Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Is the ICU Team Reasonable For Not Recommending ECMO For my Wife with ARDS in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I am here with a live stream today, where I want to answer your questions if you have a loved one in intensive care. And this is one of the most commonly asked questions for families in intensive care and it’s a question that we get all time. And today’s live stream is about how long does it take to die after a breathing tube is removed?
How long does it take to die after a breathing tube is removed? Live stream!
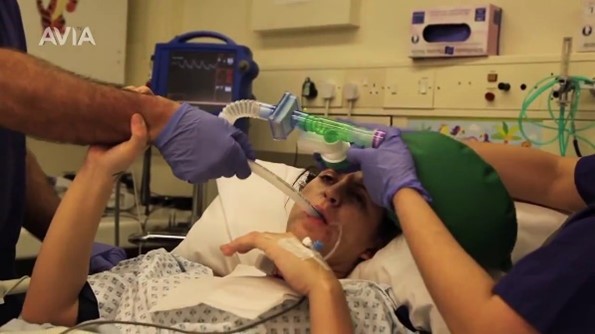
Good afternoon, wherever you are. It’s Patrik Hutzel here from intensivecarehotline.com with another live stream for families in intensive care. So everybody that has a loved one in the intensive care should subscribe to my YouTube channel, should subscribe to our website, email newsletter at intensivecarehotline.com. You can also check out intensivecareathome.com, where we provide an alternative to a long-term stay in intensive care for long-term intensive care patients.
Today’s topic is around how long does it take to die after the removal of a breathing tube? And we’ll discuss this here in our live stream today.
Just very quickly about myself. What makes me qualified to talk about this topic? I am an intensive care nurse by background. I have worked in intensive care for over 20 years in three different countries. I have done post-graduate critical care studies. I have worked as a nurse unit manager for over five years, and now I am a professional consultant and advocate for families in intensive care. I consult and advocate for families in intensive care all around the world. So I have a very good in-depth understanding of intensive care, but really I’m also an expert on family and patient rights in intensive care. I have a very good understanding of what families in intensive care want to know. And I also have a good understanding in which environment they feel safe to ask the questions they want to know, because I don’t believe that many families in intensive care ask the ICU doctors, how long does it take to die after the removal of a breathing tube? I’ll tell you in a minute why I think that’s the case.
RECOMMENDED:
Before I dive deeper into this topic, I want you to subscribe to my YouTube channel. I want you to like the video and I want you also to comment and type your questions in the chat pad so I can I answer your questions as we go along. But even if you watch this video when it’s not live, I encourage you to type your questions in so I can respond to them.
What I’ve learned after having worked in intensive care for 20 years is that very few families actually ask that very question: How long does it take to die after the removal of a breathing tube? But what I then learned after I started my website, intensivecarehotline.com, I actually realized a lot of families are asking that very question, but I’ve never heard it in ICU, which was telling me that as I always knew, families in intensive care are intimidated. They don’t see eye to eye with the intensive care team. They’re intimidated by asking questions. They’re intimidated by asking the wrong questions. They’re intimidated by feeling ridiculed by asking questions.
Once I realized that with Intensive Care Hotline, I was actually creating a safe space for families in intensive care where we don’t judge. We just make sure that families have their questions answered. And that’s the most important thing really, that you can answer the questions you want to have answers to. And a lot of ICU teams in particular, don’t want to see with you eye to eye. They feel like they’re superior to you, and they feel like they can just make life or death decisions as they please. And nothing could be further from the truth, but I’ll come to all of that in a minute.
First off, it will possibly shock you when I say to you, as much as you want the answer, how long does it take to die after a breathing tube is removed, especially if it’s for a palliative care/end-of-life situation? The first myth that I need to bust here is, it’s one of the worst questions that you can even ask in the first place because it’s basically implying that your loved one is going to die in intensive care. It’s the wrong question to ask.
Now, I understand you are curious about the answer. And I will come to the answer, but it’s such a wrong question to ask. Why is it the wrong question to ask? 90% of intensive care patients survive. That’s 9 out of 10 intensive care patients survive intensive care. They will leave intensive care alive. So the odds are actually in your loved one’s favor. So why would you even go down that track of: why would you remove the breathing tube for an end-of-life situation? Why would you do that? Well, that’s what the intensive care team wants. We know that.
