Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the questions was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“ I want to answer the questions from one my clients Roman as part of my 1:1 consulting and advocacy service!
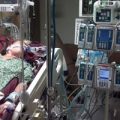
My Dad had bypass surgery and he’s not waking up, how long will it take?
Patrik: Hi, Roman. How are you?
Roman: Hi, Patrik. Thank you so much. Thank you so much for taking our call, and for being willing to give us advice at this very difficult moment. Also I have a bad cold.
Patrik: Doesn’t sound well.
Roman: Hmm..hmm..yeah. Terrible
Patrik: So this is really so that we can focus on the things that are important to you, I really want to find out your situation, and then I can tell you how I can help you going forward. If you do want me to help you going forward, I do charge a fee.
Roman: Yes.
Patrik: Okay. But it’s really about finding out about your situation, and then I can then tell you how I can help you. Yeah, just tell me about what you’re dealing with.
Recommended:
Roman: Yes. Well, my father had open-heart surgery on Monday. It was a triple bypass surgery.
Patrik: Yeah.
Roman: He’s 68. So, he’s not that young. He’s not that old either. Things to be noted, he’s diabetic, type 2. Has diabetes type 2. This was not his first heart attack. He had a heart attack in 2002, in the summer of 2002, which is actually our winter. And by then, he had a stent. It was only one artery that was compromised, and he had a stent, and the issue was taken care of for many years. And it seems, what the doctor says now, that it was not handled well in terms of his medication later on, because he had statina’s in Spanish. It’s statins.
Patrik: Statins, yes, I know what statins are, like atorvastatin, simvastatin. It’s a cholesterol controlling drug.
Roman: Exactly. So apparently he had a much lower dose than what he needed. He was with 10 mg and doctor said at least he should be 60 because he’s so bad, he had a heart attack already. So, he started to feel uneasy, 40 days ago or something like that. He’s been 35 days or something like that hospitalised because waiting for surgery. He has been stabilised, of course, at the hospital all this time, a little bit more than a month. Since he is in a public system right now, because private insurance wouldn’t cover him, of course, it’s usually the waiting time is a little bit longer. Also, apparently they want him to be more stable, et cetera, for surgery.
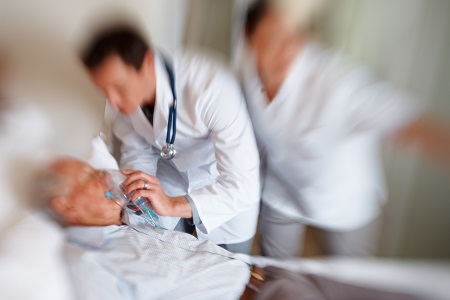
Roman: So, he started with pain chest, to feel uneasy, went to the cardiologist and he got an electrocardiogram. He got an echocardiogram, et cetera. They told him that he was fine. Imagine that.
Roman: So, he still felt uneasy and he still was told that he was fine. Then, he’s said, “No, I need to go to the hospital.” He went to the hospital, and still the hospital, they wanted to dismiss him. He insisted, “No, I’m having a heart attack.” So, he waited, waited, waited, and at 4:00 AM a doctor came and said, “Yes, you are having a heart attack.”
Patrik: How long ago was that?
Roman: This is like 35 days ago. Finally, he has his surgery on Monday, triple bypass surgery. It was like a five or six hour surgery. He was taken after that to intensive care unit.
Patrik: Prior to the surgery, where was he? Was he in intensive care as well?
Roman: No. The first days, he was like an intermediate thing, the first days. He was in an intermediate thing, and he was moved to a regular room while he waited for the surgery. After the surgery, of course, he was taken to intensive care unit.
Roman: So, the surgery was on Monday, so yesterday, around 5:00 PM, it was 72 hours already after surgery and when the doctor came out of the surgery, he told us the arteries were really bad. Those were his words, “We put a beautiful vein and if there would be complications, we could expect bleeding or we could expect …” I mean, if there was that bleeding, he would need to return to the …
Patrik: Theatre.
Roman: Yeah, to the theatre. Or it could be arrhythmias. I don’t know if that is a word in English, arrhythmias.
Patrik: Yeah, it is. Arrhythmias, yup.
Roman: And also, they put like a … it’s called …
Patrik: A balloon pump?
Roman: Balloon, yes. C-arm, they call it. A balloon.
Patrik: Can I just ask, he didn’t have the balloon before surgery?
Roman: He had the balloon before surgery, but the same day they put it. So, they placed the balloon like an hour or so before the surgery. After it was placed, he was ready to go to the open heart surgery.
Patrik: Okay. Let me ask you a few questions there. So, he was basically first diagnosed with the second heart attack 35 days before surgery, so it would be 38 days now. You said that if he’s in the public system, it sounds to me like he would have needed surgery pretty quickly after the heart attack, but it didn’t happen for a number of reasons. That’s why I’ve asked where was he before surgery, because I’ll tell you what I’ve seen over the years, and I don’t want to interrupt your story, but it’s probably important that you understand.
