Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Will My Mom Benefit from a Tracheostomy in the ICU?
You can check out last week’s question by clicking on the link here.
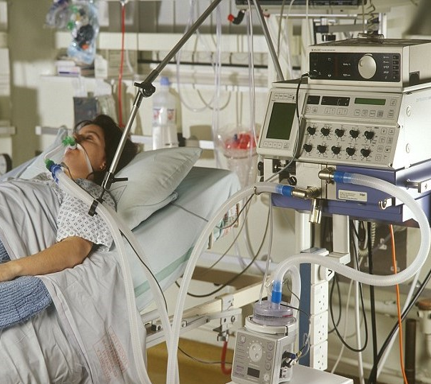
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Alexa, as part of my 1:1 consulting and advocacy service! Alexa’s mom is on a breathing machine and sedation in the ICU. Alexa is asking what are the chances that her mom will wake up after the tracheostomy.
What are the Chances that My Ventilated Mom Will Wake Up After the Tracheostomy in the ICU?
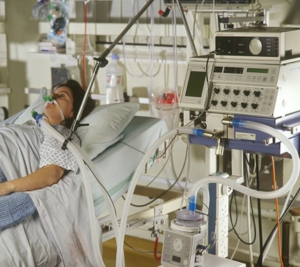
“You can also check out previous 1:1 consulting and advocacy sessions with me and Alexa here.”
Alexa: Patrik?
Patrik: Are you there?
Alexa: Yeah, yeah. So, I’ve hung up with the hospital now, so it should-
Patrik: Yeah. Yeah. Okay. Look, there are things that seem to be working for your mom. I mean, given that she’s in ARDS (acute respiratory distress syndrome), it’s positive her ventilator settings are moving in the right direction. I guess, the point that he made about her not waking up, is a point that you need to consider.
Patrik: And the question really is like he said, “How long do you want to wait? Do you want to proceed with a tracheostomy, and then wait until she wakes up? What if she never wakes up?” Those are the questions that nobody has a crystal ball to.
RECOMMENDED:
Alexa: Yeah, I don’t know how long, or why she’s not waking up, or how long it would take after the tracheostomy. But, I mean, what is the hospital’s obligation? Just in a general sense. Are they committed to keeping her there? So as long as her heart is going, her organs are somewhat functioning, and just keeping her there until that day happens that she wakes up?
Patrik: I would say, yes. There are many patients in ICU sometimes for months. The question always is, how long do you want to keep going? How long do you want to keep going, if she doesn’t wake up? We don’t know whether she will, or she won’t wake up. Let’s just say, you give consent to the tracheostomy, and she’s waking up, that’s great. If she doesn’t wake up, the question then is, what do we do next? He was talking about comfort care.
Alexa: I mean, in your experience, what’s the longest it’s taken? With your direct experience, that you’ve actually seen somebody, how long after the sedation was stopped, the sedatives were stopped, what’s the longest it’s taken for somebody to wake up?
Patrik: I’ve seen sometimes weeks. Please also keep in mind, waking up doesn’t necessarily mean your mom is going to wake up, and will be the very same than she was before. He said, “She’s not opening eyes.” So, the first thing that you’d be looking for is, is she starting to open eyes?
Patrik: Next thing you’d be looking for is, will she do things, simple things, like squeezing your fingers? When someone wakes up after an induced coma, it’s like switching on a light with a dimmer, not with a switch. If that makes sense?
Alexa: Mm-hmm. Yeah, it takes a long time to come through.
Patrik: It can take a long time. It also depends on what you want in terms of outcomes. For example, if you are expecting that your mom will wake up, and she will be the same than she was before, that may never happen. But if you are having potentially another goal, which is okay, have your mom wake up, so you can explain to her what’s happened, and then she can direct you what she wants. That’s a different goal.
Patrik: At the moment, you’d be making a decision for her, on behalf of her. If you’re feeling confident that she would feel confident with your decision-making, that’s great. But the question is, what would she decide if she could make that decision herself?
Alexa: Well, I know for a fact that she wouldn’t, whether it shows some hope or not, I know for a fact that she would not want to be resuscitated. So, I can definitely give him an answer on that. As then as far as me, for signing with absolute confidence as to what she would want, I don’t know, that would all depend on what the outcome was.
Alexa: So, if the outcome is more trending, like the probability of her having some very severe impact, resulting in some sort of very limited mobility, a cognitive decline of whatever extent. If she knows that she would be a vegetable afterwards, then she would probably not want to continue her life. I know that she wouldn’t want to be dependent on anybody.
Alexa: So, if everything that’s being suggested, like right now everything that’s taking place, if that’s the likelihood of how things are looking like right now, then the decision to take is basically to start considering end-of-life, I guess. But I don’t know what’s happening, like I don’t know.
Alexa: Right now, what I’m thinking is to definitely let him know that we are okay with the DNR (do-not-resuscitate), to respect that. And then, the other thing is to move forward with the tracheostomy, and then maybe give it a period of time, of one week, to see if there’s any change in that one week. And if not, then that would make our decision easier in terms of what to do next.
