Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
My Mom is in ICU and Can’t Come Off the Ventilator. Is Tracheostomy the Next Best Step For Her?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tom, as part of my 1:1 consulting and advocacy service! Tom’s mom is with a breathing tube and is on a ventilator. Tom is asking how they will know that it’s time to do a tracheostomy for their critically ill mom in the ICU.
How Do We Know If it’s Time to Do a Tracheostomy for our Critically Ill Mom in the ICU?
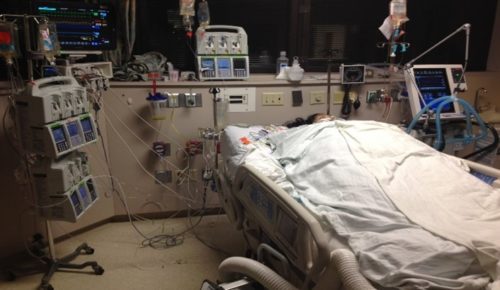
Tom: So they kind of made it seem like don’t worry, as long as she’s on that, she’s here. But then because we understand at some point, the whole thing is she’s not going to need that, but then it’s good news, bad news. Good news, she doesn’t need it, bad news, she can’t stay in an acute facility like a hospital. But we did ask them. We said, “Is there any option? Is there anything that we could do?” And we did try to say like, “We’re concerned about her medical vulnerability to leave. We would like it to be known that we want her to stay in the hospital, even if it’s not in the ICU.”
RECOMMENDED:
- Membership for families in Intensive Care
- Book your free consultation call here
- Check out our Ebooks and videos
Patrik: Correct.
Tom: And they didn’t give a definitive answer today, but they just kept kind of explaining, “Well, if she doesn’t require acute care, that’s really not what hospitals are for. She would able … ” And we were like, “Hmm. Okay, we’ll get there.” We kind of left it at that. Not agree or disagreeing, but they’re aware that that’s a concern of ours because going this route.
Patrik: Good, good. The other thing that may happen, and you know, that’s information that are missing at the moment. Depending on what ventilator settings she’s on, it could be as simple as, they’re doing the tracheostomy, they’re lowering sedation and she can tolerate that. And she may come off the ventilator reasonably quickly, but I don’t know that at the moment. Because the quicker she can come off the ventilator, the higher chances you can avoid LTAC all together.
Patrik: But we wouldn’t have that information at the moment. If they are suggesting LTAC, I would imagine that her ventilation support is still very high at the moment.
Tom: Yeah, and what would you measure high? Just generally speaking, like the PEEP (positive end expiratory pressure) and the O2 saturation level.
Patrik: PEEP.
Tom: … the tidal volume?
Patrik: All of it. PEEP, the general setting whether she’s doing some of the work herself, whether she’s triggering some breaths herself. The pressure support. FiO2 (fraction of inspired oxygen), tidal volume, all of it. Plus her arterial blood gases. Plus her chest X-rays. Plus the sedation is also important. What is she on? Do you know what sedation she’s on?
Recommended:
Tom: Yes, she is on Precedex.
Patrik: Okay.
Tom: I may be, hopefully I’m not confusing this with the pain medication. Is that a sedation medication, Precedex?
Patrik: It’s both. It’s a sedative and pain medication. Precedex is a combination of both.
Tom: Okay, so she is on Precedex. She’s on Dilaudid for pain killers that I do remember. And she’s on propofol. And they took her off of Versed, which we know is really strong and long-acting. But they took her off propofol during the week when they stopped proning her. And so far, they haven’t need to recontinue Versed, but their goal has been to continuously reduce propofol, but they haven’t been able to take her completely off propofol because she has been agitated, she has been stressed. She’s really agitated, anxious during the episodes of trying to wake her up.
Tom: Not so much recently, but last week there was … They ended up having to restrain her hands.
Patrik: Oh, my goodness. No wonder she’s anxious. No wonder. I mean, that’s terrible.
Tom: Yeah, so those were to two sedation medications, and then I mentioned the painkillers.
Patrik: Yeah, how long has she been on Precedex for?
Tom: Precedex, from what I can recall, is the newest one in this combination, because I remember Versed and propofol being like the names they were telling us every day when we were asking for updates. So I would estimate Precedex like within the last five days.
Patrik: Five days.
Tom: Somewhere in that, five. Four, to let’s say, Monday. Yeah, I would say maybe within the last four or five days, they may have transitioned to Precedex. We can get a definitive answer if that helps direct your..
Suggested links:
Patrik: No. It would help. The more information, the better. I guess the reason I’m asking is simply if someone is on Precedex, the whole purpose of Precedex is to stop propofol and stop Versed. That is the whole purpose of Precedex. In my practice, it looks like it very rarely happens. Precedex initially came on the market to reduce or eliminate propofol and Versed, but that hasn’t really happened in practice as far as I can see.
Patrik: Anyway, that is what Precedex should be used for, but if she’s still on propofol, they might as well stop the Precedex.
Tom: Oh, I see.
Patrik: That’s how I see it. Do you know how much propofol she’s getting? Have you got a number?
Tom: Right now, I don’t know of the top of my head.
Patrik: That’s all right.
Tom: But my dad is going in. Well, we are going on to visit her shortly, so I can take note of that.
Patrik: And you are mentioning they’ve done a CT scan of the brain to rule out any neurological deficits?
