Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question in this series of questions from our client Robert and the question last week was PART 9 of
You can check out last week’s episode by clicking on the link here.
You can find the previous questions answered from Robert here
PART 1, PART 2, PART 3, PART 4, PART 5, PART 6, PART 7, and PART 8
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next question from our client Robert, which are excerpts from email counselling and consulting sessions with me and the question this week is
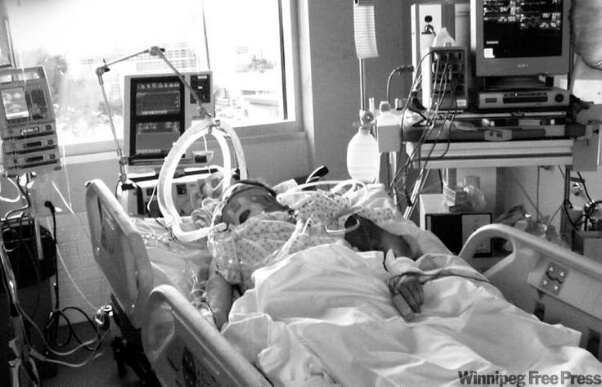
My 68 year old mother is in ICU with gastric perforation and she’s not “waking up” after the surgery! Will she need a tracheostomy? (PART 10)
Robert continues with his mother’s situation below
Hi Patrik,
My brothers and I met with the lead doctor today. They educated us on dialysis and made the recommendation that it’s what they think we should do (assuming that the family was OK with it). We reaffirmed that we were on board with that path, so signed the consent a couple of hours ago.
Feeling pretty good about that decision/step. There are several things that we are hopeful the dialysis will help (as we’ve discussed previously over email).
The dialysis will likely happen tonight (in next few hours) or in the morning. But, since there’s nothing critically urgent going on right now (potassium levels are not sky high or anything), they said that it doesn’t make much of a difference whether tis’ tonight or tomorrow.
They did say that we shouldn’t expect immediate results. It’ll take 3-5 days for the effects of the dialysis to show up. Do you agree with that time frame or are they just being conservative?
They’re going to start with “continuous” dialysis and then, as appropriate, shift to the other kind where they do dialysis a couple of times a day.
On the other front, things are relatively the same as yesterday. Kidney function still very low (almost zero production of urine today) — hence the dialysis. But, other vitals are the same or slightly improved.
The one new complication we’ve seen in the last 24 hours is that a resistant form of e-coli has shown up in the most recent culture. They’re hopeful that the antibiotics she is already on will be effective. They’re doing the culture “test” to see if we can expect it to be effective. They say it’ll take a couple of days for those results to come back.
One other change they’re making is to stop the Polymixin antibiotic. Their best sense is that it’s no longer necessary and there’s no reason to put her kidneys through the stress. We asked whether it made sense to stop that antibiotics given we were proceeding with dialysis and going to give relief to her kidneys anyways, but they said that antibiotics are generally not a good thing, and if they needed to restart it they could.
They did a CT scan and they said the first surgery is healing really well and the intestine “connection” is looking really good too. So, all seems OK on that front.
Thanks.
Robert
Recommended:
Hi Rob,
I think it’s good that they are starting Dialysis, the sooner the better.
With minimal to no urine output and kidney markers in the blood going off they shouldn’t be delaying this form of treatment from my perspective.
I believe you have made the right decision by giving consent to Dialysis.
In terms of effects there are two main effects that should be the result of the Dialysis
1) Reduce the “puffiness” and get your mother’s fluid balance corrected. She would most likely have a positive fluid balance accumulated in recent days with the kidneys failing. This is why you can visibly see the “puffiness”. Therefore the Dialysis machine will take off fluids and they will aim for a negative fluid balance over the next few days.
In a situation like this, the sooner they can get rid of excess fluids the better, at the same time if they take off fluids too quickly your mother’s blood pressure might go down and she might end up back on inotropes/vasopressors.
That’s why it’s also important to look at Albumin levels and replace Albumin if necessary. This will also help with correcting the imbalance in fluids as it will draw fluids from the cells back to the veins and arteries. This might also help with stabilizing her blood pressure
Recommended:
2) By starting the Dialysis machine the kidney markers Urea and Creatinine in the blood should be corrected.
Once Urea and Creatinine are back within normal levels the kidneys should start to produce Urine again.
Correcting the fluid balance and reducing the puffiness would most likely be priority without your mother’s blood pressure crashing and then getting the kidneys working would be next.
Also, in some situations the kidneys might still produce urine but not enough to clear all the fluids, hence the dialysis to correct a positive fluid balance.
I would also think that with your mother having had surgery recently her Haemoglobin (=red blood cells) would be low.
Replacing some Haemoglobin via blood transfusions might also help to stabilize her condition including reducing the puffiness.
As a rule of thumb, Intensive Care teams are always conservative in their outlooks. Therefore hopefully you can see results quicker than 3-5 days.
It really all depends how much fluid removal your mother can tolerate over the next 48-72 hours.
It’s normal in ICU to start continuous Dialysis as opposed to intermittent.
E-coli is concerning. Do you know where they located the E-coli? Is it in the abdomen or even in the lungs? Do you know what Antibiotics they are giving for it?
Generally speaking I agree that the more they can minimize Antibiotic use the better, irrespective of Dialysis use or not.
Any therapy in ICU that can be minimized is a good thing.
Waiting for the results to come back to see if Antibiotics are working make sense.
Related article/video:
I’m glad to hear she had a CT scan to check up on the surgery.
They wouldn’t be doing that if they think she was too unstable to even go for a CT scan.
Especially with previously being on 100% oxygen it would have been too much of a risk sending her for a CT scan.
Therefore she must be more stable generally as you pointed out.
I’m glad to hear that you sound more positive than yesterday!
Having a loved one critically ill in Intensive Care is often an emotional roller coaster and again it can be two steps forward and one step back.
It’s also often one day at the time. In your mother’s situation ICU is a marathon and not a sprint.
I hope that helps Rob!
Please let me know what else you need!
Wishing you and your family all the best!
Warm Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!