Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question in this series of questions from my client Melissa and the question last week was PART 1 of
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next question in this series of questions from one of my clients Melissa, which are excerpts from phone and email counselling and consulting sessions with me and the question this week is
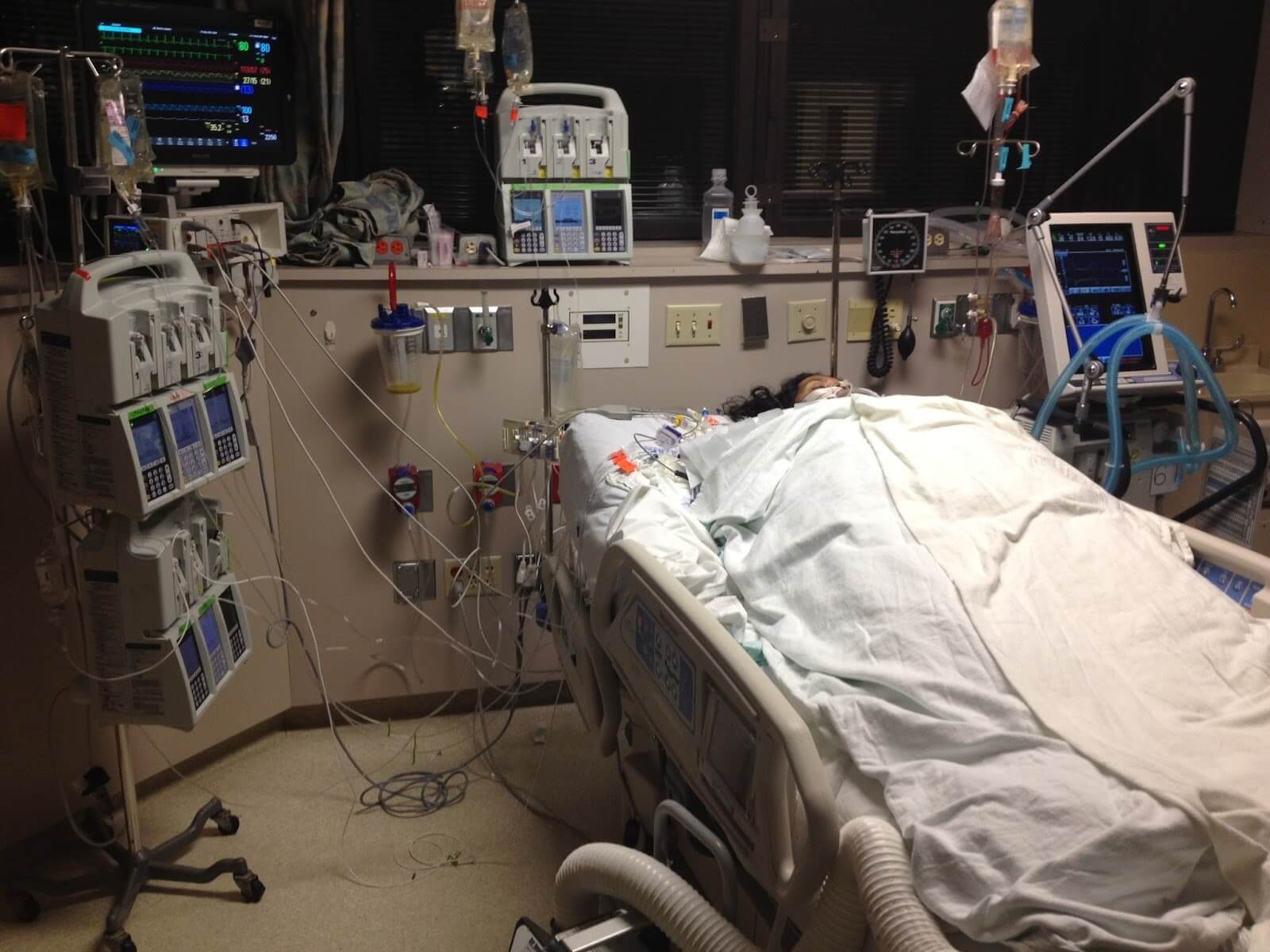
My 78 year old Mom has lung cancer and developed an infection! She’s in ICU on the breathing tube, can she get off it or will she need a tracheostomy? (PART 2)
Melissa writes
Hi Patrik,
So we asked all the questions you advised us to but the doctors dismissed all of them. He said and I quote “as I have told you 18 times now she is not going to get better”.
They have not done any physical therapy with her and refuse to do so.
The doctor (I call him doctor death) said and I quote:
“10 percent chance the rehab we want her to go to will take her”
Medicaid only pays to a certain point.
The Doctor told us we will be in the poorhouse, his exact words were “keeping her alive will have consequences for your children” money wise.
I have asked doctor EIGHT TIMES to never bring up “pulling the plug”.
Also, the hospice said they’d pay for a bed and other stuff if we bring her home. The doctor says hospice is incorrect and they will not pay anything unless we agree to remove the tube and let her die because they do not deal with people on ventilators nor pay for equipment. Hospice only deals with people who are dying. Who do we believe?
