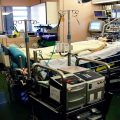
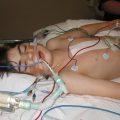
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ron, as part of my 1:1 consulting and advocacy service! Ron’s son is critically ill in ICU with a brain injury and Ron is asking why his son is not waking up from an induced coma?
My Son is Critically Ill in ICU with a Brain Injury. Why is my Son Not Waking Up From an Induced Coma?
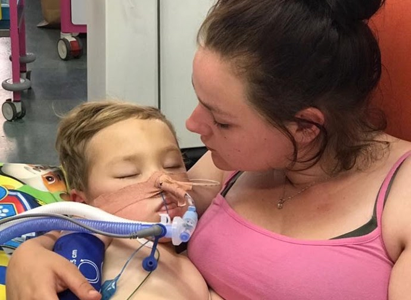
“You can also check out previous 1:1 consulting and advocacy sessions with me and Ron here.”
Patrik: Right, right. Well, with a breathing rate of 45, that’s too high. The breathing rate of 45 is too high. His pH is down, right? Which is what the doctor said.
Ron: Yeah.
Patrik: Right, and that’s a concern. So they have to do something. Right?
Ron: Okay.
Patrik: And that makes sense to me.
Ron: Okay.
Patrik: But what I’ll do next, really I’ll … If you’re okay with that, I’ll write up a list of questions that I will have with you in the next hour.
Ron: Okay.
Patrik: And then maybe we’ll jump on the phone again then.
Ron: Okay. Sounds good.
Patrik: All right. I’ll be back in the next hour or so.
Ron: Okay. All right.
RECOMMENDED:
Ron: Hello?
Patrik: Hi Ron, it’s Patrik here again, how are you?
Ron: Yeah. I’m well. So I asked if she would be willing to speak with you to answer any questions, that’s a very long question you sent me, to answer any questions. She said she would be happy to, it’s her first time meeting him. If it’s other factual information, that she has to read up on him a little more and get to know him more and more but she said she would be willing to add any questions.
Patrik: And sorry, who did you say said that? It’s the nurse?
Ron: His attendant tonight.
Patrik: Oh, okay, great. Very happy to do that, you let me know when she’s available. Have they done the rounds yet?
Ron: No, she just stopped in to take a look at him, it was her first time meeting him so just to check him out, look at him. They need to change his ventilator, she did go down on the oxygen, she said the oxygen was 60% now.
Patrik: 60? 6-0?
Ron: Yes, 6-0.
Patrik: That’s good. In and of itself, I’m very relieved by because 90% is just, the closer you get to 100%, it’s life-threatening. 60%, I’m already relieved. It’s still a fairly decent amount but 90%, the red flags go off, big time.
RECOMMENDED:
Ron: Okay. So I’ll take a picture and send you what his ventilator looks like now with the changes.
Patrik: That would be great.
Ron: She said as far as the ARDS, is that what it is?
Patrik: ARDS?
Ron: The infection in that lung?
Patrik: Yeah.
Ron: She did say that she’s not exactly sure that it is ARDS so didn’t know. In a few hours she’ll just, because right now they are pulling off. She was positive right now so they’re trying to pull it off with the dialysis machine. I guess that’s what it is. So she said she’ll probably have a better take on whether it is actually ARDS or not because it’s not set in tone that’s what it is.
Patrik: That’s good. And when you, yourself, read through the questions, is that making sense at all? Is it too overwhelming, is it too clinical?
Ron: No, they make sense, I just have to throw them in where I can throw them in. I’ll try to break them down in domino as I can.
Patrik: es. And it’s important for you in a situation like that, as part of this you will be getting a crash course in ICU.
Ron: I’m sorry, again, who?
Patrik: I said, as part of this, you almost will be getting a crash course in ICU.
RECOMMENDED:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Ron: A crash course. Right, I know.
Patrik: Because the more you understand, it’s almost imperative for you to understand what’s exactly happening. It’s imperative for you, what’s working, what’s not working, where are the dangers. But also where are opportunities for improvement. The biggest challenge is really, what does it all mean?
Ron: Right, absolutely.
Patrik: What does it all mean? And that’s often difficult to put into perspective for families. So what we’ll do then is once you have the attendant there, just give me a call or I can call you back straight away. That, I would suggest, is the next step.
Ron: Okay. She said she’s going to read over his files and everything and she’s going to add and she’ll step back in ICU.
Patrik: Right. When you’re saying she’ll read through his file, is this the first time you met her?
Ron: Yeah, this is the first time I’ve met her in the ICU. The gentlemen that she spoke to, the doctor that she spoke to earlier. I think this is his time to be on and he’s here from Monday through Friday. I think, on the day shift and then a different one comes on at night. So she was saying that he would probably be able to answer these questions best but she’s happy and willing to answer any questions that she could about my son that she knows of him. But she’s just saying that she may not go with him, to know him to see because it’s the first time, which it is. It’s the first time with me and her.
Patrik: Sure. Overall, in the bigger scheme of things, you’ve been in this hospital for quite some time now. Overall, are you satisfied with the hospital in general?
