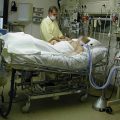
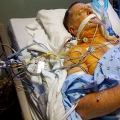
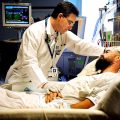
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
When is the Best Time to Do a Tracheostomy on My Ventilated & Sedated Mom in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Marsha, as part of my 1:1 consulting and advocacy. Alexa’s mom is with a breathing tube and on a ventilator. Alexa is asking if her mom will benefit from a tracheostomy in the ICU.
Will My Mom Benefit from a Tracheostomy in the ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Alexa here.”
Dr. Levi: Correct. Usually, she’s good when … And it’s been happening since she’s on hemodialysis. So, usually, she’s good on the days she’s not getting hemodialysis. She’s okay on the continuous ventilation. It’s always the days when she’s getting the hemodialysis, it’s a little bit worse. But after the hemodialysis, she’s back on continuous ventilation, and she’s okay.
Patrik: And the atrial fibrillation-
Dr. Levi: Sorry. You were wondering about the atrial fibrillation?
RECOMMENDED:
Patrik: Yeah, just going back to that for one second, that was a one off. It’s not an ongoing issue now it’s under control with Metoprolol?
Dr. Levi: Correct.
Patrik: Right.
Dr. Levi: Yeah, that was just one time.
Patrik: Yeah. Thank you.
Dr. Levi: You’re welcome. Her lungs right now, her blood gas is okay. She’s not fighting acidosis or alkalosis, and her last count is 28, so it’s good too.
Patrik: Right. That’s good.
Dr. Levi: So, we talked about the kidneys. Like I said, every time she’s not getting dialysis, all of her blood work is increasing temporarily until she’s getting the dialysis again. The other thing, depending on the day, sometimes she’s having temperature, and other times not.
Dr. Levi: Yesterday, she was not febrile, but today she’s getting a temperature again of 38.4, with her white blood cells increasing a little bit and her neutrophils increasing a little bit too.
Dr. Levi: Again, we did cultures, everything is getting back negative, except the Candida, but just localized in the lungs. So, that’s why she’s not on any antibiotics right now. We are just following that. We’re more thinking about an inflammatory process going on.
Dr. Levi: But for sure, if her temperature is going to increase again, and not going back down. The microbiologist, who is their specialist, so we’re thinking about maybe putting an antifungal type of medication.
Patrik: Yes, I was just about to say with Candida in the lungs, would that trigger some anti..
Dr. Levi: Yeah, it’s not unusual with a patient being intubated for a long time.
Patrik: Oh yeah, for sure.
Dr. Levi: … usually we don’t treat it if it’s just localized in the lungs. For example, if it was in the bloodstream, then for sure we would treat it. The specialist is thinking about it.
Patrik: Yeah, for sure.
Dr. Levi: I’m trying to not destabilize her immune response, so that’s why we’re holding off for now.
Patrik: Yeah, that’s fair enough. What’s her white cell count?
Dr. Levi: I’m sorry?
Patrik: What is her white cell count?
Dr. Levi: So, it was 13.4.
Patrik: Okay. All right. Not too high.
Dr. Levi: Yeah. No, yesterday was 10, and her neutrophils are 11.2, yesterday it was 8.
Patrik: Right. And her hemoglobin is stable?
Recommended:
Dr. Levi: Yeah, her hemoglobin is 74. She did have a transfusion weeks ago, because her hemoglobin went down to 68. But since then, they’ve just been stable. For sure, she’s on the EPREX, that medication to kind of produce the red blood cells.
Patrik: Red blood cells, yeah.
Dr. Levi: She’s had that for long term, just because it’s been a chronic problem.
Patrik: Right. I was just about to ask why is her hemoglobin so low.
Dr. Levi: She’s not bleeding from anywhere, we checked, so there’s no bleeding or breakdown or anything like that. There’s no blood in the tube. So, there’s no blood anywhere. So, we know she’s not losing blood.
Dr. Levi: At first, there was a problem with volume as well, but now that we have removed all of that extra volume, there’s no other sources, and we’re just following it. The EPREX is just to make sure that, in our bones, that’s where we’re producing those red blood cells, to make sure that it’s stimulating.
Patrik: Yeah. And what ventilator settings is she on at the moment?
