Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Mom is in ICU with a Tracheostomy. Is it Safe For My Mom If She Ends up in LTAC?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Tom as part of my 1:1 consulting and advocacy service! Tom’s mom is ventilated in ICU. Tom is asking why it is risky to transfer his ventilated mom from ICU to LTAC.
Why is it Risky to Transfer My Ventilated Mom from ICU To LTAC?
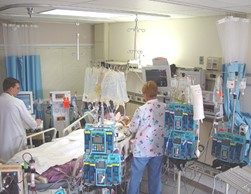
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tom here.”
Tom: Yes. The facility he really promoted is about 30 miles away from our home, from my parents’ home, a little further than I would like, but the next location after that is about 50. However, the discharge nurse describes that their location that’s about 30 miles away. We’ll call that the closest location..is one of the few that takes trach patients and ventilator patients, so some of the further ones either took trachs but not ventilator or something of that variation, so he really was like, “This place takes her condition. This place takes her insurance. They have space. We should refer now before they’re out of space,” talking on it. What the heck is all this pressure? I actually had a hard time keeping myself composed during that. I was really frustrated with him the other day.
Patrik: Sure, sure
Tom: Yeah, it was yesterday. I forgot. As I outlined in the email I sent you this morning, I said to him, “What are our other options?” His immediate answer was, “Well, what do you suggest instead?” I said, “Sir, I’m asking you to explain this. Can you lay out what other things we can choose from? You’re not even telling us if there’s another option that our insurance covers. I understand private pay is going to be extremely expensive, but I don’t even know if this is naïve of me to ask, but can you ballpark it? What is that?” I don’t know. We’re really not in a position to pay private pay, but at least tell me what does that option look like because you’re saying LTAC. He’s not saying it’s the only option, but he’s posing and framing it as it’s the best option. It sounds like it’s the only option, until I pushed back. He did tell us, though, that the hospital inpatient rehab facility would not take a ventilator. They will take tracheostomy patients but not ventilated tracheostomy patients.
Patrik: Right. Okay.
RECOMMENDED:
Tom: So it seemed like that was taken out of the picture because the doctor in the ICU has been charting my mom as a long-term ventilator need, meaning there’s no need to refer to the inpatient place because she won’t be off by the time they transfer her.
Patrik: Yeah, I see how they’re framing it. Yeah, sure. Are they telling you that she needs to be at LTAC by next Sunday? Are they giving you any timelines? What’s the line of communication there?
Tom: No, they haven’t.
Patrik: No, they’re not.
Tom: I was wondering that, too. That’s what I told my dad. I can’t tell with this timeline how much has elapsed because they’re not giving us any firm idea other than it’s starting to feel a little more rushed, but I will say, my mom has continued to have more bleeding. You know how I was telling you yesterday that they gave her a blood transfusion?
Patrik: Yeah.
Tom: So her bleeding, we wanted to share this with you, too, but I think that’s a good point in the conversation to just mention her bleeding has continued, and they conducted a blood stool check, and they ruled out that she doesn’t have any coming from her stool. They ruled out that her PEG tube was clear, and she had no gastrointestinal bleeding. They addressed her tracheostomy bleeding, so it’s no longer that’s not the source, but she’s still going on a downward trend on the hemodynamic thing you were asking me about. I saw the doctors notate that today that she’s had a downward trend and they don’t know the source of the bleeding right now, so that was really alarming to me today. I spoke to my dad about it because he went to visit and I couldn’t. I just said, “I don’t understand what that means and how critical is that. Is that going to prolong her stay until they figure it out?” Gee, I would like to know where the bleeding is from, too.
Patrik: Absolutely. You see here is the other thing, and I can’t remember whether we spoke about this, Tom, yesterday. It’s not the only reason, but one of the reasons why I’m so opposed to LTAC, and again, I can’t change the system, but I can point out what I’ve learned over the years, right? Your wife is in such a vulnerable position. She’s probably never been more vulnerable than she is now. That would be fair to say, wouldn’t it?