Tom: Yes.
Recommended:
Patrik: Right, that’s good. That’s good.
Tom: They did that two days ago.
Patrik: Okay, good.
Tom: And it came back normal.
Patrik: Good. That’s good. Okay. Quick other questions, the kidneys are working? She’s not needing dialysis?
Tom: Is dialysis the same as insulin? Is it insulin?
Patrik: No, no. Dialysis is a dialysis machine. She’s not in kidney failure?
Tom: No, okay, she’s not. No. She’s not.
Patrik: Good.
Tom: They did tell us generally the function, but they didn’t explain to us that was something they’re monitoring closely because of the antibiotics that she was getting. But no, that’s fine. They did a bladder ultrasound today. I thought that’s what they were doing this morning. On her bladder and it seemed normal, although the, what is it called, radiologist had not totally approved it, but the ultrasound technician generally said everything looks fine, but wait until the final results come through.
Tom: So that was fine. And they did something else in her like gallbladder. Gallstones. They checked her for gallstones yesterday. I don’t know the outcome of that yet. But for the most part, organs are functioning okay. No failure. Her heart is okay, it’s good, but it starts to spike up really high when she’s agitated and weaning. So that’s been part of the equation of not weaning so quickly is her heart rate goes up really high and her blood pressure goes up really high.
Suggested links:
Patrik: Yeah, okay. So from what you are sharing with me, I recommend the following steps. It would be great if I knew the exact ventilator settings. It would be good understand what other medications she’s on. It would be good to see an arterial blood gas. And once I’ve got that, then I can probably advise you should you go for a tracheostomy or not. It sounds to me like a tracheostomy is possibly the next best course of action. And then it will come down to us advocating to keep her there for as long as possible and not go to LTAC.
Patrik: Again, if she could stay where she is, I would say let’s do a trach. The challenge is going to LTAC. That, I see, is the biggest challenge.
Tom: Yeah, okay. I will get that then for you today.
Patrik: That would be good.
Tom: And I can send you that information in an email, if that works okay for you.
Patrik: Yeah, absolutely.
Tom: Okay, thank you so much. I will say the doctors, it’s possible they would like an answer from my dad tomorrow at the latest.
Patrik: Sure, right.
Tom: Tomorrow at the latest so they can stop the blood thinner medication to prepare her for the surgery. So, I mean we do have that option, although they said, “If you know today, let us know.”
Patrik: Of course, of course.
Tom: But, yeah, so we’re comfortable waiting till tomorrow.
Suggested links:
Patrik: And if you were to give consent today, would they do it tomorrow? Have they given you timelines there?
Tom: What they explained to us is they would need to stop anti- I mean, excuse me, and blood thinner medication and anti-coagulation something. I believe its 24 hours. So with that said, even if we consented today, I don’t think they would do it tomorrow or not until tomorrow late. And the doctor also said that he would need to ensure that he had ample time to do the surgery. And I said, “What do you mean.” He’s like, “Well, if we get a whole bunch of new patients in the next day or two, I need to be able to block out sufficient time to work on her.” And I was like, “Okay.” I didn’t even think of that.
Patrik: Right. Is this a surgeon, a general surgeon you’re talking to?
Tom: No, he is a pulmonologist, I think, intensivist doctor in the ICU.
Patrik: Yeah, that’s why I’m asking because most tracheostomies nowadays get done in ICU. They’re not even going to the operating room. They just do it at the bedside. It’s actually a fairly quick procedure nowadays. Like 20 years ago, patients went to the operating room and it was sort of a fairly complex procedure, whereas now, they just do it at the bedside.
Tom: Yeah, he did explain that to us. He didn’t actually mention that, but he just said he needed to be uninterrupted for at least 30, 40 minutes. Yeah, that’s what he meant. Like, “If I have a lot of new patients, I may not even be able to do that.” He said right now is a good time because everyone that’s admitted has been cared enough. Sadly, all brand new patients. Like, everyone has their current condition. I don’t know. I don’t know if everyone’s stable.
RECOMMENDED:
Tom: But anyways, that was part of him saying, “As soon as you can tell me, the better.” But we’re fine waiting till tomorrow. That’s good because that’ll give us time to get some updates today. And then we’ll just go from there. So I know that, just so that we can kind of understand how to work around your services, Patrik, I can email you that information.
Patrik: Please.
Tom: … on how should we follow up on another phone call?
Patrik: Look, just send me the information and I’ll reach out to you.
Tom: Okay. Well, I know that we made payment today.
Patrik: Yes, I saw that, thank you.
Tom: Of course, thank you for letting us know that route. But would we continue with that current payment for the remaining 30 minutes or how is that going to pan out?
Patrik: Oh, yeah, absolutely. Whatever. That works for me.
Tom: Okay. Got it. Well, no. Thank you for this time. This helps us put a lot of perspective and get more input of we’re going along. So yeah, thank you, we’re glad that we found you. Just like many others. So thank you for your services and your help and your expertise.
Patrik: Oh, pleasure, pleasure. I’m here to help.
Tom: Okay, Patrik, we’ll be in touch with you then, okay?
Patrik: Okay, thank you so much.
Tom: We’re down at the hospital now.
Patrik: Yeah, thank you so much.
Tom: All right, take care.
Patrik: Thank you, bye.
Tom: Bye-bye.
Patrik: Bye.
Tom: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!