Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Loved ones in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions that we get quite frequently as part of my 1:1 consulting and advocacy service!
How to Provide Better Intensive Care for Your Loved One?

An intensive care unit (ICU), also known as an intensive therapy unit or intensive treatment unit (ITU) or critical care unit (CCU), is a special department of a hospital or health care facility that provides intensive treatment medicine.
Intensive care units cater to patients with severe or life-threatening illnesses and injuries, which require constant care, close supervision from life support equipment and medication in order to ensure normal bodily functions. They are staffed by highly trained physicians, nurses and respiratory therapists who specialize in caring for critically ill patients.
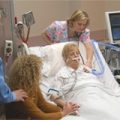
If your loved one has been admitted to the intensive care unit of a hospital, this means that his or her illness is serious enough to require the most careful degree of medical monitoring and the highest level of medical care.
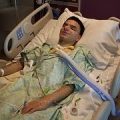
Critically ill patients in intensive care often endure invasive, life-saving technologies and procedures. They may have periods of semi-consciousness and confusion. They may be frightened.
Once discharged from the ICU, memories of the experience may invade the daily lives and long night hours of people who thought they had survived their crisis. It is a form of post-traumatic stress disorder (PTSD).
Most of us associate PTSD with soldiers returning from war. But intensive care patients have been added to ranks of those who are prone to the after effects of trauma. Post-ICU syndrome is real and, as are all other conditions that thrive in the memory, it is not consistently responsive to medication. So the question now is, how to provide better intensive care for your loved one?
Designing the ICU Experience
The environment experienced by patients in the ICU is often limited to the boundaries of their sensory system: what they touch, taste, smell, hear, and see. And, sometimes this is further limited to only what they hear.
It’s important to design the ICU experience to minimize trauma and mitigate negative experiences. Here are ways to create more positive and better experiences for ICU patients:
- Provide Positive Distractions
Positive distraction can be defined as, “an environment feature that elicits positive feelings and holds attention without taxing or stressing the individual, thereby blocking worrisome thoughts.” Positive distractions can be provided to your loved ones through music, humor, films, or relaxation programming for healthcare settings especially for patients who are semi-conscious or intubated that can reduce anxiety, alleviate pain, assist with sleep and restfulness, and minimizes the effects of hospital noise.
- Conduct Intentional Interactions
The Intensive Care Unit (ICU) is intended for your loved ones who are recovering from severe medical complications, surgery, traumatic injuries and critical illness. In most instances, your loved ones in intensive care unit are unstable and their conditions are life threatening. Outcomes for your loved ones in Intensive Care Units can vary widely, and ICU nurses play a significant role in those results.
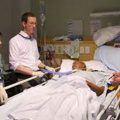
As a result, your loved ones require continuous care and monitoring by skilled nurses who understand the special needs of the ICU patient. An ICU nurse’s responsibilities include assessing a patient’s needs, making sure the patient has adequate medication, nutrition, and hygiene, and even keeping the patient’s spirits high by demonstrating a positive attitude and conducting intentional interactions.
This means being purposeful, focused, and fully present for your loved one and family. Touching the patient’s hands, having eye contact when possible, and being engaged with the whole person, not merely his/her medication, vitals, and symptoms.
By carrying out these responsibilities, the nurse may ensure that your loved one in the ICU feels comfortable and secure so that he or she can begin the journey toward healing.
It is easy to understand that a busy nurse or aid, lab tech, or housekeeper just needs to do their job. However, they can almost forget your loved one in ICU. In ICU, paying attention to your loved one, noticing signs of distress and fear, and minimizing environmental stressors can lower the risk of PSTD once your loved ones leave the ICU.
- Be Sensitive to Noise
Noise is the number one irritant to a highly acute patient and, as well, to their family. Eliciting the startle response, for example, results in both physiological and psychological reactions: increased blood pressure, heightened heart rate, fear, and anxiety.
Florence Nightingale wrote, “Any sound that creates anticipation, expectation, or fear of surprise is that which damages the patient.” Close the door (if appropriate), quiet other patients and visitors and staff. Lower the volume of monitors (if appropriate).
Again, be sensitive to the television and the sounds that go directly to the patient’s ears. News stories about war, bombings, mass shootings, political rants, even dramas with people yelling at each other are not appropriate and can put the patient at risk. ICU Delirium is real, partially an outcome of confusion caused by a chaotic environment.
- Do Continual Environmental Assessments and Interventions
Walk into the room with heightened awareness of everything that impacts the patient and family members. Since four of the five senses are the connection to the environment, look at what the patient is looking at, listen to what he/she hears, be aware of what touches the patient, and how the room smells. Remove unnecessary clutter. Make sure the bathroom is clean.
- Consistently Provide Basic Nursing Care
Never underestimate the importance of basic nursing care. Nursing is seen as “patient-centred”, individualized to the holistic needs of each person and dependent upon an understanding of what their priorities were.
Basic nursing care such as regular washes, pressure area care, back washes, showers even for ventilated patients in a shower trolley, mouth care, eye care, oral care and also mobilization is something that positively influences good outcomes for your loved ones.
One option that promises better intensive care for your loved one is the INTENSIVE CARE AT HOME which is an alternative home health service provider, with the goal of providing Quality of Life and/ or Quality-of-end-of life, for ventilated Adults & Children with Tracheostomy and their Families with currently no perceived alternative, but to stay in Intensive Care indefinitely, to stay in Intensive Care for long periods of time or worse- face treatment limitations, due to a Patient requiring long- term invasive and mechanical ventilation with Tracheostomy.
INTENSIVE CARE AT HOME is a genuine alternative to a long-term stay in Intensive Care that gives your loved ones better intensive care right straight into the comfort of your homes, taking into consideration the total well-being of your loved one for their full recovery and prevent them from getting undesirable experiences brought about by the ICU hospital environment.
You can go and check out intensivecareathome.com for more information about the service.
REFERENCES:
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!