Alexa: The other thing, it’s just a lot to take into account, the other thing he mentioned that I just wanted to confirm with you was that he mentioned about the hemodialysis. Which means that if she was able to come out of this episode, that he had mentioned, then that now means that she would also be on dialysis permanently going forward.
Patrik: That is what it sounds to me like. However, my experience has shown me that very few patients that need dialysis in ICU, need dialysis after ICU, assuming they’re surviving. Okay? But I think that is probably not so much my concern at the moment, I know it’s definitely …
Patrik: At the moment, as long as she’s in ICU, the dialysis is not an issue, they just do it. It’s part of what happens in ICU. My concern is more like in the short-term, because she will be in ICU for some time to come, and the dialysis will take care of her kidney function for now.
Patrik: But it is certainly a valid question, because if you are talking about, what does her quality of life look like down the line? And you are thinking about, “Okay, what if she survives, her brain is working, would she want to go to dialysis three times a week?” They are very relevant questions, very relevant questions.
Suggested Links:
Alexa: Okay, all right. I got it, I understand. So, we have to make a decision in terms of what the most likelihood, given the circumstances, and given what’s already taken place, about what’s the probability or likelihood of her being her again, and there’s a very small chance of that, that’s what’s being said, I guess, if I’m reading between the lines.
Patrik: Very much so. Very much so. As I said, the way I look at this is, Alexa, I have seen this situation hundreds of times in terms of someone who is not waking up after a prolonged induced coma, there’s nothing new there. Okay? It’s new for you, of course. It’s a waiting game. It’s a waiting game, and there are no guarantees that you’re going to succeed with that waiting game.
Patrik: Now, here is another tip for you and for your family, try and project yourself out into 12 months. Okay? Today is the 3rd of March. Try and think about how would you look back on this situation in 12 months’ time. And the reason I want to explain that to you, I think it really gives you all the answers that you’re looking for.
Patrik: So, let’s just say you decide tomorrow not to do the tracheostomy, and you decide let’s move towards comfort care. Okay? And your mom may pass away. And then once you’ve dealt with the grief, if your mom passes away. In 12 months’ time after reflection, you look back and you might think, “What if?” But then it’s too late. You need to ask the what if question now.
Patrik: The reason I’m bringing up the 12 months, project yourself 12 months out, we have so many families have come to us after 12 months, after they lost someone, then they’re doing research, and “Oh, I found your website, I had no idea that we had options. I had no idea someone could advocate for us. I had no idea that we could sort of renegotiate,” but now it’s too late. There is no-
Alexa: Yeah, that’s the thing.
Patrik: Pardon?
Alexa: I think that’s the thing, it could be either way. I can also have a regret in knowing that I’ve moved forward with the option to keep her alive. And basically, at that time, I made a decision and it ended up the wrong way, because she’s even suffering more now. Like you said, if she comes to, or when, who knows what she’s going to be like.
Alexa: The other thing that you had mentioned to me, which was for me not to have or to make a decision on her life, was that if the goal ultimately is to move forward with the tracheostomy. And then wait until she wakes up, and then at that point see if I’m able to communicate enough with her, to be able to get her consent in terms of what she would like to do. And in that way, that would absolve me from ever having to feel like I’ve decided on somebody’s life.
Patrik: Correct. Correct. Look, Alexa, there is no right or wrong decision. There’s only a right or wrong decision for your family. But I do believe it’s important that you try and project yourself out to 12 months from today, and think, “How would I look back to this in 12 months’ time? Would I have regrets if I decided to stop everything today? Or would I not have regrets?”
Patrik: Again, there’s no right or wrong answer. From my end, it’s giving you the options of what I’ve seen on a clinical level, but also, I talk to a lot of people every day all over the world. And there are people that I’m talking to that had the situation 12 months ago, and they now feel they’ve rushed into a decision, because they felt pressured by the hospital.
Alexa: Yeah. It’s such a time-sensitive situation-
Patrik: Absolutely.
Alexa: … and there’s so much going on. So, Patrik, I’m sorry, I don’t want to put you in the position and ask you, but I just need, I guess, some sort of your opinion.
Patrik: Yeah, I can give you.
Alexa: Should I proceed with the tracheostomy?
Patrik: Yeah, I can give you my opinion. I think clinically, she needs a tracheostomy. Okay? She needs a tracheostomy on a clinical level. However, you do two things with a tracheostomy, (a), you give her time to wake up, that can be a good thing, or (b), she’s not waking up, then you may prolong her suffering.
Alexa: Yeah, I mean, that doesn’t preclude me from making it, if within another three, four days’ time she’s not waking up, then the end-of-life is certainly, the … What you call that? The comfort care option is still available.
Recommended:
Patrik: Oh, for sure. For sure. Look, the comfort care option is always available. I’m just saying, she will be going through a procedure for a tracheostomy, that’s all.
