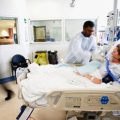
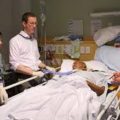
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Why is my Mom Not Waking Up After Being in an Induced Coma in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Lloyd, as part of my 1:1 consulting and advocacy service! Lloyd’s mom is in ICU, ventilated and he is asking how can his mom be able to get off the ventilator and avoid tracheostomy.
How Can My Mom Get Off the Ventilator in ICU & Avoid Tracheostomy?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Lloyd here.”
Patrik: Yeah. Okay.
Belle: That’s it.
Patrik: Okay. All right. With the insulin quickly, is she diabetic?
Lloyd: No, just as a result of the stuff that was going on.
Patrik: Yeah, no, that’s fair enough. A lot of patients in ICU are on insulin temporarily and they’re not diabetic. Yeah, no, that’s good. That’s good.
Lloyd: Yeah, she’s normally not diabetic.
Patrik: Yeah, no, that’s good. The question really is, why is she not waking up? Because from a ventilation point of view, I’d say she’s very close of having another extubation. Assuming she’s awake, assuming her arterial blood gases confirm that her ventilation is adequate and give her enough oxygen and she can blow off the carbon dioxide, then she should be extubated.
Belle: What’s the magic numbers for the … Those ABG numbers, what numbers do you need to look for?
Patrik: Yep. So PO2, which is oxygen in the arteries, should be greater than 70 millimeters per mercury roughly. And PCO2 should be between 35 and 45 millimeters per mercury.
Belle: Okay. The last readings she did, I mean this was a long time ago, she was at 37 and 190.
Patrik: Okay, that’s pretty good. That’s pretty good. Does she have an arterial line, do you know?
Lloyd: I don’t know what that means.
Patrik: When you look at her … You can look at her monitor. Is there a red line that measures her blood pressure in real time?
Lloyd: Oh, sorry, struck out. Sorry, she just struck out. Is there a red line that measures-
Patrik: Her blood pressure in real time?
Lloyd: No.
Patrik: Okay. Then she doesn’t have an arterial line. The reason I’m asking is if she hadn’t-
Lloyd: She had her blood pressure right now, though she has like a cuff.
Patrik: Yeah, yeah, a cuff, yeah.
Lloyd: Her blood pressure is 136 over 59. But not from the respiratory machine.
Patrik: Right. Because if she had an arterial line then they could very easily check the blood gas. Even if she doesn’t have an arterial line, they have to manually take a blood gas and they have to stab her for that. That’s very painful. Requires some local anesthetics, it’s quite painful. So again, what they’re not telling you is how much time do they want to give her to get extubated again? And if they do a tracheostomy, it’s disappointing that they haven’t told you they probably want to send her to an LTAC. When they asked you to give consent to a tracheostomy, have they asked you to give consent to a Percutaneous Endoscopic Gastrostomy tube?
Lloyd: Yes.
Patrk: Right. What was your response to that?
RECOMMENDED:
Lloyd: Well, we wanted to do more research.
Patrik: Okay.
Lloyd: We wanted to do more research on it. We have no idea, this is the first time we’re dealing with anything like this.
Patrik: Sure, sure.
Lloyd: We’re unaware.
Patrik: Yeah, no, I get that. I get that. So again, what often happens in situations like this, if they ask families for consent for a tracheostomy they ask for consent for a PEG (Percutaneous Endoscopic Gastrostomy) as well. Again, I feel like one doesn’t need to go with the other. She can be perfectly fine by having a nasogastric tube and getting nutrition via the nasogastric tube without needing a PEG tube.
Lloyd: Sorry, can you repeat that? I’m sorry, without the … What’s the other option to the PEG tube?
Patrik: Yep. So let me describe this. She probably has a tube in her nose at the moment, doesn’t she?
Lloyd: Yes, yes.
Patrik: Right. That’s where her nutrition is going in, okay?
