Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Lucy, as part of my 1:1 consulting and advocacy service! Lucy’s brother is in ICU due to accidental drug overdose and has a breathing tube in place. Lucy is asking what are the right questions to ask the doctors so her brother will survive?
My Brother is in ICU Due to Accidental Drug Overdose and Has a Breathing Tube in Place. What are the Right Questions to Ask the Doctors so my Brother Will Survive?
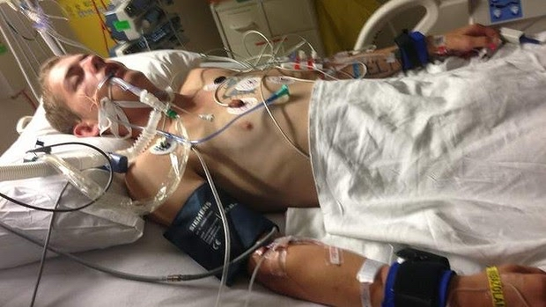
Lucy writes in and she says –
My brother is 58 years of age. He had an accidental drug overdose on pain medications, opiates to be exact. He has been in intensive care now for seven days. I’m really at a loss of what to do and I don’t know what questions I should ask and I don’t know how I should manage the doctors and the nurses.
Well, Lucy, the good news is, that’s exactly what I can help you with. So let’s go back to the emails that you’ve sent and I’m just going to read them out from the common conversation that we’d have what we have. So, and it would be very good to know what his current condition is exactly like and if he’s in a natural or in an induced coma. And also is he on a ventilator? Because you know, if he’s had a drug overdose there could well be, it could well be that he’s in a natural coma because of the drug overdose.
RECOMMENDED:
So Lucy then writes back.
Hi Patrik,
He is no longer being sedated under medical induced coma. He’s on a ventilator with a breathing tube and a feeding tube through the nose. He has surgery scheduled for a tracheostomy on Tuesday. The registered nurse said he will also have a PEG placed for feeding also, he is on kidney dialysis because the kidneys are failing and his liver enzymes are very high. It’s all very new to me. I’m not sure what questions to ask the medical staff and I wonder, will my brother pull through of this or through this also, if he does, what will his quality of life going to be?
So those are all great questions.
Lucy, because the biggest challenge for families in intensive care is simply that you don’t know what you don’t know. You don’t know what questions you need to ask and you don’t know how you need to manage doctors and nurses in intensive care to get the outcomes that you want for your brother.
RECOMMENDED:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
So let’s go through almost like a checklist of what questions you need to ask in a situation like that. So you’re saying your brother is not in a medically induced coma anymore, so you could, you want to know, you know, what’s his neurological condition like at the moment? So can he wake up? Is he obeying? Is he in pain? If he can’t answer yes or no, whether he’s in pain, is he showing signs of pain non-verbally? Does he look like he’s in distress? Can he move all limbs?
Are his pupils equal and reactive to light? Those are all very important questions. Another issue that can happen after a drug-induced overdose is, does he withdraw from the medications or from the drugs that he sometimes takes outside of ICU? And if he’s withdrawing from those drugs, is he at risk of seizures and other withdrawal symptoms and do they need to be managed medically with other medications? So that’s what you need to look for neurologically.
RECOMMENDED:
Next you need to find out if your brother is hemodynamically stable. So for example, is his blood pressure normal? Is his heart rate normally is in a normal heart rhythm? Is his blood pressure normal? Is he on inotropes or vasopressors? Or is he on vasodilators? Has he would be on inotropes if he has a weak heart or if he has low blood pressure? You would be on vasodilators if, for example, you had high blood pressure or a hypertension, right?
Is your brother febrile? Does he have a temperature? Is he warm in his limbs? Right? Again, is his heart rate normally see in irregular heart rhythm is does his heartbeat fast as you have for tachycardia for example. If he has a temporary change in cardiac and low blood pressure, does he have an infection?
Then blood results you need to look out for blood results such as hemoglobin, white cell count again to look for an infection or CRP to look for infection markers, right. You mentioned the liver enzymes need to watch out for them. You need to watch out for kidney markers and kidney results. Lab results in particular if he’s on dialysis. So with the overdose, his kidneys might have taken a hit and he might need temporary dialysis.
