Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question last week was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next question from one of our clients which are excerpts from email counselling and consulting sessions with me and the question this week is
My 68 year old mother is in ICU with gastric perforation and she’s not “waking up” after the surgery! Will she need a tracheostomy? (PART 1)
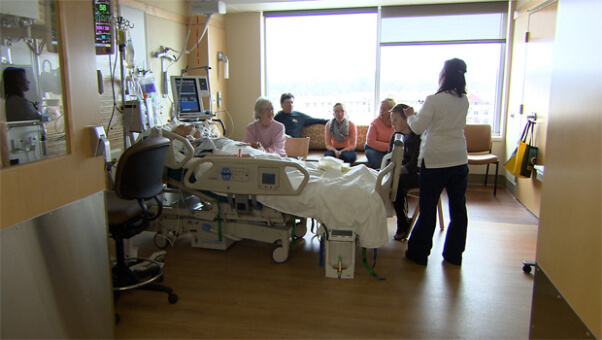
Today’s episode will start another great series of questions from one of our clients who was in a very stressful and difficult situation after his 68 year old Mom was admitted to Intensive Care for a prolonged period!
This was another complex situation that my client and their family had to deal with and I was able to explain things in detail to them so that they could make sense out of the situation.
In the end the client felt well supported and they felt that they were able to make informed decisions, get peace of mind, control, power and influence!
My Client Robert details his mother’s situation as follows
Hi Patrik,
- My mom (who lives in the USA) was travelling in Brazil (which is where she’s from).
- During her time there, she had a medical emergency (her blood sugar level dropped dangerously low — to about 20).My father took her to the nearest hospital on October 5th, but our home in Brazil is in a small town, so the quality of the hospital is not great.She was intubated that day and put under sedation.
- My father took her to the nearest hospital, but our home in Brazil is in a small town, so the quality of the hospital is not great.
- The hospital elected to intubate her because she was having trouble breathing.
- Both my two sisters and I flew to Brazil from the U.S. to help with the issue.
- We first transported her from the smaller town hospital to a much better hospital in Rio De Janeiro on October 10th. But even that hospital was not near the quality we would find here in the U.S.She took approximately 4 days before she showed any responsiveness after being taken off sedation. At that time, she was able to open her eyes at command and respond via head nodding.The primary issue at that time was a lot of secretions in her mouth that had to be manually suctioned out every hour or so. They were worried that fluids would seep into the lungs and cause Pneumonia.There was no definitive diagnosis, but the issue she was dealing with was paralyzed or highly-weakened vocal chords, this prevented her from swallowing, she couldn’t talk, etc. Suspicion is that the intubation at the first hospital may have been rough, thereby damaging the vocal chords.
- Ultimately when she was stable enough, we air evacuated her from Rio back to the US and checked her directly into one of the top leading ICU’s where we live in the US. During the trip (at a layover in Mexico City) she had to be intubated again.On October 24th, she began a medevac journey via private plane from Rio back to the US. En route (shortly before a layover in Mexico City), she was having some breathing issues. Doctors decided to put her in an ICU in Mexico City overnight to let her rest and stabilize. They re-intubated her then. The remainder of the trip from Mexico City to the US(Seattle) went without incident.Upon arrival, she was checked into ICU in Seattle. Still somewhat non-responsive, but was just starting to show signs of coming out sedation and waking up on October 29th.On November 3rd, she showed signs of struggled breathing and they decided to intubate her (this is the third time). Later that same day, doctors informed us that she needed emergency surgery because they had found air in her abdominal cavity and they suspected she had a hole in her stomach or intestines. (That was later confirmed to be true). Surgery was performed early morning on November 5th. The surgery went well, they were able to “patch” the hole, and added some fat tissue to bolster the patch.Since November 7th, she’s been up and down. Started with need for high dose of blood pressure meds. Eventually had a spiked fever (104F/ 40C). She’d show signs of improvement (no fever, blood pressure meds/inotropes/vasopressors almost off, improved breathing, etc.) but then relapse again.