Dr. Levi: So, right now, let me just check to make sure.
Patrik: Thank you.
Dr. Levi: Just give me a second, just to see that it was not changed. Yeah, so right now, that’s on the spontaneous ventilation. And she’s got inspiration of 40, and oxygen of 35%.
Patrik: 35%? Okay, that’s pretty good.
Dr. Levi: Yeah, that’s not bad. That’s not bad, yeah. And an expiratory pressure, like the peak, of 60.
Patrik: Okay, that’s pretty low.
Dr. Levi: Yeah, that’s pretty low. And like I said, even though the ARDS is there, we’re not worried from a long perspective. It was more the kidneys and the brain that we were worried about here.
Dr. Levi: There was three things I wanted to discuss with you today. Just because I know there’s kind of three alternatives, and depending on which alternative we decide to follow, it will change a little bit what we’re doing. That’s why I wanted to talk to everyone, because it depends on what the family is okay to have at the end.
Dr. Levi: Sorry, I’m going to try to make myself clearer. So, the first alternative, either way it’s going better. But we’re not sure how bad she’s going to be, if she’s going to be in bed for the rest of her life, with a feeding tube, depending on the ventilator. That’s the first alternative.
Dr. Levi: The second alternative is that she never wakes up better than that, but we just prolong her life on the machines we have. And yeah, the last alternative is waiting. I know yesterday, I think Alexa talked to one of my colleagues, and they were discussing about a miracle. But again, it’s always possible, but it depends on how long we want to wait for that miracle.
Suggested links:
Dr. Levi: And the last alternative to say, “We’ve done everything we can so far, she’s not getting better,” and to just make her comfortable. If we decide to continue ahead, the two things we need to do at this point, because it’s been a month, is that we will need to remove the breathing tube from her mouth, and put it in her throat, a tracheostomy.
Patrik: Yeah, the tracheostomy.
Dr. Levi: Correct. The other thing is that we will need to remove the feeding tube from her mouth and put it, what we call a gastrostomy.
Patrik: A PEG, yeah. A PEG tube.
Dr. Levi: Correct. So, that would be just the two surgeries we would need to do. Just because it’s been a month, and we cannot continue that, like usually after a month we remove them.
Patrik: No, I understand that.
Dr. Levi: And for sure, the other thing we wanted to make sure is about the reanimation, what we wanted to do. I know we discussed it a little bit at the beginning of the week, and there was a lot of emotion involved, but they’ll be okay and think about it.
Dr. Levi: We just wanted to make sure if we do reanimate, if something were to happen and her heart were to stop, to put her through a reanimation. Sometimes, we can break chest bones, and it could happen her heart isn’t going at that point, so it depends. It’s always a question basically of quality versus quantity.
Patrik: Of course.
Dr. Levi: So basically, those were the points I just wanted to mention today to see where we were at today.
Patrik: No, that’s good and I understand all of that. I understand tracheostomy, PEG (Percutaneous Endoscopic Gastrostomy), DNR (Do Not Resuscitate), the consequences of doing tracheostomy, PEG, consequences of doing resuscitation, or not doing them.
Recommended:
Patrik: I can talk about that offline with Alexa as well. But a quick other question there, with the ventilation in particular. So, when she’s in a spontaneous ventilation mode, she still goes back in a controlled mode here and there? Or has she been in a spontaneous mode now for hours or days?
Dr. Levi: So, like I said, so today we had the hemodialysis. So, we’re always switching back and forth. I think today, even though she was maybe in bronchospasm, I don’t think we have to switch her back today, but I know we had to switch her back two days ago. So, let me just check in my notes to make sure.
Patrik: Thank you.
Dr. Levi: The last time she was in PRVC (Pressure Regulated Volume Control). So, the last time she was in PRVC was yesterday at 6:40 in the morning.
Patrik: That’s good.
Dr. Levi: And after that we were able to put her back into spontaneous ventilation at 9:00 yesterday morning.
Patrik: Yeah. And you’re doing venous gases at the moment, no arterial gases?
Dr. Levi: Correct. We’re doing just venous, just because she’s been okay from that perspective. Like in saturation, she’s always okay. So, we didn’t feel the need to do arterial blood gas.
