Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question in this series of questions from my client Melissa and the question last week was PART 4 of
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next question in this series of questions from one of my clients Melissa, which are excerpts from phone and email counselling and consulting sessions with me and the question this week is
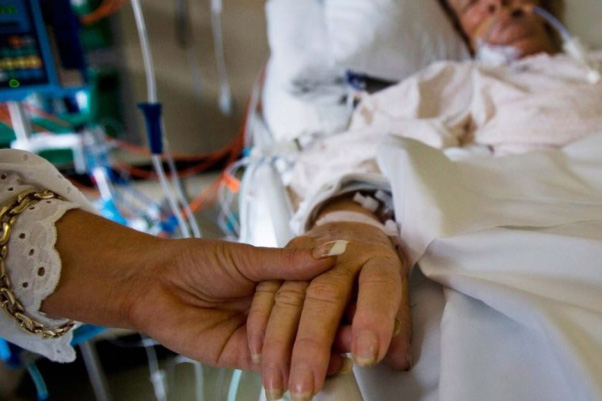
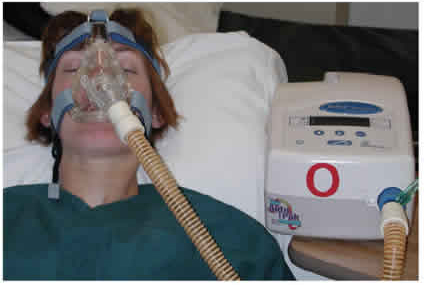
My 78 year old Mom has lung cancer and developed an infection! She’s in ICU on the breathing tube, can she get off it or will she need a tracheostomy? (PART 5)
Previous questions answered from Melissa, you can find here
PART 1, PART 2, PART 3 and Part 4
Melissa writes
Hi Patrik,
I to want to thank you very much for your support and kindness. It has meant a lot to us as a family.
We have a long road ahead of us and while I am overjoyed she is at this moment breathing on her own, I have no illusions, my Mom is still very sick and I know anything can happen. We are all trying to take it one day at a time.
She now has a tracheostomy and she will be going to LTAC(=Long-term acute care) in a couple of days. We’re just glad she’s got the tracheostomy now and she’s ready to finally move on.
Please keep us in your thoughts and if ever you are speaking to a family member in a similar situation, who are told by doctors that there is little hope, remember us and tell our story. I would hate to think someone thinks seriously about pulling the plug when there is still hope. If there is one thing I am learning through all this it is that doctors do not know everything. I guess nobody really does. Thank you again and when and if we are in a difficult situation in the future or know someone who is we will give you a call.
Sincerely,
Melissa
Recommended:
Hi Melissa,
thank you for your kind words.
You mention
“Please keep us in your thoughts and if ever you are speaking to a family member in a similar situation, who are told by doctors that there is little hope, remember us and tell our story. I would hate to think someone thinks seriously about pulling the plug when there is still hope.”
I know you and your Dad are new to my blog as well as new to my 1:1 phone and email counselling and consulting, but if you read my newsletters and if you read or watch my “your questions answered” section, you will find that all of my advice, advocacy, counselling and consulting is all about not “pulling the plug” as long as there is hope.
One of the reasons why I feel so strongly about this is that I have seen way too many situations whilst working in Intensive Care, where Intensive Care teams have been “withdrawing treatment” against a families’ wishes and without family consent, where I knew for a fact that the Intensive Care unit simply needed the bed for the next Patient.
Families have literally either been “sold”, coerced or forced into agreeing to basically kill their loved ones because it suited the Intensive Care team’s “hidden agenda”.
Related article/video:
In some cases, Patients also didn’t get full and standard treatment because they weren’t of interest for the Intensive Care team because they couldn’t do medical research or they couldn’t attract enough funding!
I was obviously very shocked when I first understood the finer details in Intensive Care and how life or death decisions were made.
