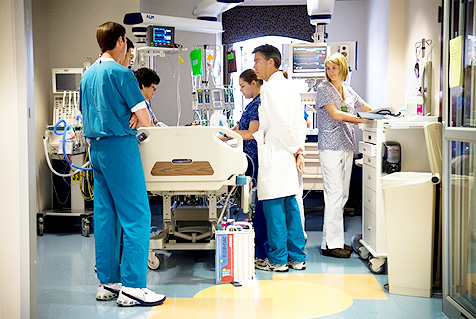
Having someone you love critically ill in the ICU is one of the things we most dread of. The part that we are most afraid of is when the doctor comes up and say “ You’re loved one is too critically ill that he or she will not be able to have a good quality of life so we need to stop life support”. After hearing those words from the doctor, what would you feel? How would you react? What decision will you make? Can doctors persistently push you to take your loved one off life support? The straight answer is no.
It is very overwhelming to make a health care decision for a loved one if being asked especially if they are in the course of being critical and can no longer make decisions on their own. It is even more difficult if you do not have a written or even verbal guidance or advanced care directive. In any case, if your loved one is critically ill, you as the family can discuss with the medical team which approach you want for your loved one. That way, decision making for crucial situations can be planned and get the kind of result as you wished and feel that your loved one would have wished for too.
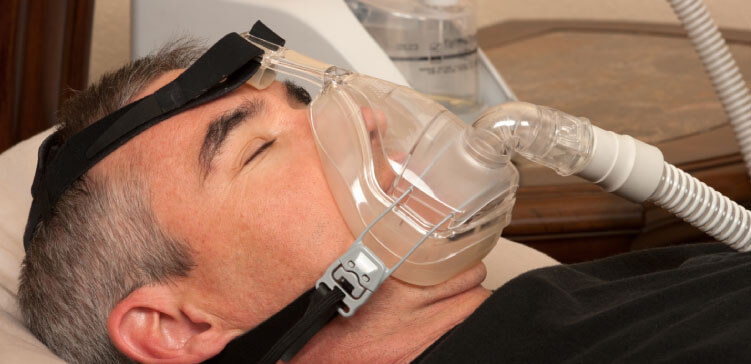
What does it mean to be on life support?
Life support is usually deployed as a short-term, temporary measure to buy sufficient time for your loved one to recover from a critical illness and be able to sustain life without help of life support devices.
There can be different forms of life support and all, multiple, or one of them may be deployed at one time, depending on your loved one’s needs. The best known life support device is a mechanical ventilation machine, which helps your loved one breathe when the lung is too sick to function on its own or when your loved one is in too deep coma to effectively breathe.
Other life support methods include certain drugs like the inotropes and vasopressors that may artificially keep the blood pressure elevated, keep it from dropping to zero or keep the heart pumping adequately. Even in some severe disease conditions, emergent hemodialysis (the usual form of kidney dialysis used to clean the blood of toxins) can be a sort of life support tool. Then there are more advanced and complex life support machines that bypass the lung and the heart and take over these organs’ core functions. This sort of life support device, known as Extracorporeal Membrane Oxygenation (ECMO).
There are many therapies and techniques that may be used by clinicians to achieve the goal of sustaining life. Some examples include:
- Mechanical ventilation
- Urinary catheterization
- Dialysis
- Cardiopulmonary resuscitation
- Defibrillation
- Artificial pacemaker
- Use of inotropes and vasopressors
Reasons Why the Medical Team Wants to Stop Life Support:
-
Life support may not be working
The medical doctors believe that your loved ones who are very sick do not respond to treatment. Despite powerful medicines, inotropes or vasopressors, and despite life support machines, your loved one may be getting sicker and sicker. Doctors and nurses caring for your loved one may recognize that there are no more life-saving treatments that can be tried.
-
Life support may not be able to save your loved one for long
Sometimes life support may be able to keep your loved one alive for a time, but cannot cure them of a very serious underlying condition. Your loved one’s health condition means that if they survive now it will only be for a relatively short time, perhaps weeks or months. For example, this might be because your loved one has a form of cancer that hasn’t responded to treatment, or it might be because their lungs are much damaged.
