Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question and CASE STUDY last week was Part 1 of
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another question from one of our clients which is an excerpt from a 1:1 phone counselling and consulting session with me and the question this week is PART 2 of last week’s CASE STUDY and we continue today with
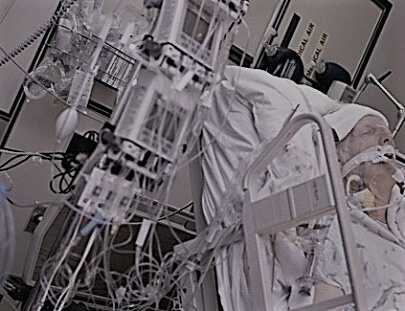
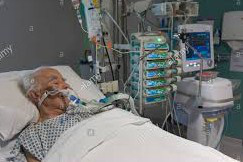
CASE STUDY: My 77 year old Dad has been in ICU ventilated for a week and he’s not “waking up”! The doctors have made him NFR without my consent and they want to switch off the ventilator, help! (PART 2)
This is another great case study where you can see how I can help a very concerned and very distressed client how to quickly make sense in a situation where the Intensive Care team hasn’t been open transparent with her and her family!
As a matter of fact, the Intensive Care team threatened to take her Dad off the ventilator by a certain date, without the client’s consent!
It’s also another great case study to show families in Intensive Care that you simply don’t know what you don’t know and that you getting informed quickly so that you can turn the dynamics in your favour is crucial!
If you do what 99% of the families of critically ill Patients in Intensive Care are doing you won’t do your own research and you will just silently nod off everything the Intensive Care team is telling you and you will be intimidated by the Intensive Care team…
If you do that, you will not being able to make informed decisions, get peace of mind, control, power and influence…
As a matter of fact, if you don’t ask the right questions and if you are not arming yourself with crucial insider and “BEHIND THE SCENES” knowledge, your critically ill loved one and your family may be doomed!
In our case study with my client Denisa, you can see that only in one phone conversation I can empower her and show her what questions she needs to ask and I can also show her what information the Intensive Care team has been hiding!
It’s also another great case study how to counteract the negativity of the Intensive Care team, if you only know what questions you need to ask and if you can interpret information correctly!
The number one complaint we’re getting from families in Intensive Care is that Intensive Care teams are negative!
We know that and in our hundreds of “YOUR QUESTIONS ANSWERED” episodes and in our hundreds of case studies we always show our clients how to stay positive and how to position your critically ill loved one’s diagnosis, their prognosis as well as their care and their treatment in a light that doesn’t allow Intensive Care teams to be negative!
This is also another great CASE STUDY how we can help our clients to not only get the best care and treatment possible for their critically ill loved one, it’s also a great CASE STUDY how we can predictably help families in Intensive Care to reverse an NFR (=not for resuscitation) order or a DNR(Do not resuscitate) order that was issues against their wishes and without their consent!
Because we know the hospital system and Intensive Care so well, we can get predictable results for you and for your critically ill loved one really quickly! We can help you position your critically ill loved one’s diagnosis and prognosis and therefore help you to get the best treatment for your critically ill loved one!
If you don’t know how to position your critically ill loved one’s prognosis and diagnosis, the Intensive Care team will do it for you and they do so with their own self-interest at top of their mind!
Enjoy the case study and enjoy the excerpt of the phone counselling and consulting sessions!
Patrik: So, the initial admission to ICU was for pneumonia, is that correct?
Denisa: It was because he went so downhill since admission and he was delirious and they said because he had an infection in his blood, that’s why they put him in ICU.
Patrik: Okay, and why did they start ventilating him?
Denisa: I think that was because his breathing.
Patrik: Breathing was laboured or … Okay.
Denisa: Yeah. They told other family members it was because he was misbehaving too much, but-
Patrik: That’s terrible.
Denisa: I was there beforehand and his breathing went really downhill, and so did his blood pressure. I don’t know what the term is. A-tach, I think? Is that it?
Patrik: Sorry, what was with his blood pressure?
Denisa: I forgot. Is it called A-tach when it goes very high?
Patrik: Very high is usually called hypertension.
Denisa: Oh okay, yeah.
Patrik: Very low is hypotension.
Denisa: Oh okay, I think his blood pressure went very high four times in a small amount of time.
Patrik: That shouldn’t get somebody on the ventilator necessarily.
Denisa: Okay. He was … He had a very … Before they put him on it, even with the big mask on his face, he was making a lot of crackling noises breathing.