Suggested links:
Intensive care team wants to empty beds. They don’t want to deal with long-term critical illness. They don’t want to deal with potentially critical illness that leads to a disability with all the flow-on-effects, what you do with patients once they leave intensive care because they just can’t see it. They’re just not mentally equipped to look at long-term outcomes because they feel like if we can’t get a patient back to where they were before they entered ICU, it’s a futile exercise, but that’s not what this is all about. It’s about saving lives. It’s about making sure that patients and families wishes are respected, irrespective of what it looks like down the line. And this is one of the purposes of this video today; to educate you about. As much as I will get to the answer, you’ve got to look at so many other facets before you have this question answered.
Let’s just quickly look at the answer of this question. How long does it take to die if someone has the breathing tube removed for potentially end-of-life situation, because they’re deemed to have a non-survivable injury? If it is really non-survivable and you take out the breathing tube, well, and you don’t intervene medically, it could take minutes. It could take hours. It could take days. It could take weeks.
Here is the crux though and here is what is happening in intensive care in the first place. When patients have the breathing tube removed for a withdrawal of treatment, the reality is it’s not as simple as just taking the breathing tube out. It’s a case of taking the breathing tube out and giving additional sedative such as midazolam/Versed, such as extra propofol, such as opiates, such as fentanyl or morphine. And those drugs are given in high doses to aid the dying process.
Let me repeat that. Once the breathing tube is removed for an end-of-life situation or for a palliative care situation, there’s no guarantee that death is going to occur. It can take minutes. It can take hours. It can take days. It can take weeks. However, the reality in intensive care is this. I have not seen an end-of-life situation where a “one-way extubation” is performed, meaning the breathing tube is being removed without an intention of putting it back in, where additional medications such as strong sedatives such as midazolam/Versed, propofol, and the combination of morphine or fentanyl, strong painkillers, are given.
I make a deliberate pause here because what does that mean? So if you’re removing the breathing tube, and somebody should be breathing spontaneously, and you’re giving sedatives such as morphine, fentanyl, midazolam, propofol, you are in essence inducing death, you are hastening death. The official definition of hastening death is euthanasia. So removing the breathing tube for a one-way extubation, with no intention to put the breathing tube back in, and giving midazolam, propofol, strong sedatives, plus morphine or fentanyl, strong opiates, strong painkillers, that is hastening death and its euthanasia and euthanasia is illegal. Euthanasia is illegal.
Wherever you are in this world, watching this video, whether you are in the United States, whether you’re in Canada, whether you’re in Australia, in the United Kingdom, South Africa, Ireland, I don’t care where you are. Look up your laws in your country and you will find that euthanasia is illegal. No intensive care unit will ever talk about euthanasia, but it’s happening every single day, all over the world. Every single day. And I’ve been involved in euthanasia, not proud to say it. I was too junior at the time to realize what was actually happening, to realize that I was actually involved in euthanasia in intensive care multiple times. It only dawned on me as time was going on as I was able to look behind the scenes and when I was realizing what was actually really happening in intensive care.
I do remember the last patient that I was involved with, where we did a one-way extubation with no intention to put the breathing tube back in, was a 46-year-old gentleman, very fit gentleman. He was running triathlons and whatnot, and he got injured. He got a knee arthroscopy. And after the knee arthroscopy, he had a thrombosis that ended up with a pulmonary embolus and he had a massive heart attack. He was basically deemed to be end-of-life, and we were actually doing a one-way extubation. He was a fit, strong man at 45, 46 years of age. He was a big guy. We’re taking the breathing tube out and we were giving morphine and midazolam to help him die, which is terrible. In retrospect, it’s terrible, and I’m not proud of it at all. I remember he needed truckloads of sedatives and opiates because he was not ready to die and he died anyway, because we were basically giving him so many sedatives that we didn’t give him a chance to breathe. But this is what’s actually happening in intensive care every day, all over the world and it’s shocking.
Recommended:
So that is why this very question is not the right question to ask. Your question needs to be not, how long does it take to die after the removal of a breathing tube? Your question should be, can my loved one survive intensive care? What are the options besides a one-way extubation? Is a tracheostomy an option? And often it is. Often a tracheostomy is an option. There are some contraindications and there could be times when a tracheostomy is getting delayed. Of course, every treatment in ICU comes with side effects. It’s a very difficult situation. Whether you decide to have the breathing tube removed and have your loved one die, or whether you decide to go down the track of a tracheostomy, it all has consequences one way or another, and you may or may not like the consequences, but the reality is this. After your loved one is dead, there’s no return from that. There’s no return from that. There’s no coming back from death. So think about this.