-
Treatment does more harm than good because of side effects
Medical team believes that life-saving treatments can have side effects. For example having a breathing tube in your mouth can be very uncomfortable, and can make people feel as if they are choking. Tests and procedures in the intensive care unit can mean many needles for a patient. If life-saving treatment would be very unpleasant for your loved one and would not bring a great benefit to them, it would sometimes not be the right thing to do for them.
Scenario: A patient has a chronic disease like of a terminal cancer that is becoming less responsive to treatment. It can also be a patient with any chronic ailment that cannot be cured, only treated, and the treatments are less effective and causing more harm and very unpleasant for the patient. Old age fits as well into this category. The physician usually start having conversations with the patient while the patient is still aware and alert enough to make decisions about their long-term care. This is where “living wills” and other documents come into play that describe how the patient wants to live until they die.
-
Life support is usually stopped when death is felt to be inevitable despite continued treatment
This would typically be when dysfunction in three or more organ systems persists or worsens despite active treatment or in cases such as multiple organ failure.
Stopping life support or withdrawal of treatment is an issue in intensive care medicine because it is now possible to maintain life for long periods without any hope of recovery. Intensive care is usually a process of supporting organ systems, but it does not necessarily offer a cure. Prolonging the process of dying is not in your loved one’s “best interest”, however, withdrawal of treatment does not equate with withdrawal of care. Care to ensure the comfort of a critically ill patient is as important as the preceding attempts to achieve cure.
Scenario: A patient had cardiac arrest, survives CPR but remains unconscious and lose the ability to breathe on his own. In this case, life-saving treatments are often continued until the patient shows improvement or meets the diagnosis of brain death. Unfortunately the patient remains unconscious, on a ventilator or, at the minimum, with a tracheostomy to maintain an airway, needing intervention to maintain bodily functions, and unable to respond to their environment. The physician initiates conversations with the family early on in this patient’s course about what life-prolonging measures they want their loved one to endure to treat the complications he is sure to have because they think these patients frequently have very little brain function left, but more measurable activity than would meet the criteria for brain death, but they have very little chance for any sort of meaningful recovery.
Reasons why you should refuse taking your loved one off life support:
-
Increase the chances of survival.
When your loved one is brain dead or no longer conscious, the decision to initiate life support falls on the hands of the surrogates (family or relatives). Most of the time, the decision to put someone on life support revolves around the idea that your loved one is given the chance to live longer or recover fully, which means that, denying them the treatment, would be equivalent to killing them.
The extended time frame that the life-sustaining treatment provides allows the family to have hope, come to terms with the traumatic event, accept the situation, and have more time to grieve. This also gives doctors a chance to continue to evaluate your loved one and provide newly discovered treatment if, there is any. There have been cases that your loved one fully recovers, after being put on life support. Nonetheless, the time given for the family to hope and for your loved one to survive is invaluable.
-
Grant patient’s wishes.
Some people who have written a living will usually specify their express wish to be allowed to fight every minute of their illness, regardless of the pain and suffering that they go through. Even when a similar request is given verbally, it is the surrogate’s duty to carry out a patient’s wish.
What do doctors mean when they say futile medical treatment?
Doctors may use the word ‘futile’ to describe treatment that they feel should not be provided because it is very unlikely to work.
Futile treatment means it is of no perceived benefit for a patient.
All medical treatment has a goal or an aim. For example, the goal of an antibiotic is to treat an infection. The goal of blood pressure tablets is to prevent your loved one from having heart problems or a stroke. There has to be a good reason to use medical treatment, otherwise doctors would not use it.
Sometimes doctors identify that a treatment can’t achieve its goal. The doctor will then usually decide not to provide that treatment. To use the same example, antibiotics do not have any effect on virus infections, only on bacteria. If the doctor is sure that your loved one does not have a bacterial infection there is no point in providing antibiotics. Antibiotics cannot cure a virus, they cannot achieve their goal of fixing the infection.
It is the same for life support treatment. The aim of life support treatment is to keep your loved one alive. The bigger aim is to help your loved one get through their illness, and back to as normal a life as possible. If it seems like life support treatment cannot actually keep your loved one alive, or cannot get them through their illness, doctors may feel that there is no point in providing that treatment.
