Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
What if the ICU is Guilt Tripping You? Live Stream!
You can check out last week’s question by clicking on the link here.
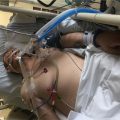
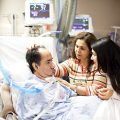
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Lloyd, as part of my 1:1 consulting and advocacy service! Lloyd’s mom is in ICU with swallowing difficulties and failed extubation attempts. He is asking how his mom can avoid aspiration pneumonia in ICU.
How Can My Mom Avoid Aspiration Pneumonia in ICU?
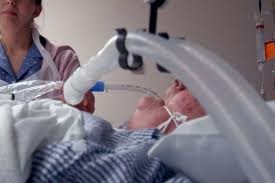
“You can also check out previous 1:1 consulting and advocacy sessions with me and Lloyd here.”
Belle: Hi Patrik! We’re all in.
Patrik: Good. How’s your mom?
Lloyd: All right. So, it didn’t work out the way we were hoping it would work out. So, I think what she has is something called dysphagia.
Patrik: Sure.
Lloyd: And so, the last time she had a similar symptom where she was, I think we explained last time that they put a trumpet tube so that it could clear out and then they didn’t want to do it this time. They were just like, there’s going to be a risk for, oh, aspiration or food going down the wrong throat or whatever. And so, we were telling her that we just wanted to go ahead with the tracheostomy.
Belle: I think Patrik needs a little more details about how it happened. Because she was doing much better over the last few days. The doctor went from not wanting to try it to this morning saying, we’re going to give it a shot, because she was getting stronger. You want to go over the vitals?
Lloyd: Yeah. She was able to kind of flicker, move her fingers and her toes, and she’s been very alert. She’s been staying up a lot of the day. She’s following commands. She’s tracking and she was doing pretty well.
Belle: And very minimal suctioning.
Lloyd: Yeah, very little mucus, that sort of stuff.
Patrik: Right. Okay.
Lloyd: Yeah.
RECOMMENDED:
Belle: Her volume was over 100. The volume went over 400 and they had her down to 35 yesterday, but that number, that’s
Patrik: Right. 35% of oxygen.
Belle: Yesterday, yeah, they put it back to 40 this morning, but they had it at 35 yesterday.
Patrik: Right. Okay.
Belle: So, everything was very encouraging. That’s why they went ahead with it, because it was so encouraging.
Patrik: Yes. But they didn’t, that I understand this correctly. They didn’t proceed in the end, did they?
Belle: So, they did, they removed the breathing tube.
Patrik: Oh, they pulled the tube?
Belle: But they didn’t leave it out for long.
Patrik: For how long?
Belle: The problem was that she was having difficulty while…
Patrik: And how did-
Lloyd: Well, when they saw that, because what they did was they saw that she had this, almost like when you have a snoring thing, they were saying that she was having trouble breathing. I mean, we saw her and it’s, yeah. So, what he did was he pulled the jaw out and I see it went away, once you pulled the jaw out, it opened the airway.
Patrik: I see.
Suggested Links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
Belle: This is what you got to explain the timeline, because they removed the tube successfully and there was no issue other than she couldn’t…She was coughing, she had a strong cough. She was bringing up mucus, but the mucus was sitting there. I guess she couldn’t spit it out or whatever the next step is. And in order for her to breathe fully, the doctor was pulling on her jaw. Can you describe that incident? I don’t remember how-
Lloyd: Yeah, she was pulling it out so that, yeah, she was pulling her jaw out so that I guess the tongue and the back of the throat, whatever it is, kind of separation. I’m sure you know what that is. And they said that she couldn’t, they didn’t want her to continue like that. And so they said they had to put the tube back in.
Patrik: I see. Okay. And how long did that take from extubation to reintubation? What timeframes are we talking about?
Lloyd: Well, they had to give her pain medications. I guess they kicked us out. So, we don’t really know exactly.
Belle: The decision was made in 10 minutes. The decision or the actual procedure? Because the decision was made very quickly.
Patrik: Right.
Belle: Within minutes.
Lloyd: Yeah. I mean, yeah, within 10 minutes.
Belle: He was very serious. The doctor was not fooling around. He wasn’t saying, do you want me to do it? This is not safe. We need to do it.
Patrik: Okay.
Belle: It was not, he wasn’t asking our opinion.
Patrik: Okay. I see. Okay. And from the time of extubation until reintubation, how much time passed?
Lloyd: Well, they did it right away. I guess they were numbing her. So, it must have been within, I would say within another 10 minutes or 15 minutes. We were out of the room. So, we couldn’t see the sequence of events. But the whole thing might have taken over 40 minutes, I guess, before we were able to come back into the room.
Patrik: Right. So less than an hour, really.
Lloyd: Yeah.
Suggested Links:
Patrik: I see. And they mentioned she got dysphagia. Is that what they said?
Lloyd: No, they were saying that it was like the tongue-
Belle: They were afraid to use the big tongue. They described it. They didn’t want to use the big medical term currently.
Patrik: I see.
Belle: When I researched it, that’s what came up.
Patrik: I see. Okay. But prior to extubation, do you remember when, I think a few days ago I texted you, I think what should happen if she can’t maintain a stable airway with Bilevel Positive airway Pressure (BIPAP) or Continuous Positive Airway Pressure (CPAP)? Do you remember that?
Lloyd: They didn’t even try.
Patrik: They didn’t even try that.
Lloyd: They didn’t want to try BiPAP or CPAP.
Patrik: Right. Okay.