Patrik: Okay, okay. Fair enough, fair enough. And then did you mention earlier that he developed the Pneumonia?
Denisa: Yes. He’s been hospitalised for the last four years with bouts of that because he’s got emphysema.
Patrik: Emphysema. Yes, that’s right, that’s right. Okay. So, how is that infection going that he initially went into hospital with? Do you know whether they’ve treated that? Do you know what the outcome of that is or was?
Denisa: They, oh gosh, a few days ago it would have been now, I spoke to a doctor this Saturday or Sunday night I think, sorry. And he said yes, the infection they think they had treated, had his blood pressure normal. They had, I think, it was his glucose levels were normal, he was breathing on his own, yeah.
Patrik: The only issue then that you’re dealing with is the emphysema and him not waking up. Would that be … From what you can see, would that be accurate?
Denisa: Yes, well they’ve even said that he physically has been able to come off the ventilator for about a week now and his consciousness is the only thing stopping him.
Patrik: Okay, okay. So despite the emphysema, you know his breathing, he is doing most of the work himself as far you are aware? The only thing that is stopping him is basically he is not waking up, okay.
Denisa: Yeah.
Patrik: Irrespective of what might happen down the line, the goal would be to get him off the ventilator obviously and as long as he is not conscious that might be challenge. When … So, you had a family meeting yesterday is that correct?
Recommended:
Denisa: Yes.
Patrik: Right and that was when the NFR was discussed, the not for resuscitation?
Denisa: Yes. They have mentioned it a couple of times, but yes they mentioned it yesterday.
Patrik: Okay, okay. With the family meeting, did you feel under pressure or how was that sort of conducted?
Denisa: Yeah, I did a little bit. I felt like they mentioned about not resuscitating him. They were really pushing we need to think about his quality of life if he was to wake up. His organs would be so damaged from the ventilator by now. They were … They were pushing it and they … It seems like they waited until I was hysterical to bring it up as well.
Patrik: Right, right, okay. Well, from what you are telling me, yes, the longer ventilation goes on it’s not great, but the reality also is that people do survive after weeks of ventilation sometimes. The reality is that 90 to 94% of patients in ICU leave ICU alive, okay? Actually, it is more a minority of patients that don’t survive intensive care! They wouldn’t tell you any of that. As I said to you before, their biggest problem or their biggest concern is that your dad will take up an ICU bed for the next four weeks. That’s their biggest concern, right?
Denisa: Okay.
Patrik: That shouldn’t be your concern. Your concern is your dad, right? What did you mention earlier in regards to the heart? Did you mention something about a small heart attack? I can’t remember.
Denisa: Yes, they only mentioned this for the first time in the meeting yesterday. They said, I think, he had it before he was ventilated.
Patrik: And they are only telling you now to?
Denisa: They only mentioned yesterday.
Patrik: To find another argument for the NFR (=Not for resuscitation)? They didn’t have the time to tell you that before, because I think that’s quite significant if your dad had a heart attack and they didn’t tell you until yesterday. I think that’s –
Denisa: Oh, definitely, definitely, yeah.
Patrik: They rubbed it in your face yesterday to basically have another point for the NFR(=Not for resuscitation), but they didn’t feel the need to tell you that prior to the meeting. I think that’s very inappropriate.
Denisa: And even on the days I haven’t gone in, I ring three times a day, at least. I’m always asking them when … I’m asking to speak to the doctors, yeah.
Recommended:
Patrik: Okay, okay. How do you feel the day after the meeting? How do you feel about the NFR(=Not for resuscitation order) today? Has your point of view changed? Have do you feel?
Denisa: I felt uncomfortable about it even during the meeting, especially since I started looking up information online, which is how I’ve got your number, especially yesterday when … The day before yesterday, my brother and I went in and I was sitting with him and holding his hand. He wasn’t holding my hand back, but he was … You could see he was sort of agitated a little bit. He was opening his eyes a little bit. He squeezed my hand randomly twice and he didn’t just move his fingers, he gripped my hand twice. I said to him, “Dad, can you squeeze my hand again?” It was delayed. It was about 5 or 10 seconds later, he did it. He gripped my hand.
Patrik: That’s a good sign.
Denisa: I yelled out to the nurse. The nurse would have been able to see him do it and the nurse just blew it off. Since then, I’ve been feeling restless about everything they are trying to day.
Patrik: Yeah, fair enough. That’s fair enough. I totally understand people’s wishes when they say, look if I ever go into ICU I don’t want to be a ventilator. I don’t want to be a vegetable, you know often use that term and I understand that. What I also understand after nearly 20 years working in ICU, I also understand that most patients survive ICU and they are usually most grateful if they do survive, right? What I’m referring to here is people simple don’t know what they don’t know, right?