Patrik: And is there anything you do for the ARDS (Acute Respiratory Distress Syndrome)? I mean, some people on ARDS, I’ve seen Methylprednisolone. Some people on ARDS, I’ve seen nitric oxide. She would probably be beyond the nitric oxide stage by the sounds of things.
Dr. Levi: So, sorry you were talking about nitric oxide? I missed your reference, I’m sorry.
Patrik: Sorry if I wasn’t clear. I said, with the ARDS, is there something you’re doing there specifically at the moment with the ARDS?
Dr. Levi: Not really, because sometimes when the ventilation pressure is higher up, sometimes we have to put them in a central position, use other medications. But for her, because the venous blood gas is okay and oxidation too, we don’t have any indication to do more.
Patrik: Yeah, understood.
Suggested links:
- I’m Very Grateful That I Found You! Your work saves Many Lives When ICU Prefers To Kill The Very Ill
Dr. Levi: The only thing that is keeping her basically, the fact why she is dependent on the mechanical intervention is just because she’s not waking up. So, we don’t have any contact, and that’s why we cannot remove the breathing tube.
Patrik: Yeah. Understood. And everything else, like she’s absorbing her feeds, her opening bowels, there’s no issue there?
Dr. Levi: No. Actually, I know last time we talked, on Tuesday, I was talking about her liver. The liver enzymes were increasing a little bit, and we’re worried about a liver failure. But it’s actually been stable since then, so it’s not been increasing anymore, it’s just stabilized. So, from that point of view it’s actually okay, she’s stable right now.
Patrik: Right. And just briefly, you mentioned earlier you’ve done a CT scan of the brain, you’ve done an EEG. And that’s been reviewed by a neurologist? Or is ICU dealing with that directly?
Dr. Levi: Yeah. So, we asked a consultation in neurology, they actually saw her last week. The only thing that we cannot explain so far, we always get a response from the right side, but on the left side she still doesn’t have any pupillary reflexes.
Patrik: Right, I see.
Dr. Levi: So, that’s not a dramatic state, and even though we understand there was nothing there on the right side, to see the brain itself, but we didn’t see any big thing explaining why she wouldn’t have any pupillary reflexes there.
Patrik: Yeah, I see. Okay. Look, I don’t have any other questions so far. I mean, it sounds like a situation that we’ve probably all seen many times in ICU, I guess. Alexa, is there anything else you would like to ask?
Alexa: No, I pretty much followed the whole conversation. I understood actually a lot where we are for today, like the direction in terms of what the family wants to do. So, I’m going to just basically have that discussion, Dr. Levi, with Patrik.
RECOMMENDED:
Alexa: And then I’ll be able to then have that discussion with my family, based on my discussion with Patrik. And then from there, I can talk to you and then we’ll definitely have a direction or two of where we want to take things.
Dr. Levi: Okay, it sounds good. And I don’t want to put any pressure, the only thing I would have to know for tomorrow is, because we have an OR available tomorrow to do the tracheostomy. So, I don’t want to put pressure, but we can totally postpone it, it’s just for now it’s open. So, if you want to go ahead, it’s up to you.
Alexa: Okay. Would I be able to call you back in a couple of hours, if that’s fine, with the answer for that?
Dr. Matil: Yeah.
Alexa: Okay, thank you, Dr. Levi.
Dr. Levi: For me, I’m here until 9 o’clock tonight, but there is a colleague that will take my shift after that. So, if you want to talk with me, I’m here until 9. Otherwise, it would just be another one of my colleagues.
Alexa: Okay, that’s fine. Thank you once again.
Patrik: Thank you so much. Thank you.
Dr. Levi: Okay. Any more questions for me?
Patrik: No, I don’t have any more questions.
Dr. Levi: All right. Well, you’re very welcome and
Patrik: Thank you so much.
Dr. Levi: … sounds good. I’ll just wait for you.
Patrik: Thank you so much.
Dr. Levi: Thank you very much.
Patrik: Really appreciate it.
Dr. Levi: Thank you, bye.
Patrik: Thank you. Bye. Bye.
Dr. Levi: You’re welcome. Bye.
Patrik: Thank you, bye. Are you there, Alexa?
Alexa: Patrik?
Patrik: Are you there?
Alexa: Yeah, yeah. So, I’ve hung up with the hospital now, so it should-
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!