Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question where I featured another CASE STUDY and the case study last week was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another the next question from my client Robert, which are excerpts from email counselling and consulting sessions with me and the question this week is
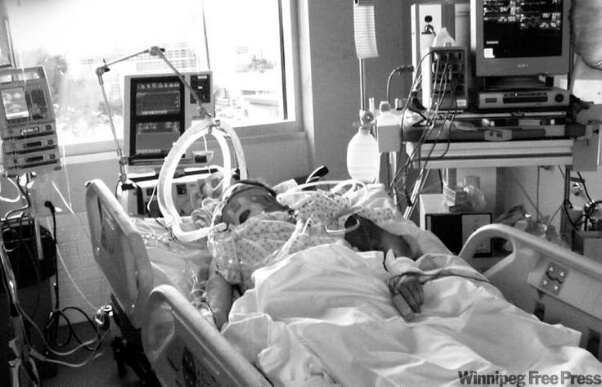
My 68 year old mother is in ICU with gastric perforation and she’s not “waking up” after the surgery! Will she need a tracheostomy? (PART 13)
You can find previous questions from this series of questions answered here
PART 1, PART 2, PART 3 , PART 4, PART 5 , PART 6, PART 7, PART 8, PART 9 and PART 10, PART 11 and PART 12
Robert continues with his mother’s situation below
Hi Patrik,
Here are the latest and updates and developments
1. They are watching her haemoglobin and her platelets closely. They gave her two blood transfusions yesterday (a unit each time). They just gave her platelets (6 units), which bumped the number up to 69 for a little bit, and then drifted back to 60.
2. They are giving her Fentanyl for pain. They are carefully managing the pain, and not being overly judicious with hold off on it. Though this impacts her ability to “wake up“, they think it’s the right thing to manage the pain.
3. For most of the day, she can stay off the bp meds(Inotropes/vasopressors). Every now and then (maybe once or twice a day), they have to give her a little bit, but it’s low or off completely most of the time.
4. The highest her white blood cell count has been was a couple of days ago (20,000). Was 18,000 yesterday and is 15,000 at last check today.
5. The dialysis is proceeding well. They’re able to put out about 100cc of fluid an hour.
6. Her complexion looks better than yesterday, but that just could be my imagination.
7. The doctors haven’t mentioned any issues and are not concerned with her liver in the conversation I had with them earlier today. But, will specifically ask at the next rounds in a few hours.
8. In the conversation I had with the attending doctor a couple of hours ago, she was very concerned about the bleeding. They’re not sure the bleeding has stopped yet. The blood coming out is darker, but she thinks that might be because it’s accumulating somewhere for a little while before it comes out, and that’s why it’s not bright red.
9. They said that if platelet count continues to drop and gets into the 10 range (vs. 30 it was at earlier today), then she’s at risk of spontaneous bleeding. The fact that she’s diabetic doesn’t help matters any.
10. They have taken her off the blood thinning medication she was regularly on — as her blood is thin enough already.
11. They took her off of the antibiotics Flagyl(Metronidazole) yesterday. Since there are no signs of major infection, they are looking into whether it’s advisable to take one of the other antibiotics off.
12. They’re being careful with her skin, especially as they turn her. They have air cuffs on her legs that are supposed to help prevent bed sores and keep some mobility there.
Your thoughts and comments are much appreciated.
Warm Regards
Robert
Recommended:
Hi Robert,
Please see my comments to your updates in red below
1. They are watching her haemoglobin and her platelets closely. They gave her two blood transfusions yesterday (a unit each time). They just gave her platelets (6 units), which bumped the number up to 69 for a little bit, and then drifted back to 60. > I’m glad to hear that they are transfusing her Platelets and red blood cells. Haemoglobin of 60is is very low and suggests major bleeding! A low Haemoglobin also doesn’t help with ventilation and oxygen dependency. To illustrate this, Haemoglobin is the oxygen binder in the blood, therefore the lower Haemoglobin levels, the less oxygen can be carried around the blood even if 100% of oxygen was being delivered. Therefore, giving red blood cells makes a lot of sense on many levels.
2. They are giving her Fentanyl for pain. They are carefully managing the pain, and and not being overly judicious with hold off on it. Though this impacts her ability to “wake up”, they think it’s the right thing to manage the pain.> Yes, Fentanyl will delay “waking up”. Pain management at this point in time still overrides the need to “wake up” especially if her breathing rate is >30 breaths/minute. One of the major side effects of Fentanyl is respiratory depression or inhibiting breathing efforts. It could cause major havoc letting your mother “wake up” with pain, she most likely couldn’t cope. Again, it’s a marathon not a sprint… “waking up” after an induced coma is a process not an event…
Furthermore, especially in acute kidney failure, Fentanyl is the preferred pain medication(Opioid) because Morphine can aggravate acute kidney failure.