He actually asked my dad if his kids know and I quote “that keeping her alive will have consequences for us”. I guess the doctor means our inheritance which frankly I do not care about.
I love my mom and would certainly give my life for her and I am not one to care about money. I thought that was distasteful and I had to leave because it made me a little sick.
My mom wants the tracheostomy…but I withdrew my consent because as soon as we said yes to the tracheostomy they want do it tomorrow. We have 8 inches of snow coming and cannot be with her but he scoffed at me and said it’s a quick harmless procedure and we do not need to be there…I said she’d be scared, the doctor said “no she wouldn’t.”
I feel worse now than before… Please advise.
Regards
Melissa
Recommended:
Hi Melissa,
I’m very sorry to hear that you are dealing with such unethical and quite frankly rude doctors.
I can only imagine how you and your family must feel after they have spoken to you so rudely and also inappropriately.
They are trying to avoid the detailed questions by just saying “she’s not going to get better”. The devil in this situation is in the detail and as long as they are not sharing chest x-ray results, arterial blood gases etc… they are not being open and transparent but we can get them to that point.
First of all, it sounds to me like the doctors are very dismissive of your concerns and the sad truth is that I’m not surprised by it!
Just because they dismissed your questions once doesn’t mean they will dismiss them again. Persistence is key here.
If you give up too early you’ll end up like the 99% of families in Intensive Care!
The fact of the matter is that 99% of the families of critically ill Patients in Intensive Care make no informed decisions, they have no peace of mind, no control, no power and no influence!
Unfortunately, the doctors know that they can get away with this sort of behaviour with 99% of the families who are intimidated by the “perceived power” and the “perceived authority” of the Intensive Care team!
The doctors and the Intensive Care team know that and as soon as you start asking the right questions they become defensive and rude!
They know that you are starting to do your own research and they know that you have no time to take any prisoners!
I’m glad you keep reminding them of not mentioning to “withdraw treatment” or “pulling the plug”, they need to hear this over and over again, because as I mentioned before they are so used to get what they want, even if it means stopping or withdrawing treatment against a family’s wish!
It’s shocking and I know from experience that’s how families in Intensive Care are often being dealt with and I know for a fact that if you don’t question, if you don’t put on the breaks and if you continue to be intimidated by the “perceived power” and the “perceived authority” of the Intensive Care team, there is a good chance they will kill your mother!
If you don’t continue to challenge them, they will tell you that stopping or withdrawing treatment or “pulling the plug” is “in the best interest” for your mother!
Recommended:
The good news is that I have helped hundreds of families in Intensive Care to get what they want and I know the system so well that I know how to stop Intensive Care teams from withdrawing treatment against your will. I have been there done that many many times!
The biggest problem for families in Intensive Care is that they don’t know what questions to ask and without asking the right questions and without challenging the Intensive Care team, you and your family are doomed!
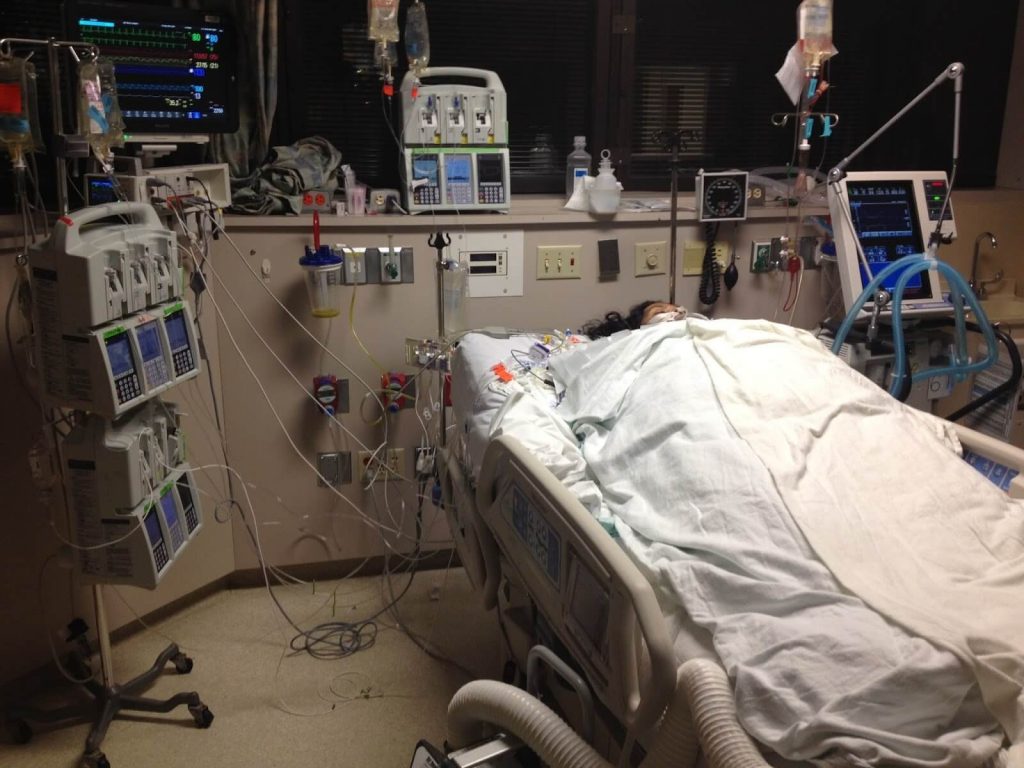
Therefore, positioning your mother’s prognosis, her diagnosis, as well as her care and treatment are key in this situation. If you don’t position your mother’s diagnosis, prognosis, as well as her care and her treatment, the Intensive Care team will do it for you and as you know by now, they are prepared to “pull the plug” against your will, letting your mother die any minute from now on!