Ron: It is pretty good in the children’s hospital. We’ve had some really good doctors here and nurses and nurse practitioners, they have some really good ones here. But to compare to somewhere else, I don’t know because Daniel has never been sick, to go somewhere, he’s had to go to the hospital. This is our first week. He’s been a pretty healthy kid all his life.
Patrik: Absolutely. And as you would have seen by now already, intensive care is a different ballgame. Yes, you’ve been in the hospital for a long time, yes, he’s been sick for a long time, by the sounds of things, however you would have noticed by now, intensive care, you can’t compare it with any other area.
Ron: Absolutely.
Patrik: The reality is, and it might sound harsh what I’m saying now, but the reality is whenever somebody’s in intensive care, they are as close to death as they can ever be.
RECOMMENDED:
Ron: Absolutely, I agree.
Patrik: That’s the unfortunate reality and it’s a matter of making sense out of it and it’s a matter of getting informed.
Ron: Right.
Patrik: Yes, so please get back to me when this doctor is available.
Ron: Absolutely, I’m going to let her look at whatever she has to look at and as soon as I can grab her in here, I definitely will so that we can get some of these questions answered.
Patrik: Questions answered, yes, that’s right. I’ll wait for your call then.
Ron: All right. Thanks Patrik.
Patrik: Thank you, bye.
Ron: Hello.
Patrik: Hi Ron, it’s Patrik again.
Ron: Yes.
Patrik: So, okay, so he’s on norepinephrine now, and they started him on the anti-fungals. When did they start the anti-fungals?
Ron: I’ve been on it for a while now. You know, so that’s part of his STEM cells.
Patrik: I see, so that’s part of his STEM cell therapy, is it?
Ron: Right, right.
Patrik: Okay. And he’s on Meropenem as a broad spectrum coverage for fevers he’s had a few days ago. He’s also been tested for Vancomycin-Resistant Enterococci (VRE). Do you know whether those tests have been coming back already?
Ron: Hold on a minute.
RECOMMENDED:
Patrik: Thank you.
Ron: Hello?
Patrik: Yes.
Ron: Yeah, I’m sorry. We’re talking about the anti-fungal? Yeah. That’s been long.
Patrik: Right. Okay. Okay. So and with the norepinephrine that’s running now, when did they start that?
Ron: Overnight.
Patrik: Overnight. Okay.
Ron: Yeah that’s what… I think last night. Yeah.
Patrik: Right. Okay. Okay. And have they mentioned to you why it was started?
Ron: I think he was probably really sick at the time, but I was waiting for him to come ask him.
Patrik: Okay. So there’s probably a number of things, a couple of things that are happened there. So the…
Ron: I have his… before you start, I have his neurologist in the room with me right now. Would you like to speak to him?
Patrik: Yeah, I’m very happy to speak to him. Yeah, for sure.
Ron: Okay, hold on.
Patrik: Thank you.
Dr. Pringle: Yeah, hi, my name’s Doctor Pringle, I’m with neurology. I’ve known Daniel for a while.
Patrik: Hi, good morning. My name is Patrik. I’m a family friend. I’m just trying to find out enough. I do have an intensive care nursing background myself. I’m just trying to find out from a neurology point of view, what are you predicting? Do you think that he can wake up or at some point what… What’s the damage that’s been done from a brain perspective?
RECOMMENDED:
Dr. Pringle: Right. So what… I’ll tell you the information we’ve been given and I’ll give you my impression. So he had a cardiac arrest a week from this past Sunday, excuse me, Saturday, so we’re nearly weeks out. His MRI showed strokes deep in the brain in the basal ganglia, and then his EEG’s, we’ve done them twice, have not shown seizures that showed this coma pattern called spindle coma. And the main significance of those patterns is you do not see a differentiation between sleep wake cycles.
Dr. Pringle: It has implications for prognosis when you’re not moving between wakefulness and sleep. That EEG pattern continued. We stopped the EEG I believe on Tuesday, but it was still there when we did it the second EEG, the second time over the weekend. The concern I have is… Now on the more positive note, he does still have pupillary responses and he still has corneal reflexes. But typically with that EEG pattern, and with the absence of waking up at this point this far from the episode, even though we’re weaning the medications. While I think it’s quite possible, he will open his eyes, I don’t think he’ll regain awareness.
Patrik: Right.
Dr. Pringle: And so I think he might sort of open his eyes and I don’t know, the eyes might move around a bit, but I don’t think he can regain awareness of what was around him.
RECOMMENDED:
Dr. Pringle: We were talking about yesterday, it’s while it is certainly the case that predicting the future in medicine or any other place is you have to be very humble about your ability to do that. And that’s, and we have every intention of giving Daniel every chance to show us that he can recover. There is a fairly large amount of literature on cardiac arrest in adults, and as time goes on and you get certain test results and don’t see improvement, those are the things you get concerned about.
