Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question in this series of questions from my client Melissa and the question last week was PART 5 of
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next question in this series of questions from one of my clients Melissa, which are excerpts from phone and email counselling and consulting sessions with me and the question this week is
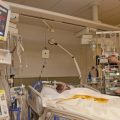
My 78 year old Mom has lung cancer and developed an infection! She’s in ICU on the breathing tube, can she get off it or will she need a tracheostomy? (PART 6)
Previous questions answered from Melissa, you can find here
PART 1, PART 2, PART 3, Part 4 and Part 5
Melissa writes
Hi Patrik,
I hope you remember us. My dad and I had contacted you about my mom some time ago. The hospital had not wanted to do anything for her. I hope you remember us.
Unfortunately she is back in hospital. The Tumour has grown again and she has fluid in the lungs which is most likely from the cancer but maybe from a bacterial infection or pneumonia.
Now it is starting again…every time I go there they ask are we sure we want to keep her alive. The tumour has grown. Maybe she should not go on a breathing tube?
We are insisting she should be put on a breathing tube if her breathing gets to point where she cannot do it on her own. Is that what you’d advise?
The tumour grew quite significantly but I don’t like to give up and I know she wants to fight because in the past she has voiced her wishes. The hospital like last time is telling us she will not get better and will most likely die in the next few weeks.
I do not want to be in denial but I still want them to do everything they can. The hospital makes me feel like an awful person sometimes by asking for that. I do not get it. I am sure we cannot be the only ones who think like this. Maybe they just think it’s to late but it is getting to the point where I dread even visiting her because some nurse or doctor will grab me and ask me the same questions over and over. I hope I am not being selfish. Have you ever heard this from other families who had a family member with lung cancer and fluid in the lungs? Any thoughts?
Melissa
Recommended:
Hi Melissa,
of course I remember you, your Mom and your Dad!
I’m very sorry to hear your Mom is back in hospital.
You are certainly not the only one who wants to keep your loved one alive against medical “expert” advise. It’s just normal for families wanting to do that.
And it’s almost “normal” for doctors in Intensive Care wanting to “pull the plug” or to “withdraw treatment” against a family’s wish, I have seen it over and over again, in nearly 20 years Intensive Care Nursing experience in three different countries, where I also worked as a Nurse Unit Manager for over five years.
Intensive Care is a highly political environment, therefore life or death decisions are almost always made due to what’s happening “BEHIND THE SCENES” in Intensive Care and not necessarily due to medical facts.
If families in Intensive Care don’t question, if they don’t do their own research and if they take everything the Intensive Care team says for face value they are doomed!
As a matter of fact 99% of families in Intensive Care don’t make informed decisions, they don’t have peace of mind, they don’t have power nor do they have control and influence!
I know you have already proven to be in the 1% bracket of families in Intensive Care and I know you leave no stone unturned in order to make informed decisions, get peace of mind, control, power and influence, give yourself a pad on your back for doing that!
The next problem that families in Intensive Care are facing is that they feel intimidated by the “perceived power” and the “perceived authority” of the Intensive Care team and they need to stop doing that…
Related article/video:
If you followed my newsletter and the questions people ask, it’s often the same over and over again, families want one thing and hospitals/ICU’s want another thing. That’s all we do day in and day out, successfully advice families in Intensive Care how to get what they want.
We are the experts at positioning diagnosis, prognosis as well as care and treatment. We have more than once successfully reversed “DNR”(Do not resuscitate) and/or “NFR” (Not for resuscitation) orders and we have more than once saved or at a bare minimum prolonged lives for Patients in Intensive Care. You can find enough case studies on our blog with evidence for that!
In fact I have written an entire Ebook about the subject here how to successfully reverse “DNR”(Do not resuscitate)/”NFR”(Not for resuscitation) orders as well as “withdrawal of treatment decisions”.
Looking at your Mom’s situation, I know she has been fighting many battles including tracheostomy ventilation and then subsequent weaning off of it. It sounds like she came fine through all of those challenges.
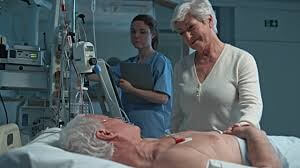
If she has fluids in the lungs now it could well be from a Pneumonia or the tumour. It could also because of kidney failure but you haven’t mentioned anything about that.
