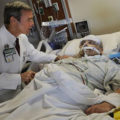
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
What Should I Expect My Mom Coming Out of Sedation in ICU and Waking Up After a Tracheostomy in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Lloyd, as part of my 1:1 consulting and advocacy service! Lloyd’s mom is in ICU, ventilated with pneumonia. He is asking how his mom can be weaned off the ventilator in ICU.
My Mom Has Pneumonia in ICU & How Can She Be Weaned Off the Ventilator?
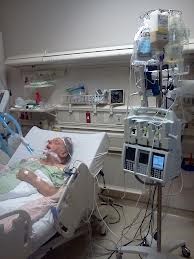
“You can also check out previous 1:1 consulting and advocacy sessions with me and Lloyd here.”
Belle: Right. Yeah.
Lloyd: Okay.
Belle: And I’m assuming they’re not going to take any chances. Within their own hospital they’re going to play it safe. They’re not going to kick her out.
Patrik: Not necessarily, I’ll tell you why. Their pathway is trach, PEG, and LTAC. That’s their pathway.
Belle: Right.
Patrik: Right? I really don’t know what the hospital has there. What’s the name of the hospital?
Lloyd: It’s a local hospital.
Patrik: Okay. We need to have a look at their website. Sometimes, if they are giving very limited information about their hospital, it’s not a good sign.
Lloyd: Okay.
Patrik: So, your next step should be, to ask within the hospital what’s available and start asking for neurology rehabilitation.
Lloyd: Okay.
Belle: Okay. But soon as the tracheostomy is in, they should resume all the rehabilitaion stuff?
Patrik: Very much so. Hopefully, I believe she needs to progress pretty quickly now. Tracheostomy, and then decisions should be made about where she’s going next. Or ideally, another situation that could unfold is she can be off the ventilator. And then the question is how quickly can she be decannulated, and have the tracheostomy removed? Is that an option at all?
Lloyd: Yeah. Well, we’re going to have to find rehabilitation on that one for the-
Patrik: That’s right.
RECOMMENDED:
Lloyd: Have to be like speech pathologist, I mean, yeah. Pathologist to be able to work with her. And that’s another thing. We need to find the resources, like a place where they can offer up all the possible therapies on that and that specific thing. And I guess that’s where the stroke specialist or neurologist comes in.
Patrik: That’s right. I’m just looking at the x-ray that you emailed, Lloyd. There’s just one thing there where it says in the x-ray atelectasis versus pneumonia. So, what they’re querying there is that she might have a pneumonia versus that she might have some atelectasis. What’s atelectasis? Atelectasis means that deep down in the lungs the alveoli are collapsed and the alveoli are where the gas exchange is taking place. So, what that means is where oxygen enters the bloodstream in the lungs and where carbon dioxide leaves the bloodstream, some of those areas might be collapsed, which might be because they’re saying atelectasis is versus pneumonia. So, they’re not quite sure what it is. I guess I would ask what they’re dealing with there? And is she on any antibiotics for that?
Lloyd: Yeah, she’s on three antibiotics. They have them on three different antibiotics.
Patrik: I see. Okay. All right. And do they think that potentially prevents her from getting extubated?
Lloyd: What? Say that again.
Patrik: Do they think that the atelectasis/pneumonia prevent her from getting extubated?
Lloyd: What? You know? Well, they did the extubation, so…
Belle: No, that’s been there for a while, I believe. I don’t think that was, that’s not a new thing. I think that’s been on… It didn’t stop them.
Lloyd: Yeah, it didn’t stop them. They don’t even know. They’ve been taking daily blood cultures, every time she spikes a fever and they can’t grow the bacteria. So they don’t know for sure if she has a pneumonia. They say she does. Some of the doctors were saying, oh, she has a pneumonia, but they can’t grow the cultures. And the infectious doctor was saying it’s like, but there’s some bacteria that don’t grow. So they’re not entirely sure if she had pneumonia or not.
Patrik: Right. Okay.