Alexa: And that could have some sort of trauma or some sort of-
Patrik: Well, I wouldn’t say trauma. What I will say is, look every procedure has pros and cons. There’s the risk for side effects. That’s all. It’s a pretty standard procedure in ICU nowadays with a tracheostomy, but just to be aware that in theory things could go wrong, like with any procedure. But the risk is pretty low, I would say, because they’re doing this every day, but just to be mindful of that.
Alexa: Would the option then, because right now she’s on morphine, she’s on sedatives, or whatever, on fentanyl. With that option, would they also then decrease those types of drugs as well, if she has a tube in her throat?
Patrik: That’s a great question. It’s hard to say. Most of the time, one of the reasons you want to do a tracheostomy is to minimize sedation, to stop sedation as a matter of fact, stop the morphine.
Alexa: That’s correct.
Patrik: However, if I understood this correctly from him, she’s struggling with a ventilator when she goes on dialysis. That’s almost unheard of, to me. I’ve never really heard of that, but that’s what he said. Was that your understanding too?
Alexa: Yes, I heard that also.
Patrik: Right. Right. So, that makes me think that if they’re giving her ketamine and fentanyl while she’s on dialysis, because she’s not breathing with a ventilator, that could continue once she’s having the tracheostomy. Nevertheless, though, you can’t keep a breathing tube in forever, whereas a tracheostomy you can keep in for a long time to come, and it’s much more comfortable.
Alexa: Okay. So, I think I know what I’m going to do. I’m going to discuss it as well with my family before I make my decision, but I have more confidence now, with the understanding of the situation I have. And I think this was my goal for this evening, in my conversation then.
Alexa: I will say, I regret that I did not have my recorder on when he was actually explaining everything in detail, because I haven’t heard it at that level of detail since I’ve been meeting with the doctors.
Patrik: Right, of course.
Alexa: They obviously reduce it for our understanding. So, I will … Yeah.
Patrik: I’ve taken some notes, so I’ve got most of the information written down, if you wanted to go through it again. But I think, as I said, you’re asking for a recommendation, I think a tracheostomy is the next step. Bear in mind, there is no guarantee that it will lead her to waking up.
Alexa: Okay, that’s fine.
Patrik: But there is something else that I want to say. So, they’ve done the EEG (electroencephalogram). They’ve done the CT (computed tomography) scan of the brain, and they have not found any brain damage. Therefore, you should be cautiously optimistic that over the next few days or weeks, assuming they can really stop the ketamine and the fentanyl, you should be seeing her waking up. I would be cautiously optimistic.
Alexa: Yeah, because these are strong narcotics and-
Patrik: Very strong.
Alexa: … remove the sedatives, but these narcotics are also having some sort of like you’re drowning the brain.
Patrik: Oh, huge.
Alexa: So, this is why in my understanding of course she’s not waking up, because she’s been so heavily sedated on drugs. And because she was so combative, they kept sedating her over, and over, and over again.
Alexa: So, I just want her to have that chance to wake up, and then I think that will give us a little bit more time in knowing how our mother has taken to things and what the next … Because, Patrik, I’m sorry, if this sounds very negative, it’s like right now I just feel that she has not had the fighting chance to try.
Patrik: Yeah, I agree. I agree. She has not had the fighting chance. If they had found a significant brain injury, like a stroke, I would say to you, you really need to think this through with your family, what you want next. But given that her brain is intact, that gives her the chance to wake up.
Patrik: And then you can sit down with her and can say, “Hey Mom, this is what’s happened. This is what it looks like. Can you direct us in what you would want?” That, I believe, will give you every peace of mind you will need that you’ve made the right decision for her.
Suggested Links:
Alexa: Yeah, Patrik, now what I’ll do is, I’ll talk with my family, and what I’d like to do is, I’d like to maybe follow up with you, maybe sometime next week and-
Patrik: Certainly.
Alexa: … explain to you the direction, just to let you discuss things, if that’s okay?
Patrik: Absolutely. Absolutely. Please reach out. Please reach out.
Alexa: Okay. Okay, listen, I appreciate it very, very, very much, Patrik.
Patrik: It’s a pleasure.
Alexa: It means a great deal to me. And if there’s any way that I can somehow pay, in another lifetime, maybe not this lifetime, within my career, because I really appreciate your help. But if ever I can help you out in any way, please don’t hesitate to reach out.
Patrik: Yeah, no, no. Let’s touch base again next week and see how we go.
Alexa: Okay. Very well, Patrik, thank you very much again, I appreciate it.
Patrik: It’s a pleasure. It’s a pleasure. Thank you so much, Alexa. All the best to you and your family for now. All the best. Thank you.
Alexa: Thank you very much.
Patrik: Thank you. Bye.
RECOMMENDED:
Alexa: Okay, Patrik. Okay, bye-bye.
Patrik: Bye.
Alexa: Thank you.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!