Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the questions was
My Dad had bypass surgery and he’s not waking up, how long will it take?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“ I want to answer the next questions from one of my clients Roman as part of my 1:1 consulting and advocacy service!
My Dad is still in coma after bypass surgery, what could be the reason for him not waking up?
Patrik: Hi Roman.
Roman: Hi Patrick. Yes.
Patrik: Okay. So thank you very much, I really appreciate you …
Roman: Thanks to you.
Patrik: Thank you being a client. Thank you.
So, let’s start … So, what we can do, and I can tell you I’ll be … so, we can break this up in two half-hour calls, if you want to we can go for an hour. But I think, I tell you what I suggest, we’ll go for half and hour, I’ll set you up with enough questions, I’ll explain to you the bigger picture, then you can go back to the hospital, ask your questions, and then we could do another half an hour later tonight, or however you feel. I think half an hour is enough for me to set you up with all the right questions.
Roman: Okay, I think the right approach so we can get back to you.
Patrik: Yeah, exactly. Exactly. And I will be ta- …
Roman: If we need more counselling, we will get more counselling from you for sure.
Patrik: You know, so let’s … I really want to give you as much value as I can, of course.
Roman: Thank you so much.
Patrik: So, what’s really important to understand is with your dad having had a heart attack 38 days ago, the pump function of the heart would have gone down significantly, right? And that’s why your sister mentioned 35%, and now it’s potentially 20%, right? The longer you wait from a heart attack to surgery, usually the worse it gets, right? Something that I’ve seen over and over again is that patients go on the balloon pump before surgery to keep the heart stable. That hasn’t happened, it happened an hour before surgery, but sometimes they go on the balloon pump a week before surgery to strengthen the heart, and that hasn’t happened in this situation.
Recommended:
But by also what I can see as well, by putting the balloon in they could see that surgery would be difficult. They could see that, that’s why they put the balloon in in the first place. And you remember I mentioned earlier seven out of 10 patients go for cardiac surgery without the balloon. That, to me, is a sign that the heart was fairly week to begin with. And also, when a patient goes to surgery with a balloon, nine times out of 10 they come back with the balloon, okay? Are you following?
Roman: No, I’m not necessarily following.
Susie: The balloon stays within the heart after surgery, that’s what he means.
Roman: That’s what we should understand is the balloon stays? But I’m not sure for how long.
Patrik: Yeah. They are right when they are saying it should be up to 72 hours. The reason it should come out after 72 hours is simply, number one, the heart should stabilize and, number two, it’s an infection risk. It’s a big infection risk, okay? Because it’s a foreign body, it’s a foreign machinery in the body. Yes, it’s stabilizing the heart, but it’s a big infection risk, right?
So, basically, what the balloon is doing, the balloon is basically pumping oxygen to the heart, because after a heart attack, especially you mentioned it’s been the second heart attack for your dad, part of his heart muscle would have died during those heart attacks, which means the heart needs more oxygen to compensate for the death of some of the heart muscles, okay? Are you following?
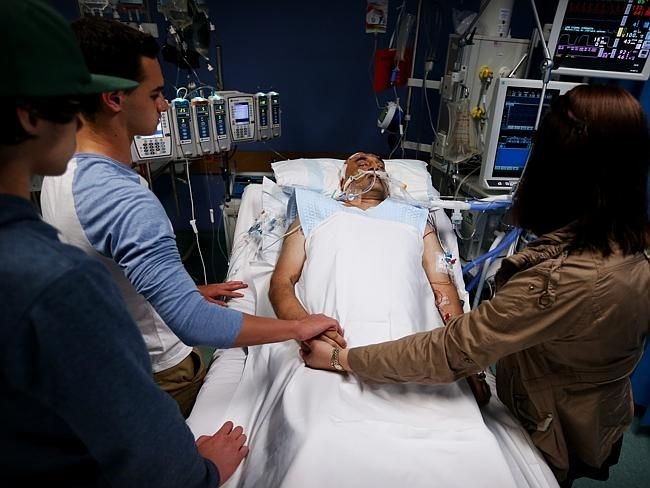
Find more information and recommended details about induced coma:
Roman: Yes, absolutely. And I think we were told that part of the tissue may die, or might already died, or something like that. It wasn’t the same after this.
Patrik: That’s right. And that’s why it would have been important to do the surgery quickly. So, what happens is: during the heart attack, the arteries supplying the heart with oxygen block off, the heart gets blocked off from oxygen throughout a heart attack. So, in order to minimize the damage by bypassing those blocked arteries the heart gets resupplied with oxygen, and that’s why the surgery should have happened fairly quickly to minimize the damage.
Roman: And that didn’t happen?
Patrik: That didn’t happen, for whatever reason. And it could have been that they found your dad was too unstable, that could have been one of the reasons.