Lloyd: But they’re giving her, either way, they’re giving her the three types of antibiotics.
Patrik: Right. Okay. No, that’s good. That’s good. Do you have blood results?
Lloyd: Not from what they just did, I guess. Not from that, but…
Suggested Links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
Jimmy: Well, they put up the arterial blood gas, that test results are in.
Lloyd: Oh, just now?
Jimmy: Yeah.
Lloyd: Oh, wow. So what does it say?
Jimmy: What’s the main one that we’re looking for? The Oxygen (O2) content?
Patrik: Oh, yeah. Okay. We are looking for Partial Pressure of Oxygen (PO2) and Partial Pressure of Carbon Dioxide (PCO2) in particular. Can you see that?
Jimmy: Yeah, the PO2is 141.
Patrik: Great. That’s good.
Jimmy: And the PCO2 is 39.
Patrik: Yep. That’s pretty, both are within range. That’s very good.
Jimmy: That’s what came in. And then they did a metabolic panel. What did they do? The chest x-ray, and the pneumonia panel.
Patrik: What’s-
Jimmy: Which everything came out not detected.
Patrik: Right. Do you have a potassium there?
Jimmy: The potassium? Yes, they did that.
Lloyd: They had to give her extra potassium today, because she was low on it, but I don’t it might have missed it.
Jimmy: Yeah, it’s 3.5 right now, the potassium.
Patrik: Okay It’s a little bit low. Hopefully, they correct that by giving her potassium. Is there a lactate there?
Jimmy: Let’s see. Not that I see.
Patrik: Okay. All right. It’s not the end of the world. Some blood gases come with a lactate, some don’t.
Jimmy: It’s under the blood gas. Lactate, yes. It’s 1.2.
Patrik: Great. Okay. That’s good. That’s fantastic. Okay. It can be an early sign of sepsis, if lactate is high, but one point something is fine.
Lloyd: So I guess, yeah, but the liver enzymes were high and so we don’t know what to do as to the nurse about speaking to a doctor about that, because the Aspartate Amino Transferase (AST) was at 121 and the Alanine Transaminase (ALT) is at 128. And the normal range they say is like five to 34 or zero to 50 respectively.
Patrik: Right. Okay.
Lloyd: And so what would they do for that to bring that down? Is that they just have to wait and see, or?
Patrik: You mean for the oxygen?
Lloyd: No, for the AST and the ALT.
Patrik: Oh, yeah. Just wait. Yeah, just wait and see. But like you mentioned earlier, if she’s on a multitude of medications that might not help the liver.
Lloyd: Yeah. Do the antibiotics take a toll on the liver too?
Patrik: Most of them do, especially I would… Have you seen a list of medications she’s on?
Lloyd: Yeah.
Patrik: Right. Is it a long list?
Lloyd: Pretty much.
Patrik: Is she-
Lloyd: Yeah, go ahead.
Patrik: Is she getting Tylenol or Panadols?
Lloyd: No. Well, we asked them to start the Motrin, which I think is now what they’re giving, because of the liver enzymes. So they’re not giving Tylenol anymore.
Patrik: Right, okay. Because that would be one of the first drugs that needs to go.
Lloyd: Yeah.
Jimmy: Tylenol, it’s still on her list.
Lloyd: It’s on her…
Jimmy: They give her 650 milligrams by nasogastric tube every four hours as needed.
Lloyd: Yeah. But they said they stopped. As of yesterday, they stopped, so I don’t know. They might have not updated that part. They have a general list of all medications, but they don’t tell you. They put the list of all medications, but they don’t say if it’s stopped or if it’s still ongoing. It’s really just to kind of catch them.
Patrik: Right. Interesting. Do you have access, you have online access to medical records
Lloyd: Yes.
Patrik: Can you share a list of-
Lloyd: That’s what we’re looking.
Patrik: Right.
Lloyd: Yeah.
Patrik: Can you share a list of medications?
Lloyd: Yes. Should I screenshot it and send it to you?