Related articles/videos:
3. For most of the day, she can stay off the bp meds(inotropes/vasopressors). Every now and then (maybe once or twice a day), they have to give her a little bit, but it’s low or off completely most of the time.> That’s a good sign, especially in light of the fact of a low Haemoglobin. Most Patients in Intensive Care with major bleeding and low Haemoglobin have a low blood pressure and do need inotropes/vasopressors. Furthermore with the Dialysis, the fluid removal as well as the low Haemoglobin the likelihood for a low blood pressure requiring inotropes/vasopressors such as Norepinephrine/Noradrenaline and/or Epinephrine/Adrenaline is pretty high, therefore if she can stay off it for now that’s encouraging, considering her overall situation. I wouldn’t be surprised if she has to go back on it at some point.
4. The highest her white blood cell count has been was a couple of days ago (20,000). Was 18,000 yesterday and is 15,000 at last check today.> Good sign that it keeps coming down. It’s a sign that the infection is getting more controlled and also that her immune system is working.
5. The dialysis is proceeding well. They’re able to put out about 100cc of fluid an hour.> Another good sign that it’s working well, they may have to look at taking off more fluids, reason being that she will most likely get up to 100 cc/hour fluid intake with Nasogastric feeds or IV nutrition(TPN) plus Antibiotics and other medications running. Therefore, if she gets up to 100 cc/hour fluid intake, are they just keeping the fluid balance equal or are they taking off 100 cc/hour on top of what she’s getting. It might be a worthwhile question to ask to find out in which direction her fluid balance is heading.Also, the more aggressive they are in removing fluids the higher the likelihood of blood pressure going down and needing inotropes/vasopressors.
6. Her complexion looks better than yesterday, but that just could be my imagination.> I believe you should trust in your feelings and intuition and in what you see. You and your family know your mother! Also, with aggressive fluid removal via the Dialysis her looks would have changed by now from being “puffy”, oedematous and fluid overloaded to a more “normal” look.
7. The doctors haven’t mentioned any issues or concerned with her liver in the conversation I had with them earlier today. But, will specifically ask at the next rounds in a few hours.> I would definitely ask, if I was you, if liver failure can be ruled out great, but in light of Platelets dropping significantly there is certainly a chance of liver issues. Keep also be asking for her Albumin levels, especially since you have mentioned a few days back that they were draining abdominal fluidsI would also ask in regards to her Albumin level, again “puffiness” and being oedematous can be a combination of fluid overload and low Albumin levels. Low Albumin levels and a drop in Platelets can be related to liver issues. If they are not related to liver issues that’s great and you can rule it out, but then they need to investigate what else might be going on. Also, where do they think the abdominal fluids are coming from that they needed to drain?
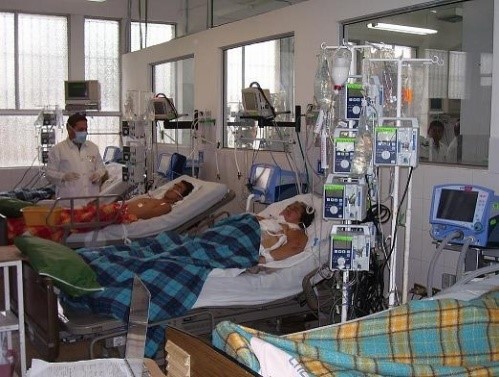
8. In the conversation I had with the attending doctor a couple of hours ago, she was very concerned about the bleeding. They’re not sure the bleeding has stopped yet. The blood coming out is darker, but she thinks that might be because it’s accumulating somewhere for a little while before it comes out, and that’s why it’s not bright red.> I’m very worried about the bleeding especially with a Haemoglobin as low as 60 and her Platelets <30. That suggests that there’s major bleeding going on somewhere. It’s probably a solid theory to suggest that the blood coming out being darker is sitting somewhere before it’s visible.You can also expect a slight drop in Haemoglobin because of the Dialysis machine running, because blood is being extracted out of the body and run through a filter.
9. They said that if platelet count continues to drop and gets into the 10 range (vs. 30 it was at earlier today), then she’s at risk of spontaneous bleeding. The fact that she’s diabetic doesn’t help matters any.> Correct and that’s why I believe they need to investigate why Platelets are so low, I.e. liver failure?
10. They have taken her off the blood thinning medication she was regularly on — as her blood is thin enough already.> Absolutely, I didn’t mention that because I assumed that’s what they would have done.
11. They took her off of the antibiotics Flagyl(Metronidazole) yesterday. Since there are no signs of major infection, they are looking into whether it’s advisable to take one of the other antibiotics off.> Good move if they’ve done that. It looks like infection markers are coming down.Keep in mind, any temperature she may have because of an infection will be “masked” as long as she’s on Dialysis because the Dialysis is extracting blood out of the body and is therefore cooling body temperature down.Therefore, keep an eye on the White Cell Count(WCC), because that’s another good indicator how she’ll be dealing with any infection, since the temperature will be masked whilst she’s on the Dialysis machine.
12. They’re being careful with her skin, especially as they turn her. They have air cuffs on her legs that are supposed to help prevent bed sores and keep some mobility there. > Skin would be extremely fragile after such a long stay in Intensive Care with being immobile, bed bound and critically ill. Furthermore, inotrope/vasopressor therapy with Noradrenaline/Norepinephrine would have made her skin constricted and even more fragile. Good and regular pressure area care is absolutely vital, as is good nursing care in general.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!