Asking this very question means that you have already bought into the intensive care team mindset. The intensive care team wants to empty beds because there’s so much demand. They want to save money and they want to be in control; who lives and who dies. And by you asking that very question, you’re already buying into the mindset of the intensive care team. It shows me you haven’t done your research. It shows me you’re taking everything they’re telling you for face value. It tells me that you haven’t understood that by them wanting to do a “one-way extubation”, you don’t want to fight for your loved one. You’ve already given up.
The worst thing here is also that when it comes to these one-way extubations, often being done after 2, 3, 4 or 5, 6, 7 days in ICU, which is not a long time. Your loved one barely had a chance to recover and the ICU team already is talking about hastening death. And you’re already buying into this mindset of, “Oh, your loved one won’t have any quality of life down the line. So let’s just cut it short here and let them die because that’s in their ‘best interest.'” Well, since when is death the best interest of a patient? Since when? Tell me.
There have also been many situations where the breathing tube has been taken out without the added-on sedation that I talked about earlier, but also without the intent of ever putting the breathing tube back in and patients die, but they die within hours, days, weeks, sometimes months. So I also need to stress there’s absolutely no guarantee that just because you’re taking the breathing tube out and the intensive care team has more or less condemned your loved one to die, there’s no guarantee that they will die. This is why I’m also saying the intensive care team is very quick at always painting the doom and gloom picture and always being negative. For what? Why?
Suggested links:
They’re being negative because they need to manage their downside. Because if they were telling you, “Oh, we take the breathing tube out and then your loved one will walk out of intensive care,” and they’re not walking out of intensive care, well, you could be suing them for misleading you. So you always have to read between the lines. Always. You always have to read between in lines. No matter what is being said in intensive care, you always have to read between the lines. That’s the biggest challenge for families in intensive care. They don’t know what they don’t know. They don’t know what to look for. They don’t know what questions to ask. They don’t know their rights and they don’t know how to manage doctors and nurses in intensive care. That’s your biggest challenge.
You have no idea how to steer the territory that is intensive care. That’s why I’m here and that’s why I and my team are here to help you getting outcomes, getting results because the intensive care team, more often than not, will push your loved one over the brink, especially if they have a very critical illness or sickness that could keep them on a ventilator for a long time to come. That could keep them on life support for a long time to come. The intensive care team will push towards end of life because their worst-case scenario is to look after a patient indefinitely with an uncertain outcome. That is their worst-case scenario because they have so many other patients needing an ICU bed. You need to understand the dynamics in intensive care.
Other criteria when it comes to what I consider one-way extubation without intent of having the breathing tube removed is, most of the times when I’ve seen it is simply after a few days. And that is way too premature, way too premature. You should be at least waiting until day 7, 10, or even day 14, because that is the cutoff when someone should have a tracheostomy, if they can’t be weaned off the ventilator. And then the question really comes down to, do you want a tracheostomy or do you want to have the breathing tube removed without intent to have the breathing tube being put back in? Basically a re-intubation. Because only then can you really make a judgment what the right steps is? The number of times that I’ve seen breathing tubes coming out after just a couple of days or after 3 days or after 4 days, it’s just ridiculous. And at that stage, I didn’t know any better. Now I know better, and you need to know better too, because you are really in a life or death situation. You are. If you get this wrong, your loved one will die, and there’s no return from that. There’s no return from that.
You also should be calling out the intensive care team about performing euthanasia. I don’t know why if while you’re watching this. Are you a religious person? I guess for any religious person, euthanasia is out the question, but even for non-religious, even for atheists, I believe that euthanasia is unlawful. It’s a criminal act. Even for an atheist, I do believe that even atheist doesn’t want to hasten death.
Recommended:
The other thing is this, that if you wanted to go down the track of a one-way extubation and if you wanted to go down the track of palliative care and potentially end-of-life, you should also be looking at services like Intensive Care at Home, and you can find out more at intensivecareathome.com. Why is this important? Now, there are number of times when I’ve seen one-way extubations in intensive care where families said, “Oh, it would be so much nicer to do this at home.” I couldn’t agree more with that. Who wants to die in intensive care if death is inevitable? Tell me, who wants to die in a sterile, non-family friendly intensive care unit? That’s where services like Intensive Care at Home come in. We have done one-way extubations at home with Intensive Care at Home. We have. And that was at the family’s wishes.
