Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of our readers
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another the next question from our client Robert, which are excerpts from email counselling and consulting sessions with me and the question this week is
My 68 year old mother is in ICU with gastric perforation and she’s not “waking up” after the surgery! Will she need a tracheostomy? (PART 17)
You can find previous questions from this series of questions answered here
PART 1, PART 2, PART 3, PART 4, PART 5 , PART 6, PART 7, PART 8, PART 9, PART 10, PART 11, PART 12, PART 13, PART 14, PART 15 and PART 16.
Robert continues with his mother’s situation below
Hi Patrik,
I have some bad news. My mother took a big turn for the worse. They think that the area that was operated on — or somewhere else, there’s a perforation and it’s seeping fluid.
I’m headed into the hospital shortly, but it sounds like:
- She might need surgery.
- She may not actually be a candidate for surgery, given all the other issues.
- Even if she were a candidate for surgery, we’re not sure, if at this point, that’s the right answer.
They’re running a CT-scan now. The attending doctor has called for a meeting with the family. We are getting everyone together.
Our assumption is that they’re going to say we have to (or should) let her go. We’re mentally preparing ourselves.
In the meantime, some hard questions:
- At this stage in the process, what does “letting her go” entail? Do they slowly just withdraw her “supports”? Something else?
- Usually how long do we have with her, even once the decision is made?
- What is general “hospital procedure”? Do they move her out of the ICU for a couple of days first? Or, is that uncommon?
Thanks, as always for your help. We were hoping she would take a positive turn, but that just hasn’t happened.
Not losing complete hope, but I’m getting the sense that odds of her making it through now are very low.
Many thanks
Robert
Recommended:
Hi Rob,
I’m very sorry to hear what you and your family are going through.
It’s certainly extremely concerning that your mother has another perforation, hopefully at least you can get some answers by them doing a CT scan.
Besides having the perforation, what other clinical signs is she showing? Is she hemodynamically unstable, I.e. low blood pressure, fast heart rate, temperature etc… Those would all be signs that she’s developing Sepsis, which would not be uncommon after a gastric/abdominal perforation.
If she shows signs of developing severe Sepsis she would most likely need high(er) amounts of BP medication, I.e. inotropes/vasopressors to support a dropping blood pressure.
It sounds to me like if she had another perforation that she will need surgery, just simply from a clinical point of view.
However, as you have correctly pointed out, you are not sure if surgery is the right answer.
I guess it really comes down to how much you want to put your mother through.
I believe that in your recent emails you were talking about your mother being more comfortable. At the same time she may not have the reserves and the strength to go through another bout of surgery.
At the same time, you never know.
I understand the ICU team would be fairly negative and they will most likely say, that it won’t be in your mother’s “best interest” to do more surgery. It might be too much for her, also depending on if she now needs inotropes/vasopressors for low and deteriorating blood pressure.
If she’s too weak to begin with she may not survive the surgery, that may well be a reasonable concern, but I would need to know more clinical facts and details to have an educated opinion of whether surgery might be clinically indicated or not.
But again besides the clinical indication, your and your family’s concerns are very important too.
I guess, the bottom line might be, what would your mother decide if she could make the decision herself?
I also would like to recommend this article/video here
I have witnessed too many “perceived” end of life situations that resulted in death, where I believe death was preventable. I’m not saying that’s the case with your mother as I would need more information to make that judgement, but I think this article/video might be a starting point to help you in your decision making.
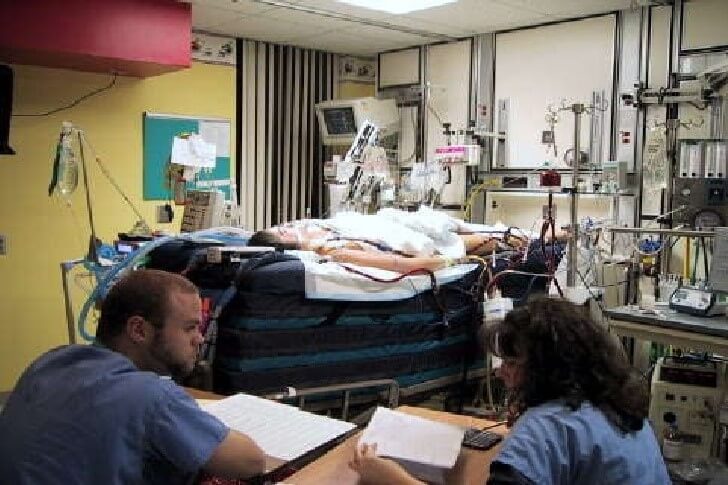
Getting to your most pressing questions, please see my comments in red.
- At this stage in the process, what does “letting her go” entail? Do they slowly just withdraw her “supports”? Something else?> It would entail removing major life support mechanisms such as ventilation, tracheostomy, Dialysis, inotropes/vasopressors. This may or may not be enough to “let her go”. It all depends. I would need to know how much ventilation support she’s on, how much inotropes/vasopressors. It would also entail stopping antibiotics and most likely commence sedation and opiates like Morphine or Fentanyl to enable her to go peacefully and without any pain and suffering. There is however no guarantee that this is a smooth and easy process
- Usually how long do we have with her, even once the decision is made?> It depends how much support she’s on and how quickly you, the family and also the ICU team want to start the process. I believe that timing in end of life situations is possible, however there needs to some planning around. I have seen too many poorly planned and then also poorly executed end of life situations leaving Patients, their families and also ICU teams in distress. It needs to be properly planned and communicated if time permits.
I believe it’s also important that you can ensure that you have all the people there with your mother you want to have there so that everybody can say goodbye.Also make sure that you have your cultural, religious and spiritual wishes granted(if any) that may be important for you and your family.
- What is general “hospital procedure”? Do they move her out of the ICU for a couple of days first? Or, is that uncommon?> The general procedure is really dependent on the hospital. If time and resources permit they may want to offer a “withdrawal of treatment” in ICU or move her to a hospice, presumably within the hospital.Some of the clients we’ve worked with in the USA we’ve also learned that they try and move people from ICU to hospices in other locations and I know that families feel overwhelmed by the change of environment in an already stressful situation.This seems to be US specific and doesn’t happen in the UK or Australia, hence ICU Patients approaching their end of life remain in ICU or they can go home with a service like INTENSIVE CARE AT HOME. Again, that’s why communication is so important!
- Family meetings in Intensive Care.As far as the Doctors calling a family meeting, I always suggest that you and your family need to be very clear in the outcome that you want out of a family meeting. If you are not clear about the outcome before such a meeting my recommendation is to not attend such a meeting.ICU teams have been running family meetings for long times, day in and day out, they know what to say, they know how to say it, they know when to say it and they know what not to say.
Recommended:
Therefore the odds are in their favour. Family meetings in such situations can be pretty dramatic and because you and your family feel a certain amount of gratitude towards the Intensive Care team for what they have done to this point, the psychological dynamics are stacked in their favour.
You need to be aware of this, especially since this is a life or death situation.
My best advice for now would be to wait for another 24 hours even before you go into a family meeting!
As long as your mother is not suffering, you may have that time, but I believe being clear about what you and your family want is very important!
In situations like that there are no right or wrong answers. There are only answers that matter to you and your family, not to the Intensive Care team!
The Intensive Care team will have their own agenda and you’ve got to weigh up the pros and cons of what’s best for your mother and your family.
Any other information you can provide may be helpful to help you with the decision making process.
I hope that helps, let me know what you need!
Warm Regards,
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



