Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
My Mother Had a Cardiac Arrest and Her Level of Consciousness is Not Improving. Help!
You can check out last week’s question by clicking on the link here.
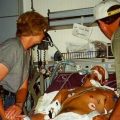
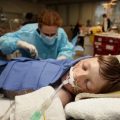
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Stephanie as part of my 1:1 consulting and advocacy service! Stephanie’s mother is a post cardiac arrest patient in the ICU and Stephanie is asking why her mom is having this inflammation and fluids going into her lungs.
My Mother Had a Cardiac Arrest and Remains Ventilated. Is the Fluid in Her Lungs a Sign of Deterioration?

Stephanie: Well, hello there Patrik.
Patrik: Hello Stephanie, how are you?
Stephanie: I’m good, I’m good, just tired. My sister is here?
Patrik: I am so sorry.
Stephanie: No problem.
Patrik: I am so sorry.
Stephanie: No problem.
Recommended:
Patrik: I tell you what I think happened. I really do believe I was fast asleep because it was 1:00am for me-
Stephanie: Oh I do too.
Patrik: That’s what I think.
Stephanie: You’re fine.
Patrik: And look normally … don’t get me wrong, I have phone calls in the middle of the night all the time and normally I do wake up. I feel so bad, I’m so sorry. But-
Stephanie: Well, please don’t and I want you to understand that I don’t hold it against you. We kind of worked you around the clock. I do understand that and we were tired too. But I don’t feel so bad because you didn’t quit us with what we need in order to still have the conversation with them, you know what I mean?
Patrik: I would hope so, I would hope so. So, what are they saying? Thursday or Friday they will do the trach?
Stephanie: Well, that’s a good question as to the day. Let me see, let me update you.
Patrik: Because from your text they’re saying … oh hang on.
Stephanie: She’s reasonably okay today.
Patrik: Yep, right.
Stephanie: Right, so that means within a few days they’ll be doing the trach, right.
Patrik: Right, and what’s the delay because from my perspective, now you’ve given them consent, you know, from my perspective there shouldn’t be any further delay unless they don’t have the resources to do it in the next couple of days, that would be fair enough. But, –
Stephanie: No, they said it … I would have to check to be sure. But, if they thought they were going to have to do an arterial line, before we left the hospital he said “No, we don’t have to do one because her pressure was stable”, but Miranda said her blood pressure’s going up. I think that’s Miranda now, hold on a minute.
Patrik: Yeah, sure, sure.
Stephanie: No, hold on.
Confusing. Alright Patrik maybe we should get Miranda on the phone.
Patrik: Yep, do you want me to dial her in?
Stephanie: Yeah. Go ahead, okay.
Recommended:
Patrik: Do you want me to dial her in?
Stephanie: Take your time.
Patrik: You tell me when you want me to dial her in.
Stephanie: Okay, it’s just that I don’t like the nurse like, she is the one from last night. She asked me to wait for rounds. Oh my God. So she wanted to ask some questions. The nurse said it’s not as important but Miranda was worried about her fluids and what has happened with her fluids. They found out that her lungs are being flooded, okay. They choose to rotate her in bed. They took a CT scan or something of her chest last night. Or some kind of a scan of her chest x-ray maybe, but I think they did take it and it said her lungs are almost half full. So, my thing is, let me talk…
So, my thing is, we told her days ago. They saw her problem but in my opinion they ignored it thinking that we were going to put her to sleep, you know what I mean?
Patrik: Yeah, yep.
Stephanie: So, another thing brought up, but they call it inflammation, you know, just to make her swell.
Patrik: Right, I tell you what I think. You remember you mentioned the swelling the day before I believe and I said it’s often from being immobile. Now that you’re telling me that her lungs are filled with fluid, there’s three other components to that. Three other components. So, number one, do you remember I asked the nurse about kidney failure? She denied that. Do you remember that?
Stephanie: You asked her once.
Patrik: Right, so they denied kidney failure because that’s the first thing you know. If fluids are being-
Stephanie: Exactly, exactly. That’s why I asked you. And I’m not a doctor.
Patrik: Yep, that’s fine.
Stephanie: Even when you talk to him, he said at that house, he said she’s making urine.
Patrik: Correct.
Recommended:
Stephanie: But then he gave you a number.
Patrik: Correct. That was fine, the numbers were fine.
Stephanie: Right.
Patrik: The numbers were fine. So, we can rule out kidney failure. We can rule out kidney failure, right. But, then there’s two other issues that could contribute to fluids in her lungs. Number one, is then, so in Intensive Care it’s incredibly important that the fluid balance is maintained. What does that mean? You’ve got to look at that what’s going in is coming out as well.
Stephanie: That’s right.
Patrik: Right.
Stephanie: And that’s what they were talking about, right. It’s not coming out.
Patrik: So, if they were giving her more fluids than were coming out in the last few days, well there’s fluid build-up in the lungs, okay. Because, unlike if you drink too much, well you go to the toilet. But she can’t regulate that at the moment so much, right? They have to regulate it for her, right. So, that could be one thing. But here is another thing what might have happened, with the cardiac arrest, her heart might be weakened to the point where it can’t pump the blood around sufficiently and if the heart can’t pump the fluids around sufficiently there could be fluid build-up in the lungs. So, those are the two probably reasons, one of the two or a combination of both, are the reasons most likely why there’s fluid build-up in the lungs.