Current situation: They think she has another infection/Sepsis. They are running out of options in terms of which antibiotic to use, because she’s already on a mix of 5 different antibiotics based on the cultures they’ve been taking. New development yesterday was a lot of fluids coming out of her stomach tube (which was not happening before).
So right now, I think doctors are first trying to figure out how to treat the infection/sepsis. The non-responsiveness part (I’m guessing) will come later.
My first question is
- She’s basically been out for 7 days now. A couple of days ago, we could get some response from her if we pinched her or when they were shifting her in the bed. She’d open her eyes briefly, could nod her head in response to some questions.
My next question is:
- As of today, she’s taken a turn for the worse. Fever is back, and blood pressure has gone down so she’s back on blood pressure medications/inotropes.
Many thanks for your wonderful website and for all your help!
Robert
Recommended:
Hi Robert,
Thank you Rob for detailing your Mom’s situation and the challenges she and your family are currently facing!
It really sounds your mother and your family have been dealing with an somewhat unusual and also challenging situation, especially with having to fly your mother from one country to another whilst being critically ill.
To answer your first question, “She’s basically been out for 7 days now. A couple of days ago, we could get some response from her if we pinched her or when they were shifting her in the bed. She’d open her eyes briefly, could nod her head in response to some questions.”, the following applies
Given your mother has been in an induced coma for a few days in Brazil and it took her a while to “wake up” and given that your mother has been in an induced coma for another 7 days since admission to ICU in Seattle(USA), including emergency surgery where she had more sedatives and opiates(=pain killers) you are describing a “normal” process.
Related article/video:
“Waking up” after an induced coma can take time and most importantly they have already done an MRI and EEG of the brain and they have determined that there is no brain damage, therefore “waking up” after the induced coma can just take time and you may take comfort in the fact that your mother came out of the induced coma in Brazil with a delay.
Therefore give her time, a positive environment, nurturing and also know that the critical illness in and of itself will delay “waking up”.
Furthermore, the hole in her stomach(=gastric perforation) is quite a severe and concerning event and will have caused an infection or sepsis and sepsis in general terms will cause a further delay in “waking up”.
I have seen that you have purchased the Ebook/2 Videos
And this resource will give you some very good insights about what to expect with your mother not “waking up” after the induced coma.
You may also look at this resource here and it’ll also give you lots of insights how to deal with this challenging but also quite common situation when it comes to critically ill Patients not “waking up” after an induced coma
Looking at your next question, “as of today, she’s taken a turn for the worse. Fever is back, and blood pressure has gone down so she’s back on blood pressure medications/vasopressors/inotropes.”, the following applies
Now, as for the hole in your mother’s stomach(=gastric perforation), it is causing abdominal sepsis, which is probably one of the worst forms of sepsis there is.
To put things in perspective, a critical illness causes the body to go into “stress mode” which triggers certain events, including the release of a stress hormone called cortisol (“fight and flight”) as well as increased acid production in the stomach. The PH goes up in the stomach with the increase in acid and therefore making it more likely to get a hole in the stomach(=gastric perforation).
This has been well known and well researched in the Intensive Care/Critical Care community and is usually managed with early feeding via an NG tube and medications such as Pantoprazole/ Esomeprazole (also Ranitidine) Proton pump inhibitors to reduce acid production in the stomach.
It could have been that this would have gone unmanaged in the early days in ICU in Brazil, however managing and preventing increased acid production in ICU should be early standard treatment.
In the early days of Intensive Care/Critical Care treatment, lots of critically ill Patients had gastric ulcers develop with a stomach perforation.
Part of being septic in Intensive Care is to become severely hypotensive(=low blood pressure) and hence needing high amounts of inotropes or vasopressors(=Blood pressure medications).
Fever, high Lactate levels and an increase in White cell count(WCC) and CRP in the blood are early markers of a septic shock or a “septic shower”.
Stay strong and positive for now Robert and let me know what you need guidance with!
Kind Regards
Patrik
PS: you can read/watch the follow on questions from my client Robert here PART 2, PART 3, PART 4, PART 5, PART 6, PART 7, PART 8, PART 9, and PART 10
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!