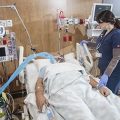
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ron, as part of my 1:1 consulting and advocacy service! Ron’s son is critically ill in ICU and is ventilated requiring high oxygen. Ron is asking if it’s possible that his son is having a pneumonia?
My Son is Ventilated in ICU Requiring High Oxygen. Would it Be Possible that My Son is Having a Pneumonia?
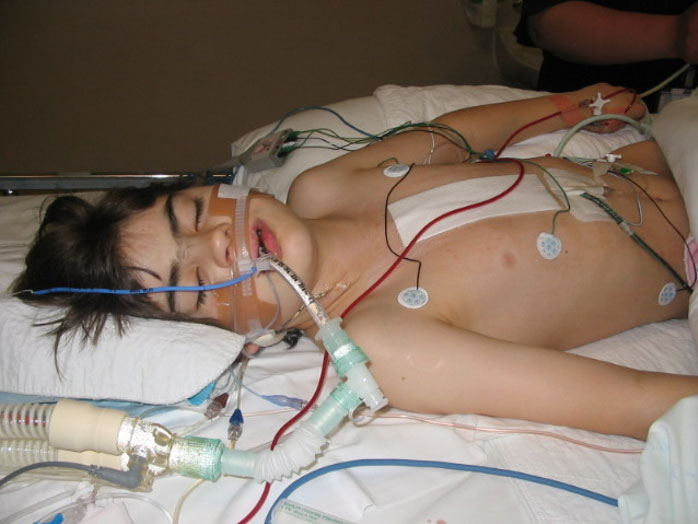
“You can also check out previous 1:1 consulting and advocacy sessions with me and Ron here.”
Patrik: It’s basically, they’re putting up a catheter towards the arteries of the heart to find out whether there are any blockages or not. That hasn’t happened, as far as you’re aware?
Ron: No. No.
Patrik: Okay. Okay. It would have been another procedure, you would have been aware if it had happened because it would have been another-
Ron: No, they didn’t have that.
Patrik: Okay. Okay. So are they stimulating him.
RECOMMENDED:
Ron: Hello?
Patrik: Hi, Ron. It’s Patrik again.
Ron: Hi.
Patrik: Hi. I can’t remember; what we were talking about when the contact dropped? We were talking about … Yes, so we were talking about angiogram. So that didn’t happen as far as you’re aware.
Ron: Right.
Patrik: Then what was the other thing? What we were talking about? Yeah, so I was talking about that sometimes it takes weeks for patients to come out of an induced coma even without any brain damage, so it’s just a matter of wait and see. But at the same time, I do feel like they need to try and wake your son up as quickly as possible.
Ron: Okay.
Patrik: Right. That’s because if there is any suspicion of brain damage, you’ll only find out by removing sedation.
Ron: Right. I think that was their attempt to do that by removing the typical-
Patrik: Yup.
Ron: … and keeping him on. But they just kept him on the Precedex; a certain amount of Precedex and a certain amount of fentanyl.
RECOMMENDED:
Patrik: Yep. Yep.
Ron: But I think we need some images.
Patrik: Yes, yes, yeah, yeah. I can see them coming through now. They’re just uploading. Okay, the numbers on the monitor look okay. If there is any concern, his heart rate is really fast. It’s 115, which could be a sign of discomfort. Do you think, can you see any signs of discomfort?
Ron: No. Not really. He’s not showing anything, but his breathing kind of fast.
Patrik: Yeah. Is he fighting that breathing tube in his mouth?
Ron: How would I tell that he’s fighting it?
Patrik: If he-
Ron: Because he’s kind of like fighting.
Patrik: Is he’s coughing? Is he coughing because of the breathing tube?
Ron: He cough when they go down the suction catheter.
Patrik: Okay. That’s good. That’s good. But is he chewing on it? Is he sort of chewing-
Ron: He was biting on it at one point.
Patrik: Okay.
Ron: He was biting on it.