Roman: We were told that his heart needed to adjust, or something like that.
Patrik: Yeah, that could be. For that call I have too little information, but let’s focus on what’s happening now. Let’s focus on what’s happening now. So, if a patient is stable after cardiac surgery, they often leave intensive care within 24 hours. 48 hours at the most, if all goes well, okay? So, with your dad going into surgery with a balloon, I could have almost … you know, if you had called me three days ago and you’d have said, “Oh, my dad’s going for surgery with a balloon.” I would have said, “He won’t be out of intensive care within 72 hours.” I could have predicted that pretty certainly.
But then the question is: why is he still in an induced coma? The reason why he’s still in an induced coma is probably the heart is too weak at this stage. In the ideal world, cardiac surgery repairs the heart to the point where it’s functioning back to a normal level, hence no need for the balloon pump, and, number two, no need for the blood pressure medication, okay? To illustrate that further, you would have seen your dad is on a ventilator at the moment.
Roman: Yes.
Patrik: Right. Ventilator, balloon pump, and the inotropes for the low blood pressure are all considered life support.
Roman: Yes.
Patrik: Ventilator, balloon pump, and the inotropes for the low blood pressure are all considered life support. With that amount of life support, your dad is not anywhere close to leave intensive care because they can’t look after those life support devices outside of intensive care. So, at this stage, looking at leaving intensive care is not even … it’s not on the cards, okay?
Find information about ventilator and life support:
Roman: Okay.
Patrik: Why is he still in an induced coma? Well, because he’s too unstable. The more life support patients are on, the longer patients need to stay in an induced coma. Before your dad will wake up, they need to stabilize him hence, number one, they need to get rid of the balloon if they can, number two, once the balloon is out, the next challenge is to wean the next level of life support off, which is the inotropes, which is for the low blood but I don’t want to get too medical here, right?
Roman: But it’s..It’s interesting.
Patrik: Yeah, no. No, it’s important. Yeah, what is it? I tell you what it is. Your dad has a low blood pressure because, number one, his heart is weak and, number two, he would have lost a fair amount of blood during surgery, right? It’s a pretty cruel procedure, I’ve seen it myself, I’ve been into the operating room witnessing surgery like that, it’s a pretty cruel procedure and patients are losing a lot of blood, okay?
So, yes, your dad would have been receiving one or two units of blood, and that’s fine, I’m not too worried about it; it’s almost standard. It’s almost like that’s part of the deal, okay? With the weak heart, if the heart is weak blood pressure will drop. Then, yes, the balloon can compensate for that for a little while, for a few days, and then they need to wean the balloon off to see what the heart is doing. If the heart is not responding to that, they need to use the inotropes or vasopressors … basically what it does, number one, it increases the pump function of the heart, so the heart’s beating stronger with medication support. And, number two, they are squeezing the blood vessels, so that the blood in the body is flowing towards the heart, right? Following?
Recommended:
Roman: Yeah. We are writing everyithing down.
Patrik: Okay, so you’re following?
Roman: Yes.
Patrik: I will give you some medication names when we come off this call, and the medication names will be fairly similar, even in Spanish, it will be very similar. So, that’s what’s happening.
Now, the challenge is the balloon needs to come off because of the infection risk, because of a foreign body, foreign machinery in the body, but if they can’t reduce the inotropes, or the vasopressors, that’s a challenge because that’s life support. And the reality is, let’s just look at the worst case scenario: if they took the balloon out and if they stopped the inotropes there’s a very high chance your dad might not survive.
Roman: Okay.
Patrik: Okay?
Roman: We can see why.
Patrik: Yeah, absolutely. Now, I always say to people, to my clients, this sounds pretty significant and it’s pretty critical, and whilst I don’t want to underestimate the situation by any means, panic is also the wrong approach. Panic is the wrong approach, okay? So, yes, he’s on numerous life support at the moment, but this is what happens in intensive care. That’s why people are in intensive care. Is this a reason for concern? Yes, absolutely. Is it a reason for panic? No.
Additional information about intensive care:
Roman: Okay.
Patrik: Okay? Definitely a reason for concern but no reason to panic, that’s why patients are in intensive care, that’s what intensive care units do: they keep people alive until they can live independently again, okay?
Roman: Okay.
Patrik: The other reason why it’s no reason to panic is more than 90% of intensive care patients do survive, and the question is: why should your dad not be within those 90%? There’s no reason your dad shouldn’t be within those 90%? Again, I have seen those situations over and over again, it’s definitely a concerning and a critical situation, but your dad can pull through it, right?
Related links:
Roman: Good.