RECOMMENDED:
So those are things that you need to look out for. Also, if he does have a temperature and a tachycardia, high heart rate develop, low blood pressure, what’s his lactate like? And again, that could be another sign of infection if his lactate is high.
Next, does he have a central line or an arterial line which is, gives him IV access, intravenous access, a central line in particular, again, to manage medications such as sedation, opiates as well as vasopressors or inotropes. Arterial line is necessary for the ventilation and the breathing tube because you can check arterial blood gases to check oxygen levels in the blood, carbon dioxide levels in the blood electrolyte levels in the blood such as potassium in particular which is important if your brother is on dialysis, you’ve got to check regular potassium levels.
So with the arterial line, you can also check whether ventilation is physiological or not or the ventilation parameters need to be adjusted. The next thing leads me to mechanical ventilation. Your brother is on a ventilator. How far away is he from getting off the ventilator?
RECOMMENDED:
You are talking about what they’ve got a tracheostomy scheduled on Tuesday, so it’s likely that your brother is not ready to come off the ventilator and that they think he won’t be ready for a while because he’ll have a tracheotomy by the looks of things. To find out what ventilator settings he’s on and then I can guide you from there.
What to do next? Is he close up coming off the ventilator? Is the tracheostomy, the right thing to do? Send me a picture of the ventilator and the monitor and then I can tell you what he’s up to. Send me the blood results and I can interpret them for you. Hopefully, the tracheostomy is temporary, hopefully, they move your brother towards weaning off the ventilator as quickly as possible. Then the nasogastric tube he’s got in his nose should be more than sufficient.
Questions to ask about ventilation as well are how much oxygen is he on? How much PEEP is he on? How much pressure support is he on? Is he breathing by himself or does he need it, does the ventilator do all the work? What are the arterial blood gases like? Those are some of the questions you need to ask in order to determine is your brother able to come off the ventilator without needing the tracheostomy?
Because the tracheostomy could be a long-term thing, a long-term device, and you don’t want that unless it’s really, really necessary. Next, does your brother get enteral feeds and is he, more importantly, absorbing those feeds? Can he tolerate them? Is the opening bowels regularly, right? Is his tummy soft? You know, if his tummy was distended and he hasn’t had his bowels open for many days, that could put pressure on his lungs and it could be an obstacle to get your brother off the ventilator.
RECOMMENDED:
Again, it all comes down at this point in time to avoid the tracheostomy. You know, even your brother’s tummy is important because again, he hasn’t had bowel to open for many days and his tummy is distended and it puts pressure back on the lungs. And it may be an obstacle to get your brother off the ventilator.
Kidneys. You mentioned kidneys earlier. Your brother is on dialysis. So we’re moving, as you might see by now, we’re moving from head to toe. We’ve gone from neurological assessment, we’ve gone to cardiovascular assessment, we’ve gone to respiratory assessment about the breathing. Then we’ve gone to the abdominal assessment with bowel movement, absorbing or feeds, you know, all of that.
And now we’re moving downwards towards the kidneys. So why is your brother on dialysis? Have the kidneys failed completely? Is it producing your own or is it just that he doesn’t produce enough your own and they’re removing more fluids, you know, again, to help your brother as well to get off the ventilator, the more fluids they can remove, the more likely it is the lungs are dry and that will help with removing your brother off the ventilator with weaning him off the ventilator.
And again, maybe you won’t need the tracheostomy and other things you need to look for his general condition. Is he getting good nursing care? Is he getting daily washers? Is he getting mouth care? Is he getting pressure area care? Is his skin intact? And all of that.
RECOMMENDED:
And also you mentioned the liver enzymes are high and that could be simply a result of, you know, the opiates that your brother has taken and the liver not coping. And also the induced coma that your brother was in. He was getting, you know, some propofol, maybe somebody does alarm over, said some morphine, some fentanyl that are all impacting on the liver enzymes as well.
