Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of my clients and the question in last week’s episode was
You can check out last week’s question by clicking on the link here.
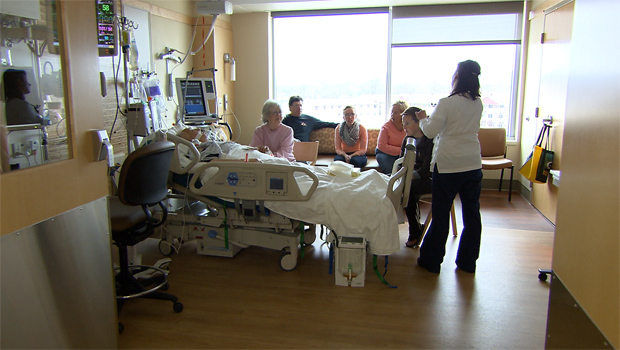
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer the next questions from one of my clients Natasha stating that documentation has not been done during the last hours of his Dad dying in the ICU.
In the last hours of my Dad dying in ICU they stopped documenting vital signs! Is this best practice?
“You can also check out previous 1:1 consulting and advocacy sessions with me and here.”
Natasha: Hello.
Patrik: Hi Natasha, it’s Patrik here. How are you?
Natasha: I’m not well. How are you?
Patrik: Very good. Did you say you’re not well?
Natasha: Yeah, I’m not well.
Patrik: Right. Is that, you’re going through the whole grieving or …?
Natasha: Yeah, I’m just … and I finished looking through all my dad’s records. I’m never going to get over this, my dad. I’m not. I don’t think there’s a grieving time that ends.
Patrik: It’ll get better. It’ll get better with time.
Natasha: I doubt it. All right, well so okay. So, well I mean, did you have a chance to …
Patrik: Yes I did, I did. So basically what I did, I didn’t look at the details but I had a glance through. The way I looked at this was, okay can we get the answers that you’re looking for from this? And I can confidently say yes. There’s enough information in there to get the information that you’re after. There’s no doubt about that. I am still surprised that out of seven days ICU that you get 1,200 pages. I can’t believe that, right? I mean, I would have said …
RECOMMENDED:
Natasha: But there’s still stuff missing.
Patrik: There is stuff missing and what’s missing-
Natasha: A lot.
Patrik: Yeah, yeah, what’s missing, for example, is the chest X-ray films or the CT films.
Natasha: Yes.
Patrik: That’s missing.
Natasha: Well I didn’t send that to you just because I don’t know how to do … but no, there’s still stuff missing though. Even in that, like the copy that I have. I couldn’t send it to you, just ’cause I don’t know how to copy it and I have to do that.
Patrik: So you do have other documents too?
Natasha: Yeah, I have chest X-rays and abdomen X-rays but even within that for one of the days it’s like white. The chest X-ray is like, white, right?
Patrik: Yeah, yeah.
Natasha: Like there’s a few missing ones and then I told you for a couple of days, they didn’t take … there’s no, it’s not on the file.
Patrik: Mm-hmm (affirmative). Mm-hmm (affirmative).
Natasha: And they’re not, last hour that my dad was dying, they just did not document the specifics of anything. Like his vital. It was horrible. That last hour before they stopped ventilating him, it went dead, the documentation.
Patrik: Mm-hmm (affirmative). With the documents, are you aware whether there’s anything documented in handwriting or is it all online, do you know?
RELATED ARTICLES:
- THE 10 THINGS YOU DIDN’T KNOW ARE HAPPENINGBEHIND THE SCENES IN INTENSIVE CARE THAT HOLD YOU BACK FROM HAVING PEACE OF MIND, CONTROL, POWER AND INFLUENCE, WHILST YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE!
Natasha: I saw them putting stuff in the computer, but I did see them writing, I saw the respiratory therapist writing something. But then I guess they put the values, because what the respiratory therapist did, they put it in the computer, they logged all of his measurements from the tidal wave and all that kind of stuff. So I think that was what he was writing down.
But I might tell you Patrik, do you want to hear other stuff that I found, what I was looking through? What happened is that so number one I didn’t find anything about the COPD study, the research study.
Patrik No. Look as I said I wasn’t, yep. And that is something you probably, you might want to ask them.
Natasha: Yeah.
Patrik: Now I do need to ask you again, you haven’t signed for consent for any of the studies, or for these studies I should say, you haven’t signed any consent?
Natasha: No I didn’t sign anything and there was no document. I just gave verbal consent because I thought they were just gonna monitor him, observe and …
Patrik: Yeah. And for example, with the bronchoscopy, did you sign for consent there?
Natasha: Oh you mean toward the end when he checked to see if the endotracheal tube was in?