Stephanie: Right.
Patrik: What are they saying with the … have they got a strategy to reduce the fluid build-up?
Stephanie: That’s what I said to them, “What do you plan to do to mitigate it?” Oh boy, they are going to do something to mitigate it, I can’t think exactly what.
Patrik: Lasix or Furosemide?
Recommended:
Stephanie: Oh, he said that she can’t do Lasix. That’s what he mentioned, she can’t do Lasix because of her blood pressure. What will Lasix do to the blood pressure?
Patrik: Okay, she’s got a low blood pressure-
Stephanie: If it’s high or if it’s low, one-
Patrik: You remember the last thing that they mentioned was that the blood pressure was low which is why they’re trying to put a central line in.
Stephanie: Right. Now it went up higher. He said “Oh, her blood pressure’s fine so we don’t need to put a central line in”. He said that today. He said it was 98, or her mean was, over bottom 60 something, so her mean was really good.
Patrik: That’s good, that’s good. So, because, if her blood pressure’s good, I can’t see why they can’t give Lasix. If blood pressure was low, I say “Okay, be careful with the Lasix”, but now that the blood pressure is fine I can’t see why they can’t give Lasix, I can’t. I would be very happy, when we come off this call, or what we can do like what we’ve done in the last two days, if you want to get Miranda into the call and if you want us to call the nurses there, we can do that, you know.
Stephanie: Oh, this is … yeah that nurse you talked to last night is the one. She didn’t seem too forthcoming. But then again, when you asked the question, she did give you the answers, correct?
Patrik: Absolutely. No she wasn’t forthcoming but she wasn’t … look, if I find one thing in the United States in particular, the nurses tend to be fairly friendly if you’re not, you know, if you are friendly, you know.
Stephanie: Yeah, okay, not antagonistic, yeah.
Patrik: Yeah, not antagonistic, exactly. So, I can’t see … you know, so far we’ve been getting all the information, you know, so I can’t see why-
Recommended:
Stephanie: I wish we had gotten the lady at 7:00am because she was amazing, the Filipino lady. She would tell you everything you needed to know. But she got off at seven, but she said “I’ll be back in the morning at seven”. Okay, then maybe we should make that call.
Patrik: We can talk to her –
Stephanie: But if you feel we should find tonight … I’d just feel better with the lady in the morning.
Patrik: Right, okay, we can keep that –
Stephanie: She was sure of herself.
Patrik: Yeah, which is important. No, no, we can ring after seven in the morning, that’s fine. I’ll be guided by you. Let me ask you this. So, trach Thursday or Friday, and then they still want to send her to LTAC.
Stephanie: No. They said no. They said at that point she said she’s not going to be stable.
Patrik: Exactly.
Stephanie: So, no we couldn’t, right. I said well, we would have made the decision on Thursday or Friday had you guys not been saying you want to ship her out the next day. We said well she was stable then but she became unstable over the weekend. Well, you led us to believe that you wanted to ship her out. But, see what happened was the social worker came in her today and she gave Miranda a piece of paper to sign. Now, she explained this paper and said it’s something for patient’s rights. Just to say that she told us that we have a right to appeal and I told Miranda, “Well I don’t think you need to sign anything”. But-
Patrik: I wouldn’t sign anything.
Stephanie: Yes, well she signed it and I said “Maybe she can go back and say I’d like to withdraw my signature”. You know.
Recommended:
Patrik: Good, I wouldn’t sign anything.
Stephanie: Huh?
Patrik: I wouldn’t sign anything.
Stephanie: She already signed it. I tried to tell her but my family, I said “Miranda I don’t know if I would sign anything”. She said “Well this one’s just saying” you know, whatever, whatever, it came from a social worker. So, to me, what does that say? You know, and you can appeal medical whatever, your medical insurance or something like that. That’s what that was saying. So the question is what did she just sign? She has a copy of it, Miranda does and she’s up here now. But we just come in at nine.
Patrik: Right, right, I wouldn’t sign anything if I was you, but for now I think, let’s do the trach, let’s keep her in there for the weaning and I mean, you’ve already seen that if you are pushing back, you know, in a nice way, if you’re pushing back in a nice way, they’re not … all you need to do is need to say to them “Hey, hang on a sec, I don’t agree with what’s happening there”. That’s all often you need to do, you know.
Stephanie: Well, this is what he said. Go ahead.
Patrik: They know that you’re talking to someone who has experience. They know that by now. They know that the questions that are coming are not … they’re the right questions. Right, they know all of that by now and they know that you can’t be fooled.
Stephanie: Yeah, and Dr. Reynolds was like, you know he was straight forward in saying, not in a bad way but saying “I would break my back you know, if this was my mom and there was anything we could do”, blah, blah, blah, and I said, “Well you don’t know what you don’t know”. And, I said to Dr. Watson, I said “Dr Watson, I asked you at the meeting, you know where is she on the Glasgow scale and you admitted you didn’t have any numbers. You told me there was … you didn’t have any numbers”.
