Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question in this series of questions from my client Melissa and the question last week was PART 6 of
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“. I want to answer the next question in this series of questions from one of my clients Melissa, which are excerpts from phone and email counselling and consulting sessions with me and the question this week is
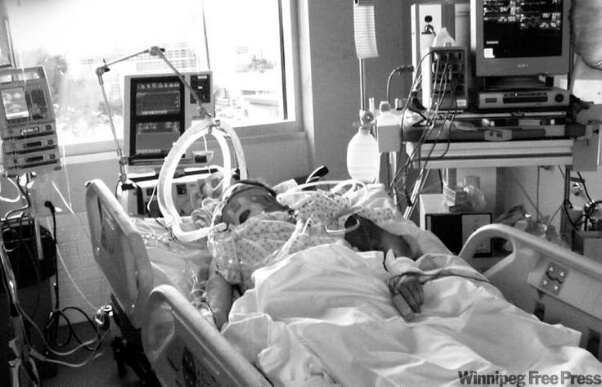
My 78 year old Mom has lung cancer and developed an infection! She’s in ICU on the breathing tube, can she get off it or will she need a tracheostomy? (PART 7)
Previous questions answered from Melissa, you can find here
PART 1, PART 2, PART 3, PART 4, PART 5 and PART 6
After I started counselling and consulting Melissa earlier this year, her Mom eventually left Hospital after going from ICU to LTAC and then home eventually.
A few months later her Mom presented back to Hospital and got readmitted back to ICU because of the lung cancer having come back.
The ICU team is adamant that Melissa’s Mom hasn’t got much time left and that she will die very soon in the next few days. They have suggested hospice and Melissa is having second thoughts about what else could be done.
Read the dialogue below so you can see how I can steer the conversation in a direction to help Melissa to come to terms with the situation and how she can make sure that she looks at the situation from many ankles so that she can actually do what’s best for her Mom!
The reality is that when Patients die in Intensive Care, the sooner you can embrace the inevitable and the sooner you are in a position to talk to your loved one about it, the sooner you can make peace with the situation as is showcased below!
This consulting dialogue is more about bereavement counselling and helping a client to come to terms with what’s actually happening.
Patrik: How’s your day been? It must have been very stressful the last few days?
Melissa: Oh, God. It’s yeah I’m sure you hear it all the time but …
Patrik: Oh, every day. Every day. So you’ve had a really rough, probably last few months even?
Melissa: Yeah, yeah. You talked to us once before and we …
Patrik: That’s right.
Melissa: Yeah, we advocated for her and she was able to breathe on her own. But as I said in my email, I really don’t know what to do next. We met with Hospice today, I got your email unfortunately, but I got it after I’d already met with them. So we went in quite early today.
Patrik: Right, right.
Melissa: Earlier than we had planned, and they were very nice but they believe in natural. And in the meantime, we saw her CT scan, we saw the fluid in her lungs Patrik and I mean I’ve gone over your website but I can’t remember every situation.
Patrik: Of course.
Melissa: In my Mom’s situation, her left lung is gone. That’s the one with the tumour, it’s completely filled with fluid. They took out a litre a couple of days ago. It filled right up, I mean they can’t keep taking it out. They’re using a needle, they are afraid they’re going to puncture the lung. Meanwhile, now the other lung is starting to fill too. So she’s losing the use of both lungs.
Patrik: I see.
Melissa: And it’s getting to the point where the only way to keep her alive is with the oxygen mask, which she has on now, or intubation and the breathing machine. Everyone is telling me they don’t want to do the breathing machine.
Patrik: Yeah and I know why…
Melissa: Even my dad now does not want to do, my dad is having a harder time with this than me, but everyone knows someone who says it’s very painful for them. And then her caregiver told me that she had a conversation with my mom early this morning and my mom is at peace and ready to go.
Patrik: Okay, that’s important. That’s important though.
Melissa: But Hospice also wants to take her off the oxygen mask and just put something in her nose that’s …
Patrik: Yeah, yeah.
Melissa: And I said okay and now I’m having second thoughts on that. But they’re saying that they can’t use the oxygen mask forever. I was thinking well what if they could use it for the next six months, maybe we could keep her until Christmas.
Patrik: Yeah, yeah.
Melissa: They looked at me like I was crazy, and they were very nice.
Patrik: Sure.
