Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tom, as part of my 1:1 consulting and advocacy service! Tom’s mom is on a breathing machine. Tom is asking why it is important for them to have access to their mom’s medical records in the ICU.
Why Is It Important for Us to Have Access to our Mom’s Medical Records in the ICU?
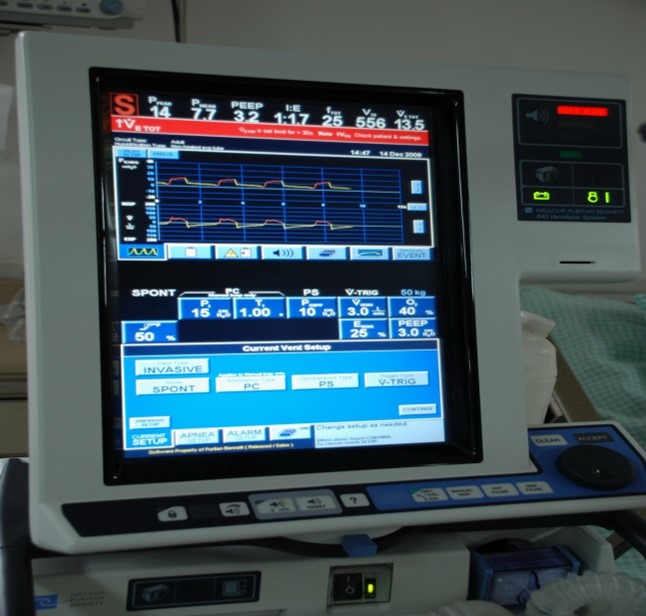
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tom here.”
Ronald: Okay, I imagine that changes her vulnerability then.
Patrik: Very, very much. So it changes her level of vulnerability. It changes, it helps with your argument that she needs to stay in ICU.
Ronald: Oh, my God.
Patrik: Right?
Ronald: Okay.
Patrik: So, that’s why it’s so important that you have access to this medical report. The other thing that’s evident from the report is her liver function is off a little bit.
Ronald: Okay.
RECOMMENDED:
Patrik: Right? And nobody knows why, it’s probably a combination of her being on all sorts of medications over the last few weeks, that’s often one of the reasons why patients have their liver function is off. So-
Ronald: But that can’t be exactly proven, so we can kind of use that to hang our hat on-
Patrik: Well, I-
Ronald: Is there another risk factor?
Patrik: … I’ll tell you two things. Let’s just quickly stick with the heart attack for now.
Ronald: Okay.
Patrik: Has a cardiologist spoken to you?
Ronald: No? No.
Patrik: Right. If I was you, I would want to talk to a cardiologist and find out more. That’s number one.
Ronald: Okay.
Patrik: With the liver function being off, I would also want to talk to a specialist there. Right? ICUs are very good at saving lives, ICUs are very good at saving lives as you can see. But they’re not so good at breaking things down when it comes to a heart attack. Well a heart attack is a specialist area. So is the-
Ronald: Yeah.
Patrik: … so is the liver. You know?
Ronald: Okay.
Patrik: So, there are already arguments that will help you, I believe, to keep her where she is. Now, there was another thing I just quickly need to bring it up from today’s report. Just give me a second, I just need to scroll all the way down.
Ronald: You’re fine.
Patrik: Yes, yes. Did you see, when you look at the report from today, have a look on page 2, number 13. Can you see that-
Ronald: Gastrointestinal bleed.
Patrik: “Query gastrointestinal bleed? Hemorrhoidal bleeding noted-
Ronald: Yes.
Patrik: … after hemorrhoid removal. However, hemoglobin hematocrit stable and no obvious bleed on esophagogastroduodenoscopy on the 11th. Repeat hemo called negative.” Okay, that’s all good. When they say “query gastrointestinal bleed,’ I mean, was there really a gastrointestinal bleed at some point? I mean, you would want to know whether they have more information around that.
Ronald: Okay.
Patrik: But it also makes sense that if there was a query gastrointestinal bleed, and that they put in an IV filter. You know, it makes sense.
Ronald: Because if the gastrointestinal tract is bleeding there’s more risk for clotting, is that?
Patrik: No, no, not at-
Ronald: Or-
Patrik: … all, not at all. The gastrointestinal bleed might… the gastrointestinal bleed in ICU is often a result of it’s a combination of stress, right? And also of anticoagulation, heparin, for example. So, patients in ICU, one of the stress responses is to develop stress ulcers, gastric ulcers, right? And if there’s a gastric ulcer because of stress, that could cause a gastrointestinal bleed.
Patrik: And on top of that, patients are anti-coagulated. So that combination could often lead to a gastrointestinal bleed, which then again makes sense to reduce anticoagulation such as heparin or Lovenox, and put an IV filter in. Make sense?
Ronald: Oh okay. Well I guess I’m just trying to understand though the IV filter is only to a limited location in her body, so if she’s at risk of developing clots elsewhere, I understand that that filter’s only, like, protecting her leg, and that’s exactly where it’s at. Is that-
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
Patrik: Yeah-
Ronald: … am I misunderstanding?
Patrik: … yeah, no, no, no, you are right. However, the reason it’s sitting low, is most clots develop in the leg. Okay?
Ronald: Hm.
Patrik: And then they travel upwards. Okay? If a clot forms in the leg, the risk is that it travels to the heart, to the brain, or any other vital organ. Right? And-
Ronald: Okay.
Patrik: … even if a clot is developed, it’s not travelling into dangerous places. The filter will stop that.
Ronald: Oh, okay. Okay.
Patrik: Right?
Ronald: Okay.
Patrik: So that’s the purpose of that. Okay? But I see so much progress.