Patrik: Yeah. Yeah.
Natasha: No, I just gave verbal consent.
Patrik: Mm-hmm (affirmative). Mm-hmm (affirmative). Because normally for a bronchoscopy you need to, my experience is a next of kin or a medical power of attorney needs to give written consent for a bronchoscopy too. That’s my experience. But it sounds like it’s all been on verbal, okay.
The one thing that’s despite the copious amounts of notes, one thing that’s missing to me is, okay so for example, if I work on a shift in ICU, at the end of my shift I write a report. Okay. I write a report.
Natasha: Yeah, right?
Patrik: I have seen reports from doctors. I have not seen any reports from nursing staff.
Natasha: Yeah, you haven’t right? I noticed that too.
Patrik: And that’s some-
Natasha: There’s none.
Patrik: And that’s why I’m asking, are they, for whatever reason, are they documenting that, number one, in separate notes by pen and paper. Or number two, they’re not documenting it at all which would surprise me.
RELATED INFO:
Natasha: So in certain places. But it’s very minuscule the way they document. They basically document, they attribute certain things to me, like statements that I said, like plan of care. Like these little plan of care blurbs, like, “Oh daughter said that sats should always be above 90% and it shouldn’t fall below 80%. Like really bullshit like little blurb, here and there on the respiratory therapist. But nothing substantial.
Patrik: No no, nothing-
Natasha: Nothing consistent, no.
Patrik: But what I have seen, and I have seen that by glancing over, there are entries from the doctors, they’re not entries from-
Natasha: Yes, yes. You see, they’re formal. They’re formal entries from the doctor but none from the nurses. No there’s none. There’s none like that. None.
Patrik: So, you know so-
Natasha: It’s for palliative care. The palliative care nurse, I think April fourth, she was the one who actually wrote an actual entry. She did like a doctor type of entry. She did that. The palliative care nurse.
Patrik: Yep. I’ve seen that.
Natasha: The useless palliative care.
Patrik: But there really must be some-
Natasha: But it’s not in his notes.
Patrik: They’re not there. And I would … the question remains, we can get a lot of information out of this, right? We can probably pretty much answer all your questions, but it would probably be good to have some nursing notes as well. It would make it more complicated, but it’s up to you what you want to do.
RECOMMENDED ARTICLES:
Natasha: Yeah. So, yeah I need to do that. I have to find out how to go about doing this because when you told me it happened Patrik, okay. Remember how you told me to find out about their DNR policy? Okay.
Patrik: Yep. Yep.
Natasha: So I called the hospital, whatever they have the main line. I blocked my number. I do that anyway sometimes, right. And I asked an operator who can I talk to about what the hospital’s Do Not Resuscitate policy is, right?
Patrik: Mm-hmm (affirmative). Mm-hmm (affirmative).
Natasha: And then they transferred me over to the CEO, the president of the hospital, Karena Kaluchi.
Patrik: Good.
Natasha: Yeah. And then okay so then her secretary picks up and she goes, “Oh you have to talk to our legal department about that.” So she gave me the paralegal’s name, transferred me over and then I was transferred over. I was asking her, “Oh I want to find out what is the DNR policy of your hospital?” I was very general, not specific, “I just want to know where I can find that information?” And she’s like, “You can find it online.” I go, “I looked online and I can’t find it for your hospital.” She’s like, “It’s the DNR policy, they’re the same everywhere. You have a written authorization from the patients.” Blah blah blah.
I go, “But what I’m saying is, that’s not how it usually happens. A patient is usually unconscious and they don’t have an advanced directive, so in that case?” She’s like, “Well then you have a signed paper with the surgeon.” Or whatever proxy. I go, but doctors often write DNR. She’s like, “Absolutely not. Absolutely not.” And then she’s like, “I don’t even know who I’m talking to. Are you a patient here?” I go, “No, but my dad was.” So I said, oh I said, “My dad was.” Oh shit. Yeah I said, “My dad was.” And she’s like, “That’s confidential.”
I go, “Why is it con-” And then, I was very calm. But she got really defensive when I asked her, “This is public knowledge. I want to find-” She said that it’s confidential, it’s in our records. I go, “But where can I obtain what Valley Hospital DNR policy is.” And she’s like, “Just look it up online. It’s the same everywhere. It’s the law.” And then I was like, “But you just said it was confidential. So if it’s the law then why can’t I have a copy of it?”
And then I was like, okay. And I said, “Okay, bye.” And then Patrik, listen to what happened after that. So I blocked my number, we have this option called Star 69 right, you can’t see the per- I called anonymously.
RECOMMENDED INFO:
Patrik: Yep.
