Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
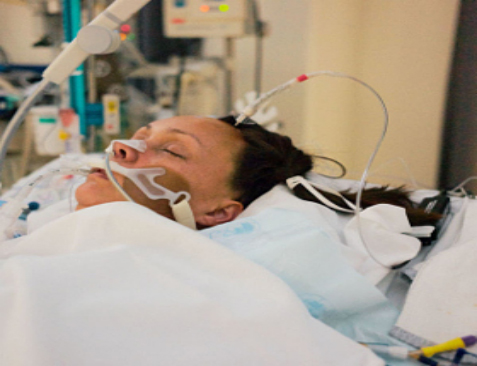
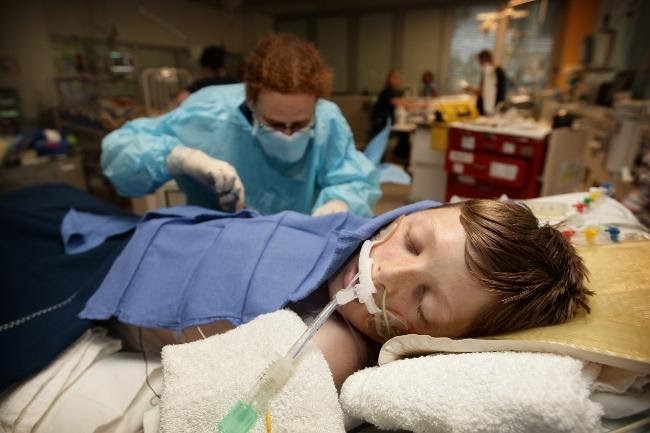
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Ron, as part of my 1:1 consulting and advocacy service! Ron’s son is in ICU due to cardiac arrest post transplantation and Ron is asking if the ICU team should wean his son from sedation so he can come off the ventilator?
My Son is Critically Ill in ICU due to Cardiac Arrest and in an Induced Coma. Should the ICU Team Wean Him from Sedation so He Can Come Off the Ventilator?
Patrik: Hello?
Ron: Hello?
Patrik: Hi, it’s Patrik again from intensive care hotline. Hi. Did you get the email?
Ron: Yeah. I did.
Patrik: Right. Okay. Okay. Are you in intensive care with your son at the moment?
Ron: Yes, I am.
RECOMMENDED:
Patrik: Right, right. And what are you currently waiting for? Are you waiting for a doctor to see him?
Ron: No, you know, they come and they do their routine, to keep him up, they check with him and they give him his medicine.
Patrik: Right. Okay. Okay. So at the moment, is he responding to you?
Ron: No, he’s not.
Patrik: Okay. Okay. But you did mention I believe earlier that-
Ron: Right.
Patrik: Did you mention earlier that his pupils are reacting to light or they’re not reacting to light?
Ron: Yes.
Patrik: They are.
Ron: Yeah, they are.
Patrik: That’s good.
Ron: When they go to touch him, they kind of react as well.
RECOMMENDED:
Patrik: Right, right. Have you heard of the term Glasgow Coma Scale?
Ron: No I haven’t.
Patrik: Okay. Okay. The reason I bring this up is your son would have a Glasgow Coma Scale. What it is, basically, it’s an assessment score. It’s an assessment score that’s being used in intensive care to assess a person’s neurological function. Now if you give me one minute… So at the moment, or at least for the first two days, they would have scored him for a Glasgow Coma Scale every hour. At the moment, they might still do it every two hours, maybe every four hours. Not sure. You got to find out.
Patrik: So when you and I are talking at the moment, we are a Glasgow Coma Scale 15, which is the maximum score. When somebody is in a coma, their Glasgow Coma Scale is significantly less than 15. The worst Glasgow Coma Scale is a 3, and the best Glasgow Coma Scale is 15 which is, again, it’s when you and I are talking.
Ron: Right.
Patrik: I’m interested to find out what Glasgow Coma Scale your son is currently having because it would give you a very good indication of how awake he is. It would give me a very good indication on how awake he is and what potentially would be the next steps. What I’ll do is, I will email you, now I’m just doing this as we speak. I will email you a picture of the Glasgow Coma Scale so you can have a bit of a look and get familiar with that because going forward, it’s going to be a good indicator to find out the level of consciousness of your son.
Ron: Okay.
Patrik: And it’s also a good indicator to talk to them about it because they will certainly be assessing your son on the Glasgow Coma Scale. In terms of life support, your son is on a ventilator at the moment. Do you know whether he’s on any other life support? For example, he’s not on a dialysis machine.
Ron: You ask me because he had fluid they had to pull off of him.
Patrik: Right. Okay. Okay. And is that because his kidneys are failing or is that because of-
Ron: Well, when he got down here they had to give him a bunch of fluids and then get him off as quickly as they needed.
RECOMMENDED:
Patrik: Okay.
Patrik: Right. I see, I see. And how long have they been doing that for?