Patrik: Okay. Oh, biting on it?
Ron: They would try to go to trachea but he was biting. Like, kind of biting on it. He wouldn’t let them go down.
Patrik: Yeah. Okay, okay. Sorry, I’m just looking at those pictures again. I’m glad you sent through those pictures. The oxygen level on the ventilator is 90%.
RECOMMENDED:
Ron: Right.
Patrik: Now, that is a lot.
Ron: Right.
Patrik: So, to put this-
Ron: They’ve been adjusting it throughout the day, throughout the day. They put it up to 90% a few hours ago.
Patrik: Yeah.
Ron: Because it’s trying to get him in a place of-
Patrik: Yeah, yeah. So here is the question with that. Do you remember, I asked you a little while back, sort of is there any infection? Now, with oxygen levels at 90%, I argue there could be a chest infection or a pneumonia, and I’ll tell you why. I’ll tell you why. So, the air that we are breathing is 21% of oxygen; room air, 21% of oxygen. If somebody is on the ventilator without a chest infection or without a pneumonia, their oxygen levels on the ventilator shouldn’t be above 40%.
Ron: Right.
Patrik: Right? 90% is a lot.
Ron: Right.
Patrik: And my suspicion is there could be an infection. The other thing that I am wondering is, his rate is 35 per minute. Can you see that, where it says AC?
Ron: Yeah.
Patrik: Right. That’s pretty high, and that’s okay. And he’s breathing on top of that. He’s breathing 45 breaths per minute. That is pretty high, and it’s okay. But when I look at the monitor, his CO2 level … And you need to stop me; if I’m getting too medical here, you need to stop me.
Ron: Yeah, it’s fine.
Patrik: His CO2 level is 45. With a breathing rate of 45, his CO2 level should be much lower. So I am not sure what’s happening there, but I think there is stuff happening with his lungs potentially. There hasn’t been any lung disease before this event?
RECOMMENDED:
Ron: No, no, no.
Patrik: Right. Okay, okay. I think we need to find out whether there is anything happening with the lungs. I do believe there is. On 90% of oxygen, there must be something happening with the lungs.
Patrik: When he had cardiac compressions, when he had the cardiac arrest, they would have done chest compressions?
Ron: Right, which they did.
Patrik: Right, right. With chest compressions, there is the risk of rib fractures. With rib fractures, there is a risk for pneumonia. Right?
Ron: Right. Right. They’ve done like BALs, the BALs, where they went down.
Patrik: Yup, yup.
Ron: It didn’t show any pneumonia or anything down there.
Patrik: Right. Okay, okay.
Ron: It didn’t show pneumonia.
Patrik: How long ago was that?
Ron: I can’t tell you exactly what it was, in his trachea. Like a gram positive and negative.
Patrik: Yeah. Gram positive or gram negative bacteria.
Ron: Yeah, in his trachea.
RECOMMENDED:
Patrik: Right, right. Okay. And how long ago was that?
Ron: That came back about two to three days ago. So currently, he’s on azithromycin, I believe.
Patrik: Yep. Okay.
Ron: He’s on azithromycin. This is a new antibiotic, so I’m not familiar with it. He’s on Bactrim.
Patrik: Bactrim?
Ron: Bactrim, yeah.
Patrik: Yeah.
Ron: And his prophylactic stuff.
Patrik: Right, yup, yup. Yes.
Ron: I want to say that’s all of antibiotics that he’s on.
Patrik: Right, right. So, the erythromycin, in particular, could be given because of an infection, but it could also be given because he’s not absorbing his feeds.
Ron: Right.
Patrik: Right? It could be either or. He would have a nasal gastric feeding tube.
Ron: Yeah, he has it. They put one in.
Patrik: Yeah.
Ron: I’ll send you an x-ray of his latest chest x-ray.
Patrik: Right, that would be good. With the erythromycin, yes that could be given for an infection, but it could also be given if he’s not absorbing his feed. It can be given for that because it increases motility in the gut.