Dad: Yes.
Tom: Yes, definitely.
Patrik: Right, so to move a critically ill patient to another facility in such a vulnerable position where she’s going to need a new team, I hate to say it. To me, that’s almost like a criminal offence. She’s now got a team that knows her, right? Transferring someone within a hospital, let’s just say going from intensive care to a step-down ICU, for example, that in and of itself has risks attached to it. Let alone, transferring her half an hour down the road to a new team, right?
Tom: Yeah.
Patrik: I mean, you see the irony of that. Chances are that if she deteriorates, she’ll end up in ICU again anyway, and there is no guarantee. If she needs ICU again once she’s in LTAC, there’s no guarantee she will go back to the same ICU. She might go to the ICU that’s closest to the LTAC, i.e. she will be in three different places within weeks in such a vulnerable condition.
Tom: Absolutely, and the LTAC that they’re referring or recommending, they are right next to another hospital. It’s considered a different county line, but that’s where she would go. She wouldn’t be going back to where she’s at right now.
Patrik: Exactly. Right.
Tom: We know. We figured that out once we looked it up, so that’s a great point.
Patrik: So, you can see the risks that are attached with a transfer.
Tom: Yes, absolutely. I just felt like I hit a brick wall with the discharge nurse because he did say-
Patrik: Oh, for sure.
Tom: … “ICU is for acute care, and she’s not going to need acute care at some point, and we can’t just keep her in there to aid her to do this.” Then I asked about a step-down unit or a ward, if there was any inpatient rehab, and he didn’t say no. He was just like, “A hospital is for acute care. She’s not going to need that at some point. We can’t just keep her here.” I’m like, “What if?” I don’t get it.
Patrik: Yeah, no. You can see. You can now understand why I’m saying what I’m saying. The risks attached to a transfer are very high, and you’ve got to weigh up whether you want to take the risk of sending her to an LTAC or whether you want to continue advocating for her in this place. The reason why you experience all this pressure is simply the hospitals only see that choice for them. That’s why you are experiencing this pressure because the system is designed for a one-size-fits-all.
Recommended:
Tom: Yeah, but what happens, Patrik, because I told him, and that’s when I told my dad. “We’re done talking with this man.” I said, “No. You may not refer us. We’re not ready, and I want to go back to visit my mom because visiting hours are almost over,” so I excused myself from the conversation. I mean, that’s not my normal demeanor, but he was really pushing on us. Again, aside from I thought it was inappropriate that he interrupted our visiting times since that’s limited too, but what happens when we say because we all told him we’ll get back to him as we discuss this more.
Patrik: Yeah, good.
Tom: But I said, “No. You do not have our permission to refer us,” so technically he can’t, right? I’m curious.
Patrik: No, no. He can’t, and you will need to give consent to what you want to do going forward. They would probably tell you at some point, if they haven’t done that already. They will probably tell you at some point that whoever the insurance is will only pay for 60 days ICU or something like that, but my argument on that level is unless the insurance is contacting you directly, I wouldn’t worry about it. If the insurance comes to you directly-
Tom: Okay. Yeah, I remember you told me that yesterday. If they’re not contacting you, it’s okay, but I wanted to ask you. Is it problematic if we reach out to them? I told you about that yesterday, and my dad, we were just talking about this last week. I said, “We should call and get an update on what they’re covering,” but we were just too overwhelmed, and we didn’t get to it last week, but is there harm in us initiating that call or do you recommend sitting back and waiting for them to contact my dad?
Patrik: I wouldn’t worry about it at the moment, if I was you. I wouldn’t worry about it. They would contact you if that’s an issue.
Tom: An issue meaning they won’t cover beyond-
Patrik: Correct.
Tom: Because they already told him they’ll cover. Oh, no. They do cover 42 days.58 days? Yeah, that is covered in 60 days.