Melissa: They said it doesn’t work like that.
Patrik: Yeah.
Melissa: She’s getting worse each day and I don’t know, I mean I realise that I am paying you and you may not have an answer for me. What I want is a miracle and I don’t think you can offer it.
Patrik: And look, it depends if I’ve got an answer for you. And the answer could be I’m doing a lot of bereavement counselling, too. I don’t know whether that’s what you need, but let me ask you a few questions.
Melissa: Okay.
Patrik: And the reason I’m talking about bereavement counselling is look, I’ve worked in Intensive Care for 20 years. I’ve seen so many people die Melissa over the years, and that’s full on. I have my own peace with end of life situations for a number of reasons because I’ve been exposed to it almost on a day-by-day basis. I’m exposed to it almost on a day-by-day basis with what I’m doing here with my INTENSIVECAREHOTLINE.COM 1:1 counselling and consulting. So I do believe I can help you with some strategies to either prolong your mother’s life or to help you come to terms with what’s happening. Either or, I believe I can help you with either or. But before we go into that, let’s just clarify a few more things that I need to clarify in my head to get clear on the exact situation. So I know your mother went into the long term acute care facility, she got off the tracheostomy. Was she ever home?
Melissa: Oh yeah, she came home.
Patrik: Okay.
Melissa: But she wasn’t home that long.
Patrik: Okay, when did she go back to hospital?
Melissa: She’s been in there pretty much since January on and off, but she went in a month ago for foot surgery.
Patrik: Oh my goodness.
Melissa: She had no pulse on the bottom of one of her feet. She’s had surgery on that before and …
Patrik: Just adding onto the long list of worries.
Melissa: Yeah, she had gangrene building up. They had to amputate two toes.
Patrik: Oh my goodness.
Melissa: And they put it in I guess it’s like an angioplasty. They put a thing in her foot and she was supposed to come home the next day. And then she caught C. Diff. again, and then she caught pneumonia, and then she got a bone infection, and then she went into respiratory failure and while treating her for that, they did an x-ray and they saw that the tumour had metastasized in a very short amount of time. She’s had this tumour for probably close to ten years, but it was the size of a dime when it was first diagnosed.
Patrik: How long ago was the next chest x-ray where they saw that the tumour has come back, how long ago was that?
Melissa: You mean where it’s metastasized?
Patrik: Yeah, where it’s metastasized yes. How long ago?
Melissa: I think that was last week sometime, about a week ago or a little more.
Patrik: Okay so all relatively recent, relatively recent?
Melissa: Yeah, oh very recent, yeah.
Patrik: Okay, okay so this all happened really in the last week?
Melissa: Yeah.
Patrik: Okay now I was what’s … Okay, so then basically …
Melissa: She went in for the surgery, like I said I think it was about a month or more.
Patrik: Okay.
Melissa: But the stuff with the fluid around the lungs happened in the last week.
Patrik: Okay, and did she go into ICU then after they found all of that?
Melissa: Well she was in surgical ICU anyway.
Patrik: Okay.
Melissa: And they moved her from surgical to medical.
Patrik: Yeah, okay. So then they put her on the breathing tube to begin with but then they took out and now she’s on oxygen. Is that accurate?
Melissa: I don’t know if she was on the breathing tube at all. I think they drained the fluid somehow.
Patrik: Okay, yep.
Melissa: think she might have been on the breathing tube just at night when she slept.
Patrik: Okay, with a mask? With a mask probably.
Melissa: She has a mask now. At first she didn’t, but she’s gone very downhill in the last few days.
Patrik: Sure. And she has … Sorry, she has initially the breathing tube down her throat, do you remember?
Recommended:
Melissa: Yes. I think so, yeah.
Patrik: Okay, all right. So your mother seems then, would she have periods of where she was awake?
Melissa: Oh yeah, she still does.
Patrik: Okay. Can you have a conversation with her? Can she tell you what she wants?
Melissa: don’t know. I was there today we said things like she whispers through the mask. I said I love you, she said I love you. I said you’re my best friend, she said you’re my best friend. But we haven’t said the doctors are saying you have a couple of days left do you want to go, what do you want … I mean I don’t think anybody’s said that to her.
Patrik: Mm-hmm (affirmative) Have you said it to her?
Melissa: I haven’t, no.