You didn’t mention if your Mom had Chemotherapy in recent months and I assume it hasn’t been the case given you haven’t mentioned it.
I do remember when I first counselled and consulted you earlier in the year that you mentioned your Mom having had Chemotherapy but I don’t think she had it since.
Now, given her current situation, if she has fluids on the lungs due to either a Pneumonia or due to the recurring tumour she may end up on the breathing tube and the ventilator if her oxygen levels are dangerously low.
To put this in perspective, if your Mom’s oxygen saturation levels drop below 90% even though she might be on oxygen, she will need to either go on BIPAP ventilation with a mask and if that’s not sufficient, she will need intubation and ventilation with a breathing tube.
Other things to look for are the results of her arterial blood gases. What do I mean by that?
In order to establish how well her gas exchange is in her body, the may have already inserted an arterial catheter to regularly check arterial blood gases.
If they haven’t inserted an arterial catheter, they are not monitoring your Mom’s gas exchange to the best of their abilities.
Gas exchange in the blood can be monitored with an arterial catheter and oxygen as well as carbon dioxide levels can be measured in the blood and depending on the numbers BIPAP ventilation with a mask or intubation and ventilation with a breathing tube may need to follow.
If they haven’t inserted an arterial catheter, they might already be thinking about not giving your mother best and standard treatment and she may already loose precious time if they are not monitoring and treating her appropriately.
For example if oxygen levels(=PO2) in the blood are <65 mmHG and if Carbondioxide(=PCO2) levels in the blood are >45 mmHG it suggests that her breathing and gas exchange is inadequate and that she will need BIPAP ventilation with a mask or intubation and ventilation with a breathing tube.
And that’s why it’s really advantageous if you hire someone like me because I can help you asking all the right questions so that there is no hiding for the Intensive Care team.
The next steps really are that if your mother’s breathing is rapidly deteriorating that she may need BIPAP ventilation with a mask and if that’s not sufficient, she will need intubation and ventilation with a breathing tube.
One way or another if she has either, it will buy her time to see where things are going and you can also be certain that if they do do it, that she can be kept alive for a period of time.
That doesn’t mean they can necessarily save her life if the tumour is growing, but it might mean that you can spend more time with her and you can also ask her what she wants.
As long as she’s awake and alert I think you should ask her what she wants and if she wants to continue fighting. As long as that’s the case you should make this very clear to the doctors and the nurses in ICU, especially if your Mom is getting more and more weak and she can’t express it herself.
If you and your family want to prolong her life, please also make sure her suffering is limited and also advocate for pain therapy and potentially palliative care and comfort care.
At this point in time your next steps are to
- Establish with your Mom what she exactly wants
- Make sure they have inserted an arterial catheter to monitor her arterial blood gases
- Get exact chest x-ray results
- Potentially ask for a CT of the chest
- Get arterial blood gas results
- Make sure the Intensive Care team is giving you options such as BIPAP ventilation with a mask and if that’s not sufficient, she will need intubation and ventilation with a breathing tube
- Make sure your mother is remaining comfortable and not in pain. She should have a pain team involved in her care
- Also speak to her Oncologist and get his views
As you know nobody can force you to “withdraw treatment” against your will and against your wishes, but it sounds like you are in for another battle to get what you want and I’m here to help of course.
Don’t feel bad about restating and reaffirming what you want, it’s your right and as you know, the Intensive Care team has their own “hidden agenda”, therefore you do whatever you feel is right for your Mom and for your family!
Recommended:
The hospital only wants you to make feel bad because they don’t want your Mom to stay in Intensive Care for much longer, something we have discussed before and something that I keep mentioning over and over again!
Intensive Care beds are in high demand, therefore the worst case scenario for Intensive Care Units is to have Patients in Intensive Care for longer than they want them to be in it, because they need the beds and staff.
Furthermore, they don’t want to deal with you and your family because they know by now that you and your family will be “difficult and demanding”…
As you know it doesn’t matter what other people think, as a matter of fact, it’s none of your business what other people think about you.
All that matters is your Mom and if neither she or you and your family are ready to give up, you should make that clear in no uncertain terms.
I have given you the first steps in what to do and in what to look for, so make sure they are doing all the right things and I’m looking forward to your next update!
Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!