Patrik: What I’ve seen over the years is if somebody has a heart attack and they don’t get operated on quickly, the heart can deteriorate further and then make surgery so much more risky. Sometimes when patients have a heart attack and they can’t be operated on straight away, they do spend time in the intensive care to begin with to stabilise them, which is why I asked where was he before surgery. I’m not surprised that they put a balloon in before surgery. I’m not surprised by that at all.
Patrik: The next question is, do you know, has he had an ultrasound of the heart before surgery? Do you know that?
Roman: I don’t know for sure, but I wouldn’t be surprised because he had studies done.
Patrik: He must have. He must have had an ultrasound.
Roman: Yes.
Patrik: Do you know the result of the ultrasound?
Roman: No.
Patrik: Okay. That’s okay. We’ll come to that later. If you have that information, I could guide you in a certain direction already, but that’s okay. You don’t have that information, there’s no point in worrying about it. Just continue then. Okay.
Roman: Okay. So, just one second.
Roman: Mama, I’m in a call. Can you not come to this conference call please? I came all the way to here from my home. She’s nursing her baby, but she should come.
Patrik: Right.
Roman: So, my sister came all the way from Canada to this and it was a whole ordeal.
Roman: This is the thing, he went to the intensive care unit on Monday. There was no bleeding so far, in turn, we don’t need to go back to surgery or anything like that. For what being told, there was no arrhythmias either. We were asked for a medication in case there was arrhythmias, but I don’t think they used it. I asked about this, “Is he having arrhythmias,” and, “No.”
Roman: So, basically, what we are a little bit worried right now is that what they told us is that his blood pressure is very low. His blood pressure is very low and they are keeping his pressure up with … I mean, this is, I think is kind of funny language, with maximum …
Patrik: Life support, yeah.
Roman: Life support. If there’s a medication, they’re using as much medication as they can to keep his blood pressure.
Recommended and additional information :
Patrik: Not surprised. Not surprised.
Roman: Yes. What seemed to be good news is that they turned off the balloon and the heart is beating by itself, but a lot of the symptoms, of course, starting with blood pressure medications. One of the things that has been difficult for us is that they put this very young and I would say inexperienced people, to give the reports, to report things.
Roman: We have asked for a more senior person, because doctors, there were two doctors in the surgery, they be using moderate positive messages. For instance, they say, “We feel a little bit better today,” For instance. That kind of … you know? “He seems to be heading in the right direction,” et cetera. But when they give the reports at night, like around 7:00 PM, and this young professionals are more dreadful in the reports. For instance, this almost a girl, said, “Oh, he’s very, very bad. He could die anytime.” We were baffled. We were like, “This is not what the surgeons told us this morning. So, we need to speak to a more senior person, someone who has much better language and of course…”
Patrik: Experience, probably, as well.
Roman: It was very obvious. He said that he is stationary for now, that he hasn’t worsened, but it’s critical still. So, their job is to stabilise him. Their job is to stabilise him. They are doing, of course, their best. He’s not behaving bad, but they are watching him. He had a little bit of pulmonary oedema, a little bit of it. They treat him and of course for the rest of it, they put diuretics. The heart is not fully doing what it has to do yet. Usually oedema can happen, and we don’t know if this is normal. Part of what can happen.
Patrik: So, what’s your biggest frustration at the moment? Is it the uncertainty? What’s your biggest frustration?
Roman: Our frustration are two things, that he is still in an induced coma. We are heading for four days, we don’t know if … from what we read on internet, patients should be woken up already by this point, and he’s still under induced coma. That’s one thing that concerned us.
RELATED ARTICLES/Videos:
Roman: The other thing is that his blood pressure. We don’t know if this is normal. we don’t know if his heart is not yet pumping the way it should. We have been asked for more blood, so in this public system in South America, you have to go and find your own blood, so we did. We did. So, the explanation we were given is that this will help oxygenation and I don’t know what else, maybe blood pressure. But, this is my guess.
Patrik: So, he had blood? He had blood?
Roman: They told us he was going to have blood last night, so this is imminent, and the doctor stare at me for like five seconds without an answer and he’s like, “Yes, but we don’t know.” We’re going to go to the hospital this morning to find if they …
Patrik: Because, the reality is, Roman, you mentioned in the beginning he had no bleeding. If he’s had blood, he must have had some bleeding.
Roman: Okay.
Patrik: Just because he didn’t go back to surgery doesn’t mean that he didn’t bleed. If he had blood, there’s a high chance he was bleeding.
Roman: Yes, probably. But, no, they didn’t tell us that he needs to go back to surgery. The explanation we were given was that will help oxygenation or something like that, and he probably has some bleeding, of course.