So then Lucy, you’re asking when is a tracheostomy the right thing to do? Well, the tracheostomy is the right thing to do after let’s just say 10 to 14 days, especially if he’s not walking upright. And if he’s waking up and he can obey commands and he can breathe by himself, he has minimal secretions, his chest X rays clear and he can cough and the arterial blood gases are fine, then your brother should be able to come off the ventilator.
I also need to share with you that, you know, you mentioned that you are in Florida, in the United States, that if your brother ends up with a tracheostomy, there’s a very good chance your brother might be sent to an LTAC facility, long-term acute care facility. And that’s a disaster from my experience.
RECOMMENDED:
Right? LTAC’s are just designed to get patients out of ICU quickly without looking at clinical needs. They’re really a vehicle to save money and free up beds in ICU and a lot of patients die in LTAC. So it’s really important that you make the right decision going forward. Right.
Without, you know, putting your brother at risk is saying that he’s been out of the induced coma now for three days and that today he’s awake and he’s communicating by opening his eyes and raising his eyebrows. He continues to be on the ventilator and the ICU nurse reports his oxygen is down to 30%. I assume that his kidneys and liver enzymes are high as a direct result of the opiate overdose he’s had.
A few days ago, the ICU nurse said that the opiates were a painkiller with Tylenol and that it’s hard on the kidneys. Yeah. The ICU nurse is right. Tylenol is hard on the kidneys, hard on the liver and it makes the liver and the kidneys fail.
So hopefully the dialysis is just going to be temporary and the kidneys and the liver will recover if oxygen is down to 30%. That’s a good thing. Right? It means that you know, if the PEEP is down as well as the pressure support is down to less than 10, and he’s obeying commands, arterial blood gases are good and he’s breathing by himself. He doesn’t need a lot of endotracheal suctioning, you should be able to come off the ventilator without the need for the tracheostomy.
So, and then I had another update from Lucy as we went along during our consulting sessions and Lucy said in another email
Hi Patrik,
I went to ICU today and the doctor did say that my brother is not showing any brain damage. He even told me that his liver enzymes are improving and he’s on dialysis just once a day. They tried solid foods on him today, but his throat is still swollen because he had the breathing tube out yesterday.
They will try again with solid food tomorrow. And obviously now that the breathing tube is out, he has no tracheostomy or PEG surgery. So I’m really very grateful for your advice. And I continue to read and watch the material that you sent and I’m telling everyone about you. Thank you again for all your kindness and your help.
RECOMMENDED:
So, Lucy, that’s really great that your brother came off the ventilator and the breathing tube and that he doesn’t need a tracheostomy, that he doesn’t need a feeding tube and for you watching that you are having a loved one in intensive care.
Keep in mind the intensive care team is always giving you the worst case scenario. The ICU team will always look at the worst-case scenario. They will never tell you the full story and they will just cover themselves. So by covering themselves, I mean you know, they would just tell you that you know your loved one is going to die. They would need a tracheostomy, they will need this, that and the other.
Just simply because if they were going to tell you, “Hey Lucy, your brother would have been in ICU for another week and then he’ll go out of ICU and it’ll recover and all we’d be hunky Dory”. It could be in big trouble. If that isn’t going to happen. So you always have to read between the lines that they will always give you the worst-case scenario, even though your last one may be at, you know, going to a hospital ward soon, right?
Always need to read between the lines and you always need to ask for professional help because intensive care is such a highly specialized area as you would have known by now. You know, you don’t know what you don’t know. And there are sometimes 10, 20, 30, 40 sometimes even 50 things happening simultaneously in a critically ill patient.
RECOMMENDED:
And every little thing is a piece of the puzzle and it’s very important. And if you haven’t worked in intensive care for a long time as I have, I’ve worked in intensive care for 20 years, it’s hard for you to interpret any meaning in the situ into the situation. And it’s hard for you to ask the right questions if you don’t know what to look for and if you don’t know what to ask.
So that’s it for today. So Lucy, thank you again for being a client.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!
Related Articles:
- 5 Ways to have control, power and influence while your loved one is critically ill in Intensive Care