Denisa: Yeah, yeah.
Patrik: I mean when looking at … I think if one of my family members would be in ICU, yes, I don’t want them to be on a ventilator. I don’t want them to have a tracheostomy, but I do want them to survive, right?
Recommended: 1:1 phone counselling and consulting with Patrik
Denisa: I think … Yeah, yeah.
Patrik: Do I want them survive at any cost? Probably not, but I also know what’s possible.
Denisa: Yeah, I think if he was never going to come off the ventilator that would be different, but …
Patrik: Right.
Denisa: Being on a ventilator for a short term even is … There’s life after that possibly.
Patrik: Absolutely, absolutely. So, you know that’s what I can see and again especially in the public health system and I can’t stress that enough. Their biggest worry is that your dad will occupy a bed for the next four weeks. That’s their biggest concern, right? So, in essence we’re really talking about them looking for a solution for their ICU and you looking for a solution for your dad and that’s often conflict of interest. You know? It’s as simple as that. My feeling around, especially if you felt under pressure yesterday, in regards to that NFR (=Not for resuscitation), my advice to you would be to go back to them tomorrow and ask them to take it off. That would be my advice. My advice would also be to not go into a family meeting until you are clear of what you want and how you go about it and we can help you with that. Yeah, go on?
Denisa: I think too with the family meeting they asked me what other relatives know the day before yesterday, before they even … He only had the MRI yesterday afternoon. They organised this meeting before he even had a MRI.
Patrik: Oh, okay, okay.
Denisa: In the meeting, we were waiting about an hour after the scheduled time because they were still down with him getting the result of the MRI, they had only just done it.
Patrik: Right, right, okay. So, that again, again you don’t know what you don’t know. If you had spoken to me two days ago, I would have said don’t go into a meeting until you have had the MRI results rights? Okay, so you really from my perspective, you’ve really got to be careful with those family meetings. My advice would always be that if you know what you want and if you also know how to get it, go into a meeting. If you don’t know what you want exactly and also you don’t know how to go about it, don’t go into a meeting, because they will eat you alive. They’re holding meetings every day of the year. They know what to say. They know how to say it. They know when to say it…
Denisa: They know when to, uh, yeah, yeah.
Patrik: They also know what not to say.
Denisa: Yeah. They wouldn’t tell me beforehand either and I asked a few times what the meeting was specifically for and all they would tell me was just a meeting to talk about dad. That’s all they would tell me as well.
Patrik: That’s when you should have told them, look I’m not going into this meeting unless you’re telling me. Most people are intimated and you’ve got to stop that. You’ve got to stop being intimated by them. You’ve got to stop that right now because that will hold you back. That will hold you back.
Recommended:
Denisa: I think a lot of it too, I’ve been thinking that maybe or maybe this is in my head a little bit because I just want dad to be okay. It’s not at a point where it’s not.
Patrik: Yeah, and I can see it’s at a point where you are obviously questioning their doings and I think that’s a good point, you know? I think it’s good that you’re questioning and from my perspective from everything that you are telling me, he needs time and they don’t want to give him the time. That’s, you know … Sort of already putting a timeframe on it, well, we’ll keep him on the ventilator until the 27th of April. That’s inappropriate.
Denisa: Yeah. She was saying as well … She was implying to take him off, to just give up now as well. My dad’s partner, she was saying oh, but there’s hope. He might be able to wake up in the next week and this lady just cut her off and snapped at her.
Patrik: Highly inappropriate.
Denisa: And said, she said I’m realistic, that’s not realistic. She said the chance of him waking up is extremely minimal.
Patrik: Yeah, well, well, from my perspective there’s no brain damage, you know? That’s a given. There’s evidence there. What … You see this is all about positioning. You know, they are trying to position your dad’s case in a very negative light and they will be negative. They will be negative until the very day your dad leaves the ICU. They will be negative up until then because that’s their job, right? They would never tell you, oh, yeah, we’re definitely going to get your dad out of ICU alive, because what if they don’t? But, in the meantime, they will be putting a negative spin on everything.
Denisa: Yeah, yeah.
Patrik: Right?
Denisa: Yeah, definitely.
Patrik: You’ve got to be aware of that, you know? I’m sure you are by now. Okay, so, you know putting a timeline on this, whatever it is, 27th of April is highly inappropriate because your dad might wake up in two weeks.