Patrik: It would, it would. You see, the biggest problem for families in intensive care is you don’t know what you don’t know. You have a good understanding of what’s happened, but the is really in the detail. There are some … you mentioned, for example, balloon pump. You mentioned the blood pressure support. And that’s good knowledge to have. It helps me to help you. But, there are so many nuances, it would depend how much support is he on for his blood pressure. I can also tell you that the main reason he’s probably on the blood pressure medication is because they weaned off the balloon. That’s probably the main reason.
Roman: I’m sorry, they weaned off the balloon?
Patrik: Yeah, you mentioned they took out the balloon.
Roman: Yes.
Patrik: Right, so if he stayed on the balloon, there’s a very good chance he wouldn’t need the blood pressure medication. There’s a very good chance of that. Are you following?
Roman: Yes. What we were told though, is usually that balloon couldn’t stay more than 72 hours.
Patrik: No, no, no. I’ve seen balloons in for three weeks.
Roman: Oh. I see.
Patrik: You do want to minimise. You definitely do want to … you don’t want to leave a balloon in for three weeks. I agree with that. But, I have seen it, because sometimes balloon is often life or death. I do believe you don’t understand how sick your dad is. I don’t think they’ve really told you how sick your dad is. The balloon pump is a sign that your dad had a big heart attack. The balloon pump only is needed when the heart is really weak.
Roman: Okay.
Patrik: So, I do believe that they haven’t said the bigger picture with you, so I’ll give you a quick example so you understand how that fits in.
Roman: Okay.
Patrik: Somebody has a heart attack …
Roman: Sorry to interrupt, but we were told that he was in a very, very delicate and serious situation.
Patrik: Oh, absolutely. So, I’ll tell you, when somebody goes for cardiac surgery, I’d say in seven out of 10 patients, there is no balloon pump needed.
Roman: Okay.
Patrik: Makes sense?
Roman: Yes.
Patrik: So, the vast majority of patients who go for cardiac surgery or bypass surgery, the balloon pump is not needed. The balloon pump is only needed if there has been a significant heart attack. Let me ask you another thing. When he had the heart attack 38 days ago, did he have an angiogram?
Roman: Yes. My sister is here.
Patrik: Do you know the result?
Roman: I don’t know what the angiogram is. Oh, yes. He had an angiogram, yes. It went inside. Yes.
Patrik: Do you know the result?
Roman: What was the result?
Sussie: Sorry doctor, I’m here. The part that was affected by the heart attack, which I think was the lower part of his heart, it was only working at 35%.
Patrik: Okay, thank you so much. This is such important information. Thank you. This is very important.
Patrik: Okay, this is really important. I was looking for a number. I was looking for the 35 or 25 or … so, that means your dad’s heart is basically only working at 35%, which is why it would have been probably important to do the surgery as quickly as possible, but obviously had to wait 35 days. So, what’s your ideal outcome? What are you looking for in terms of … what do you want to happen in an ideal scenario?
Roman: We want him to have a recovery. We want him to wake up, to have a normal … sort of a normal path to recovery. It may take longer, but of course we want him back.
Patrik: Absolutely. So, do you feel like, at the moment, you’re getting mixed messages? Is that one of the problems?
Roman: Yes.
Patrik: Right, getting mixed messages. So, do you feel like they’re trying their best? Is that how you feel?
Roman: Yes, as well. Yes, of course.
Patrik: But, are you feeling you’re dealing with junior staff, you think?
Roman: Yes, I don’t think they make the decisions though. I don’t think …
Patrik: Yeah, there would be people in the background.
Roman: Yes, they are not in charge of the decisions. I think it’s senior people in the intensive care unit, plus the surgeon, et cetera, who are taking the decisions. So, in that sense, I guess it’s interesting you’re telling us he should have had the surgery much earlier. He shouldn’t have waited. You’re saying that, that’s interesting. But, in general, this junior staff is not in charge other than giving seedy information sometimes that upsets us.
Patrik: That’s right. So, you are aware that in a situation like that, every day is critical. I think you’ve got that awareness that if you want a resolution to the situation, you need to start asking the right questions because I don’t believe they’ve given you the full picture or they haven’t explained to you the full picture.
RELATED LINKS:
Patrik: For example, when they took the balloon out, I’m not surprised that his blood pressure dropped and that they had to start what’s called inotropes or vasopressors to stabilise his blood pressure. I’m not surprised for that at all.
Roman: One detail though, they haven’t taken the balloon out yet. They turned it off.
Patrik: Oh, turned it down? Yeah, sure. They reduce the port with the balloon pump, and in the meantime they had to start medications like noradrenaline or dobutamine. I don’t want to get too medically, but I’ve seen it hundreds of times. For you, this is all brand new. I’ve seen situations like that, I’ve seen hundreds of times over the years.