There are different words that are used to describe treatment in this situation. Treatment might be called
- Futile
- Inappropriate
- Not beneficial
- Not indicated
The usual reason that doctors call treatment futile is because it is not working, or is not going to work. It is like a culture in the ICU where the doctors would be negative when it comes to the condition of your critically loved one, but despite all these, you can keep being positive by telling them straight what you really want for your loved one.
Management of perceived limited resources
The provision of critical care is complex, regardless of location. Interdisciplinary team-based care with high-technology monitoring and interventions will invariably generate high costs, including costs associated with capital equipment and consumables; salaries for nurses, other allied health personnel, and physicians; and health system costs for long-term survivors.
While you and your family are looking for the best therapy, care and treatment available for your loved one to maximize their chances of survival, the intensive care teams are looking at this situations that sets off their alarm bells as it relates to:
- Not wanting to spend too much money, staff and equipment resources to maximize their financial benefit
- Not wanting to deal with a family that is “difficult and demanding” and not wanting to invest too many emotions as well as efforts in dealing with you and your family
- Wanting to stay in control of the treatment, therapy and care options
- Wanting to stay in control of the positioning of your critically ill loved one’s diagnosis, prognosis as well as the care and treatment
- They also want to stay in control of the meaning of your critically ill loved one’s stay in Intensive Care
- Wanting to stay in control of who and for how long a critically ill Patient is occupying a precious, scarce, expensive and “in-demand” Intensive Care bed.
When is enough really enough? The principle behind withholding and withdrawal of life support states that treatment may not be initiated if your loved one or surrogate refuses. There have been cases, however, when physicians suggest for treatments to be withdrawn, but your loved one’s surrogates can strongly argue against it.
In general everywhere, your loved one can assign ‘Medical Power of Attorney’ to someone to make the choice if your loved one is critically ill and unable to make any decision. It is important of course to make sure that the medical team are aware of your and your loved one’s standards concerning ‘quality of life’, and that they need to respect these wishes.
Deleted: Intensive care professionals, mainly doctors, but sometimes also intensive care nurses like to imply that they operate in a vacuum and they can make life or death decisions at the drop of a hat.
Deleted: This is simply not accurate and they have to abide by the rules.
Deleted: The rules are that every intensive care unit has policies and procedures when it comes to withdrawal of treatment and withdrawal of life support.
The rules are that every intensive care unit has policies and procedures when it comes to withdrawal of treatment and withdrawal of life support.
This then also ties right in with the law. Nations, states and territories have laws when it comes to the removal or withdrawal of life support.
Those policies and procedures have documented that a patient or their medical power of attorney has to give consent in order to lawfully and legally remove life support.
Again, those laws usually non-ambiguously say that a patient or a medical power of attorney has to give consent before life support is removed or withdrawn.
Deleted: Again, end of life decisions can not be made in a vacuum, but most ICU teams want to make you believe so.
Deleted: Do your research and don’t let people walk all over you.Deleted:your research and don’t let people walk all over you.
We can help and support you to exercise your rights and we have case studies on our website how we have helped clients to save their loved ones lives by successfully advocating for them because we understand intensive care inside out and we understand patients and families rights!that every intensive care unit has policies and procedures when it comes to withdrawal of treatment and withdrawal of life support
| leted: |
REFERENCES:
-
Understanding Healthcare Decisions at the End of Life
https://www.nia.nih.gov/health/understanding-healthcare-decisions-end-life
-
How to Help a Loved One With End-of-Life Decisions
https://www.nextavenue.org/how-help-loved-one-end-life-decisions
-
List of 8 Main Pros and Cons of Life Support
https://connectusfund.org/list-of-8-main-pros-and-cons-of-life-support
-
Withdrawal of treatment
-
Stopping life support
https://www.rch.org.au/caringdecisions/chapters/Stopping_life_support/
-
What Does it Mean to be on Life Support?
https://www.orlandohealth.com/content-hub/what-does-it-mean-to-be-on-life-support
-
Life support
-
Global Health Care of the Critically Ill in Low-Resource Settings
https://www.atsjournals.org/doi/full/10.1513/AnnalsATS.201307-246OT
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Your loved one in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!