You know, but she said “Yes I did, I said three, I did say between three and five”, then I said “Wait a minute, I think you told me that you said that. Maybe I just didn’t hear”, you know what I mean. So, then she said between three and five, but today she said she was on five. So, to me, she went up.
Patrik: Yep, she went up. No, no she didn’t-
Stephanie: I mean-
Recommended:
Patrik: Yep. And what did they say about the seizures and about the neuro storms? Did they say more about that?
Stephanie: No, they didn’t even talk about that. They just said that her body now is unstable, not just her mind, but now her body is, because of the infection, you know and I said “Well, you not giving her any” … as you know, it wasn’t until last night that we talked to that nurse, that all of a sudden they started trying to find out what they can give her for infection. So, now today they’re giving her stuff for her infection, they were talking about an internal line last night, and they’re talking about essentially what to put her on this big piece of plastic and a couple of plastic things up under her legs to try to measure what her fluid levels were. You know what I’m talking about? It’s a wedge.
Patrik: Yeah, yeah.
Stephanie: That puts her at a certain angle so they can tell what her fluid levels are. And, he said wants our permission to okay this internal line. I said “Yes, we already said yes to that and we already said yes to the trach”. He said “I want to make sure in person”. So, I guess we need to find out exactly what day they plan to do it. We said that when they do it we want the most experienced person doing it. And he does them all the time.
Patrik: Yes, so, get the date for the trach, right, but then still be very clear to them that you do not want her in LTAC and if they say there is insurance issues, I mean I’ve given you … I’ve sent you the links you know about that.
Stephanie: Right, beautiful, yes I’ve sent it to my family too.
Patrik: Right, good, good.
Stephanie: We found out that Carmen does have insurance.
Patrik: She doesn’t have insurance?
Stephanie: She does. She does, she does. Yes, she does. The name of the insurance is, it’s an HMO but I think of a HMO based off of Medicare or whatever the case, she does have insurance.
Recommended:
Patrik: Yep.
Stephanie: And, you know, so I told Miranda I don’t think she should have signed that paper but she listened to my sister Tonette who signed a paper for Miss Joana. See Miss Joana, who is her mother-in-law, she was staying … she chose to die at home, you know what I mean. She chose not to do anything. So, I didn’t feel good about the paper coming from the social worker, you know, but everybody turned around looking. And, I told Miranda but she didn’t, she was sitting down at the coffee table, but she didn’t listen to me. You know, the lady’s trying to cover it up and I said “Well read it, what does it say?” You know, and I definitely wouldn’t sign … I didn’t feel comfortable with signing anything at all.
Why are we signing anything?
Patrik: Correct, correct. The only thing that I would sign for is for the trach. You know, that would be the only thing that I would-
Stephanie: Right, but this paper from the social worker about appealing, you know if we should want to push her out of the … our rights. What our rights are. The paper says supposedly what our rights are. And, if we wanted to leave, they want to leave and this applies to whatever and we could appeal it and to me that’s the form.
Patrik: Very much so.
Stephanie: But I don’t know, I think it is.
Patrik: Yeah. And, also, bear in mind-
Stephanie: They’re getting Miranda a copy.
Patrik: Okay, okay, maybe if you do get the copy, maybe if you can take an image and maybe send it to me.
Stephanie: Got it, I will, I will send it to you. Yeah, yeah, okay.
Patrik: And, you can see, and this has been exactly my point from the start, Stephanie, you remember I said if something happens, they can’t look after her in LTAC and that’s exactly what’s happening now. Because, if it was up to them, she would have had the trach last week and she would have gone to LTAC and now-
Stephanie: That’s what everybody says, she would be right back home again.
Patrik: She would be right back in ICU. It’s way too early and they trying to push patients out without looking at well, what could go wrong, what if, you know, and the back and forth is not what she needs. She needs to be in a stable environment.
Recommended:
Stephanie: No, nope, they’re constantly moving forward.
Patrik: Constant, yes exactly. And LTAC is a better nursing home. That’s what it is. That’s what LTAC is. And, also, here is the other important thing. Have they in all of this, have they in all of this ever mentioned that your mother might be brain dead? Have they ever mentioned any of it?
Stephanie: Not at all.
Patrik: Yeah, yeah, no, no, good, good. And, with the GCS, you know a patient who is brain dead would be consistently a GCS of three, consistently, right.
Stephanie: Consistently, what three, three of what?
Patrik: A Glasgow Coma Scale of three.
Stephanie: Exactly.
Patrik: Right and that has never the case.
Recommended:
Stephanie: Right, they say she’s got five and she’s got abnormal activity and I did question the fact that Phenobarbital is a sedative, but they said it’s not enough to do blah, blah, blah, and I said “Well, what else is she on, what else is she on?” They said … I said “Is she on Keppra?” Now he said “She’s on …” oh, what’s the other one?
Patrik: Keppra, Dilantin?
Stephanie: No, Vi … Vim-
Patrik: Vimpat?
Stephanie: Vimpat I think.
Patrik: Okay-
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!