Natasha: Like four days after my dad died, the president and CEO of the hospital, ’cause I made such a big ass stink, like really, I was such a bitch to everybody, because the way they were handling everything. And the CEO of the hospital, I guess they send it to everybody, like condolence letters. But then they wrote on the bottom, she wrote you can contact our patient relations person at blah blah blah about any questions you had about your father and blah blah blah. Someone will be contacting you in the next few weeks. Literally Patrik, 15 minutes after I made that phone call, someone from patient relations called me and left a message, asking if I wanted … “Oh we’re just following up over a letter that we sent you. If there’s anything you want to talk about, more information about your father, please give us a call.” Blah blah blah. It was so bizarre. Like they just knew that it was me or something. I don’t know.
Patrik: I’m just looking on their, I’m just on their website now. And I’m just looking whether there’s anything on the …
Natasha: She was awful. She’s so defensive.
Patrik: Oh yeah, of course they are. Of course they are.
Natasha: “Oh no, absolutely not.” Just the way she was doing it. I was like, oh chill.
Patrik: Right, right.
Natasha: And then 15 minutes later I get a call from, ’cause obviously their legal department must have heard what happened. ‘Cause I was making threats of making a complaint and stuff. I was clearly angry. But Patrik let me tell you something else that I noticed. My sister, I told you she’s a doctor. So I mean she’s been skimming over, we’ve been going back and forth and all. So let me just tell you what I noticed in the notes. So in the beginning when my dad was intubated on March 31st, 3:15 a.m.-ish, the critical care doctor, Dr. Sharma, who intubated my dad, he secured my dad’s endotracheal tube at 24 centimetres and the cuff pressure was about 20, was it a 20? I forget was it 20 H, I forget what you call it, it was 20 though, cuff pressure. And the way that they confirmed it was “hold it in place, on auscultation bilateral breaths and capnometry, okay?
Patrik: Mm-hmm (affirmative). Mm-hmm (affirmative).
Natasha: Up until about April 4th, early in the day, that was the same thing, right?
Patrik: Yep.
Natasha: Like everything was the same for the confirmation and about the placing of his tube. April 4th, later in the day, when I was reading through the notes, in the top form, his endotracheal tube was secured at 23 centimetres and his cuff pressure was 22. And they were not doing the capnometry anymore. So they never did the capnometry after that.
And it was on April 4th that there was a chest X-ray that said something along the lines of being five centimetres away from the carina. And the first time that the doctor initially put it in, it was like four centimetres away from the carina. And now take all this information Patrik, boggling, and then in the end, when the doctor said, “Oh it looks a little bit high up.” His ETT tube was high up and he pushed it in. So in the beginning, do you get, you see what I’m saying, I noticed that. That is changed.
RECOMMENDED ARTICLES:
Patrik: Yes. Absolutely.
And you know-
Natasha: To the end. So when the doctor first put it in and he confirmed it by three ways right? With the capnometry, the bilateral breath and then whatever, but then they just kind of lagged off. But in the end the other critical care doctor, Dr Chesnow he was this young white guy. He was like 39 years old. The first guy was an older Indian guy in his 50s. Young, white guy, Dr. Chesnow he said, “Oh looks a little high up.” So who the hell changed his ETT, his endotracheal tube and I noticed that gargling?
Patrik: We’ve talked about this.
Natasha: But I didn’t tell you about noticing it in the notes, about that. Like they actually, the centimetres and all, they had them as well, there’s more.
Patrik: That’s why I am wondering, is there information missing. Number one, is there information missing that they haven’t released or number two is this information just not there because they haven’t documented it. The reason this is, I believe, so important is, again, if I do a shift in ICU I take the cuff pressure for ventilated patient. I do that, okay. And that needs to be documented. So in view of the gargling and the potential of the cuff tube not being properly blocked, therefore increasing the risk of aspiration. If it’s not there, if it’s not documented, that is not best practise.
RECOMMENDED:
Natasha: They wrote down the cuff pressure.
Patrik: But that was only once. It needs to be written down at once the shift. Three times.
Natasha: No it was. It was. It was written down. The cuff pressure was written down for every time they checked it, they did write it down every time. But what I’m saying is that, all a sudden it was from March 31st until April 4th, early during the day, his endotracheal tube was a 24 centimetres and tight cuff pressure and it was chest with the capnometry, whatever device that is. But then, after that, they stopped checking with the capnometry device and his endotracheal tube was now secured at 23 centimetres and the cuff pressure was 22. But there was no capnometry confirmation. But they did write that down. So my whole thing is that it changed. Like it shifted his whole, but they did write it down. But what I’m saying is what effect did that have on him and …
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!