Ron: Probably two days on and off, they’ll take it off and put it back on, but it’s not continuous. A continuous flow, a gently flow.
Patrik: Right. Okay. Okay. Do you know if he’s on any other life support? With a cardiac arrest, often what happens, is patients need inotropes or vasopressors Have you heard of that term?
Ron: No.
Patrik: Right. Okay. So often when, during or immediately after cardiac arrest, patients need inotropes or vasopressors. What that means is because the heart is so weak, the heart needs to be supported during that critical period.
Ron: Now they said it’s fine. They did an Echo and an EKG and they said his heart was functioning fine.
Patrik: Okay. Okay. That’s good. But okay. That means at the moment he’s probably not on any of that support because again, that is a level of life support, and I’m always trying to find out how critical is the situation with life support is used to keep, your son alive at the moment. But if he’s not on any of those, that’s good.
Ron: Yeah, they have him on a Epinephrine drip to keep his pressure.
Patrik: They have him on an Epinephrine drip?
Ron: Yes.
Patrik: Epinephrine?
Ron: Epinephrine
Patrik: Yeah, that is exactly what I’m talking about. So that is another level of life support.
Ron: Yeah, they have him on it while he’s… Yeah, right now.
Patrik: Right, right.
Ron: They stopped it for a while. He hasn’t been on it for a while. They just started that back today.
Patrik: Okay.
Ron: I guess they wanted to start it back up. And he’s on a 0.6 dosage of it.
Patrik: Okay, okay. That’s good. Good information to have. And it could be if he’s on the epinephrine, it could be that his heart is still a little bit weak or it could be a side effect of the sedation. The main side effect of one of the main side effects of Precedex is hypotension, which is low blood pressure.
RECOMMENDED:
Ron: Right.
Patrik: And with that hypotension or the low blood pressure, the epinephrine could be needed because epinephrine is basically bringing up the blood pressure.
Ron: Right.
Patrik: Right.
Ron: Yes. They use it to bring up his blood pressure.
Patrik: Yep. Yep. Okay. So when was the last time you’ve had an update from the doctors or from the nurses? When was the last time you’ve had a good update with them or from them?
Ron: Well, this morning, they kind of wake him up, they took him off the Propofol.
Patrik: Right.
Ron: They did a test line, to see if he’d awake from that, but they still had him on 0.1 of the Precedex.
Patrik: Right?
Ron: Which they still have him on.
Patrik: Yep. Okay. Okay. And how are you being updated, generally speaking? Are they giving you daily updates? How is the communication?
RECOMMENDED:
Ron: I’m pretty much updated. They have rounds like two to three times a day, so I’m pretty much at the rounds every time they speak upon.
Patrik: Right. Okay. Okay. There hasn’t been any talk about treatment limitations? A lot of people when they come to us, they are often confronted with asking to sign DNRs, if you know what I mean by DNR. There hasn’t been any talk about that at all.
Ron: To sign… Say that again.
Patrik: Do you know what a DNR is?
Ron: No, I don’t.
Patrik: Right, right. That’s good. That’s good that you don’t know because that means it hasn’t been mentioned. But I’d still want to make mention of it. DNR stands for do not resuscitate, and a lot of patients, a lot of families in intensive care are being asked to sign a DNR, but if it hasn’t been mentioned that’s good. That’s good. It means that they’re not… It sounds to me like they’re doing everything that they can at this point in time.
Ron: Right.
Patrik: Have you had any sort of meetings where the doctors actually was sitting down with you, or is it sort of all informant at the bedside?
RECOMMENDED:
Ron: They happened today, yes.
Patrik: They were sitting down with you?
Ron: Yeah, that happened today.
Patrik: Right. And what was it all about? What, what did they discuss?
Ron: Well this is his third… They don’t know if he would have any functional… A good function of life, because they think he’s trying to place him in a vegetative state, a vegetable.
Patrik: Right.
Ron: They’re giving him MRI’s, but they don’t know… It’s up to me and what I want to do. I can make them comfortable. I can keep him at the centre that he’s in right now. Keep doing what they doing.
Patrik: Yeah, sure.
Ron: To keep him going.
Patrik: Yes. Yes. I see. And when they were implying to make your son comfortable, where they implying to potentially stop treatment, is that what they were hinting towards?
Ron: They didn’t say that, they’re not saying that they plan on stopping treatment.
Patrik: That means that they have given that as an option to you.
Ron: Right.
Patrik: Right. Okay. Okay.
Ron: And they also mentioned a tracheostomy, but they didn’t go into… You know, that’s a possibility.
Patrik: Yes. Yes. Okay. Okay. What are they aiming for in the next few days? With everything that you’ve shared with me, I would hope that anybody on their team would aim for a removal of the breathing tube as quickly as possible. Has that been mentioned?
Ron: No. They don’t want to remove that right now. Because I asked that, when will he be able to come off the ventilator. They’re like, the way he’s breathing. No, he can’t come off right now.