Denisa: Yeah. They were really saying about his age and everything with the ventilator damaging everything and the amount of time he would have to be in rehabilitation, which really doesn’t bother me if he’s awake. They also said that with the tracheostomy that … They were talking about it in a way that it would be harmful to him or even leaving him on the ventilator now is being harmful to him.
Patrik: Okay, so look if you can get a patient off the ventilator, that’s always preferred. There’s no question around that. I’ll give you a quick other example so that you … That I can put in perspective for you. Part of what we offer for our service is INTENSIVE CARE AT HOME we … For example, we look after long-term ventilated patients at home. They have usually a tracheostomy and, you know, they are long-term ventilated, sometimes for months, sometimes even for years. Now, so absolutely you always want to get a patient off the ventilator as quickly as possible, but the reality is that there are some people who will need ventilation for the rest of their lives, okay?
Denisa: Okay.
Patrik: Now the reality is if you give people a choice or if they can make a choice … Well, if those people want to live you want to give those people the option to live, okay? Again, you know, your dad has only been on the ventilator for 13 days, which in ICU terms is not a very long time. It’s not a very long time. So, you know, in the ideal world he’ll come off the ventilator hopefully in the next week and wake up. That’s the ideal world, but, you know, to sort of cut him off and say, yeah the 27th of April that’s sort of the deadline. That, from my perspective, is inappropriate and your dad might just need time.
Related article/video:
Denisa: Yeah, especially if he’s got no … They can’t find anything wrong with him either.
Patrik: That’s exactly right.
Denisa: They were saying to me that there was nothing wrong with … He hadn’t had a stroke and his central nervous system was okay as well.
Patrik: Yeah, so that’s … Is that helpful so far?
Denisa: Yeah, very helpful thank you, thank you.
Patrik: Right. Okay, so is there anything else you want to know?
Denisa: You just said before the service you provide besides what we’re talking about now…
Patrik: Yeah, so I’ll tell what we can do on top of you and I talking 1:1. For example I could also attend family meetings. As I explained to you, I would never go into a family meeting without a professional advocate like myself who knows Intensive Care inside out. We could talk about how you should conduct yourself in there, what you should say, what you shouldn’t say. We’re basically … If we were to help you get the outcome that you want and also get them to try their very best effort also to do things like taking the NFR off, we can help you with all of that.
Denisa: Yeah.
Patrik: Again, that would include attending family meetings either over the phone or in person given that you are close by, you know that’s not … I could definitely come to family meetings in person or I could call in over the phone, whichever you prefer. That’s part of the service! Again, if you go into a family meeting unprepared, there is a very good chance that the Intensive Care team will walk all over you!
Denisa: Yeah, okay.
Patrik: If you wanted me to come to family meetings personally, usually, you know, we do a lot of work all over the world in the USA, Canada, UK, Ireland, New Zealand, Australia, South Africa etc… and most of the time we call into family meetings, but, you know, for our local clients we come in personally if they want us to…
Denisa: That would be great.
Patrik: If you wanted to engage me for family meetings too, besides the 1:1 counselling and consulting that we are doing now, we have to talk about do you want me to be in family meetings over the phone? Do you want me to come in person? We have to clarify that probably before the family meeting.
Denisa: Yeah. I didn’t even know that family meetings were an ongoing thing, I just thought there was one.
Patrik: Look, what I believe for now is you shouldn’t go into a family meeting. Only go into a family meeting if you know what you want and you know how to go about it. That’s what I would advise for now.
Denisa: Yeah. Oh, you’ve been a lot of help even on this phone call, thank you.
Patrik: Oh, you’re welcome.
Denisa: Yeah, yeah. I definitely want you to come to the family meetings!
Patrik: Absolutely, absolutely. I can do that, you just need to give me a little bit of warning…
Denisa: Okay.
Patrik: I could come to a family meeting as early as tomorrow!
This is PART 2 of the
CASE STUDY: My 77 year old Dad has been in ICU ventilated for a week and he’s not “waking up”! The doctors have made him NFR without my consent and they want to switch off the ventilator, help! (PART2)
Tune in PART 3 of our case study, it’ll come out in a few days where I’ll show Denisa how she needs to position her Dad’s diagnosis, his prognosis as well as his care and his treatment so that she can get what she wants, needs and deserves!
And most of all I help Denisa how she can take the NFR(Not for resuscitation) order off her Dad so that he’s in the best position to get out of Intensive Care alive!
If you haven’t subscribed to our free newsletter and to your FREE “INSTANT IMPACT” report below, please do so and you get more case studies like this, including PART 3 of this case study!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!