Lloyd: Yes.
Patrik: That tube can stay in up to six months, no need for a PEG tube. They’re not telling you that. Why do they want the PEG? I’ll tell you why they want a PEG. If they want to send her out to LTAC, LTAC will only take patients with a PEG tube. They will not take patients with a nasogastric tube. I’m not going into detail why that is. But by you not giving consent to a PEG tube, that’s almost your insurance that she’s not going to a LTAC or to a skilled nursing facility. And you can still give consent to a tracheostomy if that’s what’s needed. But again, I believe she’s very close to coming off the ventilator if she’s awake.
Suggested Links:
Lloyd: And awake is just following, like moving her toes?
Patrik: Following commands, following simple instructions.
Lloyd: I mean, she can, she’ll look at people. She’ll follow their finger or she’ll look at people when they’re talking to her. But she can’t squeeze the hand and she no longer follow commands.
Patrik: Yeah, that’s really strange.
Lloyd: Or very slightly. And I don’t know if it’s because she’s laying down and she’s not being moved. There’s problem with the circulation going.
Suggested Links:
Patrik: Yep, that’s probably part of it. And the fentanyl is going in at 12.5 micrograms an hour right now?
Lloyd: No, she’s not on it. I don’t think she wants any pain meds right now.
Patrik: Okay, good. Good, good, good. No, that’s good. They need to keep that.
Lloyd: She might have been, overnight she had a little high fever, so like 101 and they gave her Tylenol overnight.
Patrik: I argue it’s fairly straightforward, she needs to wake up. And in order for them to help her wake up they need to sit her up, potentially get her out of bed, stimulate her, do physical therapy. That increases the chances of her waking up. Arterial blood gas to assess where she’s at in terms of, is that ventilation appropriate for her. And once she’s awake, I’d say, “Well, let’s get her off that ventilator.” The issue in ICU is that as much as we all want predict the future, ICU to a degree is very unpredictable. There could be unforeseen circumstances, there could be setbacks, but that’s just life, I guess. But that would be the, I’m describing here I believe the best-case scenario. And once that’s been achieved-
Lloyd: It’s possible.
Patrik: Once that’s been achieved, you should hopefully leave ICU reasonably quickly and get on with her recovery and her rehabilitation.
Lloyd: Okay, that’s great.
Belle: Which would take place where? Where would that rehab take place?
Patrik: Well, it probably depends. If she’s awake and she’s moving all limbs, might be in the hospital. If she is paralyzed, then it probably needs to be in a specialist facility. Ideally in a neuro rehabilitation facility.
Lloyd: And do you know if there’s one in this place?
Patrik: There probably would be, but I would need to do some research. My area of expertise is predominantly what’s happening in intensive care.
Lloyd: So, would it be good to bring her home? I mean, to try that at home or it’s just at a neuro rehab facility?
Patrik: I would probably be guided by the neurologist there.
Lloyd: Okay.
Patrik: Right?
Lloyd: Okay.
Belle: And how do we get the neurologist to talk to us? It seems like he just severed all communications.
Patrik: Right, right. Well, there must be a neurologist involved in this. I would argue that with a stroke she would have been admitted under a neurologist.
Belle: I don’t understand. I don’t..
Patrik: Right, right. But I would argue the admitting doctor there would need to be a neurologist because of a stroke.
Lloyd: The attending is a neurologist.
Patrik: Right. I’d say the neurological recovery at the moment is really subject to her getting off that ventilator. So, here are the two trajectories that I can see. One is, get her off the ventilator, that means she would need to be awake. And then hopefully they can rehabilitate her within the hospital or you can take her home, I don’t know. If for whatever reason she needs a trach, then the focus would shift from neurological rehabilitation to weaning off the ventilator, if that makes sense? That’s why I argue she’s at a critical point.
