Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question in this series of questions from our client Robert and the question last week was PART 4 of
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next question from our client Robert, which are excerpts from email counselling and consulting sessions with me and the question this week is
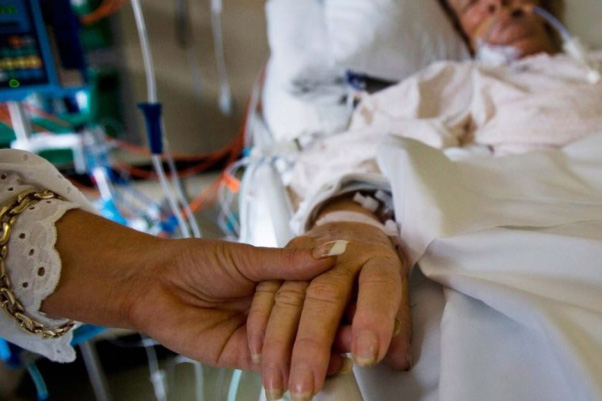
My 68 year old mother is in ICU with gastric perforation and she’s not “waking up” after the surgery! Will she need a tracheostomy? (PART 5)
Robert describes his mother’s situation as follows with those series of questions.
Hi Patrik,
Thanks for your note.
After having discussed this internally with the family, we’re inclined to proceed with the tracheostomy sooner rather than later (i.e. shoot for Wednesday, the day after tomorrow).
Rationale: We are emotionally past the point of trying to avoid the tracheostomy. If it turns out in a month or two that she’s completely off the ventilator and doesn’t need it, it’s a somewhat reversible procedure from our understanding. And, as you’ve noted earlier, it’s actually more comfortable to have the tracheostomy than be intubated. We are also a bit worried that this is already her third intubation in the last few weeks. There’s a chance that after extubation, she struggles again with her breathing.
We are also worried that the longer we wait, some other complication comes up (like another infection) thereby closing the window for a potential tracheostomy. So assuming the staff is OK with it, we’d like to make a strong request for Wednesday and not wait until Thursday/Friday.
Two questions on that front:
- How long does Keppra usually take to “wear off” a bit?
- How important do you think it is for an attending surgeon to do the tracheostomy vs. a resident? My leaning is to solve for timing/schedule instead of who does it, given the timeline and situation.
One other related set of questions. The hospital staff has asked what our position/decision is regarding:
- Dialysis (if it is needed)
- Chest compression (if it is needed)
Our position is that dialysis is OK and should be pursued but we likely don’t want to do chest compression (from what we’ve heard, it’s a last, desperate measure and very aggressive/violent).
Now, having said that, my leaning right now, in the situation we’re in, is to communicate that our position is “whatever means necessary”. This is primarily to show conviction and keep things simple as we work through what might be a potentially tricky situation this week. After the tracheostomy, we can always change our mind and communicate that we don’t want chest compression.
What do you think?
Thanks, as always.
Robert
Recommended:
Hi Robert,
I believe it is wise to proceed with the tracheostomy rather sooner than later as your mother will get the best of both worlds so to speak.
You are absolutely correct to point out that your mother already had three intubations in the last few weeks and hence another extubation(47) and then having the risk for another intubation is probably too high. Also, please keep in mind that for another intubation there would be sedatives and opiates needed too, similar to when a tracheostomy is being performed.
Related articles/videos:
The good news in all of this so far is that your mother’s heart continues to be strong, hence why she’s off the inotropes/vasopressors and she can therefore maintain a sufficient blood pressure for now. A strong heart is important during critical illness for a number of reasons, including avoiding Dialysis and I will come to that in a moment.
In some instances although not all, after a tracheostomy has been performed, Patients can be taken off the ventilator within 24-48 hours at least for a couple of hours to start off with and if they can tolerate the first weaning trial, the time off the ventilator can be gradually increased.
In some instances Patients can go from having a tracheostomy to coming off the ventilator straight away.
One of the biggest risks for complications that I can see is her prolonged time on the ventilator with a breathing tube and hence there is an increased risk for a chest infection/Pneumonia, therefore again I strongly believe the tracheostomy is the quickest way to minimise that risk from my experience.
Her conscious state and still not “waking up” is of course still a concern, but I keep referring back to the CT scan and the MRI scan of the brain which I believe showed no brain damage, therefore if no other neurological complications occur, there is a very high likelihood of your mother “waking up” in her own time.
Recommended:
You mentioned that she had a stroke in the past, hence the Keppra and I assume it would have been a mild stroke otherwise she wouldn’t have been able to travel to Brazil?
The half-life for Keppra is 7 hours +/- 1 hour and it’s being excreted by the kidneys.
From my experience and from all the information that I have thus far, your mother not “waking up” yet is a combination of being sedated on and off for quite some time and she would have also had either Morphine or Fentanyl intravenously for pain relief while she was or still is intubated and that delays “waking up” as well. I would be curious to know if she’s still getting either Morphine or Fentanyl intravenously for pain relief, not only to tolerate the breathing tube but also to deal with the abdominal pain after surgery.
Now looking at who should be doing the tracheostomy.
I actually think it’s great that either the surgeon or the resident is doing the tracheostomy. The reason I’m saying this is that in the “old” days in ICU tracheostomies were performed in the operating theatre and nowadays in most ICU’s worldwide a qualified and experienced ICU consultant is doing them. That’s OK, however doing a tracheostomy is still a surgical procedure and hence if a surgeon or their registrar is doing it I think that’s fine. Especially since a fully qualified surgeon is overseeing the procedure I would have faith that this would be going smoothly. I remember in the recording the surgeon was saying that the anatomy of your mother might be an issue, that’s’ why they might have gotten the surgeon on the case in the first place.
To your other questions.
Yes to Dialysis and yes to Cardiac compressions.
Your mother’s heart is beating strong, making it less likely for her needing dialysis. Dialysis is needed for kidney failure and kidneys can fail in ongoing severe sepsis and during prolonged low blood pressure.
The Sepsis she seems to fight Ok for now and therefore hopefully she won’t need dialysis for kidney failure.
With the heart being so strong thus far(unless there is a heart condition that I don’t know of) I would strongly advocate Cardiac Compressions(CPR) especially in light of the fact that the ICU team has mentioned “withdrawing treatment” at some stage.
By you stating that you want full treatment including cardiac compressions, you are keeping all your options open thus far and you are showing the team that “withdrawing treatment“ at this point is not an option for you and your family.
And as you have correctly pointed out, you can always change your position down the line.
I hope that helps Robert.
Warm Regards
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!