RECOMMENDED:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Ron: Oh, okay.
Patrik: Right, right. I don’t know, there is something happening with his lungs, potentially an infection. 90% of oxygen is a lot. We need to find out what’s happening. Okay, so fentanyl. Okay, okay. Parenteral nutrition. Okay, okay. So I’ll come to that in a moment. Just give me one sec.
Patrik: I’ll just quickly look at the chest x-ray. What I need to do with the chest x-ray, I just quickly need to email that from my phone to my computer, just simply because I need to bring it up on a bigger screen. Just give me one sec please, because it’s too small for me on the phone to look at it. So, for example, you look at the pump that you sent me through, the picture of the pump with fentanyl, epinephrine, and dexmedetomidine, there is also, on the top you can see parenteral nutrition.
Ron: Oh, the TPN. Yeah, he’s on TPN because he isn’t-
Patrik: Why is he on TPN?
Ron: Because he wasn’t able to really get anything down.
Patrik: Oh, okay.
Ron: He wasn’t able to get anything down. At one point he had GVHD of the gut.
Patrik: Yep. Okay.
Ron: So they started him on a treatment. What do you call it? But that hasn’t really been causing the issues.
Patrik: Right.
Ron: Which he started to, because he started to drink like Pediasure and stuff.
Patrik: Right. So, are you suggesting that the TPN has been an ongoing thing for him?
Ron: Yeah it has. He’s been on it for two months now.
Patrik: Oh, I see. I see. Okay. And no nasal gastric feed at all, and no oral feed before the cardiac arrest?
RECOMMENDED:
Ron: No. Before that, he was drinking like Pediasure.
Patrik: Right. I see, I see. Okay, okay. So I’m just quickly looking up the x-ray. I would think the right side isn’t too bad, but there is definitely some stuff happening on the left side, which suggests there could be an infection. If you want me to, and if that’s possible, you can ask the nurse who’s at the bedside, I would imagine, what’s happening. Why he’s on 90% of oxygen. I’m happy to talk to the nurse. If you can put the nurse on. I’m happy to talk to them. It’s up to you. But there is something happening with his lungs.
Ron: I sent you a second picture of his chest x-ray and that was taken this morning. So the one that you got was taken this afternoon, and the one that I just sent was taken this morning around 6:00 AM.
Patrik: Okay, okay. All right.
Ron: I think I can put you on phone with the nurse, or I can put you on directly with the attendant because he’s right here.
Patrik: Sure, sure. Before you do that, it’s probably best if you introduce me as either a family friend or a cousin or whatever. Just non-confrontational. Non-confrontational.
Ron: That’s what I was going to do; friend of the family.
Patrik: Yes, yes.
Ron: A friend of the family. That’s what I was going to introduce you as.
Patrik: Yes, yeah. Exactly. Exactly. Yep.
Ron: Okay. So, I think that the doctor is still on, and that’s been the attending for this week during the day.
Patrik: Alright.
Ron: He’s actually right here right now, so I’ll have him speak to you. Okay?
Patrik: Thank you. Thank you.
Ron: Okay. How are you?
Patrik: How are you?
Ron: One moment. One moment.
Patrik: Yeah, yeah. Sure, sure.
Ron: Say that again?
Patrik: I’m here.
Ron: One moment, one moment. Is it possible that you can … I have a friend of the family on the line. He just wants to speak to you about a few things, if you can. Okay? Let me just stick you off my phone.
Dr. Whiteside: Hello?
Patrik: Hi. How are you? My name is Patrik. How are you?
Ron: Patrik, this is Ron. I’m handing you off to Dr. Whiteside right now.
RECOMMENDED:
Patrik: Yeah. Thank you, thank you.
Ron: Okay. One moment.
Dr. Whiteside: Yeah.
Ron: Yeah.
Dr. Whiteside: Okay, what can I tell you?
Patrik: Yeah look, I’m a family friend. I do have an intensive care nursing background myself. I’m just sort of trying to find out what’s happening. Ron was telling me he’s on 90% of oxygen.