Recommended:
Paul: And what is that sweet spot? The sweet spot of when … I know she can’t be on the vent too long. She can’t be on it more than-
Patrik: Yeah, the tube-
Lloyd: Now she’s seven, eight days I should say-
Patrik: Yeah. Again, you’re right there. Sort of the two-week mark is what I would say the cutoff.
Lloyd: Okay, so we just have a few more days to get her to a rehab to-
Patrik: Well, you say it’s day eight today, I think you have more than two days. You have up to six days. And then the question is, let’s just say you’re coming to the day 14 mark and she’s still, let’s just say she’s still on the same settings and let’s just say she’s awake by then. Then I’d say, well, she’s very close. Again, you have to do then a risk benefit analysis. Should you take out the tube and give her a second chance of extubation? And if that fails, yes, then she probably needs a trach. But I’d say you have, I’d say given with what you’ve shared with me, I believe you have reason to be optimistic here. She was awake last week.
She’s on almost minimal ventilation settings. Almost, not quite, but very close. If they can get that pressure support down to eight and the volumes stay the same. If they can get the oxygen down to 35% and she’s not getting exhausted and she’s not doing the belly breathing and she’s awake and the blood gases are within range, take that tube out. And have the BiPAP ready in case she needs it. I hope I can illustrate to you that there is a stark contrast between taking out the breathing tube and get on with her recovery versus tracheostomy. They want to then push for a PEG tube, send her off to LTAC where the focus is on weaning people off the ventilator. It’s almost like a difference of day and night.
Lloyd: Yeah, this is common. This is info we didn’t have, so I appreciate that.
Patrik: And this is the part-
Belle: Do they have to obey us in terms of delaying this for six more days or whatever? Do we have the ultimate say? Can they just come and say, “We’re not waiting anymore.”
Patrik: Yeah. Look, I don’t think they’ve got any reason from what you’ve shared with me. Again, all I can say is I believe she’s very close. Can they delay? Yes, of course. Ultimately, they are the health professionals in charge of her care. But I guess I hope I’ve armed you with enough insights so that you can ask the right questions.
Lloyd: I think so.
Recommended:
Patrik: Yes, of course. In what I’ve seen certainly, if they’re not doing what you think they should be doing. Yes, of course you could put more pressure on, of course, I would. As I said, the big question mark to me at the moment is, why is she not awake? That’s the big question mark.
Lloyd: Yeah.
Patrik: And especially, which hospital are you at? Which hospital is it?
Lloyd: A local hospital.
Patrik: Right. A stroke center, is it? Right. Okay.
Lloyd: Yeah.
Suggested Links:
- Quick tip for families in ICU: Should I get access to my critically ill loved one’s medical records?
Patrik: Right. So abound, I believe she’s halfway there. She’s more than halfway there. But why is she is not waking up? Is it just too much fentanyl in the last few days? Is it just sort of the hangover from that, or is there something else?
Lloyd: Okay, so we’ll ask that. And then should she have an outside doctor?
Patrik: Should she have an outside-
Lloyd: Yeah, a doctor that’s not-
Belle: She has no doctor, like normal medical stuff, she’s never had a real doctor.
Patrik: Oh, I see. Probably should. Probably have a family doctor, yes.
Paul: I guess we just have to find one.
RECOMMENDED:
Patrik: Yes, yes. That would be advantageous, I think. And just remind me, your mom’s been fit and healthy up until this event?
Paul: Yeah, I mean she has breast cancer, but super healthy. Super healthy.
Patrik: Yeah. Do they suction her regularly?
Lloyd: Yeah, they try. I mean, they do sometimes I have to call them to get suction and I think right now she probably needs to get suctioned.
Patrik: Right. And when they suction her, she’s coughing?
Lloyd: Yeah.
Patrik: Okay.
Lloyd: She doesn’t like it, she’ll cough.
Patrik: Yeah, sure.
Lloyd: And that’s what happened last night. They said that she was really good. I mean she has a strong cough. But the nurse said she doesn’t have a strong cough.
The 1:1 consulting session will continue in next week’s episode
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!