Sussie: I think they have taken it out, from what I understood. It’s out.
Roman: I understood differently, because they said, “If we need to turn it on, we will turn it on.”
Sussie: No, but yesterday they said they took it out. But that’s the thing, I understood that it was out, but he understood that …
Roman: That it was off.
Patrik: Right. Either or, the goal is always to take it out, if you can. That’s always the goal of course. So, why do you think it’s important that you do something now?
Roman: Because we are starting to get worried that he … our expectation was that he would be starting to be better and starting to come off of the machines little by little for instance. I don’t know the deal with the machine, et cetera. So, he’s not coming off for the moment.
Patrik: Right, it hasn’t happened.
Roman: That hasn’t happened. It’s the fourth day, and we don’t know where this is headed. We don’t know if this is normal, that some patients take a bit longer and more or less the way someone would behave, because this is a shock, of course, to the body to go through a surgery.
Patrik: Oh, it’s massive. It’s massive. So, before surgery, have you or your dad been debriefed and have they sort of promised you, “Oh yeah, we’ll do the surgery and then in two days, he’ll be out of intensive care?”
Roman: No.
Recommended:
Patrik: No? Not of that?
Roman: It was a better understanding to think three to five days, they said.
Patrik: Okay, and now it’s 72 hours?
Roman: Yeah, it’s more than 72 hours. Today it will be …
Patrik: Have they told you why he hasn’t woken up yet? Have they given you a reason?
Roman: That he’s not …
Patrik: Not stable?
Roman: All stable yet.
Patrik: Yeah. Okay. So, what do you feel my … so, from my perspective, what needs to happen next really is we need to start asking all the right questions to the doctors. I think that’s … that’s what I said. You don’t know what you don’t know and you only find out what’s happening by starting to ask the right questions, and I can help you with that, with asking them all the right questions. You have a very good basic understanding, but in order to find out what’s happening, for example, we need to ask things like why did he have blood? What sedation is he on? Sedation is the medications that keep him in the coma.
Roman: Okay.
Patrik: We need to ask things like, your sister mentioned, his heart function is 35%. He must have had an ultrasound in the meantime, and in the ideal world, after surgery, that function of 35% should have improved. I can tell you that with the balloon still in and with the blood pressure going down, I can almost 100% guarantee that the heart function is not better than 35%. But, we need to find out why. We need to find out why and we need to find out what are they going to do about it.
Roman: So, yesterday they said 20%, but I wouldn’t believe them.
Patrik: I would. I would, and I’ll tell you why. I’ll tell you why I would believe that. I’ll give you a couple of reasons why I would believe that. Number one, he wasn’t on the balloon before surgery. He came back with the balloon after surgery, and they started the blood pressure medication. So, there’s a very good chance that his heart function is only 20%. There’s a very good chance of that.
Roman: Okay.
Patrik: Why would he have surgery and then go from 35 to 20% and they would use the balloon and now the blood pressure medications, so I believe that’s a possibility, but we need to start asking those questions. So, what do you think might happen if you don’t get help and if you don’t start asking the right questions?
Roman: In general, I think we don’t have control, regardless. So, what we can do is to be informed, that’s the best thing.
Patrik: Absolutely.
Roman: That’s the best thing we can hope for. Information, we can put pressure and know that we know things, and that’s a way of doing a little bit of politics then.
Patrik: Yeah, that’s a way of managing the situation. They need to know that you are talking to someone who understands the situation. So, that’s exactly where I can help you with. Then, the question is, do you want some help with that? Because, if you do, then I can tell you what we can do next.
Roman: Yes.
Patrik: So, basically what I offer is I offer one-on-one consulting and advocacy. Now, I can tell you that in many situations, I talk to doctors and nurses directly with you. I do not speak Spanish, so I wouldn’t be able to offer to talk to doctors unless they speak English or German.
Roman: Yes, they don’t speak English. They don’t speak English. The other thing is since this is kind of a public system, they are very, very closed, very dismissive sometimes. So, it’s hard to talk to them in general, and that’s where it’s frustrating.
Patrik: It is, but it’s harder if you don’t know what you’re looking for and if you don’t know what to ask.
Roman: Of course.
Patrik: Yes, public system, I agree with. It doesn’t really matter which country, it’s not a good mentality, generally speaking, but it all comes down to what questions you can ask. So, what I offer, as I said to you, but what I can definitely do, I can set you up with all the right questions.
RECOMMENDED:
Patrik: If you do find an English speaking doctor, I’m very happy to talk to them as well. That’s something that’s beyond my control, whether you have somebody who’s English speaking there or not.
Patrik: Yeah, absolutely. I think it will be enough to help you with what you need to understand, what you need to know, and also to find out what’s going to happen over the next few days.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!