Lloyd: They had an oxygen mask on her.
Patrik: Yep.
Lloyd: Just like a regular oxygen mask. But they didn’t want to try BiPAP on her.
Patrik: Right. Do you know if they’ve done an arterial blood gas after extubation?
Lloyd: I do not.
Patrik: Right.
Lloyd: I do not. Yeah.
Patrik: Okay.
Lloyd: But they did say that if she gets to tracheostomy that they’re confident that she’s not going to need the vent-
Patrik: Yeah I-
Lloyd: He was pretty adamant about, well, he seemed adamant about that.
Patrik: I agree with that. I understand what they’ve done, they pulled the jaw out. It’s called the jaw thrust. I get that. Did they use what’s called a Guedel airway? Did they put something in the mouth to keep the airway open? Did they put something in?
Lloyd: No.
Patrik: No. Okay.
Belle: Not that we saw, but, and I asked them if they could put the trumpet tube back like they did last time. He said, oh, like I said, he didn’t want to do it. He just thought that was going to be, at least until the tracheostomy, and he didn’t want to do it. She was just not having it.
Belle: He said it would keep delaying the inevitable.
Patrik: Sure.
Belle: He said it would work. It’s just that it would delay the inevitable. And the doctor is hung up on the fact that she cannot swallow.
Patrik: Sure.
Belle: She can’t swallow and doesn’t want to give her a chance to swallow.
Patrik: I see. Okay. Look-
Lloyd: And to add insult to injury, tomorrow’s going to be another attending day. Today was his last day.
Patrik: Yeah, sure. Yeah. Monday is often the change-over day. Okay. I see. Okay. So look, I guess given that she had two failed extubation attempts, I do believe the argument has been made for a tracheostomy if they are so certain that she can’t swallow, right? I mean, the only question that I have here is if she can’t swallow, was there coughing? Was she coughing after extubation? Could you see?
Lloyd: Yeah. I mean, she was coughing.
Belle: The doctor said she coughed very well. The doctor was happy with her coughing. The reason she wasn’t happy with the cough is that it actually brought up mucus from way down and she couldn’t get rid of it. But he was glad. He said the coughing was great.
Patrik: Okay. Because if she can’t swallow and she has a good strong cough, that could prevent everything that they’re trying to prevent, which is aspiration. If she can’t swallow, the biggest risk is aspiration so that her saliva is going into the lungs and causes an aspiration pneumonia. But anyway, look-
Lloyd: How do you treat the aspiration pneumonia?
Patrik: Oh, you don’t want to-
Lloyd: If she does get it, is that treatable?
Patrik: You don’t want to treat it to begin with. I mean, you want to avoid it to begin with. This is the thing. If they’re saying she can’t swallow, I agree that she needs a trach at least until her swallowing can be assessed better. And her swallowing can be assessed better if she has a trach in, as opposed to assessing the swallowing whilst she’s having a breathing tube in the mouth. The simple reason for that is that a trach is much more comfortable compared to a breathing tube in the mouth. And one way to test the swallowing is you can deflate the balloon at the back of the throat and then, with the speech therapy, you can assess whether she can swallow or not. And that is so much easier with a trach. But the risk due to-
Lloyd: So what… Go ahead, sorry.
Suggested Links:
Patrik: To answer your initial question, how do you treat an aspiration pneumonia? Well, you don’t want to treat it to begin with, because if someone, let’s just say they would’ve kept your mom off the ventilator, and she would’ve ended up with an aspiration pneumonia at that stage. She would need reintubation anyway. But you don’t really want to get to that place in the first place, if that makes sense.
Lloyd: Yeah. Well, I’m just asking.
Patrik: Yeah, sure.
Lloyd: If she swallowed some saliva today and the doctor was intimating, that she may have swallowed some stuff, but they couldn’t get everything. They couldn’t like suck everything up. So, they don’t know. But I was just like-
Patrik: I-
Lloyd: I just want to make sure. Go ahead.
Patrik: I argue they do know. And I’ll tell you why. So, after reintubation, they would’ve done another chest x-ray.
Lloyd: Okay.
Patrik: So they would see in the chest x-ray whether she aspirated or not.
Lloyd: They did another chest x-ray. Let me pull it up
Patrik: Right.
Belle: And if she aspirated, does that guarantee pneumonia, or?
Patrik: No, it’s not guaranteed. But I guess for someone as critical as your mom, I’d say chances are very high.
Belle: Endotracheal tube terminate approximately 4.9 centimeters above the carina. Enteric tube courses below the diaphragm with tip collimated from view. The cardiomediastinal silhouette is stable. No significant interval change, in mild bibasilar opacities, atelectasis versus pneumonia. Probable small left pleural effusion. No discernible pneumothorax. I will email this chest X-ray result.
Patrik : That would be great if you can send an email. Especially, I would be curious about what they’re saying about the pneumonia. Can you email it to …
Belle: Yeah, we can.
RECOMMENDED:
Patrik: Yeah, that’s all right. Can you just read out again what they’re saying there about the pneumonia?
Belle: Oh, well, it says, “The cardio mediastinal silhouette is stable. No significant interval change, in mild bibasilar opacities, atelectasis versus pneumonia. Probable small left pleural effusion. No discernible pneumothorax.”
Patrik: Okay. Yep.
Belle: I can send it. I can email it to you.
Patrik: I don’t know whether you can see what I just sent there? If you can email it to that email address, [email protected].
Belle: Okay.
Patrik: If you can email it to [email protected].
The 1:1 consulting session will continue in next week’s episode
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!