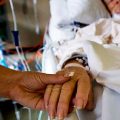
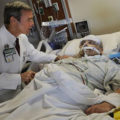
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Can I Become the Best Advocate for My Critically Ill Mom in the ICU?
You can check out last week’s question by clicking on the link here.
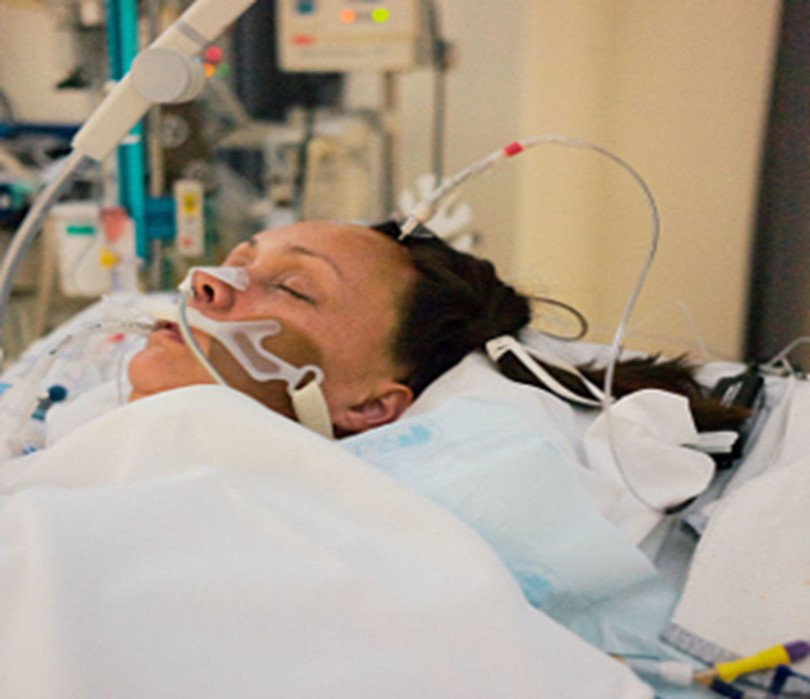
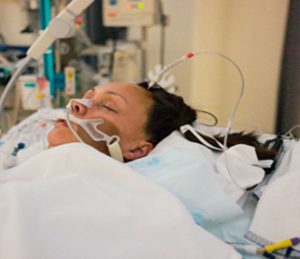
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Alexa, as part of my 1:1 consulting and advocacy service! Alexa’s mom is sedated and ventilated in the ICU. Alexa is asking when is the best time to do a tracheostomy on her mom.
When is the Best Time to Do a Tracheostomy on My Ventilated & Sedated Mom in the ICU?
Patrik: Intensive Care Hotline, Patrik speaking. How can I help you?
Alexa: Hi, Patrik. It’s Alexa.
Patrik: Hi, Alexa. Can you tell me more about your mom’s situation? So that I can guide and help you.
Alexa: We appreciate your guidance, and hopefully we can be advised by this.
RECOMMENDED:
Patrik: Yeah. Just give me another quick summary. So, she’s been in ICU now for how long again?
Alexa: Almost two months.
Patrik: Almost two months. And she still doesn’t have the tracheostomy, does she?
Alexa: No. So, today when I spoke to the doctor this morning to schedule the call. He mentioned that there’s an opening for a tracheostomy for her tomorrow.
Patrik: Okay, and how do you feel about that?
Alexa: I find it strange, because the last time when I had met with all the doctors, they were sort of pushing towards that not being an option, just because her organs were failing. They were explaining that her kidneys aren’t doing well, and her liver started to show some weakness, and her lungs weren’t doing that well either.
Alexa: And so, I just thought that there was no point in getting that done. And then yesterday, when I had gone to spend some time with my mother, I found out that she was moving on her own, and then also the respiratory therapist told me that there’s an improvement in her breathing as well.
Alexa: So, I don’t know if these doctors, they have their own agenda and they’re just using statistics, and they’re really trying to push me in a certain direction. And that’s what I really want to be able to uncover. Because if the information, or if my mother is showing some signs of improvement, then of course I would like to try for her to go on the tracheostomy.
Patrik: Right, okay. And just remind me, because I’m talking to a lot of people, she went into ICU for COVID?
Alexa: No, no, no, no. She had pneumonia.
Patrik: Pneumonia.
Alexa: Yeah. She had pneumonia, and then she was sedated because she couldn’t breathe. And they had to put her on ventilator support, that was because of pneumonia. And then afterwards, like four weeks later, they started dialysis, and they stopped the sedatives last week on Saturday, and she still hasn’t woken up.
Patrik: Yeah, okay. Okay, and they were asking for DNR (do-not-resuscitate), but you have not agreed to that?
Alexa: No, I have not agreed to that right now.
Patrik: Yeah, okay. All right. Okay, let’s dial this man. It’s a man, isn’t it?