Patrik: That’s right.
Tom: They already said they’ll cover 58 days so we’re not there yet, so actually may I ask you? Gosh. Maybe that was obvious, and I didn’t even put it in perspective yesterday. Is that our timeline right now is 58 days or just technically we’re entitled is it 58 days that they’ll pay?
Patrik: That is my experience generally speaking. There are some small differences from insurance to insurance but from my experience, whatever insurance, it’s usually all capped at 60 days, roughly speaking. However, if someone still needs ICU after 60 days, it’s not that people will cut off that lifeline. That’s not my experience. Where it might get grey, it might get grey if ICU thinks they have the evidence that she needs to go to LTAC and you’re opposing that, but again, my argument on that end is everything in life is negotiable. That’s number one, and number two, I believe there is overwhelming evidence that patients in LTAC do not get better and are stuck either in LTAC or even worse, eventually get transferred to a skilled nursing facility.
Tom: As like a step-down care, lower care?
Patrik: Very much so. That’s right, so-
Tom: Okay. That’s not higher level.
Patrik: No, no. It’s going from bad to worse sort of thing.
Tom: Yeah, okay.
Patrik: I am not trying to be negative here. I’m just educating you about the system.
Tom: I appreciate it.
Patrik: I’m not trying to be negative here or paint a bleak picture, but you need to be aware of the environment you’re dealing with.
Suggested Links:
Tom: Definitely. I don’t mind, believe me. On my watch, I am willing to push keeping her in a hospital setting because I recognize now that that level of care is a lot more. It’s a much higher quality than standard care. I get that now, but where I am now feeling knowledgeable or confident and my dad either is when we say, “Excuse me. No, we don’t want that,” I don’t even know if we’re allowed to say so. I guess yes, we are allowed to say it, but it even seems scary for me being a very articulate question-probing person. I’m trying to say no. I just said no. Can I do that here? They don’t present the information in a way that really helps us feel empowered through this process.
Patrik: No, of course not. Of course not. Well, I’ll give you the answer. If you think you can, you can. If you think you can’t, you can’t.
Tom: I know. It’s mindset. I know. I guess when I say can I, I just don’t know what the alternative is.
Patrik: Yeah. No, no.
Tom: Can I force them to keep her in the hospital?
Patrik: Look, look. There are some case studies that we published where we helped families achieve exactly that. We helped them to stay in ICU for as long as possible because if there is progress, as long as there is progress, your argument will get stronger to keep her where she is. Let’s just say he would make rapid progress of weaning off the ventilator. You could say, “Okay. Well, a few more days. Then she will be off the ventilator completely, no need for LTAC.” Right, but what I can see at the moment, she’s far away from being removed from the ventilator. That’s part of the problem.
Suggested Links:
Tom: Yeah. I understand.
Patrik: It’s a tricky situation. There’s no question about that, but now you’ve got an idea about the environment. Now you’ve got an understanding of what needs to happen to get someone off the ventilator, (A) reduce the support from the ventilator, but it needs to be supported by activities.
Tom: Yeah. I understand. I don’t know how to, where to bring those requests when they say, “Well, we do it based on how she’s looking. She really didn’t have much energy,” so I mean, I take that as true when they say that but should we be saying, “No. Still try just a little more?” I don’t know.
Patrik: Yeah. I’ll make an analogy here that I think might be helpful. If someone wants to run a marathon, they’re not going to run a marathon by sitting on the couch or sitting on the sofa. I have not seen someone being successfully weaned off the ventilator without training really, and in that instance, it’s physical therapy. It’s not going to happen without it.
Tom: Yeah. I know it did increase a bit the last four days.
Patrik: Great.
RECOMMENDED:
Tom: Yesterday was like 1 hour, and I think today was like 2 hours.
Patrik: Oh, good.
The 1:1 consulting session will continue in next week’s episode
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!