It’s time to stand up for your mother and it’s time to continue asking the right questions.
Quite frankly, I’m absolutely shocked that they still haven’t done any Physiotherapy/Physical therapy for your mother.
As I mention in this article/video here
If they are not following best practice and the guidelines above, they have already given up and especially since they are already trying to refer your mother to hospice, they seem pretty determined to let your mother die without even trying.
As I mentioned before, the biggest problem that ICU’s have is that they need their beds because they are in such high demand!
Therefore, the easiest way to free up their beds is to try and “sell” you on an end of life situation as being “in the best interest” for your mother, even though you don’t agree with it.
Well, the biggest challenge for families in Intensive Care is that they can’t read between the lines and they can’t interpret the Intensive Care language accurately.
Whenever the Intensive Care team says it’s “in the best interest” for your mother, what they really mean is that it’s “in the best interest” for them and their hidden agenda.
What’s their “hidden agenda”?
Well, once again, the biggest challenge for Intensive Care teams is to not have enough resources, including Intensive Care beds and they are not prepared to give Patients in Intensive Care the time they need to recover!
Recommended:
They would of course never tell you about it and unless you start asking the right questions and unless you start challenging the Intensive Care team on many levels…
Next, generally speaking I support a tracheostomy but only after all efforts have been made towards getting your mother off the ventilator and the breathing tube in the first place! Those efforts haven’t been maximized yet and clearly by avoiding your questions they are not open and transparent with you!
Again, if they are not doing Physical therapy for her chest, they haven’t even scratched the surface. They just keep ignoring your and your family’s requests! It’s what they are used to and it’s because 99% of the families in Intensive Care don’t question and make no informed decisions, have no peace of mind, no power, no control and no influence.
Once you start asking the right questions, everything changes.
In your and your mother’s situation the following applies.
Given that your mother is awake and says she wants a tracheostomy, she clearly says she wants to live. If the doctors continue to bring up “withdrawing treatment”, it would be clearly against your mother’s wishes. “Withdrawing treatment” and potentially letting your mother die against your and her wishes is called murder in my mind.
Their goals is to discharge your mother to either Hospice or to Long-term acute care(LTAC). Discharging her to a hospice is probably quicker from their end because it
- Doesn’t require a tracheostomy and hence they can move her out of ICU quicker
- Doesn’t require the effort to go through a potentially lengthy weaning process off the ventilator and the breathing tube(endotracheal tube)
Next, doing a tracheostomy will allow your mother to be weaned off the ventilator in her own time and it buys her time.
Related articles/videos:
I agree that a tracheostomy is a quick and harmless procedure generally speaking, therefore it can be done quickly without you needing to be there.
I can however understand that you don’t trust them and I can see why you feel the need to be there when they do the tracheostomy.
Overall, I’m absolutely shocked and horrified in how you and your mother are being dealt with and I urge you to be persistent and not give up!
They will understand what you and your mother are made of if you don’t give up.
Related article/video:
Moving forward, if for whatever reason your mother can’t be weaned off the ventilator and the tracheostomy once she has one, there is still plenty of time to revisit your Mom’s options.
Her options would be
- Home Care like INTENSIVE CARE AT HOME and unlike the doctors suggest, there is funding available for INTENSIVE CARE AT HOME, because it creates a win-win situation and gives Patients and families what they want and it reduces the cost of an Intensive Care bed by 50%
- Potentially LTAC(=long-term acute care) and again, generally speaking we don’t advocate for LTAC because it’s long-term acute care and no LTAC is ever be as equipped and skilled like an ICU to wean a Patient off the ventilator. Also, ventilation weaning can also be done at home with a service like INTENSIVE CARE AT HOME
- Potentially hospice if your Mother is really approaching her end of life. But it’s way too early to talk about hospice. Also, even if hospice is needed, you could still have your mother at home with INTENSIVE CARE AT HOME and have her pass away at home
I hope that helps Melissa for now!
Don’t give up! Don’t and never take “no” for an answer! Question everything, keep them on their toes and be relentless!
You are getting much closer to get in the 1% bracket of families in Intensive Care who make informed decisions, get peace of mind, control, power and influence!
Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!