A breaking point for me was that I eventually refused to withdraw life support on critically ill Patients when being asked to as a bedside nurse and I realized that nothing bad will happen, you just have to question things and you have to justify your point of view with solid facts.
Recommended:
I learned that I could be a Patient and family advocate if I choose to.
After nearly two decades working in Intensive Care I know how to position diagnosis, prognosis as well as care and treatment to get the best outcomes for critically ill Patients and their families.
After nearly two decades working in Intensive Care in three different countries, where I also worked as a Nursing Unit manager in Intensive Care for over five years, I have learned enough, I have seen everything that’s happening “BEHIND THE SCENES” in Intensive Care to start writing about it and to help families in Intensive Care 1:1 and get results quickly for them!
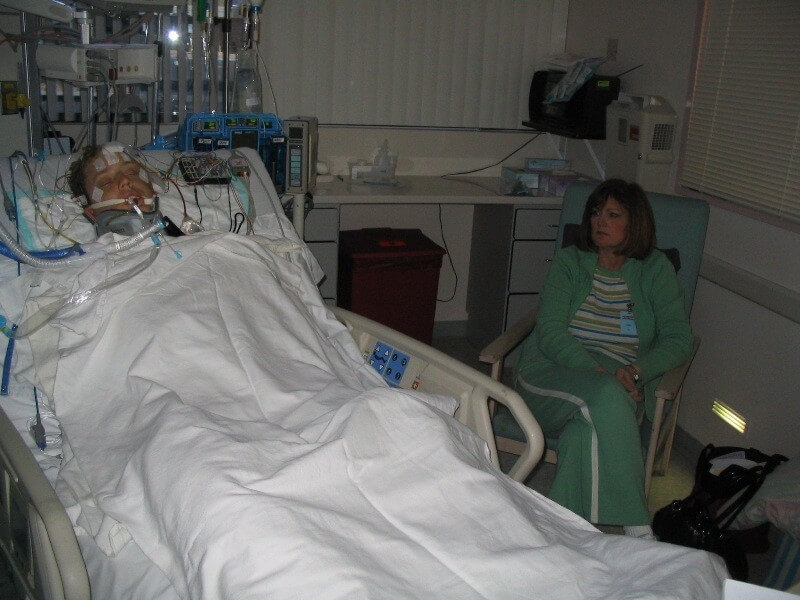
The reality is that 99% of the families in Intensive Care make no informed decisions, they have no peace of mind, no control, no power and no influence and they take everything the Intensive Care team says for face value, without questioning and without doing their own research.
I have seen too many situations, when I was still working full time in Intensive Care, where families have been “sold” on a “withdrawal of treatment” or they have been sold on a “DNR”(Do not resuscitate) or “NFR”(Not for resuscitation) order as being “in the best interest” for their critically ill loved one.
They are being told by Intensive Care teams that nothing else could be done and that their loved one would die etc… without having been told that other treatment options might be available…
Therefore it’s extremely important to question everything especially when it comes to “perceived” vs “real” end of life situations
Related article/video
The fact of the matter is that if you don’t question, nobody else will do it for you! If you don’t do your own research, no one will do it for you and the fact of the matter is that if you don’t do it, you’ll be at the mercy of the Intensive Care team, that’s making their decisions based on the financial budget as well on the bed management agenda of the Intensive Care Unit!
Recommended:
There are hundreds of answered questions (aka real world case studies), tips, strategies as well as interviews on my podcast that all have one recurring theme to never give up and to always question!
One of the reasons why I created this whole movement as well as business with INTENSIVECAREHOTLINE.COM is that I as a bedside nurse in ICU have felt compromised in my values, ethics and believes with everything that ICU’s and hospitals do because of their “hidden agenda”.
Recommended:
I know all about it and I know that Patient care is often compromised and it also costs lives because of early withdrawal of treatment or “pulling the plug” because of reasons that are unknown to people who haven’t worked in the environment.
Again, you know where I am if you need help. I help people get real results when it comes to life or death decision making and I know how to successfully steer the system in this jungle of complexities!
Kind Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!