Patrik: So, there is no reason why your dad can’t pull through it. It will probably take a little bit of time, and it will take some management skills from you, and you’re on the right track, you’re getting all the insider information, all the questions.
So, here is the next thing that’s important for you to know: with the induced coma, so they haven’t woken him up because he’s unstable, okay? And but the next question for you to ask is: what is keeping him in the induced coma? So you need to find out what drugs are keeping him in the induced coma, and I will give you … again, I will write you down some drug names when we come off this call. Because what’s important there: they’re short-acting sedation, which means when they take it off, your dad should wake up quickly, and there’s long-acting sedation which is for a prolonged induced coma.
Now, there is … we don’t know whether your dad will be in a prolonged induced coma or not, it will depend whether he will stabilize or not, okay? Both forms of long-term induced coma or short-term induced coma have pros and cons, like anything, okay? I would always advocate for a short-term induced coma, however, let’s just say you can predict somebody needs a coma for the next week, then you need to change the medication into a long-term induced coma because of side effects, and all of that.
Find more information and recommended articles:
Roman: Okay.
Patrik: Are you still following?
Roman: Yes. My guess, but this is only a guess, is that he’s in short.
Susie: He’s in short. I saw the name of the medication, and I recognized the name. I think he’s in short induced coma right now, with the medication.
Roman: We can verify it, but I think he’s in short.
Patrik: Do you know what medication he’s on? Do you have any drug names?
Susie: My brother sent me a link from how he found your information, and I think I recognize the name of that medication from …
Patrik: Propofol?
Roman: I think it’s with a D. Starts with a D.
Patrik: Hang on, what I’ll do is … just give me a sec. I’ll just write some drug names.
Susie: From this link …
Patrik: Can you recognize this?
Susie: Yes, Diprivan that’s it.
Patrik: Okay, good. So, with that we can already say he’s in a short-term induced coma, okay?
Roman: Yes.
Patrik: So, what that means is when they take the Diprivan off, he should wake up fairly quickly. He should, okay? So, that’s really good information to have, that he’s in a short-term induced coma.
Okay. So, then next, have they been mentioning anything about kidney function?
Recommended:
Roman: No.
Patrik: Okay, so here is what could happen. And again, it’s a pretty significant question that I believe you need to start asking. When patients have a low blood pressure, one of the main complications resulting from a low blood pressure is kidney failure. Now, what happens is, with a low blood pressure, the kidneys don’t get perfused, right? And the kidneys might … and I should say that, might temporarily fail, temporarily, okay? It’s a question you should ask whether they are concerned about kidney failure, okay?
Roman: Yes.
Patrik: And they will do daily bloods, and they can see, number one, they can see in the blood results whether the kidneys are failing or not. And number two, obviously, they measure urine output, and if, obviously, if urine output is minimal there’s a chance that the kidneys might fail.
Now, you mentioned earlier he’s been in pulmonary oedema?
Roman: Yes.
Patrik: Okay.
Roman: And other edemas that are from the skin and other tissue that …
Susie: Well, they said that he’s very swollen, but they said that that’s normal.
Patrik: Well, I’ll give you two ways to look at the swelling. Number one, the heart is not pumping at its best capacity, and that means there’s fluid retention because the heart can’t pump all the blood around the body, which means patients get swollen, number one. And worst case scenario is they go into pulmonary oedema. So, what happens is if the heart’s not strong enough to pump, there is reflux back to the lungs, and which is why patients are going into pulmonary oedema. However, the second reason why patients are going into pulmonary oedema is potentially kidney failure.
Recommended:
Roman: Okay.
Patrik: Okay? And it could be a combination of the two, the heart being weak and the kidneys potentially failing, okay?
Here is another important thing for you to understand: you mentioned earlier the 30%, right? So, here is why this is important: they’ve done an ultrasound before surgery, and they’ve checked what’s called ejection fraction. I’ll just type this in.
Roman: Yes, we’ve heard about ejection fraction.
Patrik: Right. So, you can see that ejection fraction basically means pump function, okay? So, an ejection fraction of 30% is too low. A healthy heart should be between 50% to 75%, right? And now you’re telling me it’s 20%, you obviously need to verify that, right? Need to verify that. And you need to ask why has it gone down and not gone up?
Roman: Yes.
Patrik: Right? I’ll tell you one of the risks during bypass surgery: one of the risks during bypass surgery is to potentially sustain another heart attack, I have seen it, because it’s high risk surgery. Yes, it’s surgery that’s being done every day, all over the world probably thousands of times, but it’s still fairly high risk surgery. So, you may want to ask them whether he’s sustained another heart attack, which could be one of the reasons why his ejection fraction might have gone down to 20%.
Now, one of the ways to find out if he had another heart attack is to ask for a troponin level, I’ll type that in.
Roman: Okay, troponin level.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!