Patrik: Yeah. I really appreciate your insights and your compassion and your honesty. I mean, it’s a very traumatic situation. Very difficult situation for everyone. I mean, I’m sure you’re doing everything that you can, but you know, if there have been strokes or mini-strokes and you know, is there any sort of… How long has the down time been during the cardiac arrests? Are there any sort of timeframes that you can point towards?
Dr. Pringle: I don’t have the time of the return of spontaneous circulation. I think it was a matter of minutes, but whereas I think I put, I kind of put more stock in that, in the beginning when I’m first seeing a child after a cardiac arrest. Now, I mean, I think that the time that matters most is the increasing time from the event without improvement. You know, that would be what worries me, and, and I’m pretty, not pretty, I’m very conservative on these things and I don’t, I want to do everything we can to not be wrong. And I very much want to be wrong here and he’s been through so much for so long and, there’s no hurry to any of this. These are the concerns are right now.
Patrik: Sure, sure. And did you say there is no seizure activity and there has been no seizure activity?
Dr. Pringle: That’s right.
Patrik: Right, right.
Dr. Pringle: We have him on some seizure meds and I was doing some things early in the week to see that what I was seeing was not a seizure. I’d never seen a seizure that looked like that. But again, an aim of trying to do anything that we could do to reverse this.
RECOMMENDED:
Patrik: Yeah. Yeah, I understand. Understand. Okay. Look, I really do appreciate your time.
Dr. Pringle: I’m happy to do it.
Patrik: Your compassion.
Dr. Pringle: Thank you.
Patrik: Thank you so much. Thank you. Bye bye.
Ron: Thank you, I appreciate it. Hello?
Patrik: Hi. Can you hear me?
Ron: Yeah.
Patrik: Yes. Did you hear what he said?
Ron: Yeah.
Patrik: Is that any different from what he’s been telling you throughout this or?
Ron: Did he say it was deep strokes in the brain?
Patrik: Say that again please.
Ron: Did he say it was deep strokes in brain?
Patrik: Yes. Yes he did. Yes.
Ron: I didn’t hear that before, no.
Patrik: Right. He was referring to mini-strokes, but he was still referring to strokes. I did ask him about, quote unquote downtime and what I mean by downtime is basically the length of the cardiac arrest and you know how long it took for circulation to return, but he didn’t have any timeframes. He didn’t have any numbers.
Patrik: His outlook is fairly bleak. By the same time, you know, he wants to give you something. What is it? Daniel?
RECOMMENDED:
Ron: My time?
Patrik: No, no, your son’s name.
Ron: Daniel.
Patrik: Daniel. Okay. Okay.
Ron: Yeah.
Patrik: He clearly said that he wants to give him every opportunity to recover, whether that’s possible or not is unsure, but there was, on the one hand, he had a bleak outlook, on the other hand, he wants to give him every chance. Again, is that the same that he shared with you? Has his approach sort of changed?
Ron: I mean, that’s… I wouldn’t say it’s so far a lot, you know, but you know, actually hearing that, out of his mouth. Yeah. You know?
Patrik: Right, right. Okay. Okay.
Patrik: What he says, is that different from what everybody else is saying?
Ron: As far as the… Well, from what I know, they’re going off of his… You know?
Patrik: Right. Right.
Ron: And also the attendant that’s on call, you know, and so basically, it is the neurons, with his brain so they’re going to turn to the neurologist.
Patrik: Yeah, absolutely. Absolutely. He did start him on some anti-seizure medications earlier in the week, which I’m not too surprised by. I mean, the last thing he needs is to have any seizures on top of what’s already happening.
Patrik: Right. By the same token, I’m not disputing his findings and I’m just not disputing his approach. What I have seen over the years Ron, though is, as I mentioned to you yesterday, the biggest goal at the moment is to get Daniel out of intensive care alive if possible. Right.
RECOMMENDED:
Ron: Right.
Patrik: And then look at sort of the next steps. Is there an option for a level of recovery? And one might say for a meaningful recovery, right? Has that sort of word been used? A meaningful recovery? Have you heard of that before?
Ron: Something like that, like quality of life.
Patrik: You might have heard him say something along the lines of, Oh, you know, down the line he might be able to open his eyes whether…
Ron: I just heard that here.
Patrik: Right, right. So you know, and again he said he is humble about predicting the future, because at the end of the day he can’t predict the future, right? And he wants to approach this sort of conservatively, which is probably a good approach to give him every chance, and then see what happens from here. You might remember yesterday, I mentioned to you that when patients are in induced coma, sometimes these can take weeks for them to wake up and they don’t have any brain damage.
Ron: Right.
RECOMMENDED:
Patrik: Right? So the challenge that your son is facing at the moment is he might be now in a cycle where he’s not coming out of the induced coma yet for a number of reasons. By the same token, he has brain damage. So what is actually not waking up from the induced coma and what is his brain damage? What’s really contributing to this? Is it the brain damage or is it just not waking up from the coma?
Ron: Right, right, right.
Patrik: Right. And that is pretty difficult to determine at the moment.
Ron: Right.
Patrik: Very few patients, by the time they are leaving intensive care with a brain injury, would be at the point where people can make a proper cognitive assessment.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!