Alexa: Yeah. Okay, so his name is Dr. Levi, and then what I’ll do is, I’ll just conference you in right now. It’s going to go through the automated system and then we’ll transfer into the ICU. And then I’ll ask for him, and I’ll just introduce you quickly. Okay?
Patrik: Yeah.
Alexa: I’ll just mention that you are overseas at the moment, or whatever, and that’s why-
Patrik: I wouldn’t even mention that. It’s irrelevant. Completely irrelevant.
Alexa: Okay, okay.
Patrik: My location is completely irrelevant.
Alexa: Okay. So, then once I introduce you, then you can just go ahead and take over the call.
Patrik: Yeah, okay. Thank you.
Alexa: Okay. And then, Patrik, can you call me back after the call to give me your insights about your conversation with the doctor?
Patrik: Oh, absolutely. Absolutely. Absolutely.
Alexa: Okay, very well. So, let me go ahead and make the call now. They’re waiting.
Patrik: Thank you. Thank you.
Alexa: Okay, hold on.
Alexa: Patrik, are you on the line?
Patrik: Yeah. Yeah.
Suggested Links:
Alexa: Patrik?
Patrick: Yeah, I’m here. I’m here.
Dan: Hi, this is Dan. What can I do for you?
Alexa: Yes, hi. This is Alexa. I am the daughter of Mrs. Santos who is in room number six, and I have a call with the doctor today, Dr. Levi, so can you-
Dan: Yeah, I will connect the call to him.
Alexa: Thank you.
Dr. Levi: Hello?
Alexa: Yeah, hi Dr. Levi, this is Alexa. How are you?
Dr. Levi: Hi, I’m good, thank you. And you?
Alexa: Yeah, I’m doing good. So, sorry we’re just a few minutes late, but I have Patrik on the phone with me right now. And Patrik, that’s Dr. Levi. Patrik, can you hear me?
Patrik: I can hear you. I can hear you.
Alexa: Okay, very well. Okay, so I’ll let you go ahead now, and you can speak with him directly.
Patrik: That’s wonderful.
Dr. Levi: Okay. Hi, Patrik, it’s Dr. Levi. I’m one of the residents taking care of Mrs. Santos for the past week.
Patrik: Yes, that’s wonderful. Thank you so much.
Dr. Levi: You’re welcome. I was wondering maybe … I don’t know what you know so far, and maybe you can just let me know, so we can start from there.
Patrik: Yeah, look, I guess I have the information from Alexa obviously. Her mom’s in ICU with pneumonia, has been on the ventilator for the last seven weeks, from what I understand. Has been heavily sedated up until last week.
Patrik: Has been on dialysis for the last couple of weeks, from what I understand. She’s now not waking up since the sedation has been stopped. I know there has been talk about a tracheostomy. I’m just trying to help Alexa and her family what are the next steps.
Patrik: Just a little bit about me, I’ve worked in ICU for over 20 years, I’m a critical care nurse by background, so that’s where I might come in. Just trying to help them work through the clutter that-
Dr. Levi: Okay, perfect.
Patrik: … for health professionals in ICU is bread and butter, but obviously for families, it’s not. And just-
Dr. Levi: Perfect. Maybe I can just give you … Oh, sorry.
Patrik: Yeah. No, go ahead. Go ahead.
Dr. Levi: I can just give you maybe a little bit of a summary of where we’re at right now.
Patrik: Thank you. Thank you.
Dr. Levi: Today, we’re day 38 in the ICU. She’s been intubated since the 8th of February.
Patrik: Right.
Dr. Levi: She’s been pretty much dependent on mechanical ventilation, due to multiple reasons. So, at first, it was because of pneumonia, and then she developed what we call ARDS (acute respiratory distress syndrome).
Patrik: Okay, she got ARDS. Okay. Yeah.
Dr. Levi: And then she got some water on her lungs that we needed to drain for that.
Patrik: Like chest drains?
Dr. Levi: Yeah, so she was being chest drained from both sides.
Patrik: For pleural effusions?
Dr. Levi: And actually, for that … Sorry?
Patrik: For pleural effusions?
Dr. Levi: Correct. Correct. So, she was having a pleural effusion on both sides. So, we tried to clamp it yesterday, and actually it’s been 24 hours without no re-accumulation of those pleural effusions, So, we actually have removed one of those drains today, on the right side.
Dr. Levi: We just kept the one on the left side, just because of this security situation, just in case something happened. But if, on the lung perspective, if there’s no re-accumulation tomorrow, we’ll remove the other drain.
Patrik: Right. Mm-hmm. Yeah.
Dr. Levi: Regarding her ARDS, it’s still there. So, we’re explaining the situation with the lung to the family. Every time, from the lung perspective, every time she’s having dialysis, so now it’s every two days, she’s having issues with the ventilator.
Patrik: Right okay. Mm-hmm.
Dr. Levi: Sorry?
Patrik: No, no. I’m just acknowledging. I’m just acknowledging.