Ronald: Yeah.
Patrik: I mean, that is-
Ronald: Can you reiterate though what the question is that we could be posing regarding number 13? I’m trying to conceptualize what you just said, so-
Patrik: Oh, yeah, it says “query gastrointestinal bleed.” Okay, well, if I was you I would want to know, was there a gastrointestinal bleed or was it not? What does that statement mean?
Ronald: Oh… okay. So just, okay. Okay, thank you for just bringing that down to that, so I wrote it down that gastrointestinal bleed.
Patrik: Yeah. You know you want to know, do you want to find out, was it or wasn’t it? So, and I can’t tell you how pleased I am to hear that she’s mobilizing and that she has some CPAP trials, even though it’s on a lot of support. I think that’s… she has come such a long way, that that is fantastic. The most important thing that I can see now is they need to keep doing that.
Ronald: Yeah.
Patrik: They need to keep doing that.
Ronald: Yes. Do you have any tips, suggestions, if I… So, with us being there present with her, like, even yesterday was like, “Oh my gosh, should we be stimulating her?” We were playing music, we were kind of talking to her a bit, and we were also like, “We don’t know if we’re being helpful or annoying her?” We don’t know, like, how to encourage her to focus the mental, psychological preparation of, like, she can do this, it’s always for an hour. Do you have any advice on that end, of like, how we could support? Because they seem-
Patrik: Yeah.
Ronald: … to be… it seems like they’re going to continue breaking it up, and the respiratory therapist yesterday and today was like, “I like doing it with you guys are here for company,” you know?
Patrik: Yeah.
Ronald: Because I always hear them all going, like, “I can’t believe they’re going to forget about me over here.”
Patrik: Yeah, absolutely. Look, if you were telling me, “She’s only doing 15 minutes on CPAP,” I would still see that as progress, you know? All I can say on this note, every little step is progress. It’s baby steps in those situations. Right? So-
Ronald: Yeah.
Patrik: … and it’ll be hard for her to see those baby steps, she’s stuck in this difficult situation of course. But all I can say is keep encouraging her, and try and explain to her how far she’s come even within a week.
Recommended:
Ronald: Okay.
Patrik: It’ll be very difficult for you, but also for her to put things in perspective, because you haven’t seen this before.
Ronald: That’s very true. Very true, very grounding explanation and reminding us of that big deal, yes. That is very true. It all just feels like a shock still.
Patrik: Mm-hmm (affirmative).
Ronald: You know? And it’s like, that’s very true. Thank you. Okay.
Patrik: There’s no-
Ronald: Because-
Patrik: … there’s no quick fix in this situation. Right? There’s no quick fix. However, a week ago, I was very worried that she would be in an LTAC within a few days, and that it would all go pear-shaped from there. Whereas now, I believe she’s still in the right environment, right? And they’re doing the right things when it comes to weaning. And that is the risk with LTAC.
Patrik: She would go to LTAC, and the level of care would, any progress she’s making now I believe would just be lost in no time.
Tom: Yeah. Well, thank you for just your education and awareness that you’re raising about refusing that or at least delaying that. So we really, we’re trying to prepare ourselves to grapple with declining it completely. Now that we understand that’s in our right, honestly, four weeks ago before we knew you, I felt like, “They say we have to go, we have to go.”
Patrik: Sure.
Tom: Like no, now it’s like, “Oh no, actually I found out we don’t have to leave.” If this is where my dad wanted her to be in, and then we’re not convincing.
Patrik: Yeah. Exactly. Exactly. And your argument, I do believe that your argument strengthens with every day that she’s making progress.
Tom: Yeah.
Patrik: You know, it’s like-
Suggested Links:
Tom: And one other question-
Patrik: Please.
Tom: … dad, go ahead, dad.
Ronald: Patrik, I wanted just to ask you how much for, I don’t know how to really phrase this question, but so she’s asking questions. Like her first question I want to say five days ago or six was, “What happened?”
Patrik: Sure.
Ronald: And then she, like today we found a note that she’s trying to write. It was very emotional for us today. She wrote on a note, a clipboard that we asked for and it’s been in her room. She just said, “Was this option the only option for me?”
Patrik: Right.
Tom: And-
Patrik: Mm-hmm (affirmative).
Tom: … we believe that she’s talking about her tracheostomy.
Patrik: Yeah..
Tom: That is heartbreaking for us to read that and know that she’s grappling with that thought, and not understanding. And so what was your question, dad?
Ronald: My question, I mean… I mean, we don’t want to lie to her. We want to be honest, but I mean, how much can we tell her, or where should we draw the line?
Tom: Yeah, where do we start, where do we draw the line so we’re not stressing her out more.
Patrik: Yes. Yes. Yes. It’s a very good question, and I do believe that the more she understands it, the more you explain to her why she needed the tracheostomy, the better it is. I do believe that honesty is the best policy in this situation. And no one, unless you’re a medical profession, no one thinks about, “Oh, what do I need to do if I go into ICU next week or if my family member goes into ICU next week?”
Patrik: Nobody thinks that way, of course not. You know, and it’s so overwhelming of course, once you’re faced with a situation like that. That those questions that you’re asking are very relevant, how much do we share? But I do believe in order for her to sort of embark on the weaning process, I do believe the more she understands, the better it is.
Suggested Links:
Tom: Yeah. That’s, okay.
Patrik: And you might have to go slow with that, you may not want to overwhelm her. But it’s understandable that she’s got all these questions. And if there is something positive in there, her brain is working.
RECOMMENDED:
Ronald: Yeah.
Patrik: You know, a lot of patients-
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!