Patrik: Screenshot it and send it. But you mentioned that your mom, prior to this hospital admission, have issues with the liver, is that right?
Lloyd: No. she was fine before, right, Paul?
Jimmy: Yeah.
Lloyd: Okay.
Jimmy: Never had any.
Patrik: Okay.
Suggested Links:
Lloyd: I mean, the good thing is that they’re giving her vitamins and they’re giving her a protein.
Patrik: Sure. Well, that should come, not normally.
Lloyd: Yeah. But yeah, I guess we’ll send that. I know we’re overtime, but I guess we’ll send that to you.
Patrik: No, we’ll have a look.
Lloyd: Reach out to you.
Patrik: Yes. No, we’ll have a look.
Lloyd: Oh, thank you.
Patrik: Did you have any other final questions?
Jimmy: Not me, Belle? Paul?
Belle: Do you have any recommendations for how we deal with this new doctor tomorrow? We’re trying to start with a fresh-
Patrik: Yeah, no.
Belle: He’s going to get filled in.
Patrik: Yeah.
Belle: What’s our strategy?
Patrik: Right. Let me ask you this. Do you think that this doctor, this week was difficult to deal with?
Lloyd: No. He was more accommodating than the last attending, but at the end-
Belle: He did a good job explaining things to us.
Patrik: Say, again.
Belle: He was good at explaining things or trying to explain things to us.
Patrik: Right.
Belle: He made an effort to explain things. The first doctor definitely did not do that as much.
Patrik: Right. Okay. Right. Look-
Belle: But to further his agenda, explaining things to make us sound like we have to do the Percutaneous Endoscopic Gastrostomy (PEG), but still she takes time to do it.
Patrik: Yeah. No, I hear you. Look, you might be surprised about it. It might get better. It might get worse. It’s hard to say. I do understand it weighs on family’s minds when they know there’s a change in doctors. I get that. Yeah.
Belle: Do you expect a new doctor to formulate his own opinions or is he going to just come in, read the case notes and everything and just say, I already know what’s going on? Or is he going to take the time to understand himself, hear from us and…
Patrik: Could it be that the same person shows up then the week before? Not this week, but the week before?
Suggested Links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
Lloyd: No, he said it was a completely different name.
Patrik: Right. I see. Yeah. Okay.
Lloyd: He gave us his name.
Patrik: Yeah. Sure. Look, my suggestion is you just wait and see.
Lloyd: Okay.
Patrik: You will gauge pretty quickly whether they want to form a completely different opinion or most of the time they fall in line. But you know, you never know. There are some doctors, they do form their own opinion, but a lot of it depends on where they are in the ranks. The younger ones fall in line. The older ones may be more confident in making up their own mind.
Suggested Links:
- THE 3 MOST DANGEROUS MISTAKES THAT YOU ARE MAKING BUT YOU ARE UNAWARE OF, IF YOUR LOVED ONE IS A CRITICALLY ILL PATIENT IN INTENSIVE CARE!
- QUALITY OF LIFE NURSING SERVICES FOR VENTILATED ADULTS WITH TRACHEOSTOMY AND THEIR FAMILIES AS A GENUINE ALTERNATIVE TO INTENSIVE CARE
Belle: Yeah. Okay.
Lloyd: Well thank you so much for all your time. I’ll send you that list of medications.
Patrik: Please. That would be really helpful.
Lloyd: Appreciate it.
Patrik: That would be really helpful.
Lloyd: Yeah.
Thank you for being there and thank you for guiding us through it. We were at a loss, so we appreciate that you were able to talk to us throughout this whole situation. It’s a comfort for sure.
RECOMMENDED:
Patrik: It’s a great pleasure.
Lloyd: All right, well thank you, Patrik. We’ll talk soon.
Patrik: All the best for now. I’m sure we’ll talk soon. Thank you so much. Thank you.
Lloyd: All right, take care.
Patrik: Bye-bye.
Lloyd: Bye.
Patrik: Thank you.
Belle: Bye-bye.
Patrik: Bye.
Lloyd: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!