Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Why Is It Important for Us to Have Access to our Mom’s Medical Records in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tom, as part of my 1:1 consulting and advocacy service! Tom’s mom is on a ventilator in the ICU. Tom is asking how he will know if the ICU team is doing the right thing to help his mom come off the ventilator in ICU.
Is It Possible for my Mom to be Weaned Off the Tracheostomy in the ICU?
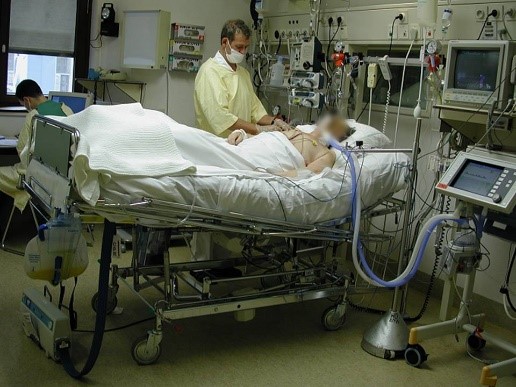
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tom here.”
Tom: Yeah. That’s, okay.
Patrik: And you might have to go slow with that, you may not want to overwhelm her. But it’s understandable that she’s got all these questions. And if there is something positive in there, her brain is working.
Ronald: Yeah.
Patrik: You know, a lot of patients-
RECOMMENDED:
Tom: Yeah.
Patrik: … a lot of patients come out of induced comas and they’re confused.
Tom: In addition, he did share with us on the charts that we brought her..
Ronald: We brought her like a communication pack. It has, like, questions, from… I’m sure you’re familiar with this. The hospital brought us one but it’s really small.
Tom: Way too small.
Ronald: We bought a big one for her, but, what were you going to say?
Tom: Well, we asked her, like we showed her pictures of stuff and asked her, “Is there anything here?”, or “How do you feel?” And right away she pointed to a picture where it said, “I’m sad.” And it was very emotional for us.
Patrik: Right. Of course.
Recommended:
Tom: And we explained to her the decision that I have to make for her, and after explaining to her I asked her, and I just straight asked her, “Are you mad, or you’re angry because I decided?” She said, “No,” she always says that, “No, no,” like, “It’s okay.” But, anyway, we recognized she wants to understand, and we did tell her quite a bit. But also we’re like, “Okay, how do we wrap up the last month?”
Patrik: Exactly.
Tom: Because she really is just starting to kind of recall information, so I had told her, “We have been telling you,” and this, and we just told her, “We understand that you don’t remember all of this, so we will continue to tell you a lot has happened and you fought very hard and you’re… It’s good, it’s a good thing. You know? You’re battled and you’re here, and let’s keep going.”
Tom: But we did explain to her about her being intubated, her being in a coma. You know, I mean, we went into some detail, but we explained to her, the alternative of staying intubated, doing an endotracheal tube we wouldn’t be able to communicate the way we are.
Patrik: Exactly.
Tom: … yeah, today and the process. And so we did try to highlight that, but we wanted her to be sure, to have some reassurance that we’ll continue to do that now that we understand, like, oh my gosh, there’s just so many things that we need to put into our frame of mind, talking and explaining to her, but letting her know that “It was a hard decision, but there was so many more benefits that… And the other situation was continuously risky and there might,” yeah.
Tom: We even told them, the doctor told him that at some point if she didn’t improve that they would withdraw, and she kind of raised her eyebrows. And then we were like, “Yeah, we don’t even want to get into that situation.” So with the need for the tracheostomy was going to get more tight, and it’s hard too, because she wants to know when it’s coming out already.
Recommended:
Tom: And so we’ve just told her, like, well I’ve explained to her that, “It is a semi-permanent procedure. Some people have it permanently,” but we’re hoping it’ll help supporting and just encouraging her recovery. And if she can come off of this tube, like, and hey, I don’t want to lie and say “It’s only temporary,” because I understand it is permanent for some people that… well, I guess.
Tom: But I also don’t want us to feel doomed, like it’s never going to come out, because it can.
Patrik: Yeah.
Tom: It can, it is possible she can wean off?
Patrik: Absolutely.
Tom: So, that’s hard.
Patrik: Absolutely. No, no, I think… I think you are doing the right thing there by gently educating her why she ended up in the situation that she’s in. I do believe that the more she understands, the more she can help with the process. They are, of course, very hard to digest news. It’s very hard to digest. But I do believe she needs to understand the situation, so she can work with you, she can work with the medical professionals.
Tom: Yeah. And we’re just reassuring her that we are with her through this trial, we’re going to be there, and she’s going to get through this.
Patrik: Absolutely.
Suggested links:
Tom: So, whatever time it takes, we are there. So I think that helps her to being reassured that, “Okay, they’re with me here.”
Patrik: Absolutely. You know, and also explain to her how much she has improved.
Tom: Yes.
Patrik: And.
Tom: Okay.
Patrik: … also, I have seen, we are talking to quite a few people at the moment that are in situations, and they’re not necessarily surviving. So, your wife pulling through this is showing that she’s got a strong will to live. I think that’s also important for you to remember, whether you’re going to share that with her or not, I can’t make that decision for you.
Patrik: But I am trying to put things in perspective for you.
Tom: Ah, yes, it is. And you know, I will just say too it’s so heartbreaking because we’re seeing patients rotate in and out of the rooms next door to her and, like, our worst thought is, like, “Oh my gosh, they die.” So it’s just like, this is just so… oh my gosh. I know it’s hard for everybody, everyone’s working, yeah, it’s just, this is wild.
Patrik: It’s very confronting.
Tom: Well.
Patrik: … you know, it’s very confronting for you, and for your family.