We know now, we have established that intensive care units want to have their beds empty as quickly as possible so they can take the next patient in. And by doing a one-way extubation at home, it’s also a win for the intensive care unit because they’ve got an empty bed and resources are being transferred to a home care environment. Again, it’s a win-win situation. There are situations where death is inevitable, but I argue a lot of one-way extubations are ending up in euthanasia. And again, I can’t stress this enough, it’s illegal and it’s hastening death.
I’m curious to know what your questions are around this topic. I’m curious to know whether you have any questions so far. I’m curious to know whether you agree, curious to know whether you disagree with what I’m saying. Do you have any experience with having a loved one in intensive care where you have been challenged with a situation like this and what did you do?
Suggested links:
Other issues that I need to bring up and that I want to discuss around the removal of the breathing tube/one-way extubation is simply many families in the intensive care come to us and they say, “Oh, tomorrow at one o’clock, we want to take out the breathing tube for your loved one because it’s in their ‘best interest’ and they won’t have any quality of life down the line.” If you are confronted with the situation like that, well, I can tell you if you are agreeing to that, and I’m sorry to be so blunt, and I’m sorry to challenge you on this. It’s your own fault, because you don’t know about patient and family rights. You have every right to stop that. Most families don’t believe it. Most families do not believe that they have rights. They take everything the intensive care team is telling for face value.
Helene, you have a question, you’re saying: “Also excessive fluid overloaded that could be on the lungs, that needs to be drained out of the lungs that could be the issue that prevented my late mother from breathing.” Yeah, for sure. If your mother had fluids on the lungs, that is definitely a… Let’s put it that way. Anybody that is on a ventilator in intensive care should have the lungs as dry as possible. The lungs should be as dry as possible, whether you do that with fluid restrictions, whether you do that with diuretics, such as Lasix to increase urine output, whether you do it with hemodialysis/ hemofilter. But the bottom line is this. It’ll be very difficult for anyone coming off a ventilator if their lungs are fluid overloaded. That’s the bottom line.
There is this approach in intensive care where you always want to have someone with a negative fluid balance, especially if the goal is to wean them off a ventilator. A negative fluid balance, which means more fluid is going out than coming in, a negative fluid balance will help a patient to come off the ventilator. It’s as simple as that.
Coming back to patient’s rights. We have been involved in many situations here at Intensive Care Hotline where we’ve been asked to intervene in situations like I just described, where family comes to us and says, “Hey, tomorrow at one o’clock we’ve been told we are removing the breathing tube. The intensive care team is going to remove the breathing tube for my loved one and they’re probably going to die. What do we do?”
Recommended:
It’s good for those families to reach out to us because we put a stop to that almost immediately. And we are not legal people. We’re not lawyers or solicitors or attorneys, but we are specialized in patients and families rights. I can almost guarantee you that if you come to us with a situation like that, that we can put a stop to that within hours, because we just remind the intensive care teams of the legalities and that if they did that, it’s actually murder.
It’s very strange where the world has come to in terms of intensive care units claiming that, “Oh, if we take out the breathing tube tomorrow at one o’clock and this patient is going to die, it’s in their best interest.” That’s like someone being executed and the judge saying, “Oh, well, it’s in their best interest to die.” I’m gobsmacked by just intensive care units telling that to families. Where intensive care units are lacking is looking outside of intensive care. If someone survives intensive care, what does their life look like 6 months down the line, 6 years down the line if that’s possible? But even if people only live for a few more months, who am I to judge how they should live, where should they live?
With services like Intensive Care at Home now, people can prolong their lives at home on life support. And their quality of life is much better than being stuck in ICU long term. Of course the debate is out there; whether they have a good quality of life. Well, I believe they do have a good, good quality of life and their families want them at home. They want to be at home surrounded by their loved ones for whatever time they’ve got left.
Suggested links:
So there’s enough food for thought, as you can see, to move away from that initial question that was the live stream today: How long does it take to die after removing the breathing tube? It’s the wrong question to ask. It is the very wrong question to ask in the first place. Yes, there is an answer to this question, but that question shouldn’t be asked in the first place.