Patrik: Right. Okay. Okay. The reason I mentioned this again, as long as your son is sedated, nobody can say what his brain function is going to be like. And that’s why I sort of said in the beginning, they need to start weaning off the sedation so you and they can get an idea of is a neurological condition.
RECOMMENDED:
Ron: You’re talking about everything. Precedex. They were saying at that point Propofol doesn’t take very long time.
Patrik: That’s exactly right. Propofol is short acting whereas-
Ron: Yeah, short acting.
Patrik: Yeah, that’s right. Propofol is very short acting. And did you say he was on Versed as well at some point?
Ron: Yeah. Versed.
Patrik: And it’s good that they’ve taken off the Versed because it is long-acting and you don’t want the Versed if you don’t have to, because you want something like the Precedex, or like the Propofol where people can wake up quickly. So that all makes sense.
Patrik: Can you tell me a little bit more when your son had a cardiac arrest? It was outside of hospital, I would imagine.
Ron: No, it was actually inside. Like I said, he was post-transplantation, so he was still inside.
Patrik: Oh, I see. Post-transplantation.
Ron: Yeah. Since the transplant. Yeah.
Patrik: Right. Okay. Okay, I see. I see. Okay. So at least he was in the right place because that would mean somebody would’ve reacted straight away.
RECOMMENDED:
Ron: Yeah.
Patrik: Right. I see. I see. Did you say treatment for stem cell cancer? Is that what you said?
Ron: Yeah, he has an immune disorder. Auto- immune disorder.
Patrik: I see, I see. And what was the treatment prior to cardiac arrest for that? Was he on chemotherapy or-
Ron: He wasn’t on chemotherapy. He stopped his chemo for a while. At the time, they were treating him for this EK virus. And then they were giving his normal prophylactic medications.
Patrik: Right.
Ron: Right. But the main-
Patrik: Right. And did any of the previous treatment potentially trigger the cardiac arrest? Is there any evidence of that or-
Ron: That’s the thing. They have no idea what. They still have no idea what.
Patrik: Right. I see. Sometimes what-
Ron: They didn’t see any bleeding on the brain or anything like that.
Patrik: Right.
Ron: No bleeding on the brain, his lungs were functional. His EKG, his Echo was functional. So they couldn’t find out what it was. They did a CAT scan, didn’t show anything. So we did an MRI. Then I think they saw some white matter in the core part of his brain.
Patrik: Yep. Yep. I see. Sometimes what can happen with the treatment that you’ve described, electrolyte levels are dropping. What I mean by that is, if for example potassium or magnesium levels dropped down through some of the treatment that you’ve described, a cardiac arrest can happen. Now that’s speculative and there’s probably no way to find out whether at the time of the cardiac arrest, the potassium or magnesium levels were low. Unless they’ve done a blood test at the time, which they probably have done at least in the first hour after the cardiac arrest, they would have done the blood test, and they would be able to track back whether any electrolyte levels would have been out of order.
RECOMMENDED:
Ron: Right.
Patrik: Right. That could be one of the reasons, but at the end of the day, it would be good for them to find out because they would want to prevent that going forward.
Ron: Going forward.
Patrik: If he is on dialysis at the moment, if they are removing fluids, they would have to supplement potassium through dialysis, right?
Ron: Yeah, they have K in it.
Patrik: Yes, yep. Yep. So that’s, that’s good that they’re doing that with. Has the neurologist given you any hint of what they would expect going forward on a neurological level?
Ron: Well, given a look of the MRI, and him not really responding, as they would look for somebody to respond. They’re very pessimist about it.
Patrik: Right, okay. Okay. Do you also know what ventilation settings he’s on at the moment? Sorry, I’m jumping around a bit here, but the reason ventilation would be important is to get an idea of how close is he of coming off the ventilator.
Ron: Well, they’ve been changing his ventilator back and forth, back and forth. Right now they have him on a PEEP of 7 and they have him on 90 oxygen, tidal volume of 260.
Patrik: Okay. And did you say in the beginning, is he breathing spontaneously or is he not breathing spontaneously?
Ron: It’s spontaneously, you know, but they flipped it over to assisted.
Patrik: Okay. Yep. Okay. Well that’s not too bad because that’s a sign that he has some level of awareness. That means he’s not-
Ron: Yeah, I can see little breaths in between.
RECOMMENDED:
Patrik: Yeah, that’s good. That’s good. Because that means he’s breathing. That’s a sign of alertness and it’s also a sign that there’s a good chance that he can come off the ventilator. This is where I was going with this in the beginning. You know, when somebody is sedated, chances are they can’t come off the ventilator. And the more awake your son is, the higher chances he can come off the ventilator. Right. And that’s why I’m sort of still suggesting that better sooner than later they should stop all sedation to make a proper assessment of, is he opening his eyes, is he responding, is he squeezing fingers, if you ask him to. Have you or the team ever tried that?
Ron: He hasn’t done any of that.
Patrik: You’ve tried that?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!