Dr. Whiteside: You broke up a little bit.
Patrik: Oh, sorry.
Dr. Whiteside: Say that again?
Patrik: Sorry. Ron was telling me that he’s now on 90% of oxygen, and I just said sort of is there a chest infection? She wasn’t quite sure about that.
Dr. Whiteside: Sure. I mean, So right now, a number of ventilators adjustments have been made. Our pH is 7.11. Basically having pretty significant neurologic hyperventilation.
RECOMMENDED:
Patrik: Right.
Dr. Whiteside: So you’ll notice with one difficulty to look at the ventilator. We’ve even tried to assist control, which is pretty unusual for us in pediatrics Were on pressure controlled volume control. On tidal volumes, we got 260. His pressure’s in the mid 30s. But what the real challenge is if he’s breathing at a rate of about 50, 45 right now. And whether we’ve been hyperventilating or hyper-oxygenating him, he’s really, he’s continuing to do that. I’m just having a lot of difficulty maintaining his ventilation without a paralytic.
Patrik: I see.
Dr. Whiteside: So what I was going to do now give a single dose of vecuronium and seeing if these numbers improve as much. I hope they do.
Patrik: Sure, sure.
Dr. Whiteside: In which case we’re stuck with that. We did some trials earlier today to try to get a better sense of his neurologic status. I think this neurologic breathing’s consistent with the rest of our exam.
Patrik: Right. I see, I see. It’s mainly an issue of him not breathing appropriately?
Dr. Whiteside: And not responding to changes in ventilation or oxygenation. Yeah.
Patrik: He doesn’t have a pneumonia?
Dr. Whiteside: Well, he has sort of … It’s Acute Respiratory Distress Syndrome or ARDS.
Patrik: Right.
Dr. Whiteside: He’s on IV fluids right to really maintain optimum fluid. But even with that, he needs blood pressure support with epinephrine, which he’s on right now, to at times needing nicardipine because he’s hypertensive.
Patrik: Yeah. I see. I see. Right, right, right. I see. Okay. Is there any evidence that there has been brain damage, or it’s still-
RECOMMENDED:
Dr. Whiteside: Yeah, hang on one second.
Patrik: Thank you.
Dr. Whiteside: Okay. Yeah, I’m afraid there’s evidence of extensive brain damage.
Patrik: Right, right.
Dr. Whiteside: The MRI really shows very significant hypoxic-ischemic injury and oxidation with minimal sedation. He won’t spontaneously respond to anything.
Patrik: Sure.
Dr. Whiteside: I’m afraid …
Patrik: Sure, it doesn’t look good. I understand I understand. The best GCS you would be getting from him, is it a three or is it more than a three?
Dr. Whiteside: No, it’s a three.
Patrik: It’s a three, okay. Okay. And just for me to hear that probably one more time; you think he’s in ARDS. Is that what you said?
Dr. Whiteside: Well, what we’re seeing, we’re not growing anything right now.
Patrik: Right, right.
Dr. Whiteside: He does have a significant oxygen requirement.
Patrik: I see.
Dr. Whiteside: We’re a very broad spectrum in sort of the spirit of hematologic oncology world; antifungal, antivirals, antimicrobials. Sort of a homogeneous bilateral lung disease, which has a little bit of fluctuation based on pool balance, but it’s been pretty persistent.
Patrik: Okay. I see.
RECOMMENDED:
Dr. Whiteside: He’s also on continuous renal replacement therapy.
Patrik: Yes, yes. I’m aware of that. I’m aware of that.
Dr. Whiteside: Yeah.
Patrik: Yeah, yeah. So, his main issue is really is, he’s not waking up obviously, because of brain damage. And he does have some sort of lung infection where his oxygen requirements are pretty high, and he’s also not conforming with any ventilation you were sort of trying to apply to him?
Dr. Whiteside: Right. And the ongoing renal placement.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!