Ronald: Yeah.
Patrik: For us as health professionals, knowing intensive care, this is… And I’ve seen those situations, I don’t know, hundreds of times probably, you know?
Ronald: Hmm.
Tom: Yeah.
Ronald: Yeah. Well, I mean I guess at the very least my mom cannot actually see who’s in and out of the room. But hopefully that’s not occurring to her. But we’re..
Recommended:
Patrik: No.
Ronald: … seeing it and it’s just like, “Oh my gosh, just don’t even look.”
Patrik: Yeah. Yeah.
Ronald: It’s so bad.
Patrik: It is, it is very sad. But it could also be somebody has left because they might have been discharged to another floor, you know?
Ronald: To an LTAC? I know.
Patrik: Or to an LTAC.
Ronald: I’m sorry, I know.
Patrik: … that’s right, no.
Ronald: I did tell my dad, I spoke to him the other day. I said, “Dad, we hope nobody died!” And then yesterday I was like, “But I don’t know, what if they did?” And then, yeah, anyways, sorry, we’re kind of digressing. But thank you for your feedback on just encouraging her, because yeah, we’re definitely seeing that. We want to give her information, but I like how you phrased it too. Like when you just give it to her in pieces, then she is digestible too.
Patrik: Yes.
Ronald: And so we want to also, we’ve been trying to also just kind of give her a little bit of a clue, like, they might ask you later about if you want to move to a facility. And my dad, I told him, I was like, “I don’t want to alarm her, but tell her to say ‘No,'” because she doesn’t understand nothing about LTACs, she doesn’t have a clue about all this stuff that we’re learning about now that we’ve been working with you.
Ronald: Honestly, this is brand-new to us from the last two weeks ourselves.
Patrik: Yeah.
Ronald: But I told my dad, like, “Just tell her to say ‘No,'” and I wanted to ask you, if you, in your experience, do you recommend a spouse, like my dad, should he get power of attorney in this situation so he’s not pressured?
Patrik: Absolutely, yes. Absolutely, yes. I’ll tell you why.
Tom: Okay.
Ronald: Okay.
Patrik: I’ll tell you why. I have seen many situations, if the power of attorney situation is not clear, and the hospital thinks you might not decide what they want, they will try and grab power of attorney. I’ve seen that, I’ve seen it. Get clearance on that power of attorney situation, and make sure that either you, Ronald, or you, Tom, is the power of attorney. Absolutely, yes.
Ronald: Do..
Patrik: No, no.
Ronald: … you by any chance know where to start with that?
Patrik: I wouldn’t probably with a family lawyer or something like that. I’m not..
Suggested links:
Ronald: Oh.
Patrik: … I’m not a legal person, but probably something with a family lawyer. But I can tell you, make sure there is no ambiguity, that either of the two of you is medical power of attorney. Because that could get murky down the line if there are issues that need to be settled.
Ronald: Do you have any advice, not legal advice, this is more like on the patient side. But how do we tell my mom that without freaking her out?
Patrik: I see what you mean, I see what you mean..
Patrik: Yeah, that’s probably the tricky part. Do you have someone in your network whether family or friends, do you have, like, an attorney that you think you could ask or you could trust?
Ronald: To do what, though, to talk to her about it?
Patrik: Yes.
Ronald: No.
Patrik: No, okay.
Ronald: Well, we don’t either way.
Patrik: Yeah.
Ronald: but..
Patrik: Yeah, sure.
Ronald: … no.
Patrik: Sure. No, no, sure. Fair enough. I, because in a complex situation like that, and I understand she’s just digesting one step at the time what’s happened. But it’s a case of, if I was you I would get that power of attorney issue settled as quickly as possible. How do you explain that to her? Maybe in a way that if there were any setbacks, God forbid, if she had any setbacks and she can’t make her own decisions, who would she want there..
Ronald: Yeah.
Patrik: … to make decisions on her behalf? I think that’s probably the best way to frame it. Which is..
Ronald: Yeah, that’s true. Okay.
Patrik: … which is confrontational in and of itself. You know, you’re talking about setbacks, but I do believe, this is what we are talking about, really, if there are setbacks, who should make decisions?
Ronald: Okay. Thank you. Thank you. And I’m glad we asked. It did occur to me a couple days ago, this whole power of attorney thing. And yeah, we’ve never done something like this so we weren’t sure. So I will look into that..
Patrik: The hospital..
Patrik: … the hospital might use of her not having a medical power of attorney against you if they see an advantage in that.
Ronald: If they see the what?
RECOMMENDED:
Patrik: Yeah. If she doesn’t have a formal power of attorney. And the hospital might use that against you if they see leverage in that at some point.
Ronald: I’m not understanding the words..
Patrik: Yeah, so me too. Yeah, it’s a very unlikely scenario, but I have seen that unlikely scenario. So let’s just say it comes to a point where, God forbid, I’m really talking about the worst case scenario, but let’s just say your wife is deteriorating again, and they want to start talking about end of life again, and they say, “Look, we should be withdrawing life support here,” and you say “No,” and then they say, “Oh, but you’re not the medical power of attorney,”
Patrik: So, then you might go and try and get that, but the hospital might also try and get it. Because the hospital might say, by you prolonging her life might not be in her best interest, because they might say she’s suffering, they might say that. So, I’m really pointing out the worst case scenario here, but I have seen it.
Ronald: Hmm, okay. I see. Understand. Got it. And no need to, we get it. You have any questions about that, dad? I know it’s hard for him because he doesn’t want my mom to feel like there’s something ill intended. I don’t think she would, but again, it’s like, it’s alarming that..
Patrik: Yeah.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!