Recommended:
- Quick tip for families in ICU: Do you know all treatment options available for ur loved one in ARDS?
Dr. Levi: Oh, okay, sorry, sorry. So, today was a bit harder on her ventilator, but every time it’s the same. So, every time she’s on dialysis, she’s having some bronchospasm from the procedure. So, that’s why every time she’s on dialysis, she needs a little bit more Ventolin and sometimes bolus of ketamine to open her lungs.
Patrik: Bolus of what?
Dr. Levi: Ketamine.
Patrik: Oh, ketamine. Okay. Yeah, yeah. Sure. Mm-hmm.
Dr. Levi: Just because she’s been responding well with ketamine for the bronchodilator, the side effect of the medication. But actually today, we didn’t need … We just put the Ventolin every hour, or as needed. So, now she’s done dialysis, so actually, now she’s okay.
Dr. Levi: But we have just realized that every time she’s on dialysis, it’s a little bit harder. Last week, she had an episode of atrial fibrillation on dialysis. That was resolved with just one dose of metoprolol IV.
Patrik: Right. Not a potassium issue with dialysis, potassium dropping, and then going into AF (atrial fibrillation)?
Dr. Levi: Yeah. So, for her, every time we’re not giving her dialysis, her creatinine is increasing, as well as her uremia. So, before the dialysis, her uremia was up to 60s, but now it’s around 15. Every time she’s not getting dialysis, it’s increasing to 30s, and then with the dialysis, it’s going down again.
Dr. Levi: For her, it’s not so much of a potassium issue, it’s more of a hyperphosphatemia issue, and the magnesium. So, every time she’s not getting dialysis, the magnesium and the phosphate are getting high.
Dr. Levi: And yeah, every time she’s not getting dialysis, she’s not peeing really. So, she’s really dependent on dialysis to pee, and to remove that extra fluid. Since the beginning of dialysis, she lost around 10 liters of water.
Dr. Levi: So, now she’s not over-flowed anymore, because we were able to remove the extra load of water. So, we were hoping that, with removing all of that water, it would resolve her issues with her peeing, but it’s not really.
Dr. Levi: So, for sure, in the long-term, depending on what we decide, it will be dependent on the hemodialysis, if ever she’s getting out of that episode. The other thing that we were worried about is her brain.
Dr. Levi: So, for her, we’re thinking, for sure there’s the component of her liver. I know they were thinking about hepatic encephalopathy before, and I’m sure there was a component of uremia, like uremic encephalopathy on top of that.
Dr. Levi: We did a CT (computed tomography) scan just to make sure there was no infarct of the brain or anything like that. There was none. We also did an EEG (electroencephalograph). The EEG showed that there was electrical activity, so we know she’s not brain dead.
Dr. Levi: The only thing that was worrying for us, since we started the sedation on the 30th, we only had brain stem reflexes, so she was only either in extension or in flexion, when we were doing DTR (deep tendon reflexes).
Patrik: So, her Glasgow Coma Scale, not above a five or a six. Is that basically what you’re saying?
Dr. Levi: I’m sorry? I missed-
Patrik: I said her Glasgow Coma Scale, her GCS would be not above five or six.
Dr. Levi: So, she’s always at E (Eye) 1, because she’s never opening her eyes and V (Verbal) 1 because she’s intubated. Today was an M (Motor) 3, because she was in flexion. Sometimes the motor response, it’s between an M (Motor) 3 and an M (Motor) 4, because during dialysis when she’s combative against the ventilator, we see some flexions, and it’s hard to differentiate between a 3 or a 4.
Suggested Links:
Patrik: When she’s combative against the ventilator, do you put her back in sedation? Or do you change the ventilator settings? What do you do if that happens?
Dr. Levi: Yeah. So, at first, we were just changing the ventilator setting, so she was always in continuous ventilation, and when this happened, we put her back to Pressure Control Ventilation (PCV) continuous pressure. The other thing, so we tried to not give her sedation, to make sure that she emerged, and to prevent accumulation of sedation in her body.
Dr. Levi: So, for now, she’s just on a profusion of fentanyl. Before today, she was in 12 cc (cubic centimeter) per hour, we had to increase it to 15 today, just because she was combative, and we gave her a bolus tube. So, she had a bolus of fentanyl of 50 to 100 mcg.
Patrik: Right, sure. Sure. Yeah, okay. And her fighting against the ventilator, that’s not a new thing, that’s an ongoing issue.
RECOMMENDED:
Dr. Levi: Correct. Usually, she’s good when … And it’s been happening since she’s on hemodialysis. So, usually, she’s good on the days she’s not getting hemodialysis. She’s okay on the continuous ventilation. It’s always the days when she’s getting the hemodialysis, it’s a little bit worse. But after the hemodialysis, she’s back on continuous ventilation, and she’s okay.
Patrik: And the atrial fibrillation-
Dr. Levi: Sorry. You were wondering about the atrial fibrillation?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!