There are some situations where the removal of the breathing tube is the only option, for example, if someone is brain dead, but even that can be up for debate. Where do people stand on a spiritual, religious, cultural level if someone is declared at brain dead by the medical faculties? Does that mean they’re brain dead on a religious, spiritual, cultural level? That is not for me to answer, but you can see that we are opening a can of worms here just by looking at this question.
Helene, you’re saying, “I advocated for my mom to live. Pulmonary team and hospitalist ganged up on me. They threatened, harassed and bullied me.” Yeah, no surprises there, Helene. No surprises there. I argue that if you had worked with me at the time when this happened, I would’ve been able to put a stop to all of this. We’ve done this many times. We have a proven track record, but I understand this was the past and I understand you’re still grieving. I understand that at that stage, maybe I didn’t have the website yet. You didn’t know where to go to seek help. But I do understand that it’s a very difficult situation for many families. I also understand that most families are intimidated by the intensive care team.
Intensive care teams are very good at pretending they’re operating in a vacuum and they can just make life or death decisions at the drop of a hat. They can just make life or death decisions without consulting anyone. They’re very good at that. And most families buy into that mindset and it’s terrible. It’s terrible. Self-history, for sure, but you can’t buy into the intensive care team’s mindset. If anything, the intensive care team has a duty of care to you, to your loved one. And it’s not duty of care to tell you the only way is to remove the breathing tube and let your loved one die.
The other issue is this. If the intensive care team comes to you and your family after 3 days of ICU, they’re saying, “Oh, we need to remove the breathing tube because it’s in your loved one’s ‘best interest’ to have them die by removing the breathing tube.” I mean, how can you not question their motives? You have to question their motives. There is no return from death as far as we know, as in 2021. There is no return from death. So you got to ask the questions. You can’t take things for face value. What you see is not what you get. Your loved one’s life is in somebody else’s hand. You have to question. I hope that helps. I hope that helps.
Helene you’re asking, “Does removing the breathing tube mean the same as…” Yeah, it’s almost a synonym. It’s almost the synonym, however, there’s probably more to that. So when someone is having the breathing tube removed for a one-way extubation with no intent of having the breathing tube put back in, often patients in ICU are also on inotropes or vasopressors, which is also considered life support. So if you are stopping both mechanical ventilation and other mechanisms of life support that is what is generally being referred to as “pulling the plug”. Yes, it is. But it depends a little bit on what is the exact situation of a critically ill patient?
Lot of patients where a one-way extubation is being suggested are often on inotropes/vasopressors, because as soon as you stop the inotropes and vasopressors, blood pressure drops to a level that is not compatible with life, plus you then remove ventilation. It’s almost certain that people are dying with the aid of the sedation and the morphine and the midazolam and the fentanyl that I discussed earlier. There’s a few ingredients in that “death recipe”, if you like. There’s a few ingredients in there.
RECOMMENDED:
All I can say is if you are watching this and you need help in this situation, what I will say, you need to pick up the phone, you need to go to intensivecarehotline.com. You need to ring us on one of the numbers on the top of the website immediately.
And that’ll be another topic at some point, but what often goes hand in hand is also brain death testing, but I will do another video just about brain death and brain death testing. It ties right in with this topic, but we will do that in a separate live stream to talk about brain death and brain death testing and what you need to look for if you are finding yourself in a situation like this.
No, Helene, brain death is not the same than encephalopathy. Encephalopathy, as far as I am aware, can lead to brain death, but it’s definitely not the same. That’s also something I want to hone in in a future video; that brain death is not the same than brain damage. It’s not the same. Its two different things, but I do want to again, do a different video live stream just on that topic in the next few weeks.
Thank you again for watching. Check out intensivecarehotline.com. Send us an email to [email protected], or call me on one of the numbers on the top of the website.
Subscribe to my YouTube channel, like this video, and I’m looking forward to more comments and questions. I’ll see you again next Saturday night, 8:00 PM Eastern Standard Time; 5:00 PM Pacific Time; 10:00 AM Sydney, Melbourne time on the Sunday.
Take care for now and thank you for joining me on this call. Take care.
This is Patrik Hutzel from intensivecarehotline.com and I will talk to you in a few days.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!