Patrik: Okay, that’s fine. That’s fine. I do believe the best way in those situations is to be honest with people and I do believe that nobody has a crystal ball, the doctors don’t have a crystal ball, you don’t have a crystal ball, I don’t have crystal ball. I find time frames extremely difficult to predict in end of life situations, or in perceived end of life situations. We don’t know whether it’s real, whether it’s perceived, we don’t know that. However, I do find that by you spelling it out, if you can, if you can’t that’s fine, we’ll talk about other strategies if you can’t. Do you feel you can bring it up with her?
Related article/video:
Melissa: I could try. I was planning to try tomorrow anyway because I had a change of heart about taking the mask off. Hospice was very nice and so I said yes, and then I came home and I had a panic attack and I’m like …
Patrik: Second thoughts.
Melissa: I called them and yeah, I don’t want to take the mask off. But they’re telling me they can’t keep it on indefinitely. That eventually we have two choices, to take it off or to put her on the breathing tube.
Patrik: Are you a religious person, may I ask?
Melissa: I would call myself a spiritual person.
Patrik: OK, that’s good to know.
Melissa: I want what my mom wants, and I have this selfish little voice inside my head that’s saying put her on the breathing tube, but my dad doesn’t want it. I even called 888, the cancer hotline, and they seem to be for that, and all her friends are for that, and my friends are for that, and my dad’s … I mean I’m the only one who’s even doubting it.
Patrik: That’s fine, that’s fine. Look, an end of life situation is very difficult and you don’t want to have, if your mom passes away you don’t want to have second thoughts. And I think you’re doing the right thing by talking to people and gathering different opinions from friends as well as from health professionals who have been in those situations before.
Melissa: Are they telling me the truth about the mask? Do you, I mean how long can someone be on an oxygen mask?
Patrik: Oh forever, forever, there’s people at home living on oxygen. I’ll give you a very quick example without dragging this out, somebody for example who’s waiting for a lung transplant and is at home would be on oxygen sometimes for years.
Melissa: But then why are they saying that they can’t keep her on indefinitely.
Patrik: Yeah look I tell you what I always say. With any client I say look ICU beds, or even beds in hospitals are in huge demand. That’s one thing, they fill their beds in no time, that’s number one. So there’s huge pressure on beds. Number two, the point of view from health professional is often I wouldn’t want to live like that. I’m criticising that because I say that’s not for you to judge. That’s for the patient and for the family to judge, right?
Meliss: Yes.
Patrik: And that’s why I believe you need to bring it up with your mom. I really believe you do need to bring it up with your Mom, especially since the health professionals can’t. Look I believe there’s a lot of health professionals out there who haven’t face their own mortality. I believe to have mature discussions around end of life people need to have faced their own mortality. And I don’t know whether you are dealing with people who have faced their own mortality. That’s just me thinking out loud. And that’s why I’ve also asked you, do you feel like you can bring it up with your mom, because depending on where people are at in their lives, in those situations it’s very confronting and …
Melissa: Her home companion was there this morning. Now the companion told me that she had a talk with my mom and my mom said she’s ready to die and she doesn’t want to fight anymore. So my brother was sceptical, he said how do we know she didn’t invent that story, which sounds crazy but she’s very religious and maybe she wanted to make us feel good. I’m like how did she have such an in-depth conversation if she has an oxygen mask on first.
Patrik: That doesn’t stop people from having conversations if they are awake.
Melissa: Yeah, I guess. They told us she’s never going to come home again, that she’s too sick to come home. That if she …
Patrik: Okay, let’s hone in on that for a moment if they’re telling you she’s too sick to come home. Do you know whether she’s on any other life support despite the oxygen? Do you know that?
Melissa: don’t think that she is, no.
Patrik: Okay. Do you know whether she’s on any blood pressure support with medication?
Melissa: I think that she is, but I think … Well, I think she may be on steroids. Let me ask, dad I’m talking to Patrik from INTENSIVECAREHOTLINE.COM. Is she on any other medical life support systems besides the oxygen mask?
Dad: Well she’s taking medications for the infection …
Melissa: Yeah, she’s taking medications intravenously right?
Dad: Yeah …
Go and look out for the next episode of “YOUR QUESTIONS ANSWERED” where I continue the conversation with Melissa and